 Back
BackThe Urinary System: Structure and Function (Chapter 25 Study Notes)
Study Guide - Smart Notes

The Urinary System
Overview and Major Organs
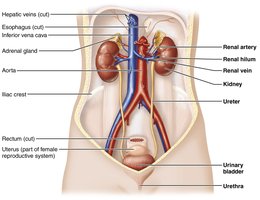
The urinary system is essential for maintaining the body's internal environment by regulating water, solute concentrations, and removing metabolic wastes. It consists of the kidneys, ureters, urinary bladder, and urethra.
Kidneys: Filter blood, regulate fluid and electrolyte balance, and produce urine.
Ureters: Transport urine from kidneys to the urinary bladder.
Urinary bladder: Temporarily stores urine.
Urethra: Conducts urine out of the body.
Functions of the Kidneys
The kidneys perform several vital functions to maintain homeostasis:
Regulate total body water volume and solute concentration
Regulate ion concentrations in extracellular fluid (ECF)
Maintain long-term acid-base balance
Excrete metabolic wastes, toxins, and drugs
Produce erythropoietin (stimulates RBC production) and renin (regulates blood pressure)
Activate vitamin D (calcitriol) for calcium regulation
Carry out gluconeogenesis during prolonged fasting
Gross Anatomy of the Kidneys
Location and External Structure
The kidneys are retroperitoneal, bean-shaped organs located in the superior lumbar region (T12–L3). The right kidney is slightly lower due to the liver. Each kidney is protected by the rib cage and is capped by an adrenal gland.
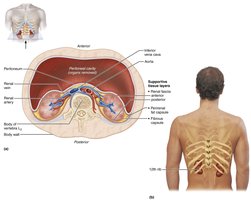
External Anatomy
Renal hilum: Medial indentation where ureters, blood vessels, lymphatics, and nerves enter/exit.
Supportive tissue layers:
Renal fascia: Anchoring outer layer of dense connective tissue
Perirenal fat capsule: Fatty cushion
Fibrous capsule: Transparent capsule preventing infection spread
Internal Gross Anatomy
The kidney has three main regions:
Renal cortex: Light-colored, superficial, granular appearance
Renal medulla: Darker, reddish-brown, contains cone-shaped pyramids
Renal pelvis: Funnel-shaped tube continuous with the ureter
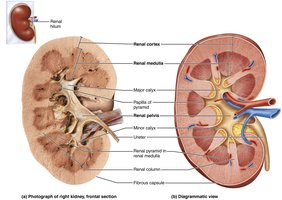
Renal Pyramids, Columns, and Calyces
Renal pyramids: Cone-shaped structures in the medulla; papilla points internally
Renal columns: Extensions of cortical tissue separating pyramids
Lobe: Each pyramid plus surrounding cortex (about 8 per kidney)
Major and minor calyces: Collect urine from papillae and funnel it into the renal pelvis
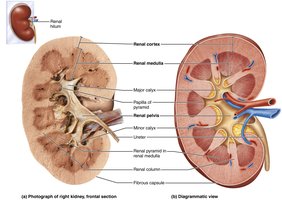
Urine Flow Pathway
Urine flows from the papilla of the pyramid → minor calyces → major calyces → renal pelvis → ureter → bladder.
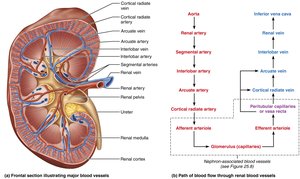
Blood Supply of the Kidneys
The kidneys receive about 25% of cardiac output per minute via the renal arteries. Blood flows through a series of arteries and capillaries, allowing for filtration and reabsorption.
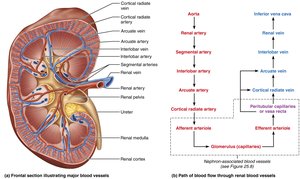
Nephrons: The Functional Units of the Kidney
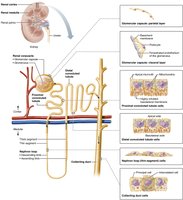
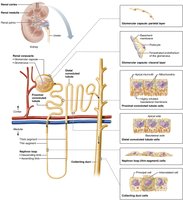
Structure of a Nephron
Each kidney contains about one million nephrons, which filter blood and form urine. Each nephron consists of a renal corpuscle and a renal tubule, and empties into collecting ducts.
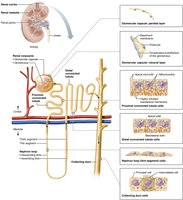
Renal Corpuscle
Glomerulus: Tuft of fenestrated capillaries; site of filtration
Glomerular (Bowman's) capsule: Surrounds the glomerulus; has parietal (simple squamous) and visceral (podocyte) layers
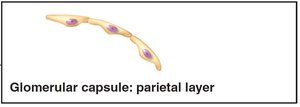
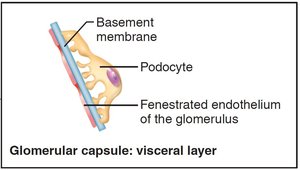
Renal Tubule and Collecting Duct
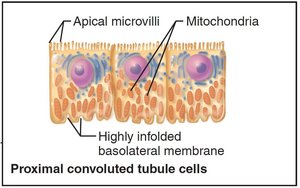
Proximal convoluted tubule (PCT): Cuboidal cells with microvilli for reabsorption and secretion
Nephron loop (Loop of Henle): Descending and ascending limbs with different epithelial types
Distal convoluted tubule (DCT): Cuboidal cells, fewer microvilli, mainly for secretion
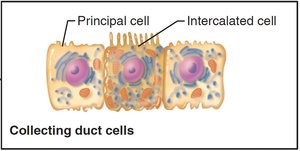
Collecting duct: Principal cells (water/Na+ balance) and intercalated cells (acid-base balance)
Types of Nephrons
Cortical nephrons: 85% of nephrons, mostly in cortex, short loops
Juxtamedullary nephrons: Long loops extend deep into medulla, essential for concentrating urine
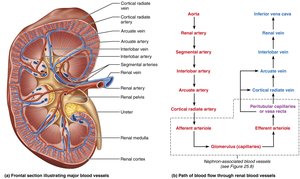
Nephron Capillary Beds
Glomerulus: Specialized for filtration; fed and drained by arterioles
Peritubular capillaries: Surround tubules in cortex; reabsorb water and solutes
Vasa recta: Long, straight vessels in medulla; maintain concentration gradient
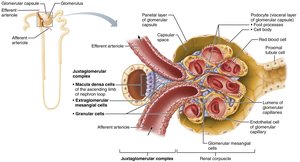
Juxtaglomerular Complex (JGC)
The JGC is a specialized structure important for regulating filtrate formation and blood pressure. It includes:
Macula densa: Chemoreceptors in the distal nephron loop, sense NaCl content
Granular (JG) cells: Mechanoreceptors in arteriole walls, secrete renin
Extraglomerular mesangial cells: Pass signals between macula densa and granular cells
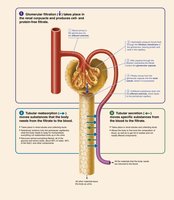
Urine Formation
Three Major Processes
Glomerular filtration: Passive process; blood pressure forces water and solutes through the filtration membrane into the glomerular capsule
Tubular reabsorption: Selective movement of substances from filtrate back into blood
Tubular secretion: Selective movement of substances from blood into filtrate
Glomerular Filtration
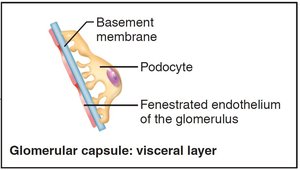
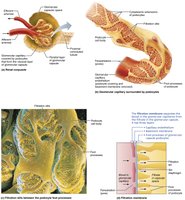
Filtration occurs across a three-layered membrane:
Fenestrated endothelium: Excludes blood cells
Basement membrane: Repels large anions and proteins
Foot processes of podocytes: Form filtration slits, restrict large proteins
Filtration Pressures
Filtration is driven by hydrostatic pressure in the glomerular capillaries (HPGC), opposed by hydrostatic pressure in the capsule (HPCS) and colloid osmotic pressure (OPGC):
HPGC: 55 mm Hg (outward)
HPCS: 15 mm Hg (inward)
OPGC: 30 mm Hg (inward)
Net Filtration Pressure (NFP):
Glomerular Filtration Rate (GFR)
GFR is the volume of filtrate formed per minute by both kidneys. It is directly proportional to:
Net filtration pressure (NFP)
Total surface area available for filtration
Filtration membrane permeability
Regulation of GFR
Intrinsic controls (renal autoregulation):
Myogenic mechanism: Smooth muscle response to pressure changes
Tubuloglomerular feedback: Macula densa senses NaCl, adjusts arteriole diameter
Extrinsic controls: Neural (sympathetic) and hormonal (renin-angiotensin-aldosterone) mechanisms regulate GFR to maintain blood pressure
Tubular Reabsorption and Secretion
Reabsorption
Most filtrate is reabsorbed into the blood via active (ATP-dependent) and passive (diffusion, osmosis) processes. Reabsorption can occur through transcellular or paracellular routes.
Proximal convoluted tubule: Major site for reabsorption of water, ions, and nutrients
Nephron loop: Descending limb reabsorbs water; ascending limb reabsorbs Na+, Cl−
Distal convoluted tubule and collecting duct: Fine-tune reabsorption under hormonal control (e.g., aldosterone, ADH)
Secretion
Tubular secretion removes additional wastes and regulates blood pH by moving substances from blood into the filtrate.
Summary Table: Nephron Types
Feature | Cortical Nephrons | Juxtamedullary Nephrons |
|---|---|---|
Location | Mostly in cortex | Close to cortex-medulla junction |
Nephron loop length | Short | Long, deep into medulla |
Function | General filtration | Concentrated urine formation |
Key Terms and Concepts
Filtrate: Plasma-derived fluid filtered by the glomerulus
Renin: Enzyme that initiates the renin-angiotensin-aldosterone system (RAAS) to regulate blood pressure
Podocyte: Specialized cell in the visceral layer of the glomerular capsule
Macula densa: Senses NaCl concentration in the distal nephron
Principal cell: Regulates water and sodium balance in the collecting duct
Intercalated cell: Regulates acid-base balance in the collecting duct
