 Back
BackThe Skeletal System: Structure, Function, and Development
Study Guide - Smart Notes

The Skeletal System
Skeletal Divisions: Axial and Appendicular
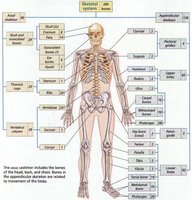
The human skeleton is divided into two main regions: the axial skeleton and the appendicular skeleton. The axial skeleton includes the bones of the head, neck, and trunk, while the appendicular skeleton consists of the bones of the limbs and girdles, which are involved in movement.
Axial Skeleton: Skull, vertebral column, thoracic cage (ribs and sternum)
Appendicular Skeleton: Pectoral girdle, pelvic girdle, upper and lower limbs
Function: Axial skeleton provides support and protection; appendicular skeleton facilitates movement.
Functions of the Skeletal System
Support, Protection, Movement, Blood Cell Production, Storage
The skeletal system performs several essential functions for the body:
Support: Provides structural framework for the body and supports organs.
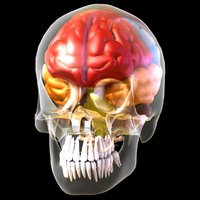
Protection: Shields vital organs such as the brain (cranium), heart and lungs (thoracic cage), and pelvic organs (pelvic girdle).
Movement: Bones act as levers for muscles, enabling movement.
Blood Cell Production: Hemopoiesis occurs in bone marrow, producing red and white blood cells.
Storage of Minerals: Stores calcium and phosphorus, essential for metabolic functions.
Storage of Energy: Adipose tissue in yellow bone marrow stores energy.
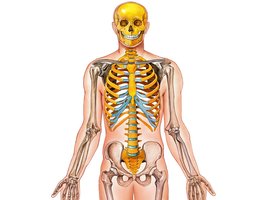
Bones Protect Organs and Support Body Posture
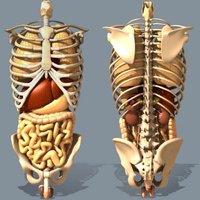
Bones are crucial for protecting internal organs and maintaining posture. The thoracic cage protects the lungs and heart, the pelvic girdle protects pelvic organs, and the cranium protects the brain.
Thoracic Cage: Ribs and sternum shield the heart and lungs.
Pelvic Girdle: Protects organs in the pelvic cavity.
Cranium: Encases and protects the brain.
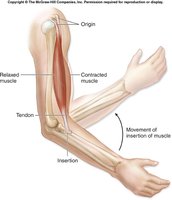
Movement: Bones Act as Levers
Bones themselves do not move; muscles contract and pull on bones, causing movement. This lever system is fundamental to locomotion and manipulation of the environment.
Lever Principle: Muscles attach to bones via tendons and contract to move bones at joints.
Example: The forearm moves when the biceps muscle contracts, pulling the radius and ulna.
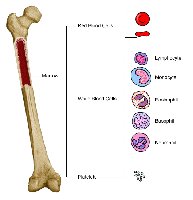
Blood Cell Production: Hemopoiesis
Blood cells are produced in the bone marrow, a process known as hemopoiesis. Red marrow is the site of new red blood cell (RBC) production.
Red Marrow: Found in trabecular cavities of spongy bone and flat bones.
Hemopoiesis: Production of RBCs, WBCs, and platelets.
Bones Store Adipose, Calcium, and Phosphate
Bones serve as reservoirs for minerals and energy. The mineral calcium phosphate, known as hydroxyapatite, is the primary component of bone matrix.
Hydroxyapatite: is the main mineral in bone.
Adipose Storage: Yellow marrow stores fat for energy.

Bone Shapes and Classification
Types of Bones
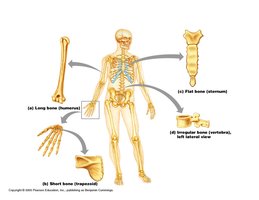
Bones are classified by their shapes, which relate to their functions:
Long Bones: Longer than they are wide; found in limbs; contain medullary cavity and growth plate.
Short Bones: Cube-shaped; found in wrists and ankles; includes sesamoid bones like the patella.
Flat Bones: Thin, flattened, and often curved; found in sternum, scapulae, ribs, and skull.
Irregular Bones: Complex shapes; vertebrae and hip bones.
Bones as Organs
Bone Tissue Composition
Bones are organs composed of several tissue types:
Bone Tissue: Includes compact and spongy bone.
Nervous Tissue: Present in nerves within bone.
Blood Tissue: Found in blood vessels.
Cartilage Tissue: Articular cartilage at joints.
Epithelial Tissue: Lines blood vessels.
The average adult skeleton contains 206 bones.
Bone Tissue Structure
Compact and Spongy Bone
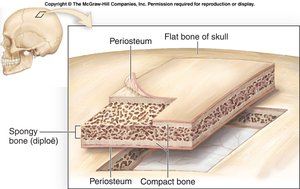
Bone tissue is organized into two main types:
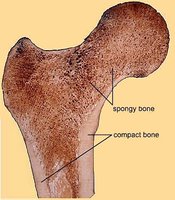
Compact Bone: Dense outer layer; appears smooth and solid; contains osteons (Haversian systems).
Spongy Bone: Honeycomb structure of trabeculae; spaces filled with red or yellow bone marrow.

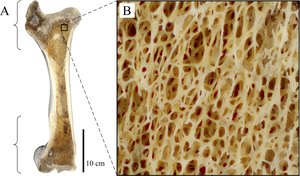
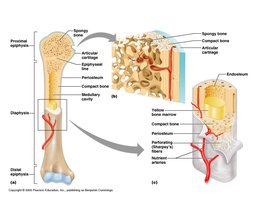
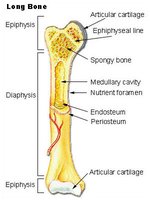
Structure of a Typical Long Bone
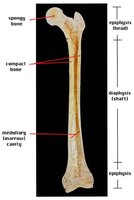
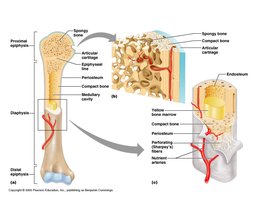
Long Bone Anatomy
A typical long bone consists of several distinct regions:
Diaphysis: Shaft of the bone.
Epiphysis: Ends of the bone.
Metaphysis: Region between diaphysis and epiphysis.
Articular Cartilage: Covers joint surfaces.
Medullary Cavity: Central cavity containing marrow.
Endosteum: Internal membrane lining the cavity.
Periosteum: External membrane covering bone.
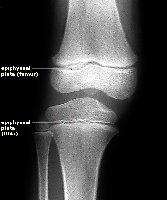
Epiphyseal Plate and Line
The epiphyseal plate is a region of cartilage that allows for bone growth in length. As maturity is reached, it becomes the epiphyseal line.
Epiphyseal Plate: Site of longitudinal growth in children and adolescents.
Epiphyseal Line: Remnant of plate in adults, indicating cessation of growth.
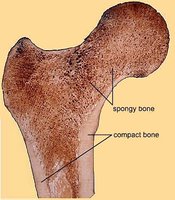
Compact and Spongy Bone Location
Compact bone forms the outer layer of all bones, providing strength and protection. Spongy bone is found inside, filled with marrow.
Compact Bone: External armor for softer internal bone.
Spongy Bone: Internal, filled with red or yellow marrow.
Red and Yellow Marrow
Bone marrow exists in two forms: red and yellow. Red marrow is the site of hematopoiesis, while yellow marrow stores fat.
Red Marrow: Found in spongy bone and flat bones; produces blood cells.
Yellow Marrow: Found in medullary cavity of long bones; stores adipose tissue.
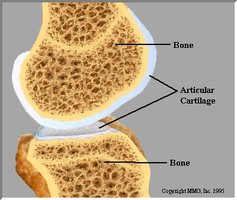
Articular Cartilage
Articular cartilage is made of hyaline cartilage and covers the surfaces of bones at synovial joints, providing a smooth, slippery surface for movement.
Location: Surrounds epiphysis in joints such as hip, knee, elbow, fingers, and shoulder.
Function: Reduces friction and absorbs shock.
Periosteum and Endosteum
The periosteum is a double membrane covering the external surface of bones, except at joints. The endosteum is a delicate membrane lining the internal surfaces.
Periosteum: Contains osteogenic stem cells; involved in bone growth and repair.
Endosteum: Covers trabeculae and lines canals; also contains osteogenic cells.
Bone Cells
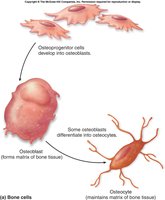
Types of Bone Cells
Bone tissue contains five main types of cells, each with specific functions:
Osteoprogenitor Cells: Stem cells that differentiate into osteoblasts or bone-lining cells.
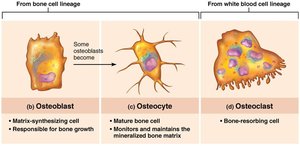
Osteoblasts: Immature cells that synthesize bone matrix; promote bone deposition.
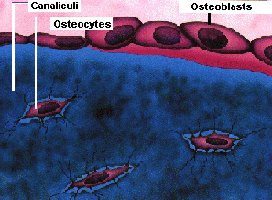
Osteocytes: Mature osteoblasts that maintain bone matrix; responsive to mechanical stress.
Bone-lining Cells: Maintain bone matrix; periosteal (external) and endosteal (internal).
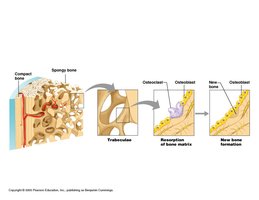
Osteoclasts: Derived from white blood cells; break down bone matrix (bone resorption).

Bone Matrix and Structure
Extracellular Matrix
The bone matrix consists of protein fibers and ground substance:
Collagen: Provides tensile strength.
Ground Substance: Mainly calcium phosphate (hydroxyapatite); minimal water content.
Structure of Compact Bone
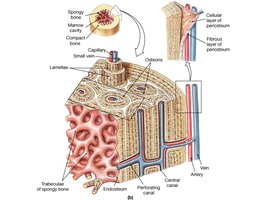
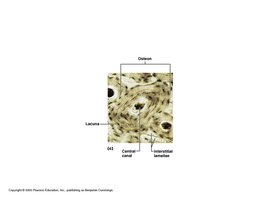
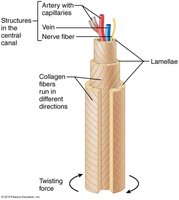
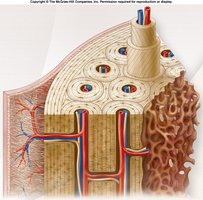
Compact bone is organized into osteons (Haversian systems), which are cylindrical structures that provide strength and resist twisting.
Osteons: Structural units; contain central canal, concentric lamellae, and canaliculi.
Lamellae: Collagen fibers run in alternating directions for strength.
Canaliculi: Small channels connecting lacunae; allow communication and nutrient/waste exchange.
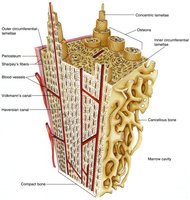
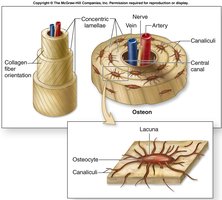
Canaliculi and Osteocyte Communication
Canaliculi are microscopic channels that connect osteocytes in their lacunae, facilitating communication and nutrient transfer.
Function: Deliver nutrients, remove wastes, and allow osteocytes to communicate.
Importance: Essential for cell survival in dense bone matrix.
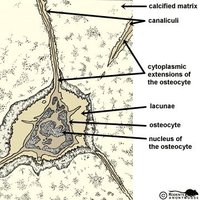
Types of Lamellae
There are three types of lamellae in compact bone:
Interstitial Lamellae: Fill spaces between osteons.
Circumferential Lamellae: Encircle the inner and outer surfaces of bone.
Concentric Lamellae: Form the rings of osteons around the central canal.
Spongy bone contains lamellae arranged as trabeculae.
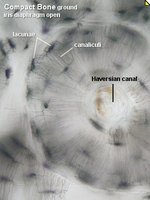
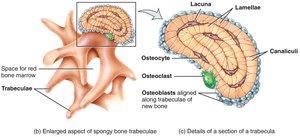
Differences Between Compact and Spongy Bone
Compact bone is dense and organized into osteons, while spongy bone is less dense and organized into trabeculae.
Compact Bone: Osteons, central canals, lamellae.
Spongy Bone: Trabeculae, marrow spaces, no osteons.
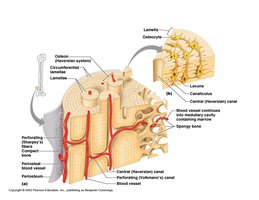
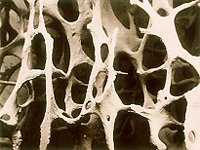
Structure of Spongy Bone
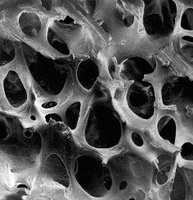
Spongy bone consists of trabeculae, which form a honeycomb structure filled with bone marrow, blood vessels, and nerves.
Trabeculae: Plates of lamellae; irregularly arranged.
Marrow Spaces: Filled with red or yellow bone marrow.
Spongy Bone Marrow Types
Spongy bone contains two types of marrow:
Red Bone Marrow: Site of hematopoiesis; found in epiphysis of long bones, flat bones, and some irregular bones.
Yellow Bone Marrow: Stores triglycerides; found in medullary cavity of long bones.
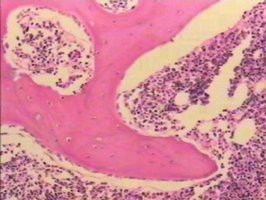
Spongy Bone Cells and Trabeculae
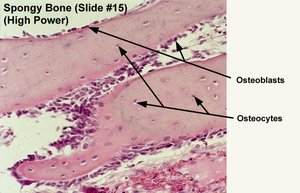
Spongy bone contains osteocytes within trabeculae, which are bridges of lamellae. Trabeculae are irregularly arranged and provide structural support.
Osteocytes: Found within trabeculae.
Trabeculae: Irregular bridges; affected in osteoporosis.

Bone Development and Ossification
Ossification (Osteogenesis)
Ossification is the process of bone tissue formation, occurring during embryonic development, postnatal growth, remodeling, and fracture repair.
Embryonic Development: Formation of bony skeleton begins in month 2.
Postnatal Growth: Continues until early adulthood.
Remodeling and Repair: Lifelong maintenance and response to trauma.
Fetal Skeleton Bone Formation
Most bones are formed through endochondral ossification, while skull bones are formed through intramembranous ossification.
Endochondral Ossification: Bone replaces hyaline cartilage.
Intramembranous Ossification: Bone develops from fibrous membrane.
Intramembranous Ossification
Bone develops within sheets or membranes of connective tissue, primarily forming flat bones of the skull, jaw, and clavicles.
Mesenchyme: Directly forms bone tissue.
Membrane Bones: Flat bones formed by this process.
Endochondral Ossification
Most bones are formed by endochondral ossification, where bone replaces an existing hyaline cartilage model.
Process: Mesenchyme to hyaline cartilage to bone tissue.
Timeline: Begins late in 2nd month of development; continues until early adulthood.
Bone Growth: Interstitial and Appositional
Long bones grow in length by interstitial growth at the epiphyseal plate and in thickness by appositional growth.
Interstitial Growth: Lengthwise growth at epiphyseal plate.
Appositional Growth: Increase in thickness by adding new layers to bone surface.
Bone Remodeling and Hormonal Regulation
Bone Remodeling
Bone remodeling involves both deposition and resorption, coordinated by osteoblasts and osteoclasts. Remodeling is influenced by genetics, hormones, and mechanical stress.
Remodeling Cycle: About every 7-10 years, the skeleton is renewed.
Regulation: Controlled by hormones and mechanical forces.
Hormonal Controls: PTH and Calcitonin
Parathyroid hormone (PTH) and calcitonin regulate blood calcium levels and bone remodeling.
PTH: Stimulates osteoclasts to increase blood calcium.
Calcitonin: Inhibits osteoclasts and stimulates osteoblasts to decrease blood calcium.
Developmental Aspects and Bone Disorders
Developmental Changes
Bone formation exceeds resorption in children and adolescents, is balanced in young adults, and resorption exceeds formation in older adults.
At Birth: Most long bones ossified except at epiphyses.
Adulthood: Bone mass and mineralization decrease with age.
Bone Disorders: Osteomalacia, Rickets, and Osteoporosis
Several disorders affect bone health:
Osteomalacia: Poor mineralization; soft, weak bones; pain with weight bearing.
Rickets: Osteomalacia in children; bowed legs and bone deformities; caused by vitamin D deficiency or insufficient calcium.
Osteoporosis: Bone resorption exceeds deposition; bone mass declines; most common in postmenopausal women.
Risk Factors: Age, gender, hormonal changes, dietary deficiencies.
Disorder | Cause | Symptoms | Prevention/Treatment |
|---|---|---|---|
Osteomalacia | Poor mineralization | Soft, weak bones | Vitamin D, calcium supplementation |
Rickets | Vitamin D deficiency | Bowed legs, bone deformities | Vitamin D fortification |
Osteoporosis | Bone resorption > deposition | Bone mass loss, fractures | Hormone therapy, calcium, exercise |
*Additional info: Academic context and expanded explanations were added to ensure completeness and clarity for college-level study.*
