 Back
BackThe Integumentary System: Structure, Function, and Clinical Aspects
Study Guide - Smart Notes

The Integumentary System
Overview and General Functions
The integumentary system is the body's largest organ system, comprising the skin and its derivatives such as hair, nails, sweat glands, and oil glands. It serves as the primary barrier between the internal environment and the external world, providing protection, sensation, and regulation of body temperature.
Protection: Shields underlying tissues from mechanical, chemical, and biological damage.
Temperature Regulation: Maintains homeostasis through sweat production and blood flow regulation.
Cutaneous Sensations: Detects touch, pressure, pain, and temperature changes.
Metabolic Functions: Synthesizes vitamin D and participates in other metabolic processes.
Blood Reservoir: Stores up to 5% of the body's blood volume.
Excretion: Eliminates nitrogenous wastes and salts through sweat.
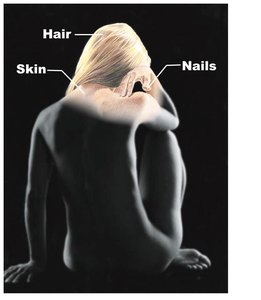
Structure of the Skin
Major Layers of the Skin
The skin consists of three main layers, each with distinct structures and functions:
Epidermis: The outermost, avascular layer composed of keratinized stratified squamous epithelium.
Dermis: The middle, vascular layer made of connective tissue, containing nerves, blood vessels, and appendages.
Hypodermis (Subcutaneous Layer): Not technically part of the skin, but anchors it to underlying tissues and provides insulation and shock absorption via adipose tissue.
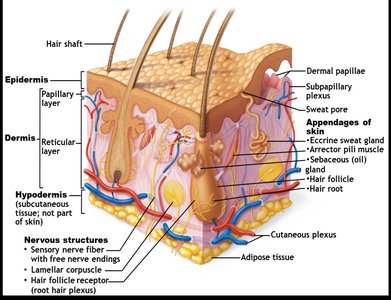
Epidermis: Layers and Cell Types
Layers of the Epidermis
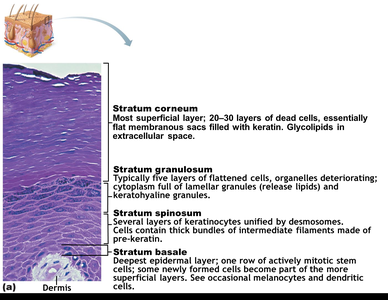
The epidermis is organized into four or five distinct layers (from deep to superficial):
Stratum Basale: Single row of mitotically active stem cells; contains melanocytes and Merkel cells.
Stratum Spinosum: Several layers of keratinocytes connected by desmosomes; contains dendritic cells and melanosomes.
Stratum Granulosum: 4–6 layers of flattened cells; keratinization begins, and lamellar granules release glycolipids for waterproofing.
Stratum Lucidum: Present only in thick skin (palms, soles); thin, translucent band of dead keratinocytes.
Stratum Corneum: 20–30 layers of dead, keratinized cells; provides a durable overcoat for protection.
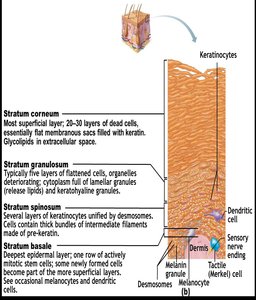
Cell Types in the Epidermis
Keratinocytes: Produce keratin, a protein that gives skin its strength and waterproofing properties.
Melanocytes: Synthesize melanin pigment, which protects against UV radiation.
Dendritic (Langerhans) Cells: Immune cells that detect and present antigens to lymphocytes.
Tactile (Merkel) Cells: Sensory receptors for touch.
Dermis: Structure and Layers
Papillary Layer
The papillary layer is the superficial portion of the dermis, composed of areolar connective tissue. It contains dermal papillae, which are projections that increase surface area for exchange of gases, nutrients, and waste products. These papillae contain capillary loops, Meissner's corpuscles (touch receptors), and free nerve endings (pain receptors). In thick skin, dermal papillae form friction ridges, which enhance grip and create fingerprints.
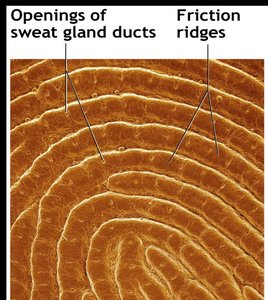
Reticular Layer
The reticular layer makes up about 80% of the dermis and consists of dense irregular connective tissue. It contains collagen and elastic fibers, providing strength, extensibility, and elasticity. Cleavage lines, formed by the orientation of collagen fibers, are important in surgical incisions for optimal healing. Flexure lines are dermal folds at or near joints, visible on the palms and fingers.

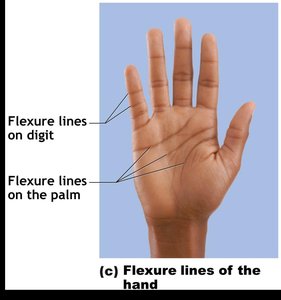
Skin Markings
Types of Skin Markings
Friction Ridges: Enhance grip and create fingerprints.
Flexure Lines: Dermal folds at joints, allowing skin to accommodate movement.
Striae (Stretch Marks): Silvery-white scars caused by dermal tearing from rapid stretching.
Blisters: Fluid-filled pockets separating epidermal and dermal layers due to acute trauma.
Skin Color
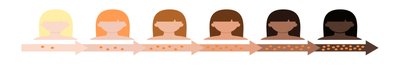
Pigments Determining Skin Color
Melanin: Only pigment produced in the skin; ranges from reddish-yellow to brownish-black. Amount and form determine skin color. Sun exposure increases melanin production.
Carotene: Yellow to orange pigment from diet (e.g., carrots); accumulates in the stratum corneum and hypodermis.
Hemoglobin: Oxygenated pigment in red blood cells; gives fair skin a pinkish hue.
Clinical Significance of Skin Color Changes
Cyanosis: Blue skin due to low oxygenation of hemoglobin.
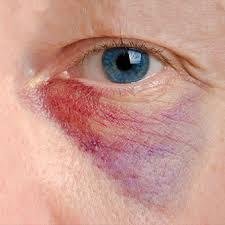
Erythema: Redness from fever, hypertension, inflammation, or allergy.
Pallor: Paleness from anemia, low blood pressure, or emotional stress.
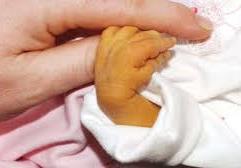
Jaundice: Yellow cast from liver disorders.
Bronzing: Metallic appearance from Addison's disease (adrenal insufficiency).
Bruises: Clotted blood beneath the skin (hematomas).
Appendages of the Skin
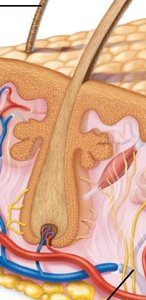
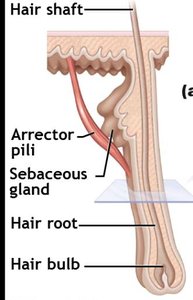
Hair and Hair Follicles
Hair is composed of dead, keratinized cells and serves protective and sensory functions. Hair follicles extend from the epidermal surface into the dermis and are associated with sebaceous glands and arrector pili muscles (responsible for "goose bumps").
Types of Hair: Vellus (fine, pale) and terminal (coarse, long).
Growth: Influenced by nutrition and hormones; follicles cycle between active and regressive phases.
Hair Color: Determined by melanin and, in red hair, trichosiderin.
Alopecia: Hair thinning with age; male pattern baldness is genetically determined.
Nails
Nails are scale-like modifications of the epidermis, composed of hard keratin. They protect the distal, dorsal surfaces of fingers and toes and aid in picking up small objects.
Sweat (Sudoriferous) Glands
Eccrine Glands: Most numerous; secrete watery sweat for thermoregulation.
Apocrine Glands: Found in axillary and anogenital areas; secrete viscous fluid that may produce body odor after bacterial decomposition.
Modified Apocrine Glands: Ceruminous (earwax) and mammary (milk) glands.
Sebaceous (Oil) Glands
Widely distributed except in thick skin of palms and soles.
Secrete sebum (oily, bactericidal substance) into hair follicles.
Activated at puberty by androgens.
Functions of the Integumentary System
Protective Barriers
Chemical Barriers: Skin secretions (acid mantle, sebum, defensins) and melanin protect against pathogens and UV radiation.
Physical Barriers: Keratinized cells and glycolipids block most water and water-soluble substances.
Biological Barriers: Dendritic cells and macrophages provide immune defense; DNA absorbs UV radiation.
Temperature Regulation
Insensible perspiration (500 ml/day) occurs under normal conditions.
Sensible perspiration increases with heat, promoting evaporative cooling.
Vasoconstriction in cold environments conserves heat.
Cutaneous Sensations
Meissner's Corpuscles: Detect light touch (in dermal papillae).
Lamellar (Pacinian) Corpuscles: Sense deep pressure (in deep dermis).
Free Nerve Endings: Detect pain, temperature, and some touch.
Metabolic Functions, Blood Reservoir, and Excretion
Synthesizes vitamin D precursor and collagenase.
Acts as a blood reservoir (up to 5% of blood volume).
Excretes nitrogenous wastes and salts in sweat.
Homeostatic Imbalances of the Skin
Infections and Allergic Reactions
Athlete’s Foot: Fungal infection.
Boils and Carbuncles: Bacterial infections.
Cold Sores: Viral infection.
Contact Dermatitis: Allergic reaction (e.g., poison ivy).
Impetigo: Contagious bacterial infection (staphylococcus).
Psoriasis: Autoimmune disease causing overproduction of skin cells.
Skin Cancer
Types and Characteristics
Basal Cell Carcinoma: Most common, least malignant; arises from stratum basale; slow-growing and rarely metastasizes.
Squamous Cell Carcinoma: Arises from keratinocytes of stratum spinosum; can metastasize if not removed.
Melanoma: Cancer of melanocytes; highly metastatic and resistant to chemotherapy.
ABCD Rule for Melanoma Detection:
Asymmetry: Two sides of the pigmented area do not match.
Border irregularity: Edges are notched or indented.
Color: Contains several colors (black, brown, tan, red, or blue).
Diameter: Larger than 6 mm (pencil eraser size).
Burns
Causes, Dangers, and Evaluation
Caused by heat, electricity, radiation, or chemicals; denature proteins and kill cells.
Major threats: dehydration, electrolyte imbalance, renal shutdown, and circulatory shock.
Severity assessed by the "rule of nines" (estimates fluid loss) and burn depth.
Degree | Layers Involved | Symptoms |
|---|---|---|
First-degree | Epidermis only | Redness, pain, swelling |
Second-degree | Epidermis and upper dermis | Blisters, pain |
Third-degree | Entire thickness of skin | Gray-white, cherry red, or blackened; not painful (nerves destroyed) |
Developmental Aspects of the Integumentary System
Fetal: Epidermis from ectoderm, dermis and hypodermis from mesoderm; lanugo coat (fine hair) and vernix caseosa (protective covering) develop.
Infancy to Adulthood: Skin thickens, subcutaneous fat increases, gland activity rises; environmental damage accumulates after age 30.
Aging: Epidermal replacement slows, skin thins and dries, elasticity decreases, risk of cancer rises, hair thins.
Prevention: UV protection, good nutrition, hydration, and hygiene delay aging effects.
