 Back
BackThe Male Reproductive System: Structure, Function, and Spermatogenesis
Study Guide - Smart Notes

The Male Reproductive System
Overview of the Reproductive System
The reproductive system is essential for the production of offspring and the continuation of genetic material. It consists of primary sex organs (gonads) and accessory reproductive organs. The primary sex organs are the testes in males and ovaries in females, which produce gametes (sperm and ova) and secrete steroid sex hormones such as androgens, estrogens, and progesterone.
Primary Sex Organs (Gonads): Testes (male), Ovaries (female)
Accessory Reproductive Organs: Ducts, glands, and external genitalia
Sex Hormones: Regulate development, sexual behavior, and influence other organs and tissues
Male Reproductive Anatomy
Testes and Scrotum
The testes are the site of sperm production and are housed within the scrotum, a sac of skin and superficial fascia that hangs outside the abdominopelvic cavity. The scrotum maintains a temperature approximately 3°C lower than body temperature, which is necessary for proper sperm development. Temperature is regulated by the dartos and cremaster muscles.
Dartos Muscle: Smooth muscle that wrinkles the scrotal skin and pulls the scrotum closer to the body.
Cremaster Muscle: Skeletal muscle bands that elevate the testes.
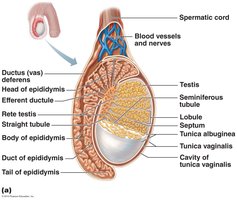
Testicular Structure
Each testis is surrounded by two tunics: the outer tunica vaginalis (derived from the peritoneum) and the inner tunica albuginea (fibrous capsule). Septa divide the testis into approximately 250 lobules, each containing 1–4 seminiferous tubules, which are the site of sperm production.
Seminiferous Tubules: Lined with spermatogenic cells and sustentacular (Sertoli) cells.
Interstitial Endocrine Cells: Located in the soft tissue around the tubules; produce androgens (e.g., testosterone).
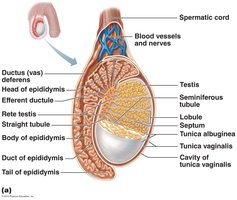
Testicular Duct System
Sperm produced in the seminiferous tubules are conveyed through a series of ducts: straight tubule, rete testis, efferent ductules, and finally the epididymis, where they mature and are stored.
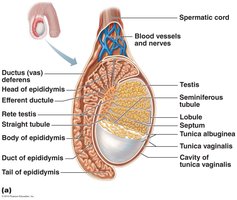
Blood Supply and Spermatic Cord
The testes receive blood from the testicular arteries and are drained by testicular veins, which form the pampiniform venous plexus. This plexus helps cool arterial blood before it reaches the testes. The spermatic cord encloses nerve fibers, blood vessels, and lymphatics supplying the testes.
The Male Perineum
The male perineum is a diamond-shaped region between the pubic symphysis, coccyx, and ischial tuberosities. It contains the root of the penis, scrotum, and anus.
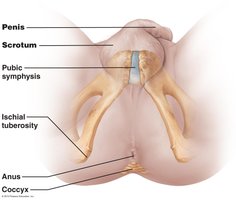
The Penis
The penis consists of a root, shaft, and glans penis. The prepuce (foreskin) covers the glans. Internally, the penis contains three cylindrical bodies of erectile tissue: the corpus spongiosum (surrounds the urethra and forms the glans and bulb) and two corpora cavernosa (dorsal erectile bodies). Erection occurs when erectile tissue fills with blood.
Male Duct System and Accessory Glands
Duct System
The ducts transport sperm from the testes to the exterior. The main ducts are the epididymis, ductus (vas) deferens, ejaculatory duct, and urethra.
Epididymis: Site of sperm maturation and storage; contracts during ejaculation to expel sperm.
Vas Deferens: Transports sperm from the epididymis to the ejaculatory duct; site of vasectomy for birth control.
Urethra: Conveys both urine and semen (at different times).
Accessory Sex Glands
Seminal Vesicles: Produce alkaline seminal fluid (fructose, citric acid, enzymes, prostaglandins); 70% of semen volume.
Prostate Gland: Secretes milky, slightly acidic fluid (citrate, enzymes, PSA); activates sperm; 1/3 of semen volume.
Bulbourethral (Cowper’s) Glands: Produce thick, clear mucus for lubrication and neutralization of acidic urine in the urethra.
Semen
Semen is a milky-white mixture of sperm and accessory gland secretions. It contains nutrients (fructose for ATP production), enzymes, and substances that enhance sperm motility and survival. Semen is alkaline, which helps neutralize the acidity of the male urethra and female vagina.
Volume: 2–5 ml per ejaculation, containing 20–150 million sperm/ml
Functions: Provides energy, protects and activates sperm, suppresses female immune response, and contains antibacterial agents
Spermatogenesis and Meiosis
Overview of Spermatogenesis
Spermatogenesis is the process of sperm production in the seminiferous tubules. It begins at puberty and continues throughout life. The process involves mitosis, meiosis, and spermiogenesis.
Spermatogonia: Stem cells that divide by mitosis to produce type A (remain as stem cells) and type B (become primary spermatocytes) cells.
Primary Spermatocytes: Undergo meiosis I to form secondary spermatocytes.
Secondary Spermatocytes: Undergo meiosis II to form spermatids.
Spermiogenesis: Spermatids mature into spermatozoa (sperm).
Meiosis: Reduction Division
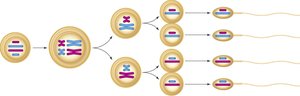
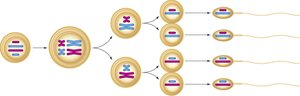
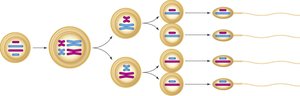
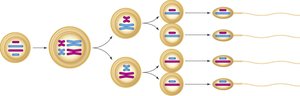
Meiosis is a specialized type of cell division that reduces the chromosome number by half, producing four haploid cells from one diploid cell. This process introduces genetic diversity through crossing over and independent assortment.
Meiosis I: Homologous chromosomes separate, reducing chromosome number from diploid (2n) to haploid (n).
Meiosis II: Sister chromatids separate, similar to mitosis, resulting in four haploid cells.

Phases of Meiosis
Phase | Description |
|---|---|
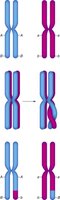
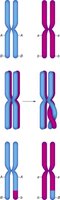
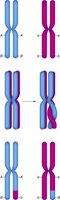
Prophase I | Homologous chromosomes pair and exchange segments (crossing over) |
Metaphase I | Paired homologous chromosomes align at the cell equator |
Anaphase I | Homologous chromosomes separate to opposite poles |
Telophase I | Two haploid cells form; chromosomes are still duplicated |
Prophase II | Chromosomes condense in each haploid cell |
Metaphase II | Chromosomes align at the equator in each haploid cell |
Anaphase II | Sister chromatids separate to opposite poles |
Telophase II | Four haploid cells form, each with unduplicated chromosomes |





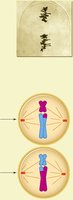
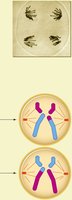
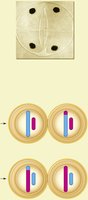
Genetic Variation in Meiosis
Crossing over during prophase I and the random assortment of chromosomes during metaphase I contribute to genetic diversity in gametes. This ensures that each sperm cell is genetically unique.
Sperm Structure
Mature sperm have three main regions:
Head: Contains the nucleus and acrosome (enzymes for egg penetration)
Midpiece: Packed with mitochondria for ATP production
Tail: Flagellum for motility
Summary Table: Male Reproductive Structures and Functions
Structure | Function |
|---|---|
Testes | Produce sperm and testosterone |
Scrotum | Maintains optimal temperature for spermatogenesis |
Epididymis | Stores and matures sperm |
Vas Deferens | Transports sperm during ejaculation |
Seminal Vesicles | Produce seminal fluid (nutrients, enzymes) |
Prostate Gland | Secretes fluid for sperm activation |
Bulbourethral Glands | Lubrication and neutralization of urethra |
Penis | Delivers sperm into the female reproductive tract |
