 Back
BackThe Male Reproductive System: Structure, Function, and Regulation
Study Guide - Smart Notes

The Reproductive System: Overview
Introduction to the Reproductive System
The reproductive system is unique among organ systems in that it does not function continuously and only becomes active at puberty. Its primary role is to ensure the continuation of the species through sexual reproduction. Both male and female reproductive systems share four main tasks:
Formation of gametes: Sperm in males and ova (eggs) in females.
Bringing gametes together: Through sexual intercourse (copulation).
Fertilization: Fusion of gametes to form a zygote, the first cell of a new individual.
Support of fetal development and birth: Gestation and parturition.
Common Features of Male and Female Reproductive Systems
Gonads and Accessory Organs
Male and female reproductive structures are homologous, sharing a common developmental origin. The primary sex organs (gonads) are the testes in males and ovaries in females. These organs produce:
Gametes: Sperm and ova, formed by meiosis.
Sex hormones: Testosterone in males; estrogens and progesterone in females. These hormones regulate reproductive organ development, sexual behavior, and secondary sexual characteristics.
Accessory reproductive organs include ducts, glands, and external genitalia.
Regulation of Reproductive Hormone Secretion
The Hypothalamic-Pituitary-Gonadal (HPG) Axis
The production of gametes and sex hormones is regulated by the HPG axis, involving the hypothalamus, anterior pituitary gland, and gonads. Key hormones include:
GnRH (Gonadotropin-releasing hormone): Released from the hypothalamus, stimulates the anterior pituitary.
FSH (Follicle-stimulating hormone) and LH (Luteinizing hormone): Released from the anterior pituitary, stimulate the gonads.
Sex hormones: Testosterone, estrogen, and progesterone act on target tissues and exert negative feedback on the hypothalamus and pituitary.
Inhibin: Released from the gonads, inhibits FSH release.
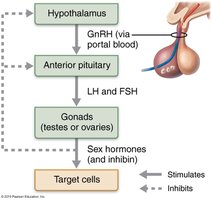
Activation at Puberty
At puberty, the hypothalamus becomes less sensitive to inhibition by sex hormones, leading to increased GnRH, FSH, and LH secretion, which in turn stimulates gonadal hormone production and gametogenesis.
Meiosis and Gametogenesis
Overview of Meiosis
Meiosis is a specialized form of nuclear division that reduces the chromosome number by half, producing haploid gametes. This process ensures genetic diversity and prevents chromosome doubling in each generation.
Diploid (2n): Normal chromosome number in body cells (46 in humans).
Haploid (n): Chromosome number in gametes (23 in humans).
Homologous chromosomes: One from each parent, carrying genes for the same traits.
Crossing over: Exchange of genetic material between nonsister chromatids during meiosis I, increasing genetic variability.
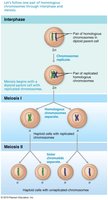
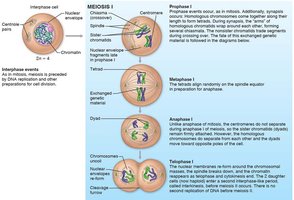
Phases of Meiosis
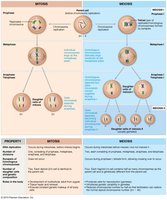
Meiosis consists of two consecutive divisions: meiosis I (reduction division) and meiosis II (equational division). Each division includes prophase, metaphase, anaphase, and telophase.
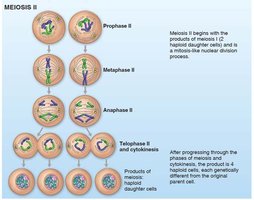
Comparison of Mitosis and Meiosis
Mitosis produces genetically identical diploid cells for growth and repair, while meiosis produces genetically unique haploid gametes for reproduction.
Feature | Mitosis | Meiosis |
|---|---|---|
Number of divisions | 1 | 2 |
Number of daughter cells | 2 (diploid) | 4 (haploid) |
Genetic variability | None | High (crossing over, independent assortment) |
Function | Growth, repair | Gamete production |
Anatomy of the Male Reproductive System
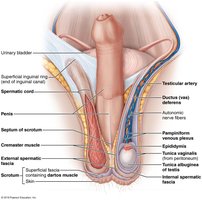
Testes and Scrotum
The testes are the male gonads, producing sperm and testosterone. They are housed in the scrotum, which maintains a temperature lower than core body temperature, essential for spermatogenesis. The scrotum contains muscles (dartos and cremaster) that regulate testicular position and temperature.
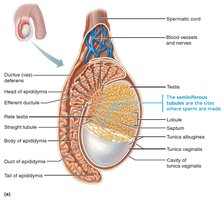
Structure of the Testis
Each testis is divided into lobules containing seminiferous tubules, the site of sperm production. Sperm travel from the seminiferous tubules to the epididymis via a network of ducts.
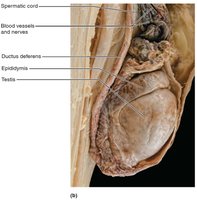
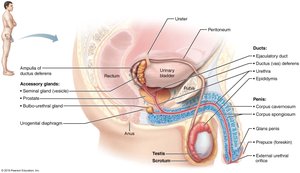
Male Duct System
Sperm are transported from the testes to the exterior through a series of ducts: epididymis, ductus deferens, ejaculatory duct, and urethra. The epididymis is the site of sperm maturation and storage.
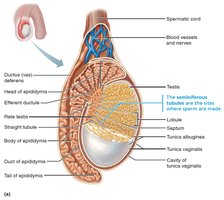
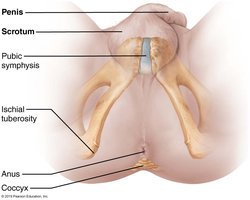
Penis and Male Perineum
The penis is the male copulatory organ, consisting of erectile tissues (corpora cavernosa and corpus spongiosum) and the urethra. The perineum is the diamond-shaped region containing the root of the penis and anus.
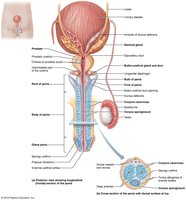
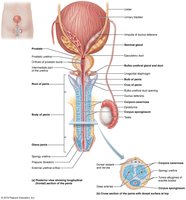
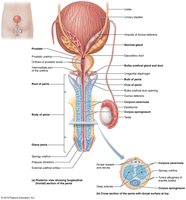
Accessory Glands
Male accessory glands include the seminal vesicles, prostate, and bulbo-urethral glands. These glands produce seminal fluid, which nourishes and protects sperm, and facilitates their movement.
Male Sexual Response
Erection and Ejaculation
Erection is caused by increased blood flow to the erectile tissues, mediated by parasympathetic stimulation and nitric oxide release. Ejaculation is a sympathetic reflex resulting in the expulsion of semen, followed by a refractory period.
Spermatogenesis
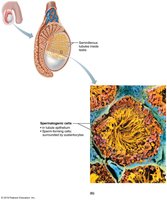
Process of Spermatogenesis
Spermatogenesis is the process of sperm production in the seminiferous tubules, beginning at puberty and continuing throughout life. It involves three main steps:
Mitosis of spermatogonia: Produces primary spermatocytes.
Meiosis: Primary spermatocytes undergo meiosis I and II to form spermatids.
Spermiogenesis: Spermatids mature into spermatozoa (sperm).
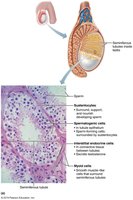
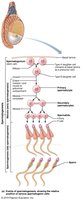
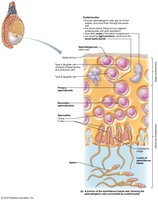
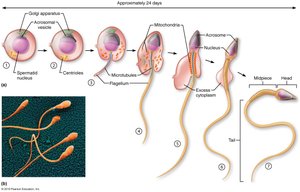
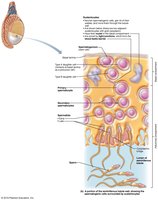
Role of Sustentocytes (Sertoli Cells)
Sustentocytes support and nourish developing sperm, form the blood-testis barrier, and secrete factors that regulate spermatogenesis, including androgen-binding protein (ABP) and inhibin.
Regulation of Male Reproductive Function
Hormonal Regulation by the HPG Axis
The HPG axis regulates spermatogenesis and testosterone production through a feedback loop involving GnRH, FSH, LH, testosterone, and inhibin.
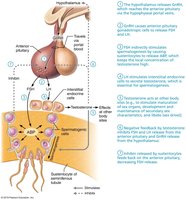
Testosterone and Male Secondary Sex Characteristics
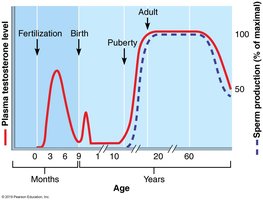
Testosterone is essential for spermatogenesis, development of male secondary sex characteristics (e.g., facial hair, deep voice, increased muscle mass), and maintenance of libido. Its levels are regulated throughout life, peaking at puberty and declining with age.
Clinical Considerations
Testicular cancer: Most common in young men; risk factors include cryptorchidism and mumps-related orchitis.
Benign prostatic hyperplasia: Age-related prostate enlargement causing urinary difficulties.
Prostate cancer: Common in older men; screening includes digital exam and PSA levels.
Erectile dysfunction: Often due to vascular or neurological issues; treatments include drugs that enhance nitric oxide effects.
Infertility: Can result from environmental toxins, hormonal imbalances, or lifestyle factors.
