 Back
BackThe Urinary System: Renal Physiology and Urine Formation
Study Guide - Smart Notes

The Urinary System
Introduction to the Urinary System
The urinary system is responsible for filtering blood, removing waste products, and regulating fluid and electrolyte balance. The kidneys play a central role in these processes by forming urine through filtration, reabsorption, and secretion.
Renal Physiology: Overview
Composition of Urine
Ammonia (NH3): Produced by intestinal bacteria from digested proteins; processed in the liver and converted to urea.
Urea: Byproduct of amino acid metabolism.
Creatinine: Breakdown product of creatine phosphate from muscle metabolism.
Inorganic salts: Such as sodium chloride (NaCl) and potassium chloride (KCl).
Urobilin: Pigment from the breakdown of hemoglobin.
Uric acid: From the metabolism of nucleotides.
These waste products are dissolved in the bloodstream and eliminated in urine, with water loss accompanying their removal.
Solution Chemistry in Renal Physiology
Solution: A uniform mixture of two or more substances.
Solute: The substance dissolved (e.g., lemonade crystals).
Solvent: The dissolving agent (e.g., water).


Example: Lemonade crystals dissolved in water illustrate how waste products are dissolved in plasma and ultimately excreted as urine.
Osmolarity and Concentration of Urine
Osmolarity: The total number of solute particles per liter, expressed in osmoles per liter (Osm/L) or milliosmoles per liter (mOsm/L).
Kidneys produce concentrated urine (1000–1400 mOsm/L), about four times the plasma concentration.
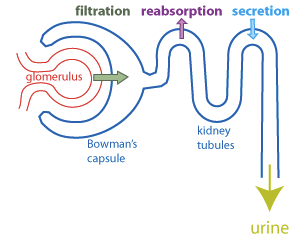
Basic Renal Processes
Filtration: Movement of water and solutes from blood into the nephron.
Reabsorption: Recovery of valuable substances from filtrate back into blood.
Secretion: Addition of waste products from blood into the filtrate.
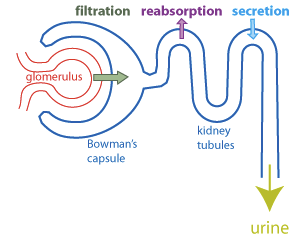
Kidney Functions
Concentrate filtrate produced by glomerular filtration.
Absorb and retain valuable materials (e.g., sugars, amino acids) for use by other tissues.
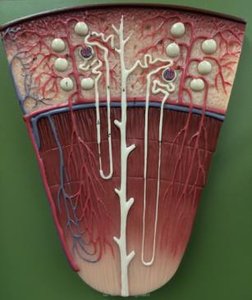
Filtration: Step 1
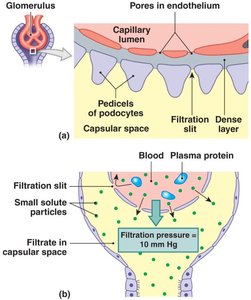
Filtration Membrane Structure
Capillary Endothelium: Fenestrated capillaries with pores (60–100 nm) that prevent passage of blood cells but allow solutes and some plasma proteins.
Lamina Densa: More selective, allowing only small plasma proteins, nutrients, and ions.
Filtration Slits: Openings (6–9 nm) that prevent passage of most small plasma proteins.
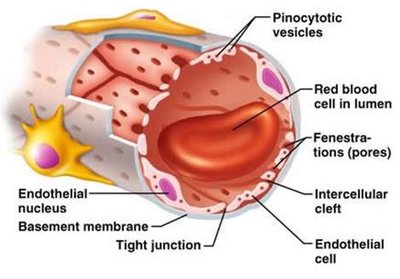
Analogy: Capillary endothelium is like a chain link fence, lamina densa like chicken wire, and filtration slits like a screen door—each layer provides increasing selectivity.
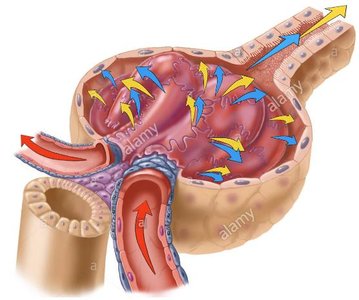


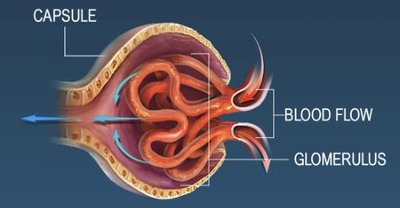
Filtration Pressures
Glomerular Hydrostatic Pressure (GHP): Blood pressure in glomerular capillaries (~50 mm Hg), pushing water and solutes into the filtrate.
Capsular Hydrostatic Pressure (CsHP): Opposes GHP (~15 mm Hg), pushing water and solutes back into plasma.
Net Hydrostatic Pressure (NHP): mm Hg
Blood Colloid Osmotic Pressure (BCOP): Draws water out of filtrate into plasma (~25 mm Hg), opposing filtration.
Filtration Pressure (FP): mm Hg

Glomerular Filtration Rate (GFR)
Amount of filtrate produced per minute (~125 mL/min).
About 180 liters of filtrate generated per day; 99% is reabsorbed.
GFR depends on filtration pressure; any change in pressure alters GFR.
Regulation of GFR
Autoregulation: Adjusts diameters of afferent/efferent arterioles and glomerular capillaries to maintain GFR.
Hormonal Regulation: Renin-angiotensin system increases GFR in response to low blood pressure or volume.
Autonomic Regulation: Sympathetic nervous system can decrease GFR during stress.

Renin–Angiotensin System
Triggered by low blood pressure, low blood volume, or sympathetic stimulation.
Leads to angiotensin II activation, which:
Constricts efferent arterioles, raising glomerular pressure and GFR.
Stimulates sodium and water reabsorption, aldosterone and ADH secretion, and thirst.

Reabsorption: Step 2
Overview of Reabsorption
Reabsorption recovers useful materials from the filtrate and occurs in all nephron segments except the renal corpuscle. The importance of reabsorption varies by nephron segment.
Transport Maximum and Renal Threshold
Carrier proteins in nephron cells have a maximum rate of transport.
If solute concentration exceeds this maximum, excess appears in urine (renal threshold).
Renal threshold for glucose: ~160–180 mg/dL; excess glucose in urine is called glycosuria.
Renal threshold for amino acids: ~65 mg/dL; excess in urine is aminoaciduria.
Secretion: Step 3
Overview of Secretion
Secretion adds waste products, toxins, and excess ions from blood into the filtrate. This process occurs in all nephron segments except the renal corpuscle, with varying importance by segment.
Secretion at the Distal Convoluted Tubule (DCT)
Removes substances not filtered at the glomerulus.
Secretion rates for potassium (K+) and hydrogen (H+) ions depend on their concentrations in peritubular fluid.
Countercurrent Multiplication in the Nephron Loop
Mechanism and Benefits
Countercurrent: Tubular fluids move in opposite directions in the nephron loop.
Multiplication: The effect of exchange increases as fluid movement continues.
Allows efficient reabsorption of water and solutes and establishes a concentration gradient for passive water reabsorption in the collecting system.
Loop of Henle Structure and Function
Thin Descending Limb: Permeable to water, relatively impermeable to solutes.
Thick Ascending Limb: Impermeable to water, actively transports Na+ and Cl- into medullary interstitium.
Role of Aldosterone and Antidiuretic Hormone (ADH)
Aldosterone: Increases Na+ reabsorption in DCT and collecting duct, reducing Na+ loss in urine.
ADH: Increases water permeability in DCT and collecting ducts, promoting water reabsorption and concentrating urine.
Both hormones are opposed by natriuretic peptides, which promote water and sodium loss.
Water Reabsorption and Urine Concentration
Osmosis in the Nephron
Water is reabsorbed by osmosis when the osmotic concentration of peritubular fluid exceeds that of tubular fluid.
Occurs primarily in the proximal convoluted tubule and descending limb of the nephron loop.
Effects of ADH
High ADH: More water channels, increased water reabsorption, concentrated urine.
Low ADH: Fewer water channels, less water reabsorption, dilute urine.
Vasa Recta Function
Returns solutes and water reabsorbed in the medulla to general circulation without disrupting the concentration gradient.

Composition and Concentration of Normal Urine
Urine is a clear, sterile solution with yellow color from urobilin.
Urinalysis is an important diagnostic tool.
Normal adult urine output: ~1200 mL/day (0.6% of filtrate), with osmotic concentration of 1000–1400 mOsm/L.

Summary of Renal Function by Location
Location | Main Function |
|---|---|
Glomerulus | Filtrate produced; similar to plasma minus proteins |
Proximal Convoluted Tubule (PCT) | Active reabsorption of ions and nutrients; water follows by osmosis |
PCT & Descending Limb | Obligatory water reabsorption; concentrates tubular fluid |
Thick Ascending Limb | Active transport of Na+ and Cl-; urea concentration increases |
DCT & Collecting Ducts | Final adjustments of volume and composition; ADH determines final urine concentration |
Vasa Recta | Maintains medullary concentration gradient |
Renal Pelvis | Urine production complete |
Key Terms and Concepts
Filtration: Occurs at the glomerulus; driven by hydrostatic and osmotic pressures.
Reabsorption: Movement of water and solutes from filtrate back into blood.
Secretion: Active transport of substances from blood into filtrate.
Countercurrent Multiplication: Mechanism in the nephron loop that concentrates urine.
Renal Threshold: Plasma concentration at which a substance begins to appear in urine.
Glycosuria: Glucose in urine, often due to diabetes mellitus.
Aminoaciduria: Amino acids in urine, often after a protein-rich meal.
