 Back
BackThe Parathyroid Glands and Calcium Homeostasis
Study Guide - Smart Notes

The Endocrine System
The Parathyroid Glands: Structure and Function
The parathyroid glands are small, yellow-brown endocrine glands located on the posterior aspect of the thyroid gland. Most individuals have four parathyroid glands, but the number can vary, and some may be found in other regions of the neck or thorax. These glands are composed of two main cell types: parathyroid cells, which secrete parathyroid hormone (PTH), and oxyphil cells, whose function remains unclear.
Parathyroid cells: Responsible for the synthesis and secretion of PTH, the primary hormone regulating blood calcium levels.
Oxyphil cells: Larger cells with an unknown function, present in smaller numbers.
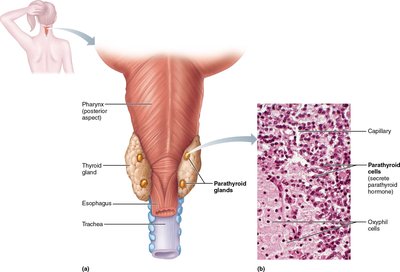
Figure: Anatomy and histology of the parathyroid glands, showing their location behind the thyroid gland and the cellular composition (parathyroid cells and oxyphil cells).
Parathyroid Hormone (PTH) and Calcium Homeostasis
Parathyroid hormone (PTH), also known as parathormone, is the most important hormone for controlling calcium balance in the blood. Calcium homeostasis is essential for physiological processes such as nerve impulse transmission, muscle contraction, and blood clotting. The secretion of PTH is regulated by blood calcium levels through a negative feedback mechanism:
Falling blood calcium levels stimulate PTH release.
Rising blood calcium levels inhibit PTH release.
PTH acts on three main target organs to increase blood calcium levels:
Skeleton: Stimulates osteoclasts to resorb bone matrix, releasing calcium and phosphate into the blood.
Kidneys: Enhances reabsorption of calcium from urine and increases phosphate excretion.
Intestine: Promotes activation of vitamin D in the kidneys, which increases calcium absorption from the diet in the small intestine.
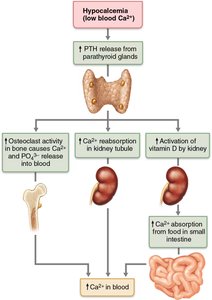
Figure: Mechanism of PTH action on calcium homeostasis. PTH release is triggered by low blood calcium, leading to increased calcium release from bone, reabsorption in the kidneys, and absorption from the intestine.
Key Equation:
Vitamin D Activation: PTH stimulates the conversion of vitamin D to its active form, calcitriol, in the kidneys. Calcitriol is necessary for efficient dietary calcium absorption.
Clinical Imbalances of Parathyroid Function
Disorders of parathyroid hormone secretion can lead to significant clinical consequences:
Hyperparathyroidism (excess PTH): Often caused by a parathyroid tumor, leading to excessive bone resorption, bone deformities, and spontaneous fractures (osteitis fibrosa cystica). Hypercalcemia (high blood calcium) can depress the nervous system, cause muscle weakness, and result in kidney stones due to calcium salt precipitation.
Hypoparathyroidism (PTH deficiency): Usually follows parathyroid gland trauma or removal during thyroid surgery. Hypocalcemia (low blood calcium) increases neuronal excitability, causing tingling, muscle twitching (tetany), convulsions, and, if untreated, respiratory paralysis and death.
Disorder | Cause | Main Effects |
|---|---|---|
Hyperparathyroidism | Parathyroid tumor | Bone softening, fractures, nervous system depression, kidney stones |
Hypoparathyroidism | Gland trauma/removal | Tetany, convulsions, respiratory paralysis |
Example: A patient with a parathyroid tumor may present with bone pain, frequent fractures, and kidney stones due to hyperparathyroidism-induced hypercalcemia.
