 Back
BackThe Urinary System: Structure, Function, and Regulation
Study Guide - Smart Notes

The Urinary System
Overview and Functions
The urinary system is essential for maintaining homeostasis by removing metabolic wastes, regulating blood pressure, and balancing solute concentrations. It consists of the kidneys, ureters, urinary bladder, and urethra.
Excretion: Removal of metabolic wastes from the blood.
Elimination: Discharge of wastes from the body, coordinated by the bladder.
Homeostatic Regulation: Regulation of blood pressure, blood volume, and solute concentration.
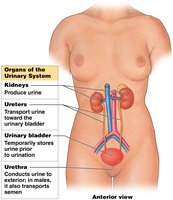
Organs of the Urinary System
Kidneys
The kidneys are retroperitoneal organs responsible for filtering blood and producing urine. They receive more than 20% of the body's blood volume at any time. The hilum is the entry and exit site for renal arteries, veins, and the ureter.
Location: Posterior abdominal wall, protected by the lower ribs.
Major Blood Vessels: Renal artery (in), renal vein (out).
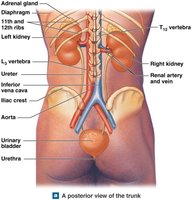
Ureters, Bladder, and Urethra
Urine produced by the kidneys is transported by the ureters to the urinary bladder, where it is temporarily stored before being expelled through the urethra.
Homeostatic Functions of the Kidneys
Regulation of Blood Volume and Blood Pressure
The kidneys regulate blood volume and pressure by adjusting the amount of water excreted in urine and by releasing hormones such as erythropoietin (EPO) and renin.
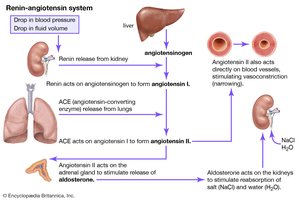
Renin: Initiates the renin-angiotensin-aldosterone system (RAAS) to increase blood pressure.
EPO: Stimulates red blood cell production in response to low oxygen.
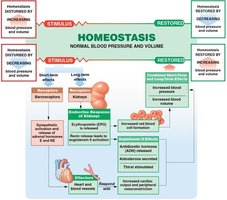
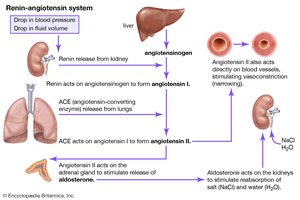
Regulation of Plasma Ion Concentrations
The kidneys control the excretion or reabsorption of ions such as sodium (Na+), potassium (K+), and chloride (Cl-) to maintain electrolyte balance.
Regulation of Calcium Ion Levels
Calcium ion levels are regulated through the synthesis of calcitriol, the active form of vitamin D, which increases calcium absorption in the digestive tract.
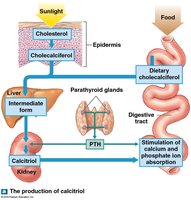
Stabilization of Blood pH
The kidneys help stabilize blood pH by controlling the excretion of hydrogen ions (H+) and bicarbonate (HCO3-).
Conservation of Nutrients
Essential nutrients such as glucose and amino acids are reabsorbed from the filtrate back into the blood, preventing their loss in urine.
Detoxification Assistance
The kidneys assist the liver in detoxifying substances such as ammonia and bilirubin, converting them into less toxic forms for excretion.
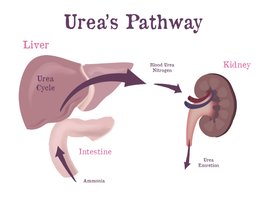
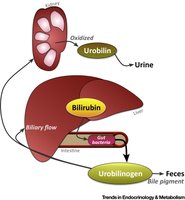
Anatomy of the Kidney
Internal Structure
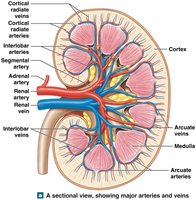
The kidney is divided into the renal cortex, renal medulla, and renal pelvis. Urine is produced in the renal lobes and funneled to the renal pelvis before passing into the ureter.
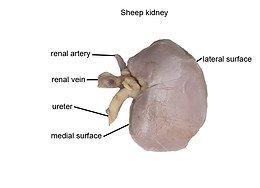
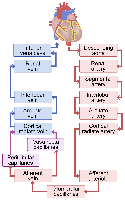
Blood Flow Through the Kidneys
Blood enters the kidney via the renal artery, passes through a series of smaller arteries and capillaries, and is filtered in the glomerulus before exiting through the renal vein.
The Nephron: Functional Unit of the Kidney
Types of Nephrons
Each kidney contains over one million nephrons, which are responsible for filtering blood and forming urine. There are two main types:
Cortical Nephrons: Located primarily in the cortex; involved in excretion and regulation.
Juxtamedullary Nephrons: Have long loops of Henle extending into the medulla; crucial for concentrating urine.
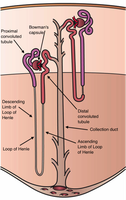
Nephron Anatomy
A nephron consists of a renal corpuscle (glomerulus and Bowman's capsule) and a renal tubule (proximal convoluted tubule, loop of Henle, distal convoluted tubule). The renal tubule empties into a collecting duct.
Urine Formation
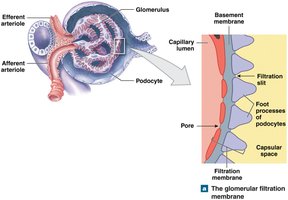
Filtration
Filtration occurs in the glomerulus, where blood pressure forces water and small solutes across the filtration membrane into Bowman's capsule. Large proteins and blood cells are retained in the blood.
Filtration Membrane: Consists of fenestrated endothelium, basement membrane, and podocytes.
Glomerular Filtration Rate (GFR): The amount of filtrate produced per minute, averaging 125 mL/min in adults.
Reabsorption
Most water, ions, and nutrients are reabsorbed from the filtrate back into the blood, primarily in the proximal convoluted tubule (PCT).
Secretion
Additional wastes and excess ions are secreted from the blood into the tubular fluid for excretion.
Hormonal Regulation
The distal convoluted tubule (DCT) is responsive to hormones such as aldosterone, atrial natriuretic peptide (ANP), brain natriuretic peptide (BNP), and parathyroid hormone (PTH), which regulate the reabsorption of sodium, potassium, and calcium.
Regulation of Glomerular Filtration Rate (GFR)
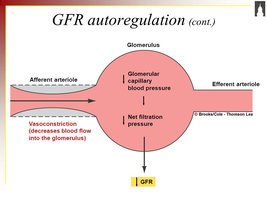
Autoregulation
The kidneys can locally regulate GFR by adjusting the diameter of afferent and efferent arterioles in response to changes in blood pressure.
Hormonal Regulation
The renin-angiotensin-aldosterone system (RAAS) increases blood pressure and GFR when blood volume is low. ANP and BNP decrease blood pressure and GFR when blood volume is high.
Autonomic Regulation
Sympathetic nervous system activity can decrease GFR by constricting afferent arterioles, reducing blood flow to the glomerulus, and stimulating renin release.
Summary Table: Key Hormones in Renal Regulation
Hormone | Source | Effect on Kidney | Overall Effect |
|---|---|---|---|
Renin | Juxtaglomerular cells | Activates RAAS, increases Na+ and water reabsorption | Increases blood pressure |
Aldosterone | Adrenal cortex | Increases Na+ reabsorption, K+ secretion | Increases blood volume and pressure |
ADH (Vasopressin) | Posterior pituitary | Increases water reabsorption in collecting ducts | Increases blood volume |
ANP/BNP | Heart (atria/ventricles) | Decreases Na+ and water reabsorption | Decreases blood volume and pressure |
Calcitriol | Kidney | Increases Ca2+ absorption in gut | Increases blood calcium |
Key Terms and Concepts
Glomerular Filtration Rate (GFR):
Renal Threshold: Plasma concentration at which a substance begins to appear in urine (e.g., glucose >180 mg/dL).
Osmotic Concentration: Number of solute particles per liter of solution.
Example: If plasma glucose exceeds the renal threshold, glucose will appear in the urine, a condition known as glucosuria.
Additional info: The kidneys play a vital role in long-term regulation of blood pressure, acid-base balance, and the removal of metabolic wastes, making them essential for overall homeostasis.
