 Back
BackThe Stomach: Anatomy, Physiology, and Regulation
Study Guide - Smart Notes

The Stomach: Anatomy and Function
Gross Anatomy of the Stomach
The stomach is a muscular, J-shaped organ that serves as a temporary storage tank and initiates the chemical breakdown of proteins. It converts the ingested bolus of food into a semi-fluid paste called chyme. When empty, the stomach's mucosa forms folds known as rugae, which allow for expansion as the stomach fills.
Cardial part (cardia): Surrounds the cardial orifice where the esophagus enters the stomach.
Fundus: Dome-shaped region beneath the diaphragm.
Body: The midportion and largest region of the stomach.
Pyloric part: Includes the antrum and pyloric canal, ending at the pylorus, which is continuous with the duodenum via the pyloric valve (a sphincter controlling stomach emptying).
Greater curvature: Convex lateral surface of the stomach.
Lesser curvature: Concave medial surface of the stomach.
The stomach receives autonomic innervation:
Sympathetic fibers: From thoracic splanchnic nerves via the celiac plexus.
Parasympathetic fibers: Supplied by the vagus nerve.
Microscopic Anatomy of the Stomach
The stomach wall consists of four tunics, with modifications in the muscularis and mucosa:
Muscularis externa: Contains three layers: circular, longitudinal, and an additional oblique (diagonal) layer. These layers allow the stomach to churn, mix, and propel chyme, enhancing mechanical digestion.
Mucosa: Composed of simple columnar epithelium entirely made up of mucous cells. These cells secrete a two-layer mucus that traps a bicarbonate-rich fluid beneath it, protecting the stomach lining.
The mucosa is dotted with gastric pits leading to gastric glands that produce gastric juice.
Types of Gland Cells in the Stomach
Gastric glands in the fundus and body produce most of the gastric juice. The main secretory cells include:
Mucous neck cells: Secrete thin, acidic mucus (function not fully understood).
Parietal cells: Secrete hydrochloric acid (HCl) (pH 1.5–3.5; denatures proteins, activates pepsin, breaks down plant cell walls, kills bacteria) and intrinsic factor (required for vitamin B12 absorption).
Chief cells: Secrete pepsinogen (inactive enzyme, activated to pepsin by HCl and pepsin itself) and gastric lipases (digest ~15% of lipids).
Enteroendocrine cells: Secrete chemical messengers (serotonin, histamine, somatostatin, gastrin) into the lamina propria, acting as paracrines or hormones.
Mucosal Barrier
The stomach is protected from self-digestion by the mucosal barrier, which consists of:
Thick layer of bicarbonate-rich mucus
Tight junctions between epithelial cells
Rapid replacement of damaged epithelial cells by stem cell division
Clinical—Homeostatic Imbalances
Gastritis: Inflammation caused by anything that breaches the mucosal barrier.
Peptic or gastric ulcers: Erosions in the stomach wall, potentially leading to peritonitis or hemorrhage. Most ulcers are caused by Helicobacter pylori infection or NSAIDs (e.g., aspirin).
The Stomach: Digestive Functions
Digestive Roles of the Stomach
Breaks down food mechanically and chemically
Acts as a holding area for food
Delivers chyme to the small intestine
Denatures proteins via HCl
Pepsin carries out enzymatic digestion of proteins
Absorbs lipid-soluble substances (e.g., alcohol, aspirin)
Secretion of intrinsic factor for vitamin B12 absorption (essential for life)
Regulation of Gastric Secretion
Gastric secretion is regulated by neural and hormonal mechanisms:
Neural: Vagus nerve stimulation increases secretion; sympathetic stimulation decreases secretion.
Hormonal: Gastrin stimulates HCl secretion; antagonistic hormones from the small intestine inhibit it.
Gastric secretion occurs in three phases:
Cephalic (reflex) phase: Triggered by sight, aroma, taste, or thought of food.
Gastric phase: Initiated by stomach distension and chemical stimuli (e.g., partially digested proteins, caffeine, low acidity), leading to gastrin release from G cells, which stimulates HCl secretion by parietal cells.
Intestinal phase: Begins as chyme enters the small intestine, causing a brief stimulatory effect, followed by inhibition (enterogastric reflex and enterogastrones such as secretin and CCK) to prevent overfilling.
Mechanism of HCl Formation
Parietal cells pump H+ (from carbonic acid breakdown) into the stomach lumen via H+/K+ ATPase (proton pumps).
As H+ is pumped into the lumen, HCO3− is exported to the blood via Cl−/HCO3− antiporter.
This causes an increase in blood HCO3− (the "alkaline tide").
Cl− is pumped into the lumen to combine with H+, forming HCl.
Equation for HCl formation:
is pumped into the lumen, enters the blood, and joins $\mathrm{H^+}$ in the lumen to form .
Regulation of Gastric Motility and Emptying
Stomach Response to Filling
Receptive relaxation: Reflex-mediated relaxation of smooth muscle coordinated by the swallowing center in the brainstem.
Gastric accommodation: The stomach's intrinsic ability to stretch without increasing tension or contractions.
Gastric Contractile Activity
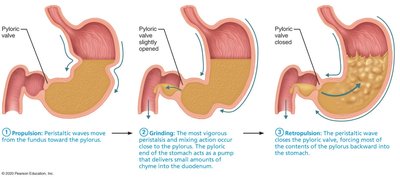
The stomach contracts to mix and propel chyme toward the pylorus. The pyloric region acts as a pump, delivering small amounts of chyme to the duodenum while forcing most of it backward for further mixing (retropulsion).
Regulation of Gastric Emptying
The duodenum regulates gastric emptying by responding to stretch and chemical signals.
Enterogastric reflex and enterogastrones (secretin, CCK) inhibit gastric secretion and slow duodenal filling to prevent overloading.
Clinical—Homeostatic Imbalance: Vomiting (Emesis)
Caused by extreme stretching or irritants (bacterial toxins, excessive alcohol, spicy food, certain drugs).
Sensory impulses stimulate the emetic center in the medulla.
Excessive vomiting can lead to dehydration, electrolyte, and acid-base imbalances (alkalosis).
Cell Type | Secretion | Function |
|---|---|---|
Mucous neck cells | Thin, acidic mucus | Unknown |
Parietal cells | HCl, Intrinsic factor | Protein denaturation, pepsin activation, vitamin B12 absorption |
Chief cells | Pepsinogen, Gastric lipase | Protein and lipid digestion |
Enteroendocrine cells | Serotonin, histamine, somatostatin, gastrin | Regulation of digestive processes |
Additional info: The stomach's ability to regulate its secretory and motor functions is essential for efficient digestion and protection of the gastrointestinal tract. Disorders such as ulcers and gastritis highlight the importance of the mucosal barrier and regulatory mechanisms.
