 Back
BackThe Urinary System: Filtration, Reabsorption, Secretion, and Urine Properties
Study Guide - Smart Notes

The Urinary System
Overview of Kidney Function
The urinary system is essential for maintaining homeostasis by filtering blood, removing waste, and regulating fluid and electrolyte balance. The kidneys perform three main processes: glomerular filtration, tubular reabsorption, and tubular secretion.
Filtration: Removal of water and solutes from blood into the nephron.
Reabsorption: Return of essential substances from filtrate back to blood.
Secretion: Addition of specific substances from blood into filtrate for excretion.
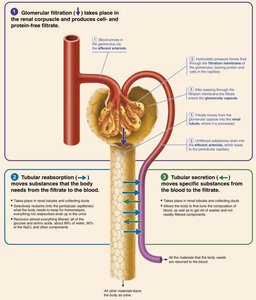
Glomerular Filtration
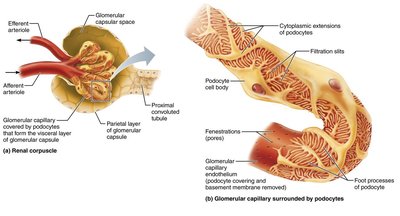
Glomerular filtration is a passive process that occurs in the renal corpuscle, producing cell- and protein-free filtrate. Hydrostatic pressure forces fluids and solutes through the filtration membrane into the glomerular capsule.
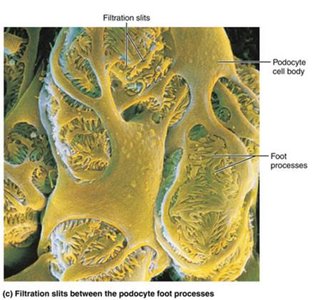
Filtration Membrane: Consists of fenestrated endothelium, basement membrane, and podocyte foot processes.
Excludes: Blood proteins and cells, allowing water and solutes smaller than plasma proteins to pass.
Clinical Implications: Damage increases permeability, leading to proteinuria or hematuria, and can cause edema due to loss of plasma proteins.
Pressures Affecting Filtration
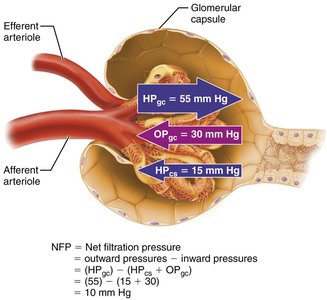
Filtration is governed by opposing pressures:
Outward Pressure: Hydrostatic pressure in glomerular capillaries (HPgc), pushing water and solutes out.
Inward Pressure: Hydrostatic pressure in capsular space (HPcs) and colloid osmotic pressure in capillaries (OPgc).
Net Filtration Pressure (NFP):
Clinical Implications: Low glomerular BP can cause anuria (abnormally low urine output).
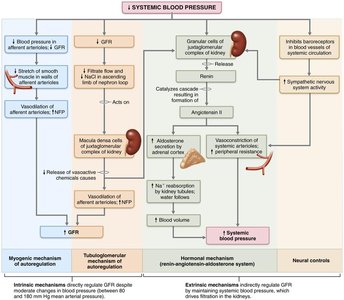
Regulation of Glomerular Filtration Rate (GFR)
GFR is the volume of filtrate formed per minute by both kidneys and is directly proportional to NFP and surface area available for filtration.
Intrinsic Controls: Renal autoregulation via myogenic and tubuloglomerular feedback mechanisms.
Extrinsic Controls: Neural and hormonal mechanisms (e.g., sympathetic nervous system, renin-angiotensin-aldosterone system) override intrinsic controls during extreme blood pressure changes.
Tubular Reabsorption
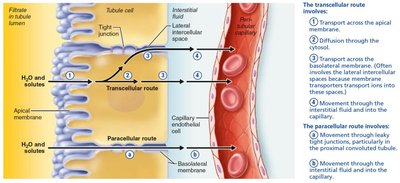
Tubular reabsorption quickly reclaims most tubular contents and returns them to the blood. It occurs via transcellular and paracellular routes.
Transcellular Route: Substance moves across tubule cell, through cytosol, and into interstitial fluid.
Paracellular Route: Substance passes between tubule cells, especially in proximal convoluted tubule (PCT).
Reabsorbed Substances: Almost all organic nutrients, water, ions (regulated by hormones).
Sodium and Water Reabsorption
Sodium is the most abundant cation in filtrate, and its reabsorption drives the reabsorption of other substances and water.
Primary Active Transport: Na+ exits tubule cells, maintaining low intracellular Na+.
Secondary Active Transport: Glucose, amino acids, and other solutes cotransported with Na+.
Water Reabsorption: Follows Na+ via osmosis through aquaporins; regulated by ADH.
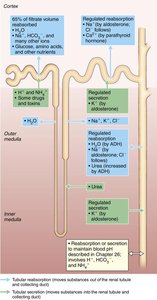
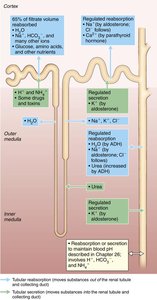
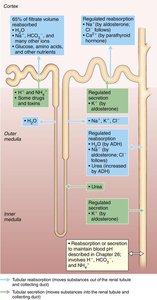
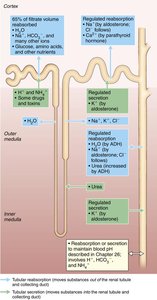
Reabsorptive Capabilities of Renal Tubules
Proximal Convoluted Tubule (PCT): Most active in reabsorption; reabsorbs all glucose, amino acids, 65% of Na+ and water.
Nephron Loop: Descending limb reabsorbs water; ascending limb reabsorbs solutes.
Distal Convoluted Tubule (DCT) and Collecting Duct (CD): Fine-tune reabsorption; regulated by hormones (ADH, aldosterone, parathyroid hormone).
Hormonal Regulation of Urine Volume
Antidiuretic Hormone (ADH): Increases water reabsorption in CD by increasing aquaporins.
Aldosterone: Increases Na+ reabsorption, raising blood volume and pressure.
Atrial Natriuretic Peptide (ANP): Inhibits Na+ reabsorption, increasing water loss.
Parathyroid Hormone (PTH): Increases Ca2+ reabsorption in DCT.
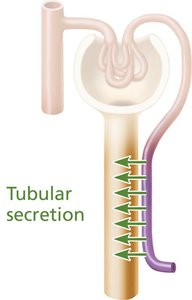
Tubular Secretion
Tubular secretion moves specific substances from blood into filtrate, providing another mechanism for waste removal and regulation of blood pH.
Secreted Substances: K+, H+, NH4+, creatinine, organic acids/bases.
Functions: Disposal of drugs/metabolites, elimination of reabsorbed wastes, regulation of K+ and pH.
Physical and Chemical Properties of Urine
Urinalysis is used to assess renal function and diagnose diseases. Normal urine is 95% water and 5% solutes, including nitrogenous wastes (urea, uric acid, creatinine) and ions (Na+, K+, PO43-, SO42-, Ca2+, Mg2+, HCO3-).
Color: Pale to deep yellow due to urobilin/urochrome; abnormal colors may indicate disease or diet.
Odor: Slightly aromatic; changes with diet or disease.
pH: Slightly acidic (average pH ~6, range 4.5–8).
Specific Gravity: Ratio of urine mass to mass of equal volume of distilled water.


Major Organs of the Urinary System
The urinary system consists of the kidneys, ureters, urinary bladder, and urethra.
Ureters: Transport urine from kidneys to bladder.
Urinary Bladder: Temporary storage of urine; highly distensible.
Trigone: Triangular area in bladder where infections tend to persist.
Urethra: Conducts urine out of the body.
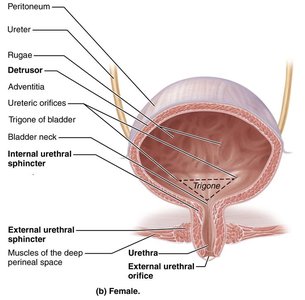
Micturition (Urination)
Micturition is the act of emptying the urinary bladder, requiring three simultaneous events:
Contraction of detrusor muscle by autonomic nervous system (ANS).
Opening of internal urethral sphincter by ANS.
Opening of external urethral sphincter by somatic nervous system.
Clinical Implications
Renal Calculi (Kidney Stones): Crystallized calcium, magnesium, or uric acid salts; can cause pain and obstruction.
Chronic Renal Disease: GFR < 60 ml/min for at least three months; seen in diabetes and hypertension.
Renal Failure: GFR < 15 ml/min; causes uremia and requires dialysis or transplant.
Process | Main Function | Key Substances |
|---|---|---|
Glomerular Filtration | Removes water and solutes from blood | Water, glucose, amino acids, nitrogenous wastes |
Tubular Reabsorption | Returns essential substances to blood | Na+, water, glucose, amino acids |
Tubular Secretion | Adds specific substances to filtrate | K+, H+, NH4+, drugs |
Additional info: The notes include expanded explanations of nephron function, clinical implications, and hormonal regulation for completeness and academic quality.
