 Back
BackThe Respiratory System: Structure, Function, and Pulmonary Ventilation
Study Guide - Smart Notes

Respiratory System: Structure and Function
Overview of the Respiratory System
The respiratory system is responsible for providing an airway for the movement of air into and out of the body, coordinating with the cardiovascular system to deliver oxygen to tissues and remove carbon dioxide. The main organs include the nose, pharynx, larynx, trachea, bronchi, and lungs. Functionally, the system is divided into the conducting zone (air passageways) and the respiratory zone (sites of gas exchange).
Conducting Zone: Nose, pharynx, larynx, trachea, bronchi, and terminal bronchioles; these structures filter, warm, and moisten air and conduct it into the lungs.
Respiratory Zone: Respiratory bronchioles, alveolar ducts, and alveoli; these structures are involved in gas exchange.
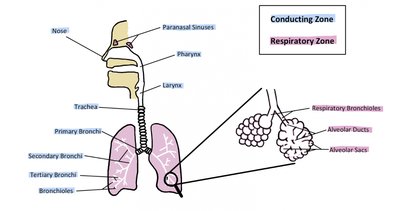
Anatomy of the Upper Respiratory Tract
Nasal Anatomy
The nose is composed of bone and cartilage, with two external nares (nostrils) that allow air to enter the nasal cavity. The nasal septum divides the cavity into right and left sides. The superior, middle, and inferior nasal conchae (turbinates) are bony structures that increase surface area, enhancing air warming and humidification as air passes over the mucous membranes of the meatuses.
Highly vascular: The nasal cavity contains many blood vessels to warm incoming air.
Deviated septum: A condition where the nasal septum is displaced, potentially affecting airflow.
The Pharynx (Throat)
The pharynx is divided into three regions:
Nasopharynx: Extends from the internal nares to the soft palate; contains the uvula and auditory tubes, and the pharyngeal tonsil (adenoid).
Oropharynx: From the soft palate to the hyoid bone; contains the palatine and lingual tonsils.
Laryngopharynx: From the hyoid bone to the beginning of the esophagus.
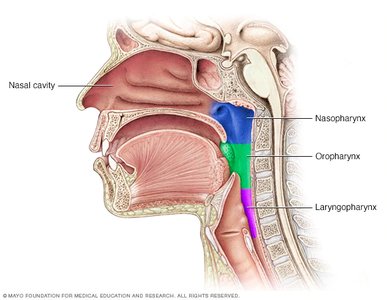
The Larynx (Voice Box)
The larynx connects the laryngopharynx with the trachea and is involved in sound production and airway protection. Key structures include:
Thyroid cartilage: Forms the Adam’s apple; made of hyaline cartilage.
Cricoid cartilage: Ring-shaped hyaline cartilage below the thyroid cartilage.
Epiglottis: Elastic cartilage that closes over the glottis during swallowing to prevent aspiration.
Vocal folds: Vibrate to produce sound; inflammation leads to hoarseness (laryngitis).
Lower Respiratory Tract: Bronchial Tree and Lungs
The Bronchial Tree
The bronchial tree resembles an inverted tree and consists of branching airways that conduct air from the trachea to the alveoli. The trachea divides at the carina into the right and left main (primary) bronchi, which further branch into lobar (secondary) bronchi, segmental (tertiary) bronchi, and bronchioles.
Tracheal cartilages: C-shaped rings that keep the trachea open.
Trachealis muscle: Located posteriorly, allows for flexibility and diameter adjustment.
Bronchioles: Smallest airways, ending the conducting zone.
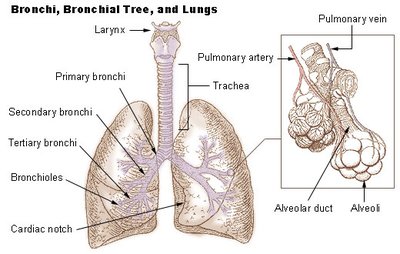
Respiratory Zone Structures
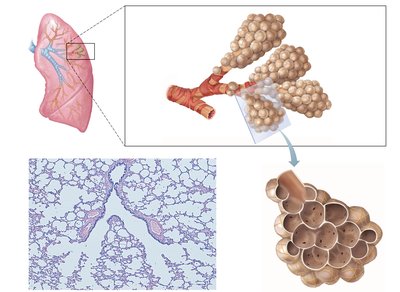
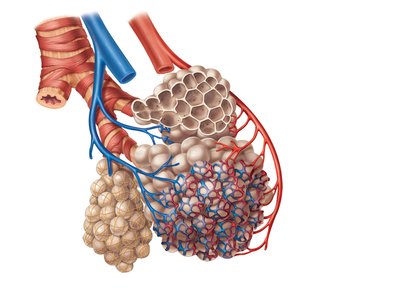
The respiratory zone begins with the respiratory bronchioles, which branch into alveolar ducts and terminate in alveolar sacs composed of clusters of alveoli. These structures are surrounded by capillaries and are the primary sites of gas exchange.
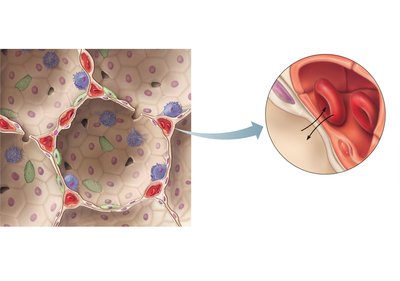
Alveoli: Tiny air sacs where oxygen and carbon dioxide are exchanged between air and blood.
Respiratory membrane: Formed by the alveolar and capillary walls, allowing efficient gas diffusion.
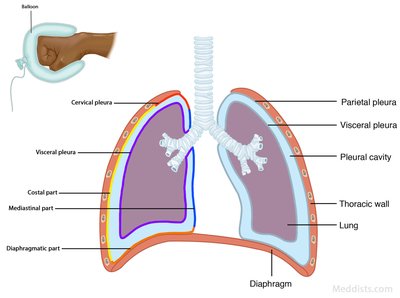
Lungs and Pleura
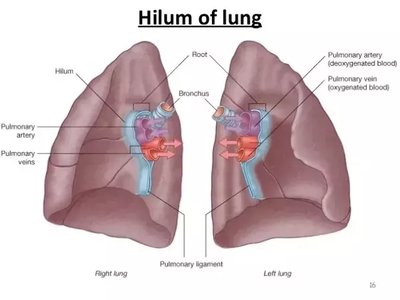
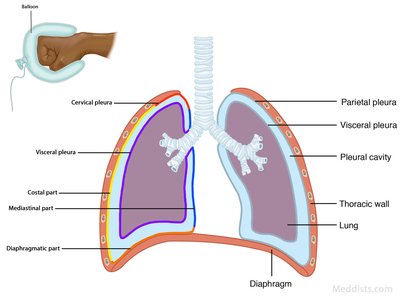
The lungs are divided into lobes (right: three; left: two with a cardiac notch). The hilum is the entry/exit point for bronchi, blood vessels, lymphatics, and nerves. Each lung is surrounded by a double-layered serous membrane called the pleura:
Parietal pleura: Lines the thoracic cavity.
Visceral pleura: Covers the lung surface.
Pleural cavity: Space between layers, containing pleural fluid to reduce friction.
Pulmonary Ventilation (Breathing)
Mechanics of Breathing
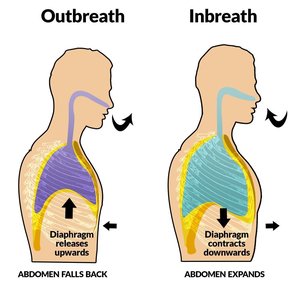
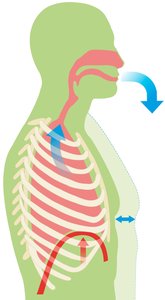
Pulmonary ventilation consists of two phases: inhalation (inspiration) and exhalation (expiration). The process is driven by changes in thoracic volume and pressure, primarily due to the action of the diaphragm and intercostal muscles.
Inhalation: Diaphragm contracts and flattens, external intercostals raise the ribs, increasing thoracic volume and decreasing pressure, causing air to flow into the lungs.
Exhalation: Diaphragm relaxes, thoracic volume decreases, pressure increases, and air is expelled passively.

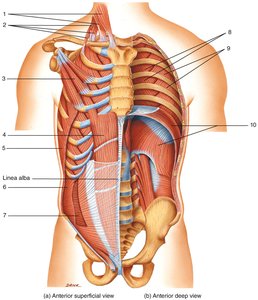
Muscles of Respiration
During forced breathing, additional muscles are recruited:
Forced inhalation: Sternocleidomastoid, scalenes, and pectoralis minor increase thoracic volume.
Forced exhalation: Internal intercostals and abdominal muscles decrease thoracic volume.
Muscle | Function | Effect on Thoracic Dimensions |
|---|---|---|
External intercostals | Elevate ribs | Increase diameter |
Internal intercostals | Depress ribs | Decrease diameter |
Sternocleidomastoids | Elevate sternum | Increase diameter |
Scalenes | Elevate 1st and 2nd ribs | Increase diameter |
Pectoralis minors | Elevate 3rd, 4th, and 5th ribs | Increase diameter |
Diaphragm | Flattens when contracted | Increase vertical length |
Abdominal muscles | Compress abdominal contents, increase abdominal pressure, force diaphragm superiorly | Decrease vertical length |
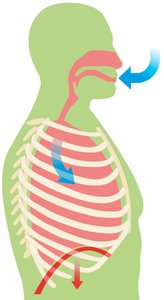
Pressure Changes During Ventilation
Air moves according to pressure gradients:
Inhalation: Thoracic volume increases, intrapleural and alveolar pressures decrease, air flows into lungs.
Exhalation: Thoracic volume decreases, pressures increase, air flows out of lungs.
Key principle: Air flows from high to low pressure.
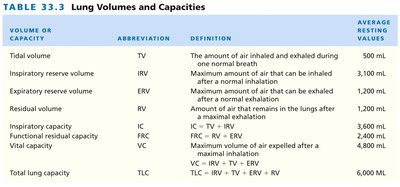
Lung Volumes and Capacities
Measuring Lung Function
A spirometer is used to measure lung volumes and capacities, which vary by age, sex, body composition, ethnicity, and height. Key volumes and capacities include:
Volume or Capacity | Abbreviation | Definition | Average Resting Values |
|---|---|---|---|
Tidal volume | TV | Amount of air inhaled/exhaled during one normal breath | 500 mL |
Inspiratory reserve volume | IRV | Maximum air that can be inhaled after a normal inhalation | 3,100 mL |
Expiratory reserve volume | ERV | Maximum air that can be exhaled after a normal exhalation | 1,200 mL |
Residual volume | RV | Air remaining in lungs after maximal exhalation | 1,200 mL |
Inspiratory capacity | IC | IC = TV + IRV | 3,600 mL |
Functional residual capacity | FRC | FRC = ERV + RV | 2,400 mL |
Vital capacity | VC | VC = IRV + TV + ERV | 4,800 mL |
Total lung capacity | TLC | TLC = IRV + TV + ERV + RV | 6,000 mL |
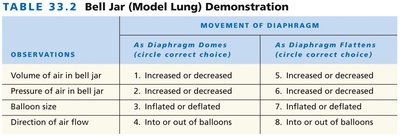
Summary Table: Bell Jar Model (Model Lung Demonstration)
The bell jar model is used to demonstrate the mechanics of breathing. The movement of the diaphragm (represented by the rubber sheet) changes the volume and pressure inside the jar, simulating inhalation and exhalation.
Observation | As Diaphragm Domes | As Diaphragm Flattens |
|---|---|---|
Volume of air in bell jar | Decreased | Increased |
Pressure of air in bell jar | Increased | Decreased |
Balloon size | Deflated | Inflated |
Direction of air flow | Out of balloons | Into balloons |
Key Equations
Boyle’s Law: (Pressure and volume are inversely related at constant temperature.)
Vital Capacity (VC):
Total Lung Capacity (TLC):
Summary
The respiratory system is essential for gas exchange, providing oxygen to the body and removing carbon dioxide. Its structure is specialized for efficient airflow and gas diffusion, and its function is closely tied to the mechanics of breathing and the regulation of lung volumes and pressures.
