 Back
BackThe Respiratory System: Structure, Function, and Physiology
Study Guide - Smart Notes

The Respiratory System
Overview and Organization
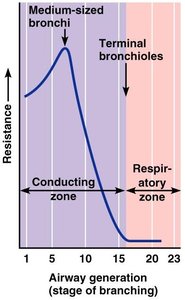
The respiratory system is essential for gas exchange, supplying oxygen to the body and removing carbon dioxide. It is divided into the upper respiratory system (nose, paranasal sinuses, pharynx) and the lower respiratory system (larynx to alveoli). The system is further organized into conducting and respiratory zones.
Conducting zone: Passageways for air to reach sites of gas exchange (nose to terminal bronchioles).
Respiratory zone: Site of gas exchange (respiratory bronchioles, alveolar ducts, alveoli).
Respiratory muscles: Diaphragm and other muscles that promote ventilation.
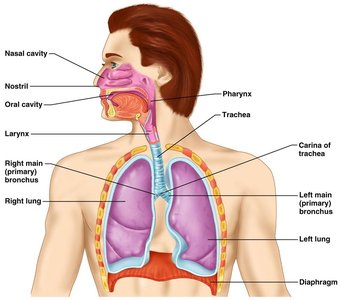
Major Functions of the Respiratory System
Processes of Respiration
The respiratory system's primary function is to supply oxygen and remove carbon dioxide. Four key processes are involved:
Pulmonary ventilation: Movement of air into and out of the lungs.
External respiration: Gas exchange between lungs and blood.
Transport: Movement of oxygen and carbon dioxide between lungs and tissues.
Internal respiration: Gas exchange between systemic blood vessels and tissues.
Upper Respiratory System
Structure and Function of the Nose
The nose is the only externally visible part of the respiratory system. It provides an airway, moistens and warms air, filters and cleans inspired air, serves as a resonating chamber for speech, and houses olfactory receptors.
External nose: Includes root, bridge, dorsum nasi, apex, philtrum, and external nares (nostrils).
Internal nasal cavity: Divided by the nasal septum, opens into the nasopharynx, and is bounded by the ethmoid and sphenoid bones (roof) and hard/soft palates (floor).
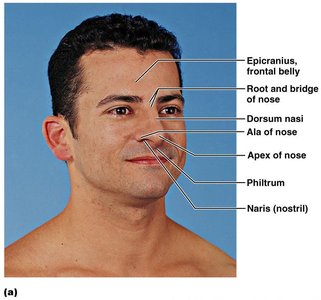
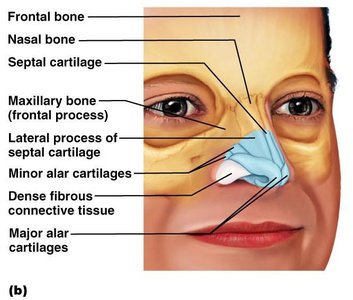
Nasal Cavity and Associated Structures
The nasal cavity is lined with vibrissae (hairs) to filter particles, olfactory mucosa for smell, and respiratory mucosa that secretes mucus with lysozyme and defensins. The conchae increase surface area and air turbulence, aiding in filtering, heating, and moistening air.
Paranasal sinuses: Lighten the skull and help warm/moisten air.
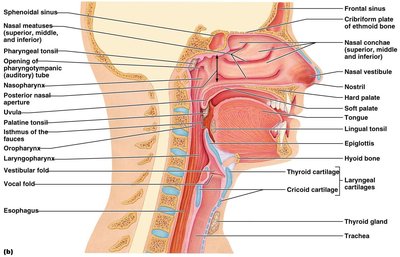
Pharynx
The pharynx is a muscular tube connecting the nasal cavity and mouth to the larynx and esophagus. It is divided into three regions:
Nasopharynx: Air passageway, lined with pseudostratified columnar epithelium.
Oropharynx: Common passageway for food and air, lined with stratified squamous epithelium.
Laryngopharynx: Common passageway for food and air, posterior to the epiglottis.
Lower Respiratory System
Larynx (Voice Box)
The larynx attaches to the hyoid bone and opens into the laryngopharynx. It provides an airway, routes air and food, and functions in voice production. The framework consists of hyaline cartilages (thyroid, cricoid, arytenoid, cuneiform, corniculate) and the elastic cartilage epiglottis.
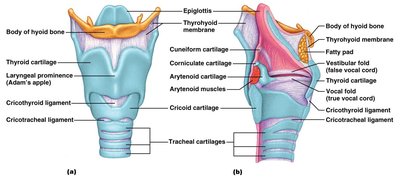
Vocal Folds
Vocal folds (true vocal cords) are elastic fibers that vibrate to produce sound. The glottis is the opening between them. Vestibular folds (false vocal cords) are superior and do not produce sound.
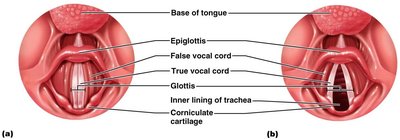
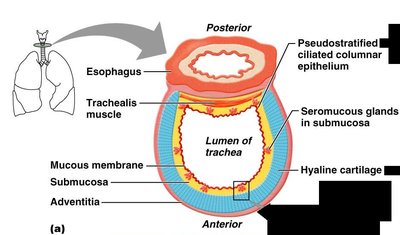
Trachea
The trachea is a flexible tube extending from the larynx into the mediastinum. It consists of three layers: mucosa (goblet cells, ciliated epithelium), submucosa (connective tissue), and adventitia (outer connective tissue with C-shaped hyaline cartilage rings).
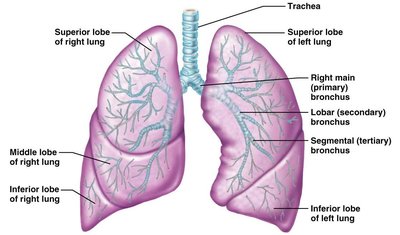
Bronchial Tree and Lungs
The bronchi branch from the trachea into primary, secondary, and tertiary bronchi, undergoing 23 orders of branching. Bronchioles lack cartilage and have more smooth muscle. The lungs are divided into lobes and bronchopulmonary segments.
Respiratory Zone Structures
The respiratory zone includes respiratory bronchioles, alveolar ducts, and alveoli. Alveoli are the primary sites of gas exchange, with approximately 300 million in the lungs, providing a large surface area.
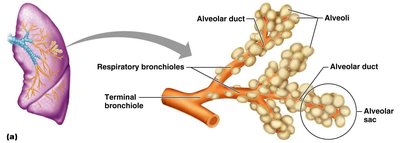
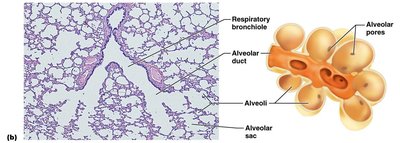
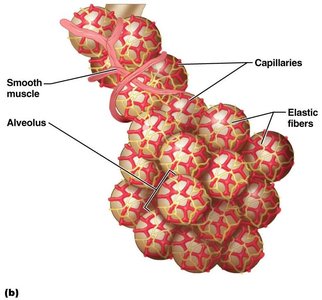
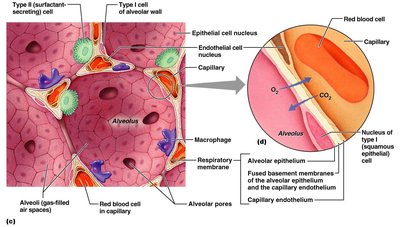
Respiratory Membrane
The respiratory membrane consists of alveolar and capillary walls and their fused basal laminas. Type I cells allow gas exchange by diffusion; Type II cells secrete surfactant. Alveoli contain pores and macrophages for air pressure equalization and sterility.
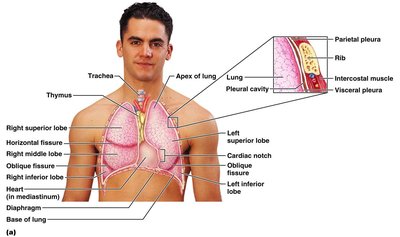
Pleura and Thoracic Cavity
The pleura is a double-layered serosa: parietal pleura lines the thoracic wall, and visceral pleura covers the lungs. The pleural cavity contains fluid to reduce friction during breathing.
Mechanics of Breathing
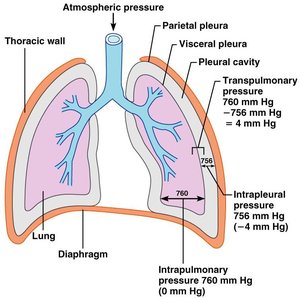
Pressure Relationships
Breathing depends on pressure differences between the atmosphere, alveoli, and pleural cavity. Intrapulmonary pressure equalizes with atmospheric pressure; intrapleural pressure is always less, preventing lung collapse. Transpulmonary pressure keeps airways open.
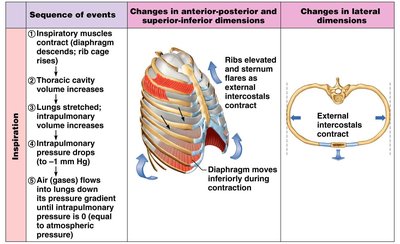
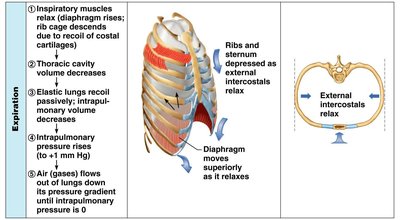
Inspiration and Expiration
Inspiration occurs when inspiratory muscles contract, increasing thoracic volume and decreasing intrapulmonary pressure, causing air to flow in. Expiration is usually passive, resulting from muscle relaxation and lung recoil, increasing intrapulmonary pressure and expelling air.
Physical Factors Influencing Ventilation
Airway resistance, alveolar surface tension, and lung compliance affect ventilation. Surfactant reduces surface tension, preventing alveolar collapse. Lung compliance is determined by tissue distensibility and alveolar surface tension.
Gas Exchange and Transport
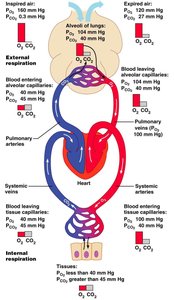
External and Internal Respiration
Gas exchange occurs by diffusion across partial pressure gradients. Oxygen diffuses from alveoli to blood; carbon dioxide diffuses from blood to alveoli. Internal respiration is the exchange between systemic capillaries and tissues.
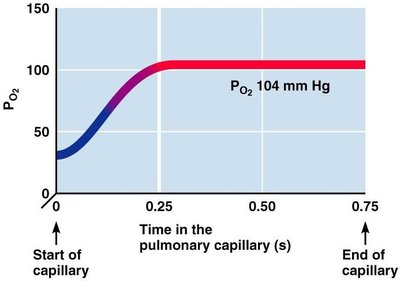
Oxygen Transport
Oxygen is transported bound to hemoglobin (Hb) and dissolved in plasma. The oxygen-hemoglobin dissociation curve shows the relationship between PO2 and hemoglobin saturation. Factors such as pH, temperature, and BPG affect oxygen release (Bohr effect).
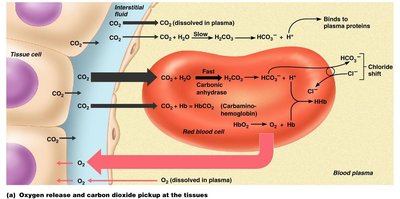
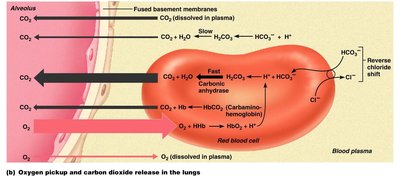
Carbon Dioxide Transport
Carbon dioxide is transported dissolved in plasma, bound to hemoglobin, and as bicarbonate ions. The chloride shift maintains ionic balance during CO2 transport. The Haldane effect describes increased CO2 transport when PO2 is low.
Control of Respiration
Neural Regulation
Respiratory centers in the medulla (DRG and VRG) and pons (apneustic and pneumotaxic centers) regulate breathing rhythm and depth. Reflexes and higher brain centers (hypothalamus, cortex) also influence respiration.
Chemical Regulation
Central and peripheral chemoreceptors respond to changes in CO2, O2, and pH. Increased CO2 (hypercapnia) stimulates increased ventilation. Substantial drops in O2 are required to stimulate breathing.
Clinical and Developmental Aspects
Respiratory Volumes and Capacities
Key volumes include tidal volume (TV), inspiratory reserve volume (IRV), expiratory reserve volume (ERV), and residual volume (RV). Capacities are combinations of these volumes. Pulmonary function tests (e.g., spirometry) assess respiratory health.
Respiratory Adjustments
Exercise and high altitude require adjustments in ventilation and oxygen transport. Acclimatization involves increased ventilation and erythropoietin release. Respiratory efficiency decreases with age.
