 Back
BackThe Lymphatic System and Immunity: ANP College Study Notes
Study Guide - Smart Notes

The Lymphatic System and Immunity
Introduction to the Lymphatic and Immune Systems
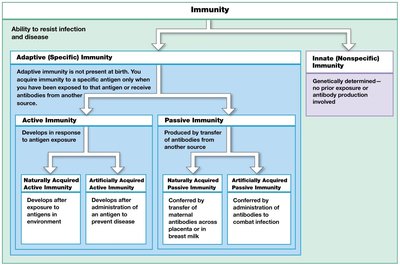
The lymphatic system is a network of cells, tissues, and organs that defends the body against environmental hazards and internal threats. The immune system includes all body cells and tissues involved in immunity, spanning the lymphatic, integumentary, skeletal, cardiovascular, respiratory, and digestive systems. Immunity is the ability to resist infection and disease, while pathogens are organisms such as viruses, bacteria, fungi, and parasites that cause disease.
Components of the Lymphatic System
Lymph: Fluid similar to plasma but lacking plasma proteins.
Lymphatic vessels: Carry lymph from peripheral tissues to veins.
Lymphoid cells: Include lymphocytes, phagocytes, and other immune cells.
Lymphoid tissues: Connective tissues dominated by lymphocytes.
Lymphoid organs: Sites where lymphocytes form, mature, or become activated (e.g., lymph nodes, thymus, spleen).
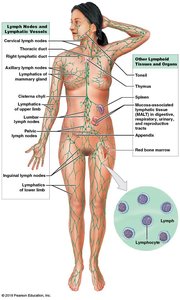
Primary and Secondary Lymphoid Tissues and Organs
Primary lymphoid tissues/organs: Sites of lymphocyte formation and maturation (red bone marrow, thymus).
Secondary lymphoid tissues/organs: Sites where lymphocytes are activated (tonsils, lymph nodes, spleen).
Functions of the Lymphatic System
Production, maintenance, and distribution of lymphocytes and other lymphoid cells.
Return of excess tissue fluid to the bloodstream to maintain normal blood volume.
Regulation of interstitial fluid composition by transporting hormones, nutrients, and wastes.
Lymphatic Vessels and Capillaries
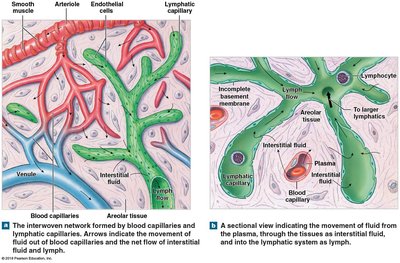
Lymphatic capillaries are the smallest lymphatic vessels, present in almost every tissue. Compared to blood capillaries, they:
Are closed at one end and begin in tissues.
Have larger luminal diameters and thinner walls.
Feature overlapping endothelial cells acting as one-way valves, allowing entry of fluids, solutes, viruses, and bacteria, but preventing their return.
Major Lymph-Collecting Vessels
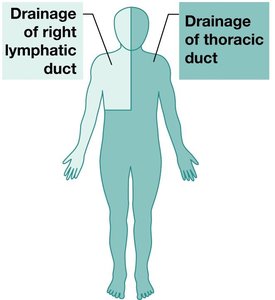
Lymphatic vessels join to form large lymphatic trunks that empty into two major collecting vessels:
Thoracic duct: Drains lymph from all body regions inferior to the diaphragm and the left side superior to the diaphragm; empties into the left subclavian vein.
Right lymphatic duct: Drains lymph from the right side of the body superior to the diaphragm; empties into the right subclavian vein.
Lymphoid Cells and Organs
Lymphoid cells: Include phagocytic cells (macrophages, microphages) and lymphocytes (T cells, B cells, NK cells).
Lymphoid organs: Encapsulated structures such as lymph nodes, thymus, and spleen.
Lymph nodes: Filter lymph, remove antigens, and present them to lymphocytes.
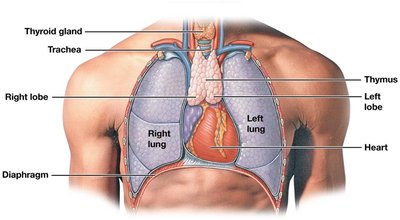
Thymus: Site of T cell development and maturation; produces thymosin.
Spleen: Filters blood, removes abnormal blood cells, stores iron, and initiates immune responses to blood-borne antigens.
Innate (Nonspecific) Immunity
Overview of Innate Defenses
Innate immunity provides the first line of defense against pathogens. It is present at birth and does not distinguish between different threats. Major components include physical barriers, phagocytes, immune surveillance, interferons, complement, inflammation, and fever.
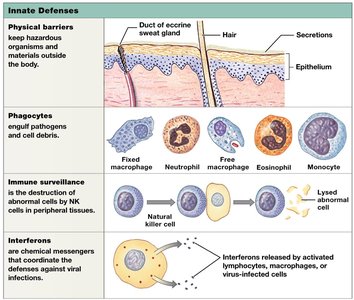
Physical Barriers
Skin, hair, and mucous membranes prevent pathogen entry.
Secretions (sweat, urine, mucus) flush away materials and may contain enzymes, antibodies, or acids that kill or inhibit microorganisms.
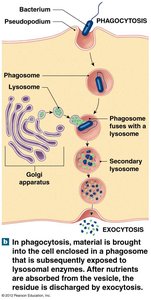
Phagocytes
Cells that engulf and destroy microorganisms and debris.
Microphages: Neutrophils and eosinophils, which enter tissues to fight infection.
Macrophages: Large phagocytic cells derived from monocytes; can be fixed (in specific tissues) or free (wandering).
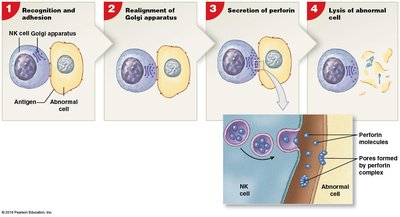
Immune Surveillance
Carried out by natural killer (NK) cells that detect and destroy abnormal cells (e.g., cancer or virus-infected cells).
NK cells recognize abnormal antigens, realign their Golgi apparatus, secrete perforins, and lyse the target cell.
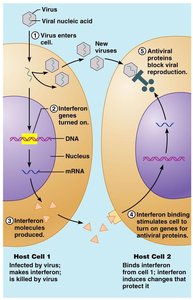
Interferons
Small proteins (cytokines) released by activated lymphocytes, macrophages, and virus-infected cells.
Trigger production of antiviral proteins in neighboring cells, blocking viral replication.
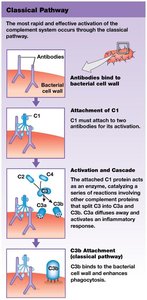
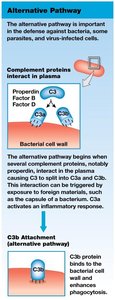
Complement System
Over 30 plasma proteins that assist antibodies in destroying pathogens.
Activated via three pathways: classical, lectin, and alternative.
All pathways lead to the activation of C3, producing C3a (inflammation) and C3b (opsonization, MAC formation).
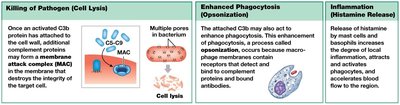
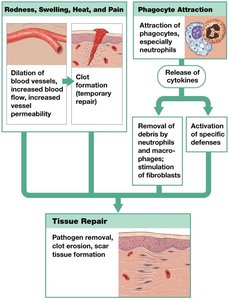
Inflammation
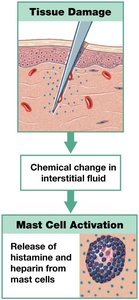
Localized tissue response to injury, characterized by redness, swelling, heat, and pain.
Triggered by mast cell release of histamine and heparin, increasing capillary permeability and blood flow.
Mobilizes defenses, slows pathogen spread, and initiates tissue repair.
Fever
Elevated body temperature (>37.2ºC) induced by pyrogens.
Increases metabolic rate and may inhibit some pathogens.
Adaptive (Specific) Immunity
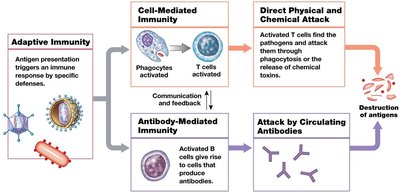
Overview of Adaptive Defenses
Adaptive immunity is mediated by lymphocytes (T cells and B cells) and develops after exposure to specific antigens. It provides long-term protection and memory against previously encountered pathogens.
Types of Adaptive Immunity
Active immunity: Develops after exposure to an antigen (naturally or via vaccination).
Passive immunity: Acquired by receiving antibodies from another source (e.g., maternal antibodies, antibody injection).
Properties of Adaptive Immunity
Specificity: Each lymphocyte responds to a specific antigen.
Versatility: Immune system can recognize a vast array of antigens.
Memory: Memory cells provide rapid response to previously encountered antigens.
Tolerance: Immune system ignores self-antigens.
T Cells and Immunity
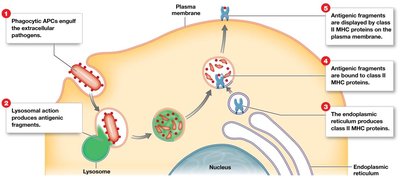
Antigen presentation: T cells recognize antigens presented by MHC proteins on antigen-presenting cells (APCs).
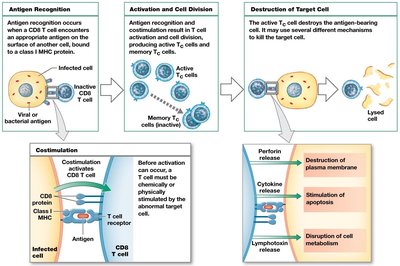
Class I MHC: Found on all nucleated cells; present endogenous antigens to CD8+ T cells.
Class II MHC: Found on APCs and lymphocytes; present exogenous antigens to CD4+ T cells.
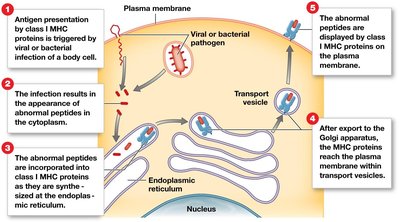
CD Markers and T Cell Activation
CD8 markers: On cytotoxic and regulatory T cells; respond to class I MHC.
CD4 markers: On helper T cells; respond to class II MHC.
Costimulation: Second signal required for T cell activation.
B Cells and Immunity
B cell sensitization: Antigen binds to B cell receptor, is internalized, processed, and presented on class II MHC.
B cell activation: Helper T cell provides cytokines, leading to B cell division and differentiation into plasma cells (antibody production) and memory B cells.
Antibodies: Soluble proteins with two heavy and two light chains; variable regions form antigen-binding sites.
Immunoglobulin classes: IgG, IgE, IgD, IgM, IgA.
Antigen–Antibody Interactions
Antigen–antibody complex: Antibody bound to antigen; leads to immune response.
Hapten: Partial antigen that must bind a carrier to elicit a response (e.g., penicillin allergy).
Actions of Antibodies
Neutralization of pathogens/toxins.
Precipitation and agglutination (immune complex formation).
Activation of complement system.
Attraction of phagocytes and opsonization.
Stimulation of inflammation.
Prevention of bacterial/viral adhesion.
Immune Responses to Antigen Exposure
Primary response: Slow, with IgM produced first, followed by IgG.
Secondary response: Rapid and strong due to memory cells; IgG rises quickly and remains elevated.
