 Back
BackThe Respiratory System: Structure, Function, and Physiology
Study Guide - Smart Notes

The Respiratory System
Functions of the Respiratory System
The respiratory system is essential for gas exchange and maintaining homeostasis in the human body. It performs several critical functions:
Gas Exchange: Oxygen is absorbed and carbon dioxide is expelled.
Regulation of Blood pH: By controlling CO2 levels, the respiratory system helps regulate blood acidity.
Olfaction: Contains sensory receptors for smell.
Filtration: Filters inspired air to remove particles and pathogens.
Sound Production: The larynx produces sounds for speech.
Removal of Water and Heat: Small amounts of water and heat are lost during respiration.
Structural Components of the Respiratory System
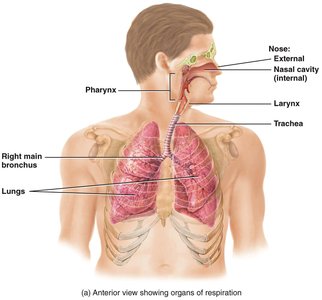
The respiratory system is divided into upper and lower tracts, each with specific anatomical features:
Upper Respiratory Tract: Includes the nose, nasal cavity, pharynx, and larynx.
Lower Respiratory Tract: Includes the trachea, bronchi, bronchioles, and lungs.
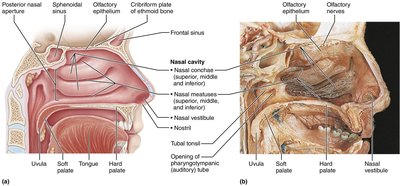
Nose and Nasal Cavity
The nose and nasal cavity filter, warm, and moisten incoming air. The nasal cavity contains conchae that increase surface area and turbulence, aiding in filtration and olfaction.
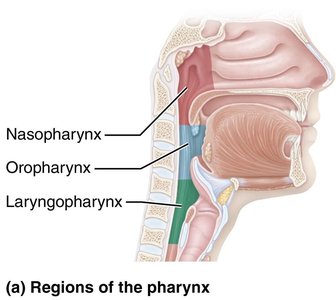
Pharynx
The pharynx is a muscular tube that serves as a passageway for air and food. It is divided into three regions:
Nasopharynx: Located behind the nasal cavity.
Oropharynx: Located behind the oral cavity.
Laryngopharynx: Located behind the larynx.
Mucous Membrane and Cilia
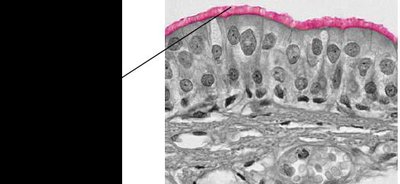
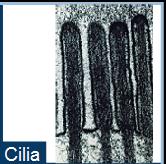
The respiratory passageways are lined with ciliated pseudostratified columnar epithelium. Cilia move mucus and trapped particles toward the pharynx for removal.
Larynx
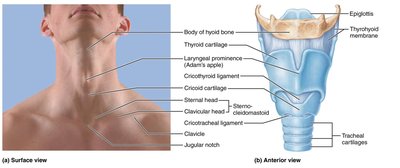
The larynx, or voice box, is involved in sound production and protects the lower airways. It is composed of several cartilages, including the thyroid, cricoid, and epiglottis.
Trachea
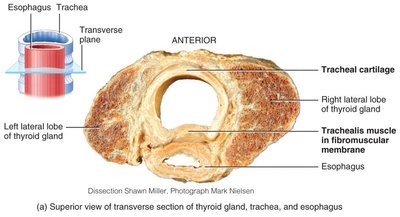
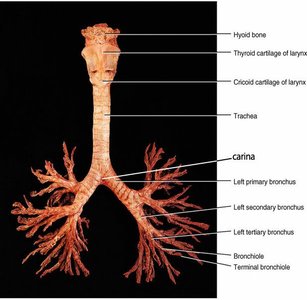
The trachea, or windpipe, is a tube supported by cartilaginous rings that keep it open for air passage. It bifurcates into the right and left main bronchi.

Bronchi and Bronchioles
The bronchi branch into smaller bronchioles, which undergo structural changes as they descend. Cartilage decreases, smooth muscle increases, and the autonomic nervous system regulates their diameter.
Sympathetic Nervous System (SNS): Causes bronchodilation.
Parasympathetic Nervous System (PSNS): Causes bronchoconstriction.

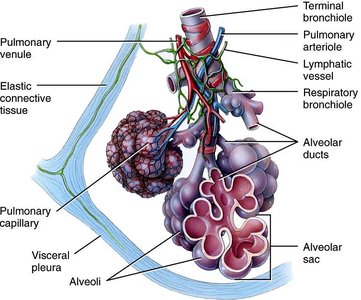
Pulmonary Lobule and Alveoli
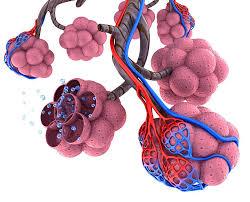
The pulmonary lobule is the functional unit of the lung, containing alveolar ducts, sacs, and alveoli. Alveoli are the site of gas exchange.
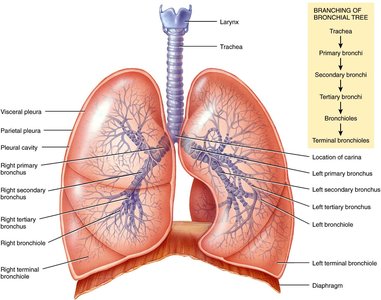
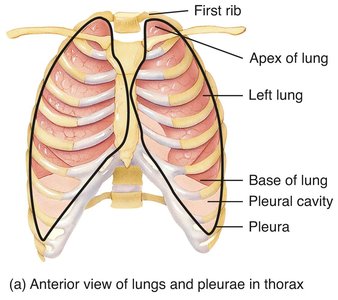
Pleural Membrane
The pleural membrane consists of two layers (visceral and parietal) that enclose the pleural cavity. This cavity contains lubricating fluid, allowing the lungs to expand and contract smoothly.
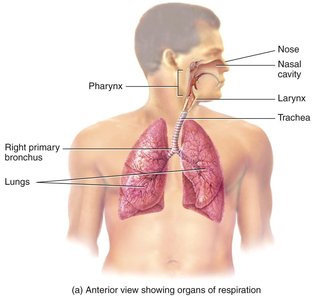
Functional Classification: Conducting vs. Respiratory Zones
The respiratory system is functionally divided into:
Conducting Zone: Brings air to the site of external respiration (nose, pharynx, larynx, trachea, bronchi, bronchioles).
Respiratory Zone: Site of gas exchange (respiratory bronchioles, alveolar ducts, alveolar sacs).
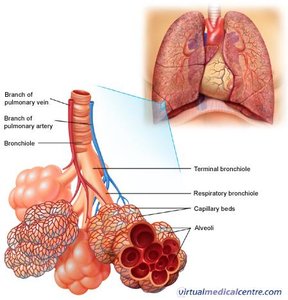
Blood Supply to the Lungs
The pulmonary artery carries deoxygenated blood to the lungs, where it divides into capillaries for gas exchange. Pulmonary veins return oxygenated blood to the heart.
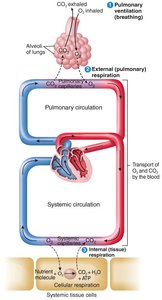
Ventilation and Respiration
Ventilation refers to the movement of air in and out of the lungs. Respiration includes both external (pulmonary) and internal (tissue) gas exchange.
Pulmonary Ventilation: Inhalation and exhalation between atmosphere and alveoli.
External Respiration: Gas exchange between alveoli and pulmonary capillaries.
Internal Respiration: Gas exchange between systemic capillaries and tissue cells.
Mechanics of Ventilation
The diaphragm is the primary muscle of respiration. Inhalation is active, requiring muscle contraction; exhalation is passive during rest, relying on elastic recoil.
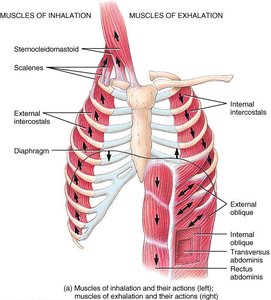
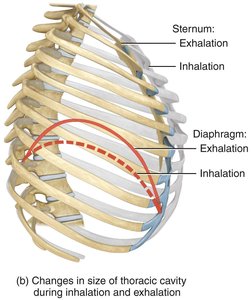
Pressure Changes During Ventilation
Boyle's Law states that the pressure of a gas in a closed container is inversely proportional to the volume of the container:
During inhalation, air moves from higher atmospheric pressure to lower alveolar pressure.
During exhalation, air moves from higher alveolar pressure to lower atmospheric pressure.
Equation:
Factors Affecting Pulmonary Ventilation
Surface Tension: Within alveoli, prevents collapse; surfactant reduces tension.
Compliance: Ease of lung expansion; high compliance means easy stretch, low compliance means resistance.
Airway Resistance: Resistance to airflow; increased resistance requires greater pressure differences.
Surface Tension and Respiratory Distress Syndrome
Premature infants may lack surfactant, leading to increased surface tension and alveolar collapse (respiratory distress syndrome). Treatment includes supplemental oxygen and synthetic surfactant.
Lung Compliance
Compliance is affected by elastic fibers, surfactant, and conditions such as fibrosis, edema, or emphysema.
Airway Resistance
Bronchioles are regulated by smooth muscle. Conditions like COPD increase resistance, requiring greater pressure differences for airflow.
Equation:
Pulmonary Volumes and Capacities
Different volumes of breathing are measured to diagnose respiratory conditions such as asthma.
Gas Exchange Laws
Dalton's Law
Each gas in a mixture exerts its own pressure independently. Partial pressure is calculated as:
Equation:
Henry's Law
The quantity of a gas that dissolves in a liquid is proportional to its partial pressure and solubility. CO2 is more soluble in blood than O2; N2 is not very soluble at sea level.
Respiratory Membrane
The respiratory membrane consists of five layers and is the site of gas exchange between alveoli and capillaries.
External and Internal Respiration
External Respiration: O2 moves from alveolar air to blood; CO2 moves from blood to alveolar air.
Internal Respiration: O2 diffuses from blood to tissues; CO2 diffuses from tissues to blood.
Rate of Gas Exchange
The rate of gas exchange depends on partial pressures, surface area, diffusion distance, and molecular weight/solubility of gases. Destruction of alveoli (e.g., emphysema) reduces exchange rate.
Transport of Gases
Oxygen Transport
1.5% dissolved in plasma
98.5% bound to hemoglobin (Hb) in red blood cells
Hemoglobin Saturation
The amount of O2 bound to Hb depends on PO2. Percent saturation expresses average saturation of Hb with O2 in 100mL blood.
Factors Affecting Hemoglobin Affinity for Oxygen
Acidity (Bohr Effect): Increased acidity reduces affinity, enhancing unloading.
PCO2: Increased PCO2 reduces affinity, enhancing unloading.
Temperature: Increased temperature releases more O2 from Hb.
2,3-BPG: Marker of glycolysis in RBCs, helps unload O2.
Carbon Dioxide Transport
7% dissolved in plasma
23% as carbamino compounds (bound to proteins, mainly Hb)
70% as bicarbonate ions (HCO3-)
Equation:
Control of Breathing
The respiratory center in the brainstem (medulla oblongata and pons) regulates breathing rhythm. Chemoreceptors respond to changes in CO2, O2, and pH.
Hypercapnia: Increased PCO2 stimulates inspiration.
Hypocapnia: Decreased PCO2 inhibits inspiration.
Example: Swimmers may hyperventilate to decrease CO2 and prolong breath-hold.
Additional info: Academic context was added to clarify structural, functional, and physiological aspects of the respiratory system, including relevant equations and clinical applications.
