 Back
BackThe Integumentary System: Structure, Function, and Clinical Aspects
Study Guide - Smart Notes

The Integumentary System
Overview
The integumentary system is composed of the skin, hair, nails, subcutaneous tissue, and various glands. It serves as the body's primary barrier against environmental hazards and plays a crucial role in homeostasis, sensation, and metabolic processes.
Protection: Shields the body from injury, infection, and dehydration.
Temperature Regulation: Maintains internal temperature through sweat production and blood flow adjustments.
Sensory Perception: Contains receptors for touch, pain, temperature, and pressure.
Water Loss Regulation: Prevents excessive water loss via keratinized cells and glycolipids.
Chemical Synthesis: Synthesizes vitamin D and other substances.
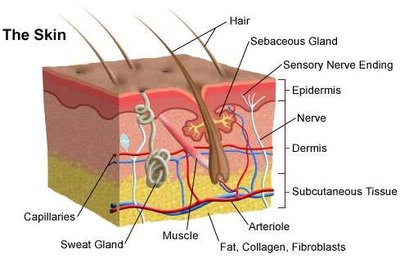
Functions of the Integumentary System
Protective Barriers
Physical Barriers: Keratinized cells and glycolipids prevent water loss and block pathogens. Only lipid-soluble substances (e.g., oxygen, carbon dioxide, steroids) can penetrate easily.
Chemical Barriers: Sebum, acid mantle, and antimicrobial peptides (e.g., defensins, cathelicidins) inhibit microbial growth. Melanin protects against UV radiation.
Biological Barriers: Langerhans cells and macrophages provide immune defense; DNA absorbs UV radiation and dissipates it as heat.
Temperature Regulation
Sweating: Evaporation of sweat dissipates heat.
Vasodilation: Blood vessels in the dermis dilate to release heat.
Vasoconstriction: Blood vessels constrict to retain heat in cold conditions.
Cutaneous Sensations
Meissner’s corpuscles & Merkel discs: Detect light touch.
Pacinian corpuscles: Detect deep pressure and vibration.
Hair root plexus: Detects hair movement.
Bare nerve endings: Detect pain, heat, and cold.
Excretion and Absorption
Eliminates wastes such as ammonia, urea, uric acid, sodium chloride, and water.
Metabolic Functions
Vitamin D Synthesis: UV light converts precursors in the skin to vitamin D, which is activated in the liver and kidneys. Essential for calcium and phosphate regulation.
Blood Reservoir: The skin can store up to 5% of the body’s blood volume.
Types of Body Membranes
Classification and Function
Serous Membranes: Line closed body cavities; secrete lubricating serous fluid.
Mucous Membranes: Line cavities open to the exterior; secrete mucus for protection and moisture.
Synovial Membranes: Line joint cavities; secrete synovial fluid for lubrication.
Cutaneous Membrane: The skin; protects underlying tissues.
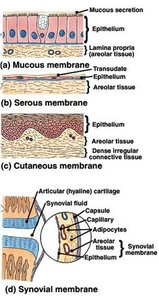
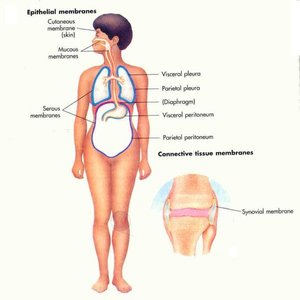
Characteristics and Types of Skin
General Features
Largest organ of the body (~2 m2, 16% of body mass).
Composed of two main layers: epidermis (superficial) and dermis (deep).
Thickness varies from 0.5 mm (eyelids) to 6 mm (palms, soles).
Thin vs. Thick Skin
Thin Skin: Covers most of the body, contains hair, fewer sweat glands, lacks stratum lucidum.
Thick Skin: Found on palms and soles, hairless, more sweat glands, contains stratum lucidum, pronounced dermal papillae.
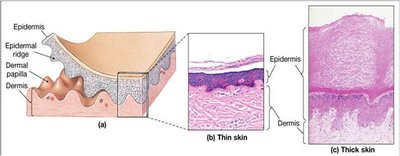
Layers of the Skin
Epidermis
The epidermis is a stratified squamous epithelium composed of several cell types and layers.
Keratinocytes: 90% of epidermal cells; produce keratin for protection and waterproofing.
Melanocytes: 8%; produce melanin for UV protection.
Langerhans Cells: Immune function; present antigens to lymphocytes.
Merkel Cells: Sensory receptors for touch.
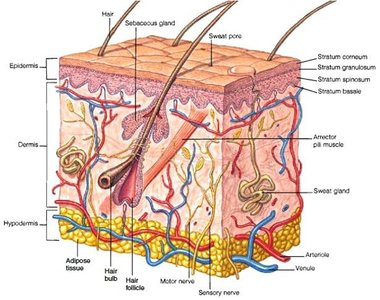
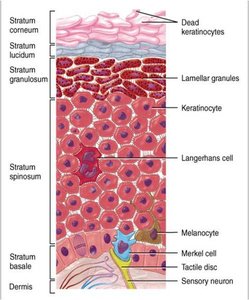
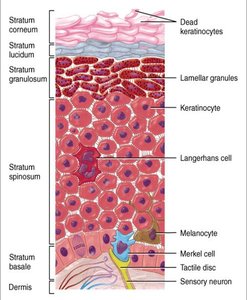
Layers of the Epidermis (from superficial to deep)
Stratum Corneum: 25–30 layers of dead, keratinized cells; barrier to water, microbes, and injury.
Stratum Lucidum: Only in thick skin; 3–5 layers of clear, dead cells.
Stratum Granulosum: 3–5 layers; cells undergo apoptosis, contain lamellar granules (waterproofing).
Stratum Spinosum: 8–10 layers; provides strength and flexibility.
Stratum Basale (Germinativum): Single row of dividing cells; site of new cell formation.
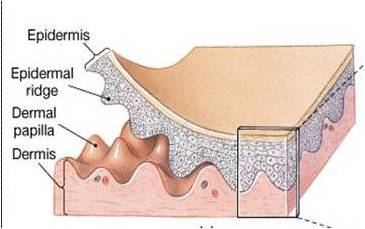
Dermis
Papillary Layer: Superficial; areolar connective tissue with dermal papillae (increase surface area, contain capillaries and tactile receptors).
Reticular Layer: Deep; dense irregular connective tissue with collagen and elastic fibers, houses hair follicles, nerves, and glands.
Hypodermis (Subcutaneous Layer)
Not part of the skin; attaches skin to underlying tissues.
Composed of connective and adipose tissue for insulation and energy storage.
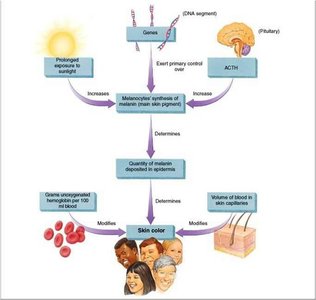
Skin Color and Pigmentation
Determinants of Skin Color
Melanin: Produced by melanocytes; amount and type (eumelanin, pheomelanin) determine color.
Carotene: Yellow-orange pigment; precursor to vitamin A, accumulates in stratum corneum and fat.
Hemoglobin: Red pigment in blood; visible in fair skin due to low melanin.
Clinical Clues from Skin Color
Cyanosis: Blue tint due to low oxygen.
Jaundice: Yellow tint from bilirubin buildup (liver disease).
Erythema: Redness from increased blood flow (inflammation, heat, allergy).
Pallor: Paleness (anemia, shock).
Bronzing: Addison’s disease (adrenal cortex dysfunction).
Bruising (Hematoma): Blood leakage under skin.
Skin Markings and Aging
Skin Markings
Friction Ridges: Fingerprints; enhance grip.
Flexion Lines: Creases at joints.
Freckles and Moles: Local accumulations of melanin.
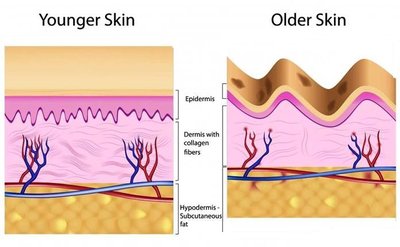
Aging of the Skin
Stem cell activity declines; skin thins and repairs slowly.
Reduced immune response and vitamin D production.
Decreased glandular activity; drier skin.
Loss of elasticity and subcutaneous fat; wrinkles and sagging.
Accessory Structures of the Skin
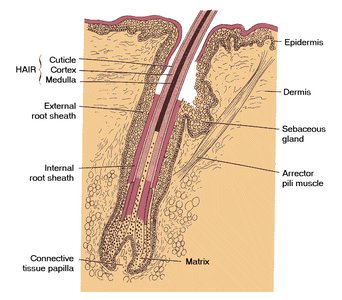
Hair
Shaft: Visible part; shape determines hair type (straight, wavy, curly).
Root: Below the surface; contains medulla, cortex, and cuticle.
Follicle: Surrounds root; contains bulb and matrix (growth zone).
Arrector Pili Muscle: Causes hair to stand (goosebumps).
Hair Root Plexus: Sensory nerve endings for touch.
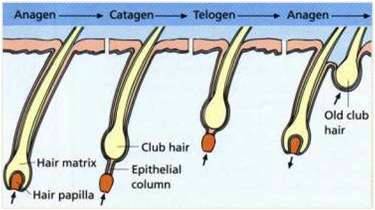
Hair Growth Cycle
Anagen (Growth Phase): 2–6 years; active hair growth.
Catagen (Transitional Phase): 1–2 weeks; follicle shrinks.
Telogen (Resting Phase): 5–6 weeks; hair falls out, new hair forms.
Functions and Color of Hair
Protects scalp, eyes, and respiratory passages.
Color determined by melanin type and amount; gray/white hair results from decreased melanin or air bubbles in shaft.
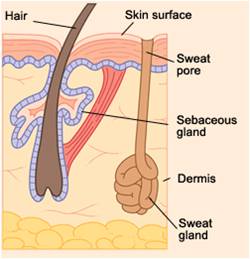
Skin Glands
Sudoriferous (Sweat) Glands: Eccrine (thermoregulation, waste excretion) and apocrine (emotional stress, puberty, viscous secretion).
Sebaceous (Oil) Glands: Secrete sebum; lubricate skin/hair, inhibit bacteria, increase at puberty.
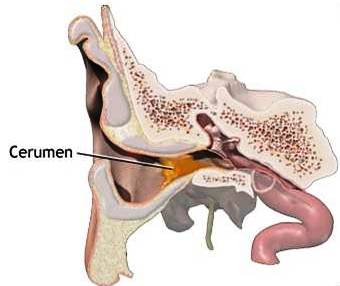
Ceruminous Glands: Modified sweat glands in ear canal; produce earwax (cerumen) for protection.
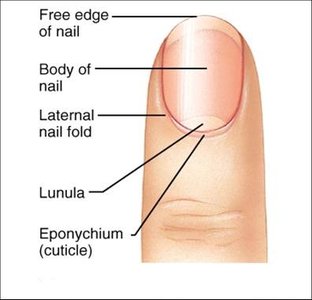
Nails
Composed of hard, keratinized cells.
Parts: Nail body, free edge, root, lunula, hyponychium, eponychium (cuticle), nail matrix (growth zone).
Functions: Grasping, manipulating objects, protection, scratching.
Imbalances of Homeostasis
Skin Disorders
Lesions: Elevated (warts, blisters), flat (scabs, hives), depressed (ulcers, fissures).
Infections: Viral (herpes, warts), fungal (athlete’s foot), bacterial (boils, impetigo).
Contact Dermatitis: Inflammatory response to irritants or allergens; treated by avoidance and corticosteroids.
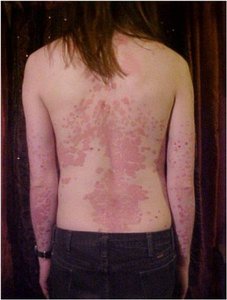
Genetic Diseases: Psoriasis (rapid cell turnover, thick scales), Vitiligo (loss of melanocytes, patchy depigmentation).
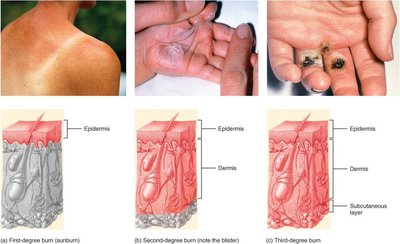
Burns
First-degree: Red, inflamed, superficial.
Second-degree: Blisters, deeper tissue involvement.
Third-degree: Full-thickness destruction, risk of dehydration and infection.
Fourth-degree: Extends to muscle or bone.
Rule of Nines: Used to estimate burn area for treatment.
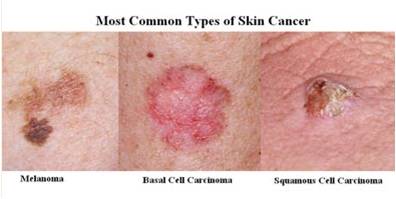
Skin Cancer
Basal Cell Carcinoma: Most common, least malignant, arises from stratum basale.
Squamous Cell Carcinoma: Arises from stratum spinosum, can metastasize if untreated.
Malignant Melanoma: Cancer of melanocytes, highly metastatic and deadly if not detected early.
Additional info: The integumentary system is essential for maintaining homeostasis, protecting against environmental hazards, and providing sensory information. Disorders of the skin can indicate systemic diseases and require prompt recognition and management.
