 Back
BackThe Respiratory System: Structure, Function, and Physiology
Study Guide - Smart Notes

The Respiratory System
Overview and Functions
The respiratory system (RS) is essential for gas exchange, providing oxygen to the body and removing carbon dioxide. It also plays roles in sound production, olfaction, and protection of respiratory surfaces.
Gas Exchange: Supplies oxygen (O2) to the blood and removes carbon dioxide (CO2).
Sound Production: The larynx enables speaking and singing.
Olfaction: Olfactory receptors in the nasal cavity detect odors.
Protection: Mucosal surfaces and immune cells protect against pathogens and debris.
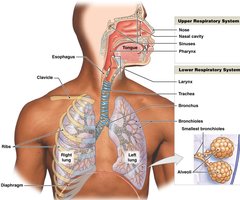
Divisions of the Respiratory System
Upper Respiratory System: Nose, nasal cavity, sinuses, and pharynx. Functions include filtering, warming, and humidifying air.
Lower Respiratory System: Larynx, trachea, bronchi, bronchioles, and alveoli. Main function is gas exchange.
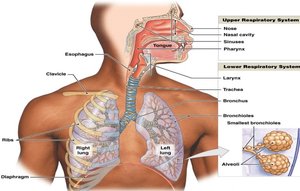
Respiratory Tract: Conducting vs. Respiratory Portions
Conducting Portion: Nasal cavity to terminal bronchioles; moves air to the lungs.
Respiratory Portion: Respiratory bronchioles and alveoli; site of gas exchange.
Histology and Defense Mechanisms
Respiratory Mucosa and Epithelial Changes
The respiratory tract is lined by a mucosal membrane, which varies in structure along its length to optimize protection and function.
Nasal cavity & nasopharynx: Pseudostratified ciliated columnar epithelium (traps and moves debris).
Oropharynx, laryngopharynx, larynx: Stratified squamous epithelium (protection from abrasion).
Trachea & larger bronchi: Pseudostratified ciliated columnar epithelium with goblet cells (mucus production).
Bronchioles: Simple cuboidal epithelium with cilia.
Alveoli: Simple squamous epithelium (facilitates gas exchange).
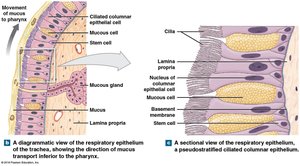
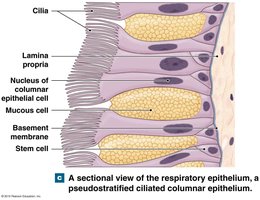
Respiratory Defense System
Mucus: Traps pathogens and debris.
Cilia: Move mucus toward the pharynx (mucus escalator).
Nasal hairs: Filter large particles.
Alveolar macrophages: Engulf small particles in the lungs.
Anatomy of the Upper Respiratory Tract
Nasal Cavity and Pharynx
Air enters through the external nares, passes through the nasal vestibule (with hairs for filtration), and into the nasal cavity, which is divided by the nasal septum. The nasal conchae create turbulence, increasing filtration, humidification, and warming of air.
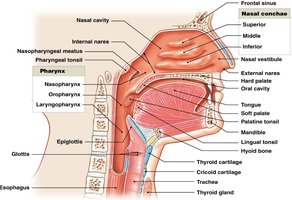
Hard palate: Forms the floor of the nasal cavity.
Olfactory region: Superior portion, important for smell.
Pharynx: Shared by respiratory and digestive systems; divided into nasopharynx, oropharynx, and laryngopharynx.
Larynx
The larynx is a cartilaginous structure that surrounds the glottis and is the site of sound production. It is composed of several cartilages:
Thyroid cartilage: Forms the anterior and lateral walls (Adam's apple).
Cricoid cartilage: Forms the inferior and posterior portion.
Epiglottis: Covers the glottis during swallowing.
Arytenoid and corniculate cartilages: Involved in opening/closing the glottis and sound production.
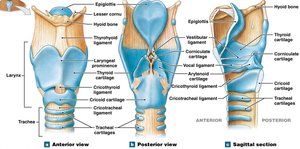
Vocal and Vestibular Folds
Vocal folds: Highly elastic, produce sound when air passes through.
Vestibular folds: Support the larynx and block particle entry.
Anatomy of the Lower Respiratory Tract
Trachea and Bronchial Tree
The trachea (windpipe) is a tough, flexible tube supported by C-shaped cartilages. It branches into the right and left primary bronchi at the carina. The right bronchus is wider and steeper than the left.
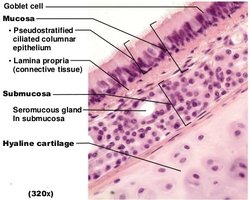
Primary bronchi: Enter the lungs at the hilum.
Secondary (lobar) bronchi: Two in the left lung, three in the right lung.
Tertiary (segmental) bronchi: Supply specific bronchopulmonary segments.
Bronchioles: Less cartilage, more smooth muscle; terminal bronchioles lead to pulmonary lobules.
Lungs
The lungs are located in the pleural cavities and are divided into lobes by fissures. The right lung has three lobes; the left has two and a cardiac notch for the heart.
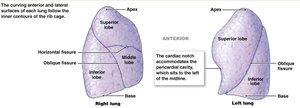
Apex: Superior tip of the lung.
Base: Rests on the diaphragm.
Hilum: Entry/exit point for bronchi, blood vessels, nerves, and lymphatics.
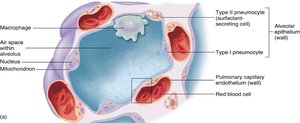
Alveoli and Gas Exchange
Alveoli are the primary sites of gas exchange, surrounded by capillaries and elastic fibers. The alveolar wall consists of:
Type I pneumocytes: Simple squamous cells for gas exchange.
Type II pneumocytes: Produce surfactant to reduce surface tension and prevent alveolar collapse.
Alveolar macrophages: Remove debris and pathogens.
Respiratory Physiology
Pulmonary Ventilation and Boyle’s Law
Pulmonary ventilation is the movement of air into and out of the lungs, driven by pressure changes according to Boyle’s Law:
Boyle’s Law: or (Pressure is inversely related to volume).
Inspiration increases lung volume, decreasing pressure and drawing air in.
Expiration decreases lung volume, increasing pressure and pushing air out.
Respiratory Volumes and Capacities
Tidal Volume (VT): Air moved in/out in a single cycle (~500 mL).
Expiratory Reserve Volume (ERV): Extra air that can be exhaled after normal expiration.
Inspiratory Reserve Volume (IRV): Extra air that can be inhaled after normal inspiration.
Residual Volume: Air remaining after maximal exhalation.
Vital Capacity:
Total Lung Capacity:
Gas Laws and Gas Exchange
Dalton’s Law: Each gas in a mixture exerts its own partial pressure.
Henry’s Law: The amount of gas dissolved in a liquid is proportional to its partial pressure and solubility.
Efficient gas exchange: Due to large surface area, thin membrane, and coordinated blood/air flow.
Transport of Gases
Oxygen Transport
98.5% of O2 is transported bound to hemoglobin (Hb) as oxyhemoglobin (HbO2).
Hemoglobin saturation depends on partial pressure of O2, pH, and temperature.
Fetal hemoglobin has a higher affinity for O2 than adult hemoglobin.
Carbon Dioxide Transport
7% dissolved in plasma.
23% bound to hemoglobin as carbaminohemoglobin.
70% converted to carbonic acid by carbonic anhydrase, then to bicarbonate (HCO3-).
CO2 transport is crucial for pH regulation (bicarbonate buffer system).
Control of Respiration
Neural Control and Reflexes
Chemoreceptors: In carotid and aortic bodies, sense CO2, O2, and pH.
Respiratory Centers: Medulla (DRG and VRG) and pons (apneustic and pneumotaxic centers) regulate rate and depth of breathing.
Baroreceptors: Sense blood pressure changes.
Mechanoreceptors: Hering-Breuer reflexes prevent overinflation or excessive deflation of lungs.
Disorders of the Respiratory System
Asthma: Bronchoconstriction due to excessive parasympathetic stimulation.
Bronchitis: Inflammation of bronchial walls.
Pneumonia: Infection/inflammation of lung lobules, fluid in alveoli.
Emphysema: Destruction of alveoli, reduced surface area for gas exchange.
Cystic Fibrosis: Overproduction of mucus, impairs gas exchange.
