 Back
BackThe Respiratory System: Structure and Function
Study Guide - Smart Notes

The Respiratory System
Overview
The respiratory system is essential for gas exchange, supplying oxygen to the body and removing carbon dioxide. It consists of a series of organs and structures that facilitate the movement and exchange of gases between the atmosphere and the bloodstream.

Anatomy of the Respiratory System
Main Components
Nose and Nasal Cavity: Entryway for air, encased in cranial and facial bones.
Pharynx (Throat): Passageway for air from the nasal cavity to the larynx.
Larynx (Voice Box): Located in the anterior neck, prevents food and liquids from entering the lower respiratory tract and houses the vocal cords.
Trachea (Windpipe): Extends from the larynx into the mediastinum, conducting air to the bronchi.
Bronchial Tree: Branching tubes that distribute air to the lungs.
Lungs: Paired organs in the thoracic cavity, containing millions of alveoli for gas exchange.
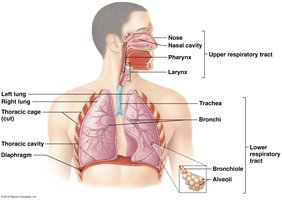
Respiratory Tract Divisions
Upper Respiratory Tract: Nasal cavity to larynx.
Lower Respiratory Tract: Trachea to alveoli.
Alveoli: Tiny air sacs where gas exchange occurs.
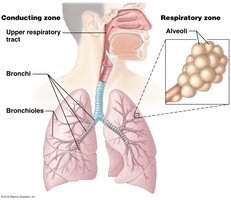
Functional Zones of the Respiratory System
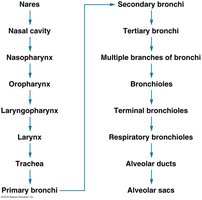
Conducting Zone
The conducting zone consists of all the respiratory passages that carry air to the sites of gas exchange. It filters, warms, and moistens air as it travels to the lungs. Structures include the nose, nasal cavity, pharynx, larynx, trachea, bronchi, and bronchioles.
Respiratory Zone
The respiratory zone is where gas exchange occurs and includes structures that contain alveoli, such as respiratory bronchioles, alveolar ducts, and alveolar sacs.
Basic Functions of the Respiratory System
Respiration: Provides oxygen to body cells and removes carbon dioxide. Involves four processes:
Pulmonary ventilation (breathing)
Pulmonary gas exchange (between lungs and blood)
Gas transport (through blood)
Tissue gas exchange (between blood and tissues)
Other Functions:
Speech and sound production
Olfaction (sense of smell)
Assists with defecation, urination, and childbirth by increasing thoracic pressure
Helps maintain acid-base balance
Synthesizes angiotensin-II for blood pressure regulation
The Nose and Nasal Cavity
Functions
Warms and humidifies inhaled air
Filters debris and secretes antibacterial substances
Houses olfactory receptors
Enhances resonance of voice
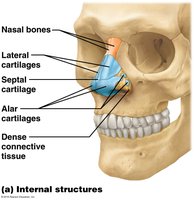
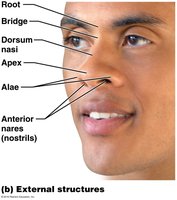
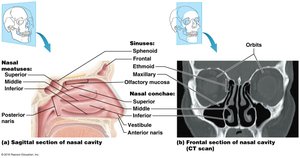
The Pharynx
Divisions
Nasopharynx: Posterior to nasal cavity; lined with respiratory epithelium.
Oropharynx: Posterior to oral cavity; passageway for food and air.
Laryngopharynx: Extends from hyoid bone to esophagus.
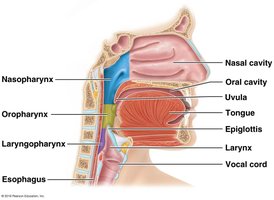
The Larynx
Structure and Function
The larynx is a cartilaginous structure that routes air and food into the proper channels and plays a role in voice production. It is supported by nine cartilages (three unpaired and three paired):
Thyroid cartilage: Largest, forms the anterior wall (Adam's apple).
Cricoid cartilage: Inferior to thyroid cartilage; provides support.
Epiglottis: Covers the glottis during swallowing to prevent aspiration.
Arytenoid, corniculate, and cuneiform cartilages: Involved in sound production and support.
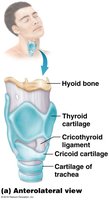
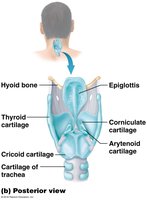
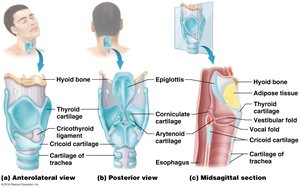
Vocal Folds
Vestibular folds (false vocal cords): Close off the glottis during swallowing.
True vocal cords: Produce sound when air passes over them; pitch and loudness are controlled by tension and force of air.
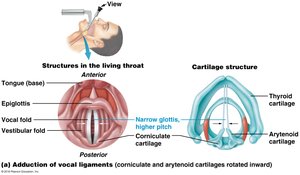
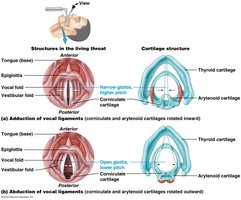
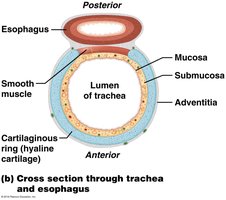
The Trachea
Structure
Extends from the larynx to the mediastinum.
Supported by C-shaped hyaline cartilage rings, which keep the airway open.
The carina is the last tracheal cartilage, containing sensory receptors that trigger the cough reflex.
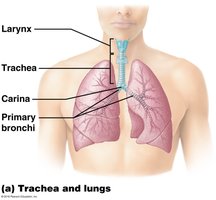
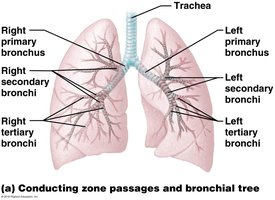
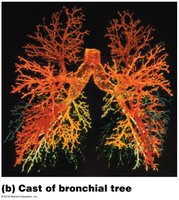
The Bronchial Tree
Branching Pattern
Primary bronchi branch into secondary bronchi (three on the right, two on the left), then into tertiary bronchi, and continue branching into smaller bronchioles.
The right primary bronchus is wider, shorter, and more vertical than the left, making it more likely for inhaled objects to enter the right lung.
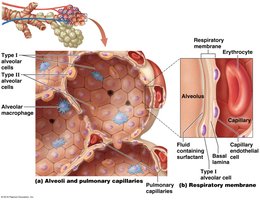
Alveoli and the Respiratory Membrane
Cell Types
Type I alveolar cells: Squamous cells for rapid gas diffusion.
Type II alveolar cells: Produce surfactant to reduce surface tension.
Alveolar macrophages: Phagocytes that remove debris and pathogens.
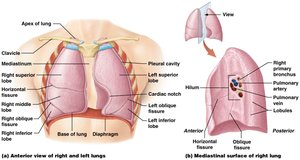
The Lungs and Pleurae
Structure
Right lung: Three lobes (superior, middle, inferior).
Left lung: Two lobes (superior, inferior) and a cardiac notch for the heart.
Each lung is divided into bronchopulmonary segments and further into lobules.
Pleurae: Double-layered serous membranes (visceral and parietal) surrounding each lung.
Pulmonary Ventilation
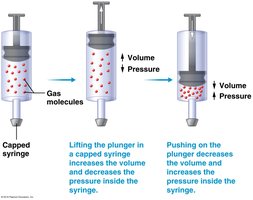
Pressure-Volume Relationship (Boyle's Law)
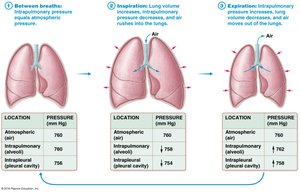
Boyle’s law states that at a constant temperature, the pressure and volume of a gas are inversely related:
As lung volume increases, pressure decreases, allowing air to flow in (inspiration).
As lung volume decreases, pressure increases, causing air to flow out (expiration).
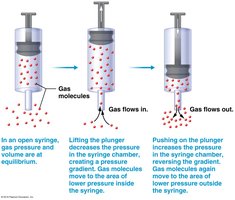
Mechanics of Breathing
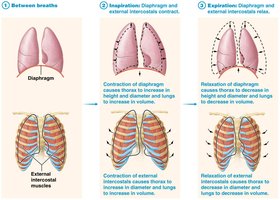
Inspiration: Diaphragm and external intercostal muscles contract, increasing thoracic volume and decreasing pressure.
Expiration: Usually passive; diaphragm relaxes, lung tissue recoils, decreasing volume and increasing pressure.
Forceful Breathing
Accessory muscles (internal intercostals, abdominal muscles) are used for forceful expiration.
The Heimlich maneuver uses abdominal thrusts to forcefully expel obstructions from the airway.
Nonrespiratory Movements
Sigh: Reopens collapsed alveoli.
Yawn: Maximizes lung volume and opens alveoli.
Sneeze: Clears irritants from the nasal cavity.
Cough: Clears the larynx, trachea, or lower airways.
Physical Factors Influencing Pulmonary Ventilation
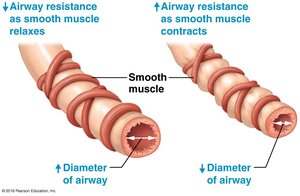
Airway Resistance: Determined by airway diameter; bronchodilation decreases resistance, bronchoconstriction increases resistance.
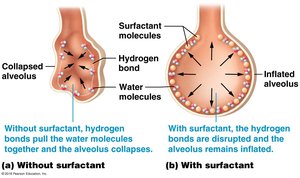
Alveolar Surface Tension: Surfactant reduces surface tension, preventing alveolar collapse (atelectasis).
Pulmonary Compliance: The ability of the lungs and chest wall to stretch.
Pulmonary Volumes and Capacities
Key Volumes
Tidal Volume (TV): Air inspired or expired during normal breathing (~500 mL).
Inspiratory Reserve Volume (IRV): Additional air that can be inhaled after a normal inspiration.
Expiratory Reserve Volume (ERV): Additional air that can be exhaled after a normal expiration.
Residual Volume (RV): Air remaining in lungs after forceful expiration.


Minute Volume and Alveolar Ventilation Rate
Minute Volume (VE):
Alveolar Ventilation Rate (VA):
Where = breaths per minute, = tidal volume, = dead space volume.
Gas Exchange
Dalton’s Law of Partial Pressures
Each gas in a mixture exerts its own pressure (partial pressure). The total pressure is the sum of all partial pressures.
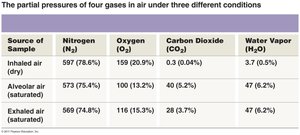
Henry’s Law
The amount of gas dissolved in a liquid is proportional to its partial pressure and solubility in the liquid.
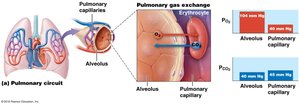
Pulmonary Gas Exchange (External Respiration)
Oxygen diffuses from alveoli (high PO2) to blood (low PO2).
Carbon dioxide diffuses from blood (high PCO2) to alveoli (low PCO2).
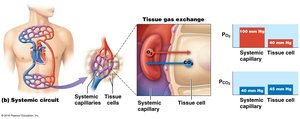
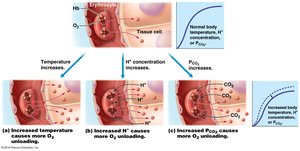
Tissue Gas Exchange (Internal Respiration)
Oxygen diffuses from blood (high PO2) to tissues (low PO2).
Carbon dioxide diffuses from tissues (high PCO2) to blood (low PCO2).
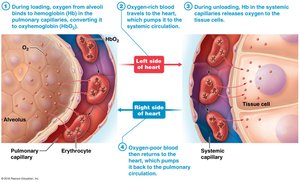
Oxygen Transport
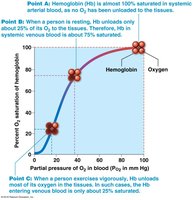
Most oxygen is transported bound to hemoglobin (Hb) in erythrocytes.
Each Hb molecule can bind four oxygen molecules.
Percent saturation of Hb depends on PO2 and Hb affinity for oxygen.
Carbon Dioxide Transport
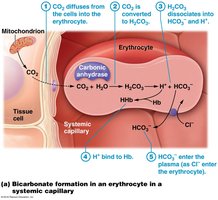
7–10% dissolved in plasma
20% bound to hemoglobin (carbaminohemoglobin)
70% as bicarbonate ions (HCO3–) in plasma, formed by the reaction:
Neural Control of Ventilation
Brainstem Centers
Medulla oblongata: Contains the respiratory rhythm generator (RRG), ventral respiratory group (VRG), and dorsal respiratory group (DRG).
Pons: Modifies respiratory rhythm.
Chemoreceptor Regulation
Central chemoreceptors: Detect changes in CO2 and H+ in cerebrospinal fluid; adjust ventilation to maintain pH homeostasis.
Peripheral chemoreceptors: Located in carotid and aortic bodies; respond to low PO2, high PCO2, and low pH.
High-Altitude Acclimatization
Gradual exposure to high altitude increases sensitivity of peripheral chemoreceptors, stimulating increased ventilation to maintain adequate oxygen levels.
