 Back
BackThe Urinary System: Structure and Function
Study Guide - Smart Notes

The Urinary System
Overview and Functions
The urinary system is essential for maintaining homeostasis by eliminating metabolic wastes, regulating salt and water balance, and controlling blood volume and pH. It consists of several organs that work together to filter blood, form urine, and excrete it from the body.
Elimination of metabolic toxins and wastes: Removes substances such as urea, creatinine, and uric acid.
Regulation of salt and water balance: Maintains osmotic equilibrium and blood pressure.
Maintenance of blood volume and pH: Adjusts water reabsorption and secretes hydrogen ions to regulate acid-base balance.
Organs of the Urinary System
The urinary system is composed of four main organs:
Kidneys: Major excretory organs responsible for urine formation.
Ureters: Tubes that transport urine from the kidneys to the urinary bladder.
Urinary bladder: Temporary storage reservoir for urine.
Urethra: Conducts urine from the bladder out of the body.
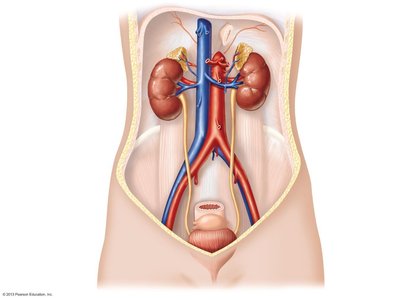
Anatomy of the Kidney
External and Internal Structure
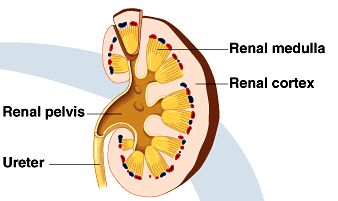
The kidneys are bean-shaped organs located on either side of the vertebral column. Each kidney is connected to a ureter, which conducts urine to the bladder. Internally, the kidney is divided into three main regions:
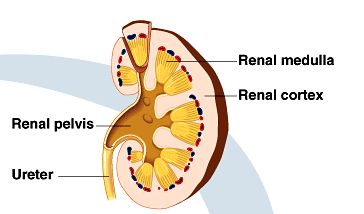
Renal cortex: The thin, outer region.
Renal medulla: The inner region, composed of pyramid-shaped structures.
Renal pelvis: The innermost hollow chamber that collects urine before it enters the ureter.
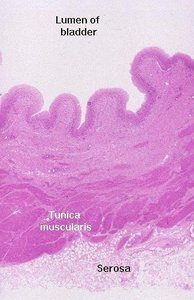
Histology of the Urinary Bladder and Ureter
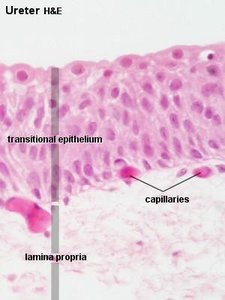
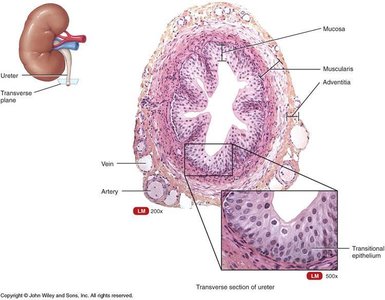
The urinary bladder and ureter are lined with transitional epithelium, which allows them to stretch as they fill with urine. The bladder wall consists of several layers, including the tunica muscularis and serosa.
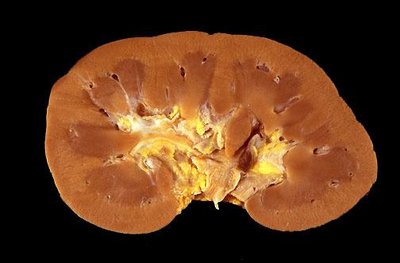
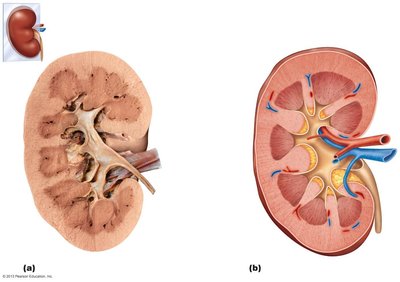
Internal Anatomy of the Kidney
Regions and Structures
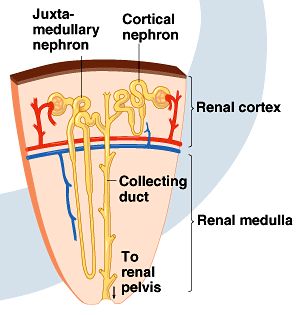
Each kidney contains about one million nephrons, which are the structural and functional units responsible for urine formation. Nephrons are distributed in both the cortex and medulla.
Renal cortex: Contains cortical nephrons.
Renal medulla: Contains juxtamedullary nephrons and renal pyramids.
Renal pelvis: Collects urine from nephrons.
Nephrons: Structure and Function
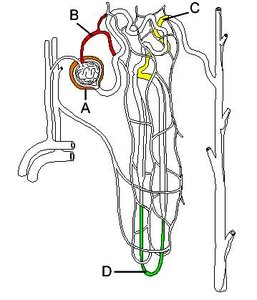
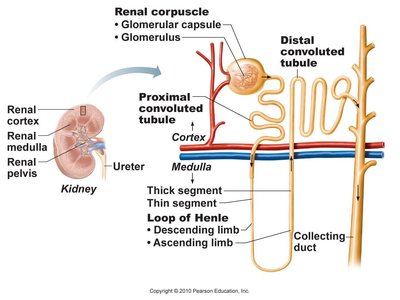
Parts of the Nephron
Nephrons are the basic units that filter blood and form urine. Each nephron consists of two main parts:
Renal corpuscle: Includes the glomerulus and Bowman's capsule.
Renal tubule: Includes the proximal convoluted tubule, loop of Henle, distal convoluted tubule, and collecting duct.
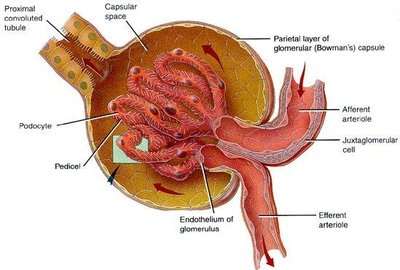
Renal Corpuscle
The renal corpuscle is the site of blood filtration and consists of:
Glomerulus: A network of fenestrated capillaries that allow filtrate formation.
Glomerular (Bowman's) capsule: Surrounds the glomerulus and collects the filtrate.
Parietal layer: Simple squamous epithelium.
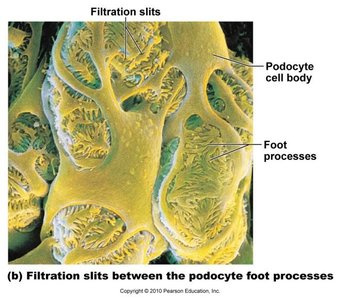
Visceral layer: Composed of podocytes with foot processes and filtration slits.
Urine Formation
Three Major Processes
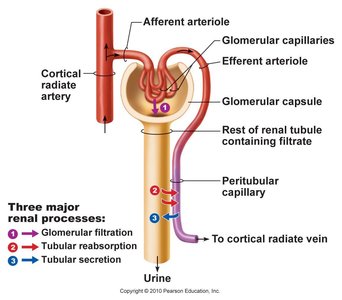
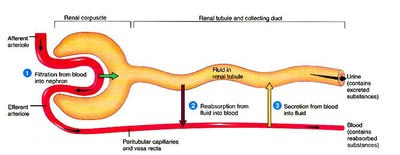
Urine production involves three distinct processes:
Glomerular filtration: Occurs at the glomerular capsule, where blood is filtered to form glomerular filtrate. Plasma proteins and blood cells are too large to pass through.
Tubular reabsorption: Solutes and water are reabsorbed from the nephron back into the blood, primarily at the proximal convoluted tubule. Sodium ions are actively reabsorbed, and water follows passively.
Tubular secretion: Substances are actively transported from the blood into the nephron, including H+, K+, NH4+, creatinine, and drugs. This process helps regulate blood pH and remove toxins.
Role of Antidiuretic Hormone (ADH)
ADH acts on the collecting ducts to increase their permeability to water, promoting water reabsorption and reducing urine volume. When ADH is released, more water is retained; when it is not released, more water is excreted.
Dehydration: ADH is released, increasing water reabsorption.
Hydration: ADH is not released, resulting in more urine formation.
Chemical Composition of Urine
Normal and Abnormal Constituents
Urine is composed of 95% water and 5% solutes. It is slightly acidic, with a pH around 6 (range 4.5–8.0). The main solutes include:
Nitrogenous wastes: Urea, uric acid, and creatinine.
Electrolytes: Na+, K+, PO43–, SO42–, Ca2+, Mg2+, HCO3–.
Abnormally high concentrations of any constituent may indicate pathology.
Functions of the Kidney
Summary of Kidney Functions
Formation of plasma filtrate: Initial step in urine production.
Reabsorption of useful molecules: Prevents loss of essential substances.
Secretion of excess electrolytes and wastes: Maintains electrolyte balance and removes toxins.
Regulation of water balance: Concentrates or dilutes urine as needed.
Endocrine function: Releases erythropoietin to stimulate red blood cell production.
Summary Table: Processes of Urine Formation
Process | Location | Main Function |
|---|---|---|
Glomerular Filtration | Glomerular capsule | Filters blood plasma |
Tubular Reabsorption | Proximal convoluted tubule | Reabsorbs water and solutes |
Tubular Secretion | Distal convoluted tubule | Secretes waste and regulates pH |
Key Equations
Glomerular Filtration Rate (GFR):
Where:
= Filtration coefficient
= Glomerular capillary hydrostatic pressure
= Bowman's space hydrostatic pressure
= Glomerular capillary oncotic pressure
Renal Clearance:
Where:
= Concentration of substance x in urine
= Urine flow rate
= Concentration of substance x in plasma
Additional info: The notes have been expanded to include definitions, examples, and key equations for academic completeness.
