 Back
BackThe Respiratory System: Structure, Function, and Clinical Connections
Study Guide - Smart Notes

The Respiratory System
Anatomy of the Respiratory System: Overview
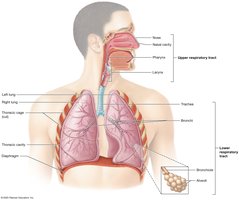
The respiratory system consists of organs and structures located in the head, neck, and thoracic cavity. Its primary function is to facilitate the exchange of gases between the body and the environment. The system includes the pulmonary circuit blood vessels, thoracic cage structures, respiratory muscles, paired lungs, and the respiratory tract.
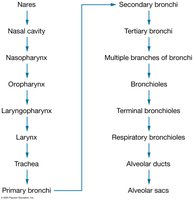
Respiratory Tract: Includes the nose, nasal cavity, pharynx, larynx, trachea, and bronchial tree (bronchi and bronchioles).
Upper Respiratory Tract: Passageways from the nasal cavity to the larynx.
Lower Respiratory Tract: Passageways from the trachea to the alveoli.
Alveoli: Tiny air sacs in the lungs where gas exchange occurs; each lung contains about 150 million alveoli.
Basic Functions of the Respiratory System
The respiratory system provides oxygen to the body's cells and removes carbon dioxide. It also performs several other vital functions.
Conducting Zone: Air is filtered, warmed, and moistened as it travels through the conducting zone (nose to bronchioles).
Respiratory Zone: Site of gas exchange; includes structures containing alveoli only.
Respiration: Consists of four processes:
Pulmonary Ventilation – Movement of air in and out of the lungs
Pulmonary Gas Exchange – Exchange of gases between lungs and blood
Gas Transport in the Blood – Movement of gases through the blood
Tissue Gas Exchange – Exchange of gases between blood and tissues
Other Functions: Speech production, odor detection, expulsion of abdominal contents, assisting venous blood and lymph flow, acid–base homeostasis, and production of angiotensin for blood pressure regulation.
Structures of the Respiratory System
The Nose and Nasal Cavity
The nose and nasal cavity warm, humidify, and filter inhaled air, house olfactory receptors, and enhance voice resonance.
The Pharynx
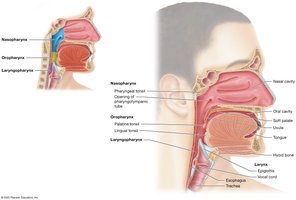
The pharynx (throat) is divided into three regions, each with distinct functions and epithelial linings:
Nasopharynx: Posterior to the nasal cavity; lined with pseudostratified ciliated columnar epithelium; contains pharyngeal tonsil and pharyngotympanic tube openings.
Oropharynx: Posterior to the oral cavity; lined with nonkeratinized stratified squamous epithelium; houses palatine and lingual tonsils.
Laryngopharynx: Extends from the hyoid bone to the esophagus; lined with nonkeratinized stratified squamous epithelium.
The Larynx
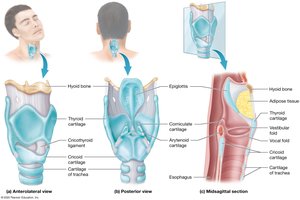
The larynx extends from the third to the sixth cervical vertebra and functions to keep food and liquids out of the lower respiratory tract and to house the vocal cords for sound production.
Cartilage Framework: Nine cartilages, including the thyroid cartilage (Adam's apple), cricoid cartilage, and epiglottis.
Epiglottis: Flap of elastic cartilage that covers the glottis during swallowing to prevent aspiration.
Mucosal Folds: Vestibular folds (false vocal cords) and vocal folds (true vocal cords) are involved in sound production and airway protection.
The Trachea
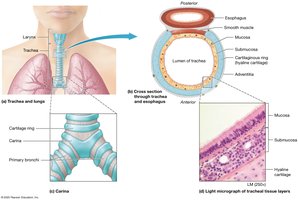
The trachea is a tube about 2 cm in diameter and 10–12 cm long, delivering air to the lower respiratory tract. It is supported by C-shaped rings of hyaline cartilage to maintain patency and flexibility.
Posterior Surface: Contains elastic connective tissue and smooth muscle, allowing for esophageal expansion during swallowing.
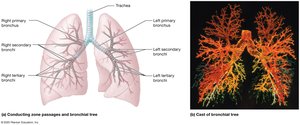
The Bronchial Tree
The bronchial tree consists of branching airways that conduct air from the trachea to the alveoli.
Primary Bronchi: Right and left branches from the trachea; right is wider, shorter, and straighter.
Secondary (Lobar) Bronchi: Three in the right lung, two in the left lung.
Tertiary (Segmental) Bronchi: About 10 in each lung; further branching leads to bronchioles.
Bronchioles: Less than 1 mm in diameter, lack cartilage, and have more smooth muscle.
Terminal Bronchioles: Final part of the conducting airways; branch into respiratory bronchioles and alveolar ducts.
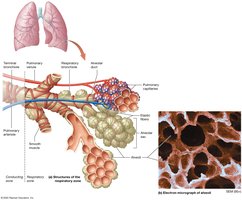
Alveoli and the Respiratory Membrane
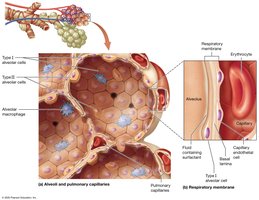
Alveoli are the primary sites of gas exchange and are surrounded by elastic fibers, smooth muscle, and pulmonary capillaries. The respiratory membrane is extremely thin, facilitating efficient gas exchange.
Type I Alveolar Cells: Squamous cells for rapid gas diffusion (about 90% of alveolar wall).
Type II Alveolar Cells: Cuboidal cells producing surfactant to reduce surface tension (about 10%).
Alveolar Macrophages: Phagocytes that remove debris and pathogens.
Respiratory Membrane: Composed of alveolar epithelium, fused basal lamina, and capillary endothelium; thickness 0.2–0.6 µm.
Lungs and Pleurae
Gross Anatomy of the Lungs
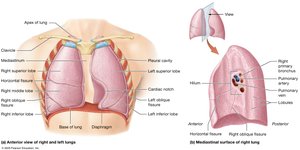
The lungs are separated by the heart and mediastinum. The base rests on the diaphragm, and the apex sits above the clavicle. Each lung has distinct lobes and bronchopulmonary segments.
Left Lung: Two lobes (superior and inferior) separated by the oblique fissure; contains the cardiac notch.
Right Lung: Three lobes (superior, middle, inferior) separated by horizontal and oblique fissures.
Hilum: Entry/exit point for bronchi, blood vessels, lymphatics, and nerves.
Bronchopulmonary Segments: Each supplied by a tertiary bronchus; further divided into lobules.
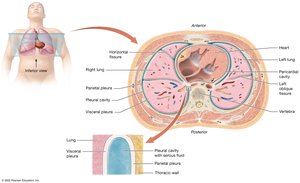
Pleurae and Pleural Cavities
The lungs are enclosed by a double-layered serous membrane called the pleura. The pleural cavity contains pleural fluid to lubricate lung movement.
Parietal Pleura: Lines the thoracic wall and diaphragm.
Visceral Pleura: Covers the lung surface.
Pleural Fluid: Reduces friction during breathing movements.
Physical Factors Influencing Pulmonary Ventilation
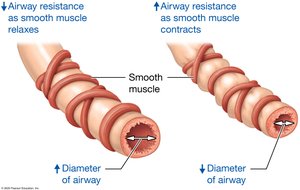
Airway Resistance
Airway resistance is influenced by the diameter of the airways. Bronchodilation decreases resistance, while bronchoconstriction increases it. Diseases such as asthma, COVID-19, and influenza can increase airway resistance.
Bronchodilation: Triggered by sympathetic stimulation (norepinephrine); increases airway diameter.
Bronchoconstriction: Triggered by parasympathetic stimulation or irritants; decreases airway diameter.
Pulmonary Volumes and Capacities
Pulmonary Volumes
Tidal Volume (TV): Air inspired or expired during normal breathing (~500 ml).
Minute Volume: TV × breaths per minute (~6 L/min in adults).
Anatomical Dead Space: Air remaining in conducting zone (~150 ml).
Alveolar Ventilation Rate (AVR): Volume of air reaching alveoli × breaths per minute (~4.2 L/min).
Inspiratory Reserve Volume (IRV): Additional air inspired after normal inspiration (2,100–3,300 ml).
Expiratory Reserve Volume (ERV): Additional air expired after normal expiration (700–1,200 ml).
Residual Volume (RV): Air remaining in lungs after maximal expiration; not measured by spirometry.
Pulmonary Capacities
Inspiratory Capacity: TV + IRV
Functional Residual Capacity: ERV + RV
Vital Capacity: TV + IRV + ERV
Total Lung Capacity: TV + IRV + ERV + RV
Forced Vital Capacity (FVC): Maximal inspiration followed by maximal expiration; used to assess pulmonary disease.
Gas Exchange and Transport
Oxygen Transport on Hemoglobin
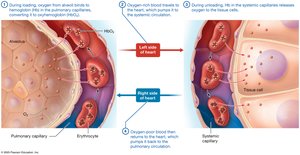
Hemoglobin (Hb) in erythrocytes binds and transports oxygen. Each Hb molecule can carry four oxygen molecules, and each erythrocyte contains about 280 million Hb molecules.
Loading: Oxygen binds to Hb in pulmonary capillaries (forms oxyhemoglobin).
Unloading: Hb releases oxygen to tissues in systemic capillaries.
Oxygen Saturation: Hb with four oxygen molecules is fully saturated; with one to three, it is partially saturated.
Clinical Connections: Respiratory Diseases
Tuberculosis (TB)
TB is a respiratory infection caused by Mycobacterium tuberculosis. It spreads through airborne droplets and can be latent or active. Active TB triggers an immune response, forming granulomas in the lungs.
Symptoms: Persistent cough, blood-tinged sputum, fever, night sweats, weight loss.
Diagnosis: Chest X-ray, tuberculin skin test, sputum analysis.
Treatment: Multiple antibiotics for active TB; single antibiotic for latent TB.

COVID-19
COVID-19 is caused by SARS-CoV-2 and primarily affects the respiratory system. It spreads via airborne droplets and can cause a range of symptoms, from mild to severe respiratory distress (ARDS).
Symptoms: Vary by strain; may include fever, cough, dyspnea, loss of taste/smell, night sweats, sore throat.
High-Risk Groups: Elderly, smokers, those with chronic diseases, immunocompromised individuals.
Complications: ARDS, multi-organ involvement, high mortality in severe cases.
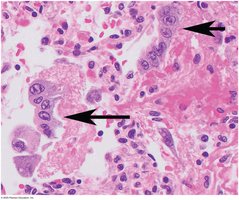
Influenza
Influenza (the "flu") is a viral infection of the respiratory epithelium, causing inflammation, increased mucus, and cell destruction. It is highly contagious and mutates frequently, requiring annual vaccination.
Symptoms: Fever, rhinorrhea, cough, muscle aches, sore throat, fatigue.
Complications: Secondary bacterial infections, high mortality in certain strains (e.g., 1918 pandemic).
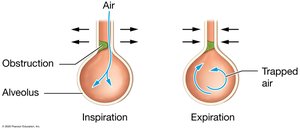
Restrictive and Obstructive Lung Diseases
Respiratory diseases are classified as restrictive or obstructive based on their effects on lung function.
Restrictive Diseases: Decrease pulmonary compliance and inspiratory capacity (e.g., idiopathic pulmonary fibrosis, pneumoconiosis, neuromuscular diseases).
Obstructive Diseases: Increase airway resistance, making expiration difficult (e.g., COPD, emphysema, chronic bronchitis, asthma).
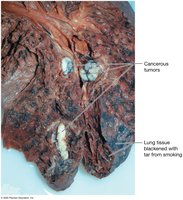
Lung Cancer
Lung cancer arises from the epithelium of the bronchi, bronchioles, or alveoli. It is the leading cause of cancer death and is strongly associated with smoking and exposure to carcinogens.
Symptoms: Cough, blood-streaked sputum, chest pain, recurrent infections.
Treatment: Surgery, radiation, chemotherapy.
Summary Table: Function and Composition of Regions of the Conducting and Respiratory Zones
Region | Function | Epithelium/Structure |
|---|---|---|
Nasal cavity | Warm, humidify, filter air | Pseudostratified ciliated columnar epithelium |
Pharynx | Passage for air and food; immune defense | Stratified squamous epithelium (oropharynx, laryngopharynx) |
Larynx | Sound production; airway protection | Stratified squamous (superior), pseudostratified ciliated columnar (inferior) |
Trachea/Bronchi | Conduct air; trap debris | Pseudostratified ciliated columnar; cartilage support |
Bronchioles | Control airflow | Simple cuboidal; smooth muscle |
Alveoli | Gas exchange | Simple squamous; surfactant-producing cells |
