 Back
BackThe Renal System: Structure and Function
Study Guide - Smart Notes

The Renal System
Overview and Functions
The renal system, also known as the urinary system, is essential for maintaining homeostasis by regulating water volume, solute concentration, and acid-base balance. The kidneys are the primary excretory organs, responsible for filtering blood, removing metabolic wastes, and producing hormones.
Excretory Functions: Removal of metabolic wastes, toxins, and drugs from the body.
Regulation: Controls water volume, solute concentration, and acid-base balance.
Hormone Production: Produces erythropoietin (stimulates red blood cell production) and renin (regulates blood pressure).
Other Functions: Activates vitamin D and performs gluconeogenesis during prolonged fasting.
Major Components of the Urinary System
Kidneys: Filter blood to form urine.
Ureters: Transport urine from kidneys to urinary bladder.
Urinary Bladder: Temporarily stores urine.
Urethra: Conducts urine out of the body.
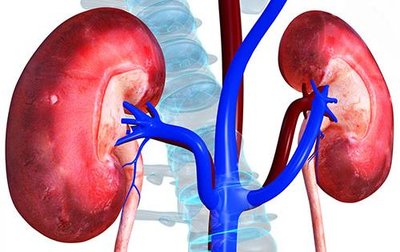
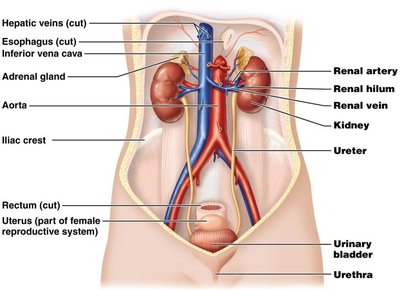
Kidney Anatomy
External Anatomy
The kidneys are retroperitoneal organs located between the T9 and L2 vertebrae. The right kidney is slightly lower due to the position of the liver.
Renal Hilum: The concave medial surface where blood vessels, nerves, and the ureter enter and exit.
Renal Sinus: Internal cavity within the kidney.
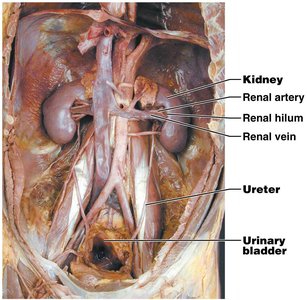
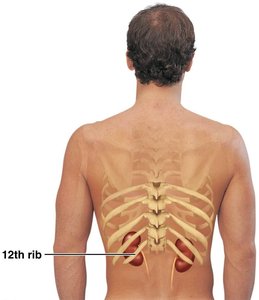
Protective Layers of the Kidney
Renal Fascia: Outermost dense fibrous connective tissue anchoring the kidney.
Perirenal Fat Capsule: Fatty cushion that protects and supports the kidney.
Fibrous Renal Capsule: Thin, tough layer that prevents infection spread to the kidney.
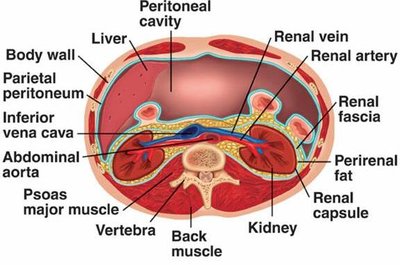
Internal Anatomy
Renal Cortex: The outer region of the kidney.
Renal Medulla: The inner region, containing renal pyramids.
Renal Pyramids: Cone-shaped tissues in the medulla.
Renal Columns: Extensions of cortex between pyramids.
Renal Pelvis: Funnel-shaped tube that collects urine and channels it to the ureter.
Calyces (Minor and Major): Collect urine from pyramids and pass it to the renal pelvis.
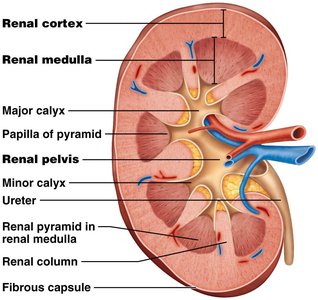
Clinical Correlations
Renal Ptosis
Renal ptosis is a condition where the kidney drops to a lower position due to a deficiency of supporting pararenal fascia. This can cause the ureter to become kinked, leading to urine backup.
Hydronephrosis
Hydronephrosis is the swelling of a kidney due to a build-up of urine, often caused by an obstruction such as a ureteral stone. This can severely damage the kidney if untreated.
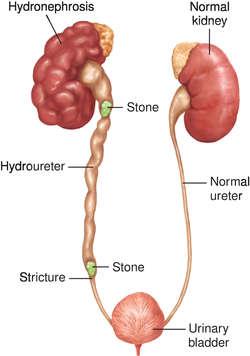
Pyelitis and Pyelonephritis
Pyelitis: Infection of the renal pelvis and calyces.
Pyelonephritis: Infection of the entire kidney, which may result in pus accumulation and, if untreated, permanent kidney damage.
Treatment: Antibiotics are typically effective.
Etiology: Most common in females, often due to fecal bacteria entering via the urethra.
Blood and Nerve Supply
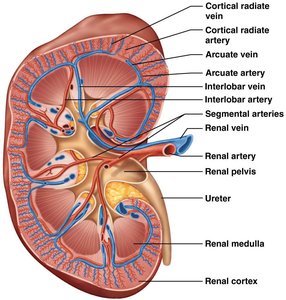
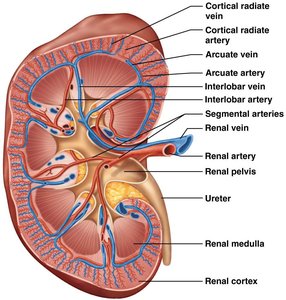
Renal Blood Supply
The kidneys receive about one-fourth of the cardiac output via the renal arteries. The blood supply is crucial for filtration and homeostasis.
Renal Arteries: Branch from the abdominal aorta and enter the kidneys at the hilum.
Renal Veins: Drain filtered blood from the kidneys into the inferior vena cava.
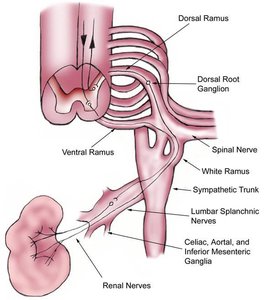
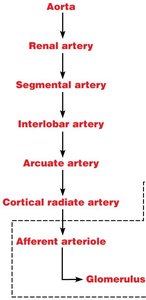
Nerve Supply
The kidneys are innervated by sympathetic fibers from the renal plexus, which regulate blood flow and influence urine formation.
Nephrons: The Functional Units of the Kidney
Structure of Nephrons
Nephrons are the microscopic structural and functional units of the kidney, responsible for urine formation. Each kidney contains over one million nephrons.
Renal Corpuscle: Consists of the glomerulus and glomerular (Bowman's) capsule.
Renal Tubule: Composed of the proximal convoluted tubule, nephron loop (loop of Henle), and distal convoluted tubule.
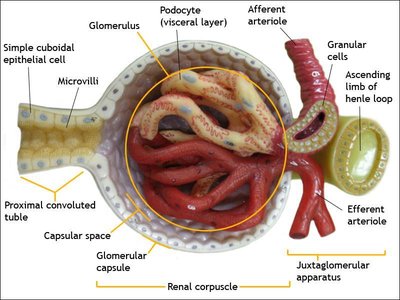
Renal Corpuscle
Glomerulus: A tuft of fenestrated capillaries specialized for filtration.
Glomerular Capsule (Bowman's Capsule): Surrounds the glomerulus and consists of two layers:
Parietal Layer: Simple squamous epithelium.
Visceral Layer: Made of podocytes with foot processes that form filtration slits, allowing filtrate to enter the capsular space.
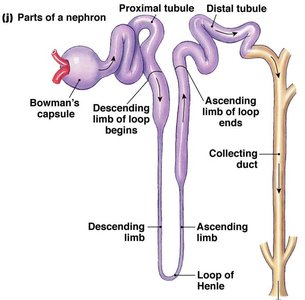
Renal Tubule and Collecting Duct
Proximal Convoluted Tubule (PCT): Lined with cuboidal cells with dense microvilli for reabsorption and secretion; confined to the cortex.
Nephron Loop (Loop of Henle): Has descending (thin, simple squamous) and ascending (thick, cuboidal or columnar) limbs.
Distal Convoluted Tubule (DCT): Cuboidal cells with few microvilli; primarily involved in secretion; confined to the cortex.
Collecting Ducts: Receive filtrate from multiple nephrons, run through medullary pyramids, and deliver urine to the minor calyces.

Classes of Nephrons
Cortical Nephrons: 85% of nephrons; almost entirely in the cortex.
Juxtamedullary Nephrons: Long nephron loops that deeply invade the medulla; essential for producing concentrated urine.
Nephron Capillary Beds
Types of Capillary Beds
Glomerulus: Specialized for filtration; fed and drained by arterioles (afferent and efferent).
Peritubular Capillaries: Low-pressure, porous capillaries adapted for absorption; arise from efferent arterioles and surround renal tubules in the cortex.
Vasa Recta: Long, straight capillaries parallel to nephron loops of juxtamedullary nephrons; play a role in forming concentrated urine.

Glomerulus Capillary Beds
High Blood Pressure: The afferent arteriole is larger in diameter than the efferent arteriole, resulting in high pressure that favors filtration.
Peritubular Capillaries and Vasa Recta
Peritubular Capillaries: Adapted for absorption of water and solutes from the filtrate.
Vasa Recta: Maintain the osmotic gradient in the medulla, crucial for urine concentration.
Summary Table: Main Structures and Functions of the Renal System
Structure | Main Function |
|---|---|
Kidney | Filtration of blood, urine formation, regulation of fluid/electrolyte balance |
Ureter | Transport urine from kidney to bladder |
Urinary Bladder | Temporary storage of urine |
Urethra | Conducts urine out of the body |
Nephron | Filtration, reabsorption, secretion, urine concentration |
Key Equations
Glomerular Filtration Rate (GFR):
Renal Clearance (C):
Where: U = concentration of substance in urine V = flow rate of urine formation P = concentration of substance in plasma
Additional info: The above equations are fundamental for assessing kidney function in clinical practice.
