 Back
BackThe Respiratory System: Structure, Function, and Physiology
Study Guide - Smart Notes

The Respiratory System: An Overview
Introduction to the Respiratory System
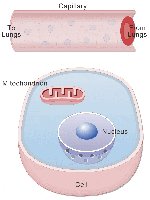
The respiratory system is essential for supplying oxygen to body cells and removing carbon dioxide, a waste product of metabolism. This system works closely with the cardiovascular system to ensure efficient gas exchange and transport throughout the body.
Oxygen is required for cellular ATP production.
Carbon dioxide must be removed to prevent toxic accumulation.
Gas exchange occurs via diffusion across lung surfaces and is transported by the blood.
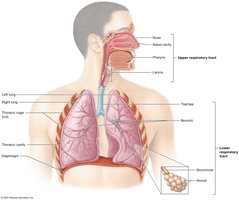
Major Organs and Divisions
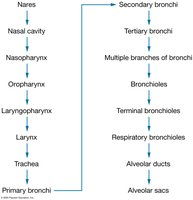
Upper respiratory system: Nose, nasal cavity, paranasal sinuses, pharynx
Lower respiratory system: Larynx, trachea, bronchi, bronchioles, alveoli
Function: Upper system filters, warms, and humidifies air; lower system conducts air, produces sound, and enables gas exchange.
Functional Divisions
Conducting portion: Nasal cavity to terminal bronchioles (air conduction only)
Respiratory portion: Respiratory bronchioles and alveoli (site of gas exchange)
Histology of the Respiratory Tract
Respiratory Mucosa
The respiratory mucosa lines the conducting portion and consists of an epithelial layer and a deeper lamina propria. It contains mucous glands and, in some regions, smooth muscle.
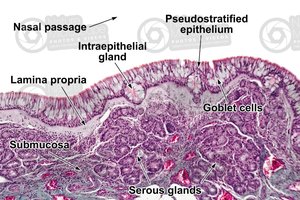
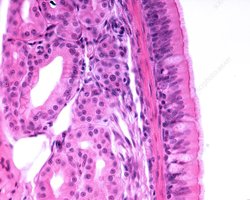
Types of Respiratory Epithelium
Pseudostratified ciliated columnar epithelium: Nasal cavity, nasopharynx, superior lower respiratory tract
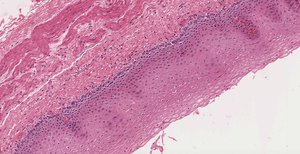
Stratified squamous epithelium: Inferior pharynx, oropharynx, laryngopharynx
Cuboidal epithelium: Smaller bronchioles
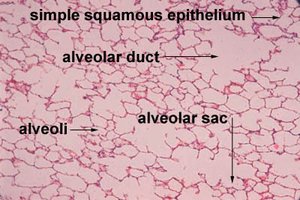
Simple squamous epithelium: Alveoli (site of gas exchange)
Respiratory Defense System
Nasal hairs: Filter large particles
Mucous/goblet cells: Trap debris and pathogens
Cilia: Sweep mucus toward the pharynx
Alveolar macrophages: Engulf small particles in the lungs
Anatomy of the Upper Respiratory Tract
Nose and Nasal Cavity
Lined with pseudostratified ciliated columnar epithelium
Functions: Warm, humidify, filter air; house olfactory receptors
Bony projections: Superior, middle, and inferior nasal conchae create turbulence
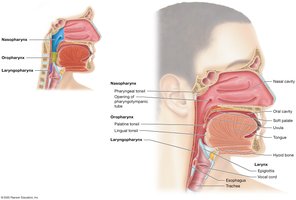
Pharynx
Nasopharynx: Pseudostratified ciliated columnar epithelium; contains pharyngeal tonsil
Oropharynx: Stratified squamous epithelium; contains palatine and lingual tonsils
Laryngopharynx: Stratified squamous epithelium
Anatomy of the Lower Respiratory Tract
Larynx
Cartilaginous structure surrounding the glottis
Main cartilages: Thyroid, cricoid, epiglottis
Functions: Protect airway, produce sound, prevent food entry during swallowing
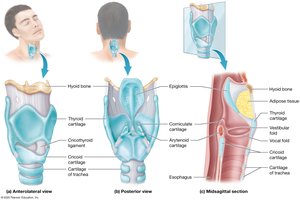
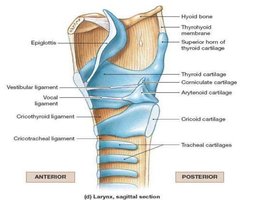
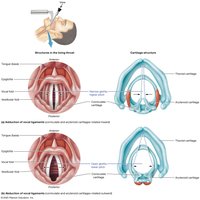
Trachea
Conducts air to the bronchi
Supported by C-shaped hyaline cartilage rings
Carina: Contains sensory receptors for cough reflex
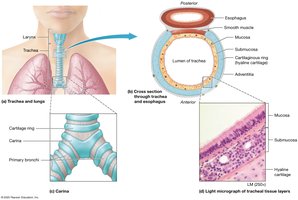
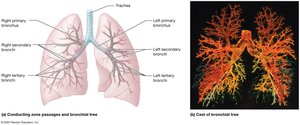
Bronchial Tree
Primary bronchi branch into secondary (lobar) and tertiary (segmental) bronchi
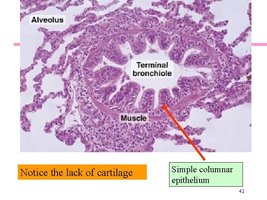
Bronchioles: Smallest airways, lack cartilage, lined by simple cuboidal epithelium
Terminal bronchioles: Final part of conducting airways
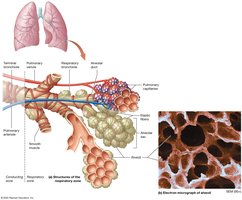
Alveoli and the Respiratory Membrane
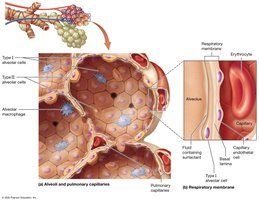
Alveoli: Air-filled sacs where gas exchange occurs
Respiratory membrane: Formed by alveolar and capillary walls and their fused basement membranes
Type I alveolar cells: Simple squamous cells for diffusion
Type II alveolar cells: Produce surfactant to reduce surface tension
Alveolar macrophages: Phagocytose debris
The Lungs and Pleurae
Lung Structure
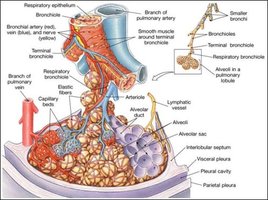
Lungs are divided into lobes and further into pulmonary lobules by connective tissue partitions (trabeculae and interlobular septa)
Each terminal bronchiole supplies a pulmonary lobule
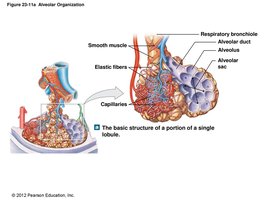
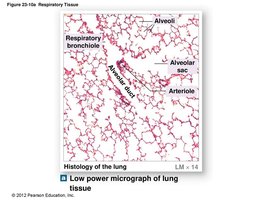
Respiratory bronchioles connect to alveoli via alveolar ducts and sacs
Pleural Cavities and Membranes
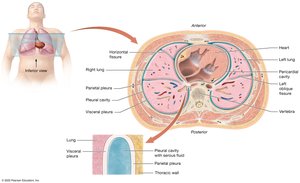
Each lung is enclosed in a pleural cavity lined by a double-layered serous membrane (pleura)
Parietal pleura: Lines thoracic wall
Visceral pleura: Covers lung surface
Pleural fluid lubricates and reduces friction, maintaining surface tension
Mechanics of Breathing
Pressure-Volume Relationship (Boyle’s Law)
Boyle’s Law states that the pressure of a gas is inversely proportional to its volume, provided the number of gas molecules is constant:
As the thoracic cavity volume increases, pressure decreases, allowing air to flow in (inhalation). As volume decreases, pressure increases, pushing air out (exhalation).
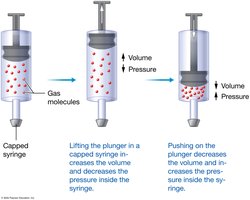
Pulmonary Ventilation
Driven by pressure gradients between atmospheric and intrapulmonary pressures
Intrapleural pressure remains below atmospheric pressure, keeping lungs inflated
Tidal volume: Amount of air moved in and out during a single respiratory cycle
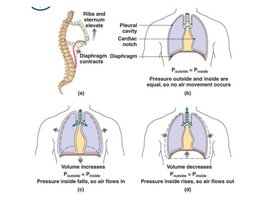
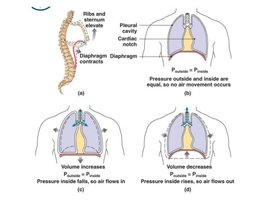
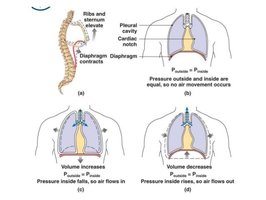
Respiratory Muscles
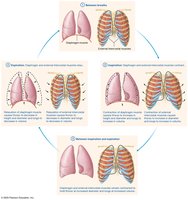
Diaphragm: Main muscle for inhalation
External intercostals: Assist in elevating the ribcage
Accessory muscles: Used during forced breathing
Normal exhalation is passive (elastic recoil); forced exhalation uses accessory muscles
Gas Exchange and Transport
Pulmonary Gas Exchange (External Respiration)
Oxygen diffuses from alveoli to blood; carbon dioxide diffuses from blood to alveoli
Occurs across the thin respiratory membrane
Tissue Gas Exchange (Internal Respiration)
Oxygen diffuses from blood to tissues; carbon dioxide diffuses from tissues to blood
Oxygen Transport
Most oxygen is transported bound to hemoglobin in erythrocytes
Oxygen loading and unloading depend on partial pressures and affinity of hemoglobin
Carbon Dioxide Transport
Transported in three forms:
Dissolved in plasma (7–10%)
Bound to hemoglobin as carbaminohemoglobin (20%)
As bicarbonate ions in plasma (70%)
Conversion to bicarbonate is catalyzed by carbonic anhydrase:
Control of Respiration
Neural Control Centers
Medulla oblongata: Dorsal (DRG) and ventral (VRG) respiratory groups
Pons: Pontine respiratory group (pneumotaxic center)
Regulate rate and depth of breathing in response to blood gas levels and pH
Chemoreceptor Reflexes
Central and peripheral chemoreceptors monitor CO2, O2, and pH
Adjust ventilation to maintain homeostasis
Noninfectious Respiratory Diseases
Restrictive Lung Diseases
Decreased pulmonary compliance
Reduced inspiratory capacity, vital capacity, and total lung capacity
Obstructive Lung Diseases
Increased airway resistance, decreased efficiency of expiration
Examples: Chronic Obstructive Pulmonary Disease (COPD), emphysema, asthma
Asthma: Hyperresponsive airways, bronchoconstriction, inflammation, increased mucus
