 Back
BackThe Reproductive System: Structure, Function, and Development
Study Guide - Smart Notes

The Reproductive System
Overview of the Reproductive System
The reproductive system is responsible for producing, maintaining, and transporting gametes (sperm in males, ova in females), as well as secreting sex hormones. It ensures the continuation of species through sexual reproduction and supports the development of offspring.
Gonads: Primary sex organs (testes in males, ovaries in females) that produce gametes and hormones.
Gametes: Sperm (male), ova or eggs (female).
Accessory structures: Ducts and glands that support gamete transport and reproductive function.
Anatomy of the Male Reproductive System
Gross Structure and Duct System
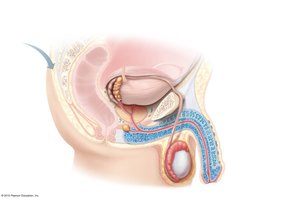
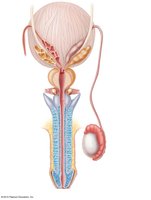
The male reproductive system includes both internal and external structures that function in the production, maturation, and delivery of sperm.
Testes: Produce sperm and testosterone; surrounded by the tunica albuginea and divided into lobules containing seminiferous tubules.
Epididymis: Site of sperm maturation and storage; sperm gain motility here.
Ductus (vas) deferens: Transports sperm from the epididymis to the ejaculatory duct via peristalsis.
Urethra: Shared terminal duct for urine and semen; divided into prostatic, membranous, and spongy (penile) regions.
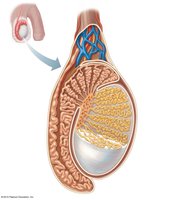
Testicular Microanatomy
Each testis is divided into lobules containing seminiferous tubules, where spermatogenesis occurs. Interstitial cells between tubules produce testosterone.
Tunica albuginea: Fibrous capsule surrounding the testis.
Seminiferous tubules: Sperm-forming structures.
Rete testis: Network collecting sperm from tubules, leading to the epididymis.
Accessory Glands and Semen
Accessory glands produce seminal fluid, which nourishes and protects sperm, forming semen.
Seminal vesicles: Secrete fructose-rich fluid (energy for sperm).
Prostate gland: Secretes milky fluid that activates sperm.
Bulbo-urethral glands: Produce mucus for lubrication and neutralization of acidic urine.
Semen: Mixture of sperm and glandular secretions; alkaline to neutralize vaginal acidity, contains nutrients and motility enhancers.
Spermatogenesis and Sperm Structure
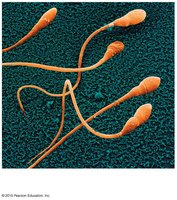
Spermatogenesis is the process of sperm cell formation, beginning at puberty and continuing throughout life. Mature sperm have specialized structures for motility and fertilization.
Head: Contains nucleus and acrosome (enzymes for egg penetration).
Midpiece: Packed with mitochondria for energy.
Tail: Flagellum for motility.
Testosterone and Male Secondary Sex Characteristics
Testosterone, produced by interstitial cells, is essential for male reproductive organ development, sex drive, and secondary sex characteristics.
Deepening of the voice
Increased hair growth
Enlargement of skeletal muscles
Increased bone growth and density
Anatomy of the Female Reproductive System
Gross Structure and Duct System
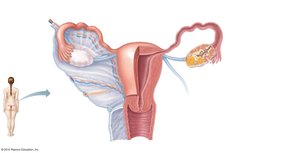
The female reproductive system includes structures for egg production, fertilization, and support of fetal development.
Ovaries: Produce ova and hormones (estrogen, progesterone); contain follicles at various stages of development.
Uterine (fallopian) tubes: Receive ovulated oocyte, site of fertilization, transport to uterus.
Fimbriae: Fingerlike projections that help capture the oocyte.
Uterus: Muscular organ for implantation and nourishment of embryo; regions include body, fundus, and cervix.
Vagina: Canal for menstrual flow, intercourse, and childbirth.
Ovarian and Uterine Cycles
The ovarian cycle involves the maturation and release of an oocyte (ovulation), while the uterine (menstrual) cycle prepares the endometrium for possible implantation.
Oogenesis: Production of ova; begins before birth, resumes at puberty, ends at menopause.
Ovulation: Release of mature oocyte, typically every 28 days.
Menstrual cycle phases:
Menstrual phase (days 1-5): Shedding of endometrium.
Proliferative phase (days 6-14): Endometrial repair and ovulation.
Secretory phase (days 15-28): Endometrium prepares for implantation.
Hormonal Regulation and Female Secondary Sex Characteristics
Estrogens and progesterone regulate the female reproductive cycle and secondary sex characteristics.
Estrogens: Breast development, pubic/axillary hair, fat distribution, pelvic widening, onset of menses.
Progesterone: Maintains pregnancy, prepares breasts for milk production.
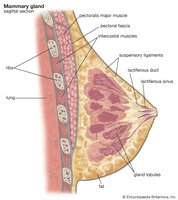
Mammary Glands
Mammary glands are modified sweat glands that produce milk in response to hormonal stimulation, functioning only in females.
Stimulated by estrogens to increase in size during puberty and pregnancy.
Fertilization and Embryonic Development
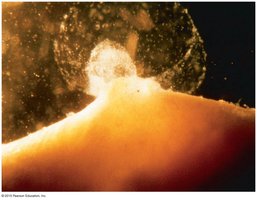
Fertilization
Fertilization occurs when a sperm cell fuses with an oocyte, forming a zygote. The oocyte is viable for about 24 hours post-ovulation, while sperm can survive several days in the female tract.
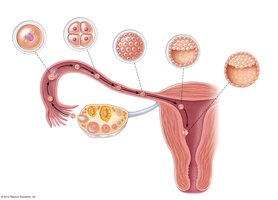
Zygote: First cell of a new individual, with a full set of chromosomes (2n = 46).
Cleavage: Rapid mitotic divisions of the zygote, forming a morula and then a blastocyst.
Implantation: Blastocyst embeds in the endometrium by day 14 post-ovulation.
Embryonic and Fetal Development
Development proceeds from zygote to embryo (weeks 1-8) to fetus (week 9 to birth). The placenta forms to support the growing conceptus.
Placenta: Delivers nutrients/oxygen, removes wastes, produces hormones to maintain pregnancy.
Gestation period: Approximately 280 days from last menstrual period to birth.
Effects of Pregnancy on the Mother
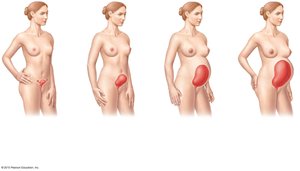
Pregnancy induces anatomical and physiological changes in the mother, including uterine enlargement and hormonal shifts.
Enlargement of uterus
Increased lumbar curvature (lordosis)
Relaxation of pelvic ligaments
Childbirth (Parturition)
Initiation of Labor
Labor is initiated by hormonal changes, including increased estrogen, prostaglandins, and oxytocin, leading to rhythmic uterine contractions and eventual delivery of the infant.
Positive feedback mechanism enhances contractions.
Braxton Hicks contractions (false labor) may occur before true labor begins.
Developmental Aspects of the Reproductive System
Puberty and Menopause
Puberty marks the onset of reproductive capability, while menopause signals the end of female reproductive function.
Males: Testes and scrotum enlarge (~age 13).
Females: Breast development and menarche (~age 11).
Menopause: Ovaries cease hormone production; reproductive ability ends; no male equivalent, but testosterone declines with age.
Comparison of Male and Female Gametogenesis
Meiosis and Gamete Structure
Meiosis produces gametes with half the chromosome number (n = 23). Males produce four functional sperm per meiosis; females produce one ovum and three polar bodies.
Sperm: Small, motile, nutrient-limited.
Ovum: Large, nonmotile, nutrient-rich.
Feature | Male (Sperm) | Female (Ovum) |
|---|---|---|
Number per meiosis | 4 | 1 (+3 polar bodies) |
Motility | Motile | Nonmotile |
Size | Small | Large |
Nutrient reserves | Minimal | Abundant |
