 Back
BackThe Urinary System II: Filtration, Reabsorption, Secretion, and Regulation
Study Guide - Smart Notes

Chapter 25: The Urinary System II
Overview of Urine Formation
The urinary system maintains homeostasis by filtering blood, reabsorbing essential substances, secreting wastes, and excreting urine. The nephron is the functional unit of the kidney, with each kidney containing about 1 million nephrons. The processes of filtration, reabsorption, secretion, and excretion determine the final composition and volume of urine.
Filtration: Movement of plasma from glomerular capillaries into Bowman’s capsule.
Reabsorption: Return of filtered substances (e.g., glucose, amino acids, water) to the blood.
Secretion: Active transport of additional wastes from blood into the tubular fluid.
Excretion: Removal of urine from the body.
Example: About 180 L of plasma is filtered daily, but less than 1% is excreted as urine; the rest is reabsorbed.
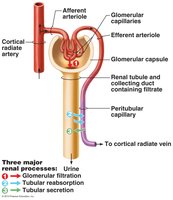
Microscopic Structure of the Nephron
The nephron consists of the renal corpuscle (glomerulus and Bowman’s capsule) and the renal tubule (proximal convoluted tubule, loop of Henle, distal convoluted tubule, and collecting duct). Blood enters the glomerulus via the afferent arteriole and exits via the efferent arteriole.
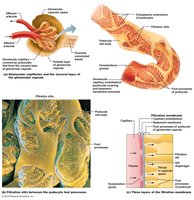
Glomerular Filtration Barrier: Composed of fenestrated endothelium, basement membrane, and podocytes.
Permeability: Allows passage of water and small solutes (<3 nm), but restricts proteins and cells.
Glomerular Filtration Rate (GFR) and Net Filtration Pressure (NFP)
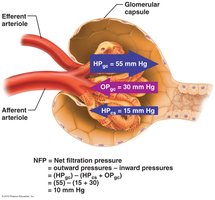
GFR is the volume of filtrate formed per minute by both kidneys (normal: 120–125 mL/min). NFP is determined by the balance of hydrostatic and oncotic pressures across the glomerular capillaries.
Forces: Hydrostatic pressure in glomerular capillaries (HPGC), colloid osmotic pressure (OPGC), and hydrostatic pressure in Bowman’s capsule (HPBC).
Equation:
Example Calculation:
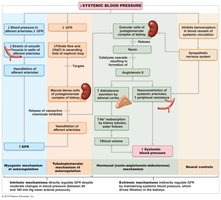
Regulation of Glomerular Filtration
GFR is tightly regulated by intrinsic (autoregulation) and extrinsic (neural and hormonal) mechanisms to maintain homeostasis and prevent kidney damage.
Intrinsic Controls: Myogenic mechanism (smooth muscle response to stretch) and tubuloglomerular feedback (macula densa senses NaCl).
Extrinsic Controls: Sympathetic nervous system (SNS) constricts afferent arterioles during stress; renin-angiotensin-aldosterone system (RAAS) increases blood pressure and GFR.
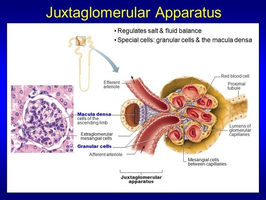
Juxtaglomerular Apparatus (JGA): Includes juxtaglomerular (granular) cells and macula densa, regulating renin release and GFR.
Tubular Reabsorption and Secretion
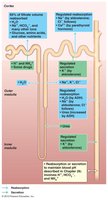
Reabsorption returns filtered substances to the blood, while secretion removes additional wastes. These processes occur along different segments of the nephron and are regulated by hormones and transport proteins.
Proximal Convoluted Tubule (PCT): Reabsorbs 100% glucose, amino acids, most water, and electrolytes.
Loop of Henle: Descending limb reabsorbs water; ascending limb reabsorbs Na+ and Cl-.
Distal Convoluted Tubule (DCT) and Collecting Duct (CD): Regulated reabsorption of Na+ (aldosterone), water (ADH), and Ca2+ (PTH); secretion of K+ and H+.
Transport Maximum (Tm): Maximum rate of reabsorption for substances like glucose; exceeded in diabetes mellitus, leading to glycosuria.
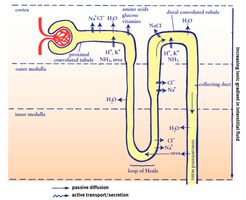
Countercurrent Mechanism and Medullary Osmotic Gradient
The countercurrent multiplier (loop of Henle) and countercurrent exchanger (vasa recta) establish and maintain the medullary osmotic gradient, allowing the kidney to concentrate urine.
Descending Limb: Permeable to water, not solutes.
Ascending Limb: Impermeable to water, actively transports NaCl out.
Collecting Duct: Water reabsorption regulated by ADH; urea recycling contributes to gradient.
Hormonal Regulation of Renal Function
Several hormones regulate kidney function to maintain fluid, electrolyte, and acid-base balance.
Antidiuretic Hormone (ADH): Increases water reabsorption in the collecting duct by inserting aquaporins.
Aldosterone: Increases Na+ reabsorption and K+ secretion in the DCT and CD.
Atrial Natriuretic Peptide (ANP): Inhibits Na+ reabsorption, increasing urine output.
Parathyroid Hormone (PTH): Increases Ca2+ reabsorption in the DCT.
Renal Clearance and Micturition
Renal clearance measures the kidney’s ability to remove a substance from the blood. Micturition is the process of urination, controlled by the micturition reflex and voluntary control.
Renal Clearance Equation: , where C = clearance, U = urine concentration, V = urine flow rate, P = plasma concentration.
Micturition Reflex: Involuntary contraction of the bladder, with voluntary control over the external urethral sphincter.
Disorders of the Urinary System
Common urinary disorders include chronic renal disease, renal failure, urinary tract infections (UTIs), kidney stones, and diabetes insipidus.
Chronic Renal Disease: GFR < 60 mL/min for over 3 months.
Renal Failure: GFR < 15 mL/min; requires dialysis.
UTI: Infection of the urinary tract, more common in females.
Kidney Stones: Crystallization of Ca2+ or Mg2+ in urine.
Diabetes Insipidus: Deficiency of ADH (central) or renal insensitivity (nephrogenic); causes polyuria and polydipsia.
Summary Table: Comparison of Filtration, Reabsorption, and Secretion
Process | Direction | Main Location | Substances Involved |
|---|---|---|---|
Filtration | Blood → Tubule | Glomerulus/Bowman’s Capsule | Water, ions, glucose, amino acids, small solutes |
Reabsorption | Tubule → Blood | PCT, LoH, DCT, CD | Water, glucose, amino acids, ions |
Secretion | Blood → Tubule | PCT, DCT, CD | K+, H+, drugs, metabolites |
Pathways of Substances Through the Kidney
Not Filtered: Aorta → Renal Artery → ... → Peritubular Capillaries → Renal Vein → Inferior Vena Cava
Filtered and Reabsorbed: Aorta → ... → Glomerulus → Bowman’s Capsule → PCT → Peritubular Capillary → Renal Vein
Filtered and Excreted: Aorta → ... → Glomerulus → Bowman’s Capsule → PCT → LoH → DCT → CD → Calyces → Renal Pelvis → Ureter → Bladder → Urethra
Additional info: For more details on acid-base balance and pH regulation, see Chapter 26.
