 Back
BackThe Respiratory System: Structure, Function, and Regulation
Study Guide - Smart Notes

The Respiratory System
Overview and Major Functions
The respiratory system is essential for gas exchange, supplying the body with oxygen (O2) for cellular respiration and removing carbon dioxide (CO2), a metabolic waste product. It also plays roles in regulating blood pH, olfaction, and speech. The respiratory and circulatory systems are closely linked to ensure efficient gas transport and exchange.
Respiration: The process of exchanging gases between the atmosphere, blood, and cells.
Olfaction: The sense of smell, facilitated by olfactory receptors in the nasal cavity.
Speech: Air movement through the larynx enables vocalization.
Processes of Respiration
Pulmonary ventilation: Movement of air into and out of the lungs (breathing).
External respiration: Exchange of O2 and CO2 between lungs and blood.
Transport: Movement of O2 and CO2 in the blood.
Internal respiration: Exchange of O2 and CO2 between systemic blood vessels and tissues.
Functional Anatomy of the Respiratory System
Major Organs and Divisions
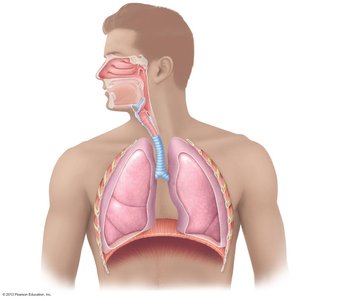
The respiratory system is divided into upper and lower regions, each with specialized structures for air conduction and gas exchange.
Upper respiratory tract: Nose, nasal cavity, paranasal sinuses, pharynx
Lower respiratory tract: Larynx, trachea, bronchi, bronchioles, lungs, alveoli
The Nose and Nasal Cavity
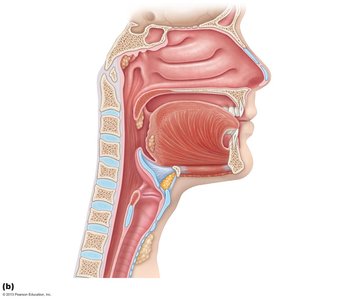
The nose provides an airway, moistens and warms incoming air, filters particles, serves as a resonating chamber for speech, and houses olfactory receptors. It consists of the external nose and the nasal cavity, which is divided by the nasal septum and lined with mucous membranes.
Nasal vestibule: Contains vibrissae (hairs) that filter large particles.
Olfactory mucosa: Contains olfactory epithelium for smell.
Respiratory mucosa: Contains mucus and serous secretions with lysozyme and defensins; cilia move mucus posteriorly.
Nasal conchae: Superior, middle, and inferior projections that increase surface area and enhance air turbulence, aiding in filtering, heating, and moistening air.
Paranasal Sinuses
Located in the frontal, sphenoid, ethmoid, and maxillary bones.
Lighten the skull, secrete mucus, warm and moisten air, and act as resonance chambers for sound.
Pharynx
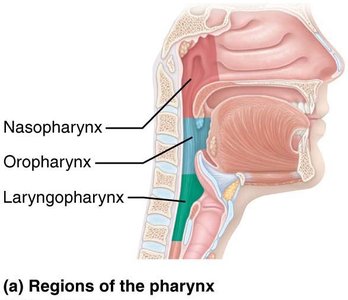
The pharynx is a muscular tube connecting the nasal cavity and mouth to the larynx and esophagus. It is divided into three regions:
Nasopharynx: Air passageway posterior to the nasal cavity; contains pharyngeal tonsil and pharyngotympanic tubes.
Oropharynx: Passageway for food and air; contains palatine and lingual tonsils.
Laryngopharynx: Passageway for food and air; continuous with the esophagus.
Lower Respiratory System
Larynx
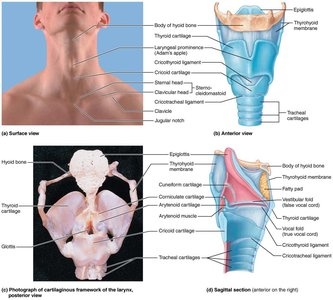
The larynx (voice box) is composed of nine cartilages (mostly hyaline), including the thyroid cartilage (Adam's apple), cricoid cartilage, and epiglottis (elastic cartilage). It routes air and food into proper channels and houses the vocal cords for sound production.
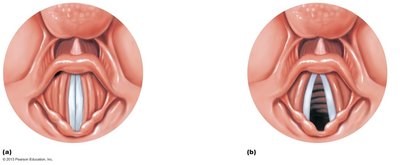
Vocal folds (true vocal cords): Vibrate to produce sound as air passes through the glottis.
Vestibular folds (false vocal cords): Superior to vocal folds; help close the glottis during swallowing.
Trachea
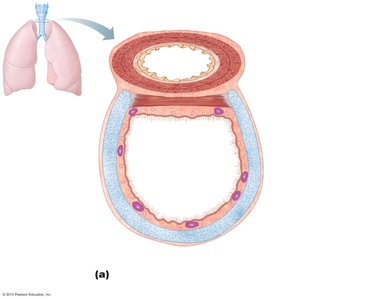
The trachea (windpipe) extends from the larynx into the mediastinum and divides into the right and left main bronchi. It is supported by C-shaped cartilage rings and contains the trachealis muscle, which contracts during coughing to expel mucus. The carina is the last tracheal cartilage, marking the point of bifurcation into the main bronchi.
Bronchial Tree and Lungs
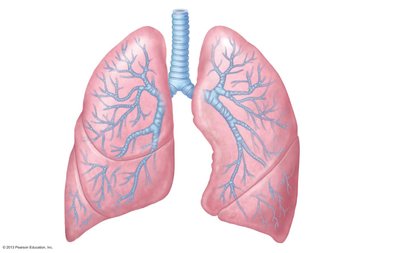
The bronchial tree consists of the branching system of bronchi and bronchioles conducting air from the trachea to the alveoli. The right main bronchus is wider, shorter, and more vertical than the left, making it more likely for foreign objects to become lodged there. The lungs are divided into lobes (three on the right, two on the left) and contain millions of alveoli for gas exchange.
Conducting zone: Trachea, bronchi, bronchioles, terminal bronchioles (no gas exchange).
Respiratory zone: Respiratory bronchioles, alveolar ducts, alveolar sacs (site of gas exchange).
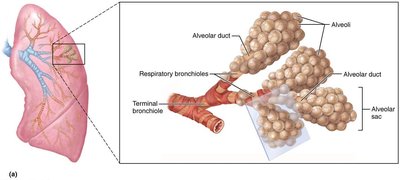
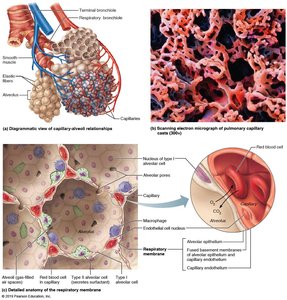
Alveoli and the Respiratory Membrane
Alveoli are tiny air sacs where gas exchange occurs. The respiratory membrane consists of alveolar and capillary walls with fused basement membranes, allowing efficient diffusion of gases. Type II alveolar cells secrete surfactant to reduce surface tension and prevent alveolar collapse. Alveolar macrophages provide immune defense.
Mechanics of Breathing
Pulmonary Ventilation
Breathing involves two phases: inspiration (air enters lungs) and expiration (air exits lungs). These processes depend on pressure differences between the atmosphere and the lungs, governed by Boyle's law:
Boyle's Law: (Pressure and volume are inversely related for a given amount of gas at constant temperature.)
During inspiration, the diaphragm and external intercostal muscles contract, increasing thoracic volume and decreasing intrapulmonary pressure, causing air to flow in. Expiration is usually passive, resulting from muscle relaxation and lung recoil.
Respiratory Volumes and Capacities
Respiratory volumes are measured to assess lung function:
Tidal volume (TV): Air moved in and out with each breath at rest (~500 mL).
Inspiratory reserve volume (IRV): Additional air inhaled after a normal inspiration.
Expiratory reserve volume (ERV): Additional air exhaled after a normal expiration.
Vital capacity (VC): Maximum air exhaled after maximum inhalation (TV + IRV + ERV).
Residual volume (RV): Air remaining in lungs after forced expiration.
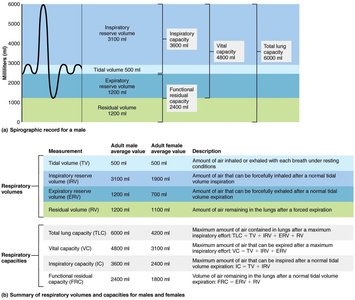
Gas Exchange and Transport
External and Internal Respiration
Gas exchange occurs by diffusion across partial pressure gradients:
External respiration: O2 moves from alveoli to blood; CO2 moves from blood to alveoli.
Internal respiration: O2 moves from blood to tissues; CO2 moves from tissues to blood.
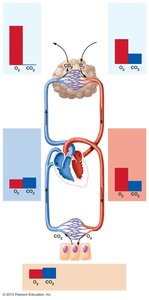
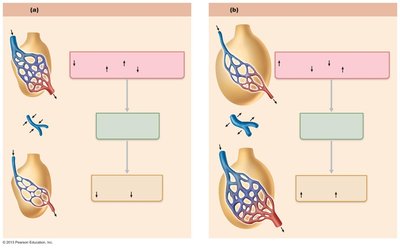
Ventilation-Perfusion Coupling
Efficient gas exchange requires matching of alveolar ventilation (airflow) and pulmonary perfusion (blood flow). Local changes in O2 and CO2 levels regulate arteriolar and bronchiolar diameter to optimize gas exchange.
Oxygen Transport
1.5% of O2 is dissolved in plasma; 98.5% is bound to hemoglobin (Hb) in red blood cells.
Each Hb molecule can bind four O2 molecules; binding is cooperative (affinity increases as O2 binds).
Factors affecting O2 unloading: partial pressure of O2, temperature, pH, PCO2, and 2,3-DPG levels.
Carbon Dioxide Transport
7–10% dissolved in plasma
20% bound to hemoglobin (carbaminohemoglobin)
70% as bicarbonate ions (HCO3–) in plasma
The reaction for CO2 transport and buffering is:
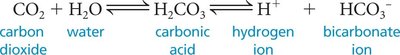
Control of Respiration
Neural Regulation
Respiratory rhythm is generated by the medullary respiratory centers (ventral and dorsal respiratory groups) and modified by the pontine respiratory centers. These centers coordinate the rate and depth of breathing in response to chemical and neural signals.
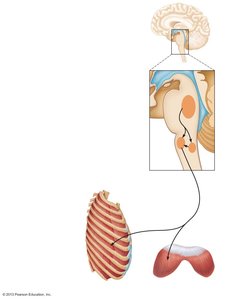
Chemical Regulation
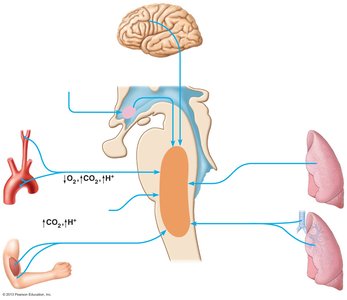
Central and peripheral chemoreceptors monitor CO2, O2, and H+ levels. The most potent stimulus for breathing is increased CO2 (hypercapnia), which lowers blood pH and stimulates increased ventilation. Peripheral chemoreceptors in the carotid and aortic bodies respond to significant drops in O2 or pH.
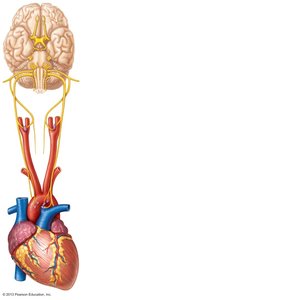
Homeostatic Imbalances and Clinical Correlations
Chronic Obstructive Pulmonary Disease (COPD): Includes chronic bronchitis and emphysema; characterized by irreversible airflow limitation, decreased lung elastance, and frequent infections.
Asthma: Reversible airway inflammation and bronchospasm, often triggered by allergens or irritants.
Tuberculosis (TB): Infectious disease caused by Mycobacterium tuberculosis.
Lung cancer: Leading cause of cancer death, strongly associated with smoking.
Cystic fibrosis: Genetic disorder causing thick, sticky mucus that obstructs airways and leads to recurrent infections.
Developmental Aspects
By the 28th week of gestation, the fetal lungs can support breathing if premature birth occurs.
At birth, lungs inflate and respiratory rate is highest in newborns, gradually decreasing with age.
