 Back
BackThe Respiratory System: Structure, Function, and Physiology
Study Guide - Smart Notes

The Respiratory System
Overview and Functions
The respiratory system is essential for gas exchange, providing oxygen to the body and removing carbon dioxide. It also plays roles in sound production, olfaction (sense of smell), and protection against environmental hazards.
Gas Exchange: Occurs in the alveoli, providing a large surface area for efficient diffusion of gases.
Air Movement: Air is moved to and from the exchange surfaces through a series of conducting passages.
Protection: The system protects against dehydration, temperature changes, and pathogens.
Sound Production: The larynx produces sound for speech.
Olfaction: Sensory receptors in the nasal cavity detect odors, relaying information via the olfactory nerve (CN I) directly to the cerebrum.
Anatomical Organization of the Respiratory System
Structural and Functional Divisions
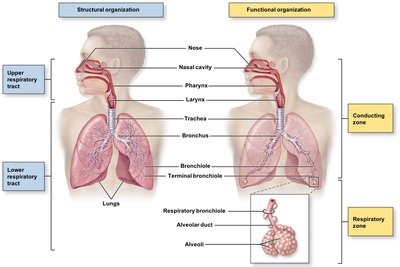
The respiratory system is divided into upper and lower tracts, as well as conducting and respiratory zones based on function.
Upper Respiratory Tract: Nose, nasal cavity (with paranasal sinuses), and pharynx. Functions to filter, warm, and humidify incoming air, protecting lower structures.
Lower Respiratory Tract: Larynx, trachea, bronchi, bronchioles, and alveoli. Responsible for air conduction and gas exchange.
Conducting Zone: Nasal cavity to terminal bronchioles; no gas exchange occurs here.
Respiratory Zone: Respiratory bronchioles, alveolar ducts, and alveoli; site of gas exchange.
Upper Respiratory Tract
Nasal Cavity
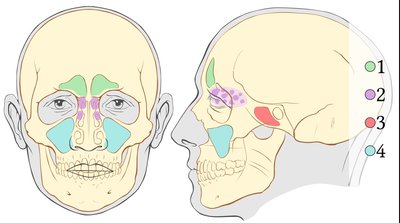
The nasal cavity is the primary entrance for air, lined with hairs and mucosa to trap particles and pathogens. The nasal septum divides the cavity, and the conchae create turbulence for better air conditioning.
Paranasal Sinuses: Maxillary, frontal, ethmoid, and sphenoid sinuses warm and humidify air.
Olfactory Epithelium: Contains receptors for smell.
Internal Nares: Connect the nasal cavity to the nasopharynx.
Pharynx
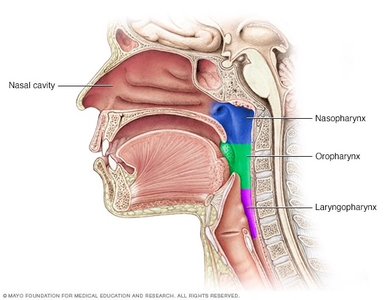
The pharynx is a shared passageway for the respiratory and digestive systems, divided into three regions:
Nasopharynx: From internal nares to soft palate; lined with ciliated pseudostratified columnar epithelium; contains pharyngeal tonsil and auditory tube openings.
Oropharynx: From soft palate to hyoid bone; lined with stratified squamous epithelium for protection; contains palatine and lingual tonsils.
Laryngopharynx: From hyoid bone to larynx/esophagus; also lined with stratified squamous epithelium.
Lower Respiratory Tract
Larynx
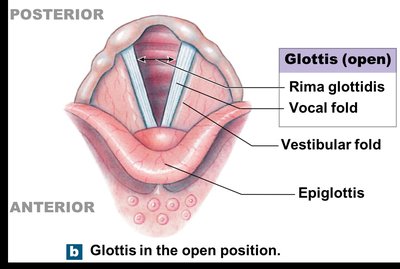
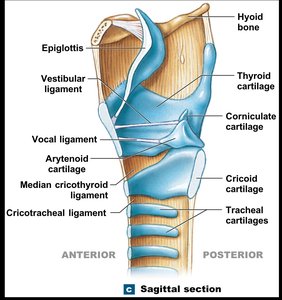
The larynx is the gateway to the lower respiratory tract and is involved in sound production. It contains the glottis, a slit-like opening for air passage.
Epiglottis: Elastic cartilage that covers the glottis during swallowing, preventing aspiration.
Thyroid Cartilage: Hyaline cartilage forming the Adam’s apple, protecting the glottis and entrance to the trachea.
Cricoid Cartilage: Hyaline cartilage providing structural support.
Vocal Ligaments and Sound Production
Ligaments connect the laryngeal cartilages. The vocal ligaments (true vocal cords) are involved in sound production, while vestibular ligaments (false vocal cords) are not.
Sound Production: Air passing through the glottis vibrates the vocal folds, producing sound. Pitch depends on the diameter, length, and tension of the vocal folds.
Trachea and Bronchial Tree
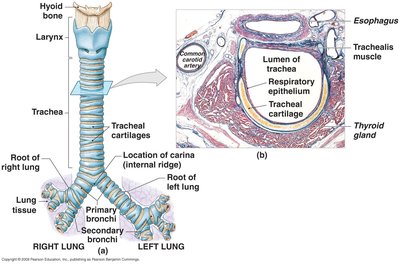
The trachea is a flexible tube reinforced by C-shaped hyaline cartilage rings, allowing for expansion of the esophagus and maintaining airway patency. The trachea splits at the carina into right and left primary bronchi, which enter the lungs at the hilum.
Mucosa: Lined with ciliated pseudostratified columnar epithelium and goblet cells that trap and move debris upward.
Bronchial Tree: Primary bronchi branch into secondary (one per lobe), tertiary bronchi, terminal bronchioles, and finally respiratory bronchioles.
Bronchioles
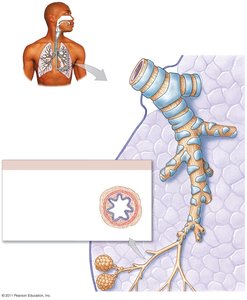
Bronchioles are smaller airways with less cartilage and more smooth muscle. Their diameter is regulated by the autonomic nervous system: sympathetic stimulation causes bronchodilation, while parasympathetic stimulation causes bronchoconstriction.
Terminal Bronchioles: Last part of the conducting zone.
Respiratory Bronchioles: First part of the respiratory zone, where some gas exchange begins.
Gas Exchange Structures
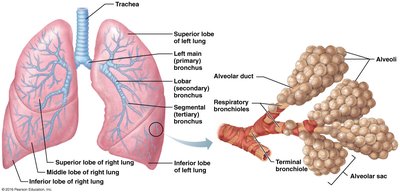
Alveoli and Respiratory Membrane
Alveoli are tiny air sacs surrounded by elastic fibers and capillaries, providing a vast surface area for gas exchange. The respiratory membrane is extremely thin (~0.5 µm), allowing rapid diffusion of gases.
Type I Pneumocytes: Thin cells for gas diffusion.
Type II Pneumocytes: Secrete surfactant to reduce surface tension and prevent alveolar collapse.
Alveolar Macrophages: Patrol and remove debris/pathogens.
The respiratory membrane consists of:
Squamous epithelial tissue of alveolus
Endothelial cells of capillary
Fused basal laminae between them
Lungs and Pleura
Lung Anatomy
The right lung has three lobes (superior, middle, inferior) and is larger, while the left lung has two lobes (superior, inferior) and a cardiac notch. Each lung is surrounded by a pleural membrane (parietal and visceral layers) with pleural fluid to reduce friction.
Mechanics of Breathing (Pulmonary Ventilation)
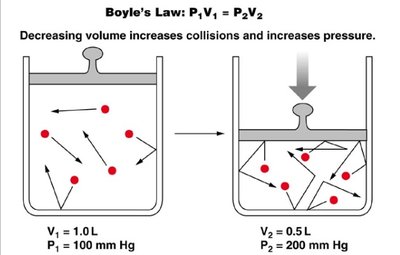
Boyle’s Law and Pressure Changes
Boyle’s Law states that pressure and volume are inversely related: as lung volume increases, pressure decreases, and vice versa. Air moves in and out of the lungs based on pressure gradients relative to atmospheric pressure.
Inhalation: Diaphragm and external intercostals contract, increasing thoracic volume and decreasing pressure, drawing air in.
Exhalation: Muscles relax, thoracic volume decreases, pressure increases, and air is expelled.
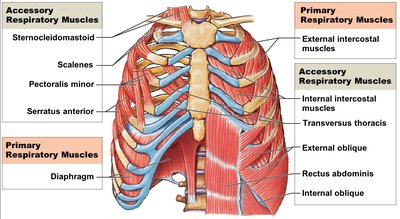
Muscles of Respiration
Primary muscles include the diaphragm and external intercostals. Accessory muscles assist during forced breathing.
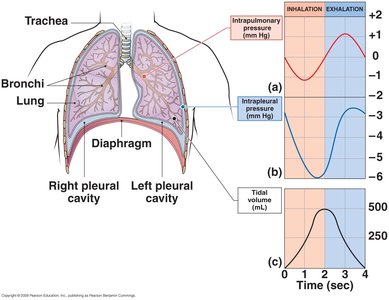
Pressure During Breathing
Intrapulmonary (alveolar) pressure fluctuates around atmospheric pressure during the breathing cycle. Intrapleural pressure is always negative, helping keep the lungs inflated.
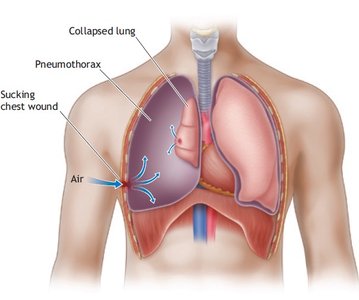
Pneumothorax
Pneumothorax occurs when air enters the pleural cavity, causing lung collapse (atelectasis). This can result from chest injury or alveolar rupture.
Gas Laws and Gas Exchange
Dalton’s Law
The total pressure of a gas mixture is the sum of the partial pressures of each component gas. Partial pressure is calculated as the percentage of the gas in the mixture times the total pressure.
Atmospheric air: 78.6% N2, 20.9% O2, 0.5% H2O, 0.04% CO2
Example:
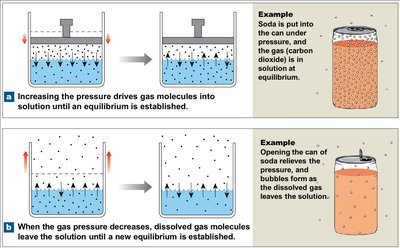
Henry’s Law
The amount of gas dissolved in a liquid is proportional to its partial pressure and solubility. CO2 is highly soluble, O2 less so, and N2 is almost insoluble in body fluids.
Gas Transport in Blood
Oxygen Transport
Oxygen is transported mainly bound to hemoglobin (Hb) in red blood cells (98%), with a small amount dissolved in plasma (2%). The binding and release of O2 are reversible and depend on local conditions.
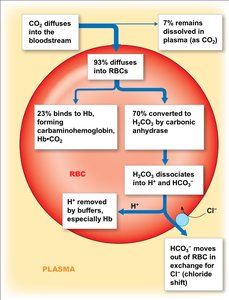
Carbon Dioxide Transport
CO2 is transported in three forms:
7% dissolved in plasma
23% as carbaminohemoglobin (HbCO2)
70% as bicarbonate (HCO3-) formed in RBCs
Key reaction:
Control of Respiration
Nervous Regulation
Respiratory centers in the medulla oblongata and pons regulate the rate and depth of breathing. The dorsal respiratory group (DRG) controls inspiration, while the ventral respiratory group (VRG) is active during forced breathing. The apneustic and pneumotaxic centers in the pons modulate these rhythms.
Chemoreceptor Reflexes
Chemoreceptors respond to changes in CO2, O2, and pH, adjusting ventilation accordingly. Hypercapnia (high CO2) increases respiratory rate, while hypocapnia (low CO2) decreases it.
Hering-Breuer Reflexes
These reflexes prevent over-inflation (inflation reflex) and excessive deflation (deflation reflex) of the lungs during forced breathing.
Disorders of the Respiratory System
Respiratory Distress Syndrome
Occurs in premature infants due to insufficient surfactant production, leading to alveolar collapse and impaired gas exchange.
Chronic Obstructive Pulmonary Disease (COPD)
Includes emphysema, characterized by destruction of alveolar walls, loss of elasticity, and reduced oxygenation.
Lung Cancer
A leading cause of cancer death, strongly associated with smoking and exposure to second-hand smoke.
Cystic Fibrosis
A genetic disorder causing thick mucus buildup, loss of lung elasticity, and increased risk of infection.
Asthma
Characterized by airway inflammation, bronchoconstriction, and excess mucus production, leading to wheezing and difficulty breathing. Treated with bronchodilators and expectorants.
