 Back
BackThe Urinary System: Structure, Function, and Regulation
Study Guide - Smart Notes

Organs of the Urinary System
Overview of the Urinary System
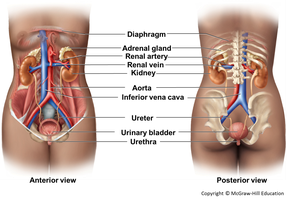
The urinary system is responsible for filtering blood, removing waste products, and maintaining fluid, electrolyte, and acid-base balance. It consists of paired kidneys, paired ureters, the urinary bladder, and the urethra.
Kidneys (2): Filter blood and produce urine.
Ureters (2): Transport urine from the kidneys to the bladder.
Urinary bladder: Stores urine until excretion.
Urethra: Conducts urine from the bladder to the outside of the body.
Functions of the Kidneys
Major Roles of the Kidneys
The kidneys perform several essential functions to maintain homeostasis:
Filtration of blood: Removal of metabolic wastes (e.g., urea, creatinine).
Regulation of water and electrolyte balance: Maintains osmolarity and volume of body fluids.
Acid-base balance: Regulates pH by excreting hydrogen ions and reabsorbing bicarbonate.
Hormone secretion: Produces renin (regulates blood pressure) and erythropoietin (stimulates red blood cell production).
Vitamin D metabolism: Converts vitamin D to its active form, calcitriol.
Gluconeogenesis: Generates glucose from non-carbohydrate sources during starvation.
Kidney Structure
Gross Anatomy of the Kidneys
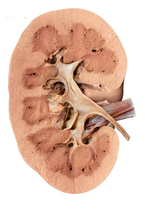
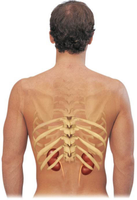
The kidneys are bean-shaped organs located lateral to the spine, extending from vertebra T12 to L3. Each kidney contains an outer cortex and an inner medulla, and houses over a million nephrons.
Cortex: Outer region, contains renal corpuscles and convoluted tubules.
Medulla: Inner region, contains nephron loops and collecting ducts.
Nephrons (Kidney Tubules)
Structure and Function of Nephrons
A nephron is the functional unit of the kidney, responsible for filtering blood and forming urine. Each nephron consists of two main parts: the renal corpuscle and the renal tubule.
Renal corpuscle: Site of blood filtration; includes the glomerulus (a tuft of capillaries) and the glomerular (Bowman's) capsule.
Renal tubule: Modifies the filtrate through reabsorption and secretion; consists of the proximal convoluted tubule (PCT), nephron loop (loop of Henle), distal convoluted tubule (DCT), and collecting duct.
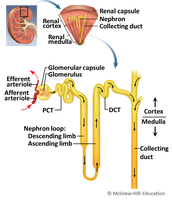
Classes of Nephrons
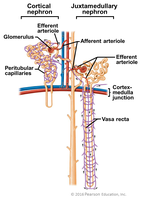
Cortical nephrons: ~85% of nephrons; located mostly in the cortex; surrounded by peritubular capillaries.
Juxtamedullary nephrons: ~15% of nephrons; long loops extend deep into the medulla; surrounded by vasa recta; crucial for concentrating urine.
Urine Formation
Three Main Processes
Urine formation involves three sequential processes:
Glomerular filtration: Blood is filtered in the renal corpuscle, producing a plasma-like filtrate.
Tubular reabsorption: Useful substances are reabsorbed from the filtrate back into the blood.
Tubular secretion: Additional wastes and ions are secreted into the filtrate for excretion.
The final product, urine, is composed of approximately 95% water and 5% solutes (mainly nitrogenous wastes such as urea, ammonia, uric acid, and creatinine).
Glomerular Filtration
Renal Corpuscle Structure
The renal corpuscle consists of the glomerulus (a specialized capillary bed) and the glomerular capsule. The glomerulus is a fenestrated capillary, allowing efficient filtration. The capsule has a parietal layer and a visceral layer composed of podocytes, which form filtration slits.
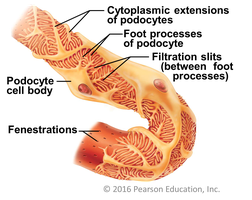
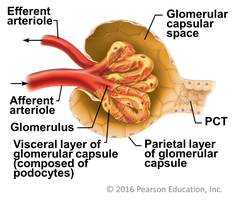
Filtration Membrane
The filtration membrane consists of three layers: the fenestrated endothelium of the glomerulus, the basement membrane, and the filtration slits formed by podocytes. This structure allows water and small solutes to pass while retaining blood cells and large proteins.
Pressures Affecting Filtration
The primary force driving filtration is the hydrostatic pressure in the glomerular capillaries. This pressure is higher than in other capillaries due to the large diameter of the afferent arteriole and the smaller diameter of the efferent arteriole.
Glomerular Filtration Rate (GFR)
GFR is the volume of filtrate formed per minute by both kidneys (normal adult value: 120–125 mL/min). GFR is tightly regulated by intrinsic (renal autoregulation) and extrinsic (neural and hormonal) mechanisms to maintain homeostasis and stable blood pressure.
Intrinsic controls: Myogenic mechanism and tubuloglomerular feedback (macula densa cells).
Extrinsic controls: Sympathetic nervous system and hormones (e.g., angiotensin II, ANP).
Tubular Reabsorption
Overview
Tubular reabsorption is essential for reclaiming water, ions, and nutrients from the filtrate. It begins in the proximal convoluted tubule (PCT) and continues along the nephron and collecting ducts. Both active and passive transport mechanisms are involved.
Sodium Reabsorption
Sodium is the most abundant cation in the filtrate. Its active reabsorption drives the reabsorption of water (osmosis), other solutes (via cotransport), and anions (via electrical gradients).
Proximal Convoluted Tubule (PCT)
The PCT is the major site of reabsorption, characterized by a large surface area (microvilli), many mitochondria, and numerous aquaporins for water transport.
Nephron Loop (Loop of Henle)
The nephron loop establishes a salt concentration gradient in the medulla, crucial for urine concentration. The descending limb is permeable to water but not solutes, while the ascending limb is permeable to solutes (especially NaCl) but not water. This countercurrent multiplier system allows the kidney to produce concentrated urine.
DCT and Collecting Ducts
Reabsorption in the distal convoluted tubule (DCT) and collecting ducts is regulated by hormones:
Antidiuretic hormone (ADH): Increases water reabsorption by inserting aquaporins in collecting duct cells.
Aldosterone: Increases sodium (and thus water) reabsorption in the DCT and collecting ducts.
Atrial natriuretic peptide (ANP): Decreases sodium and water reabsorption, promoting excretion.
Tubular Secretion
Importance of Tubular Secretion
Tubular secretion removes additional wastes (e.g., hydrogen ions, potassium, drugs) from the blood into the filtrate, helping to regulate acid-base balance and eliminate toxins.
Renal and Hormonal Regulation of Blood Pressure
Renin-Angiotensin-Aldosterone Mechanism
The kidneys regulate blood pressure by controlling blood volume. When blood pressure drops, the kidneys release renin, which initiates the renin-angiotensin-aldosterone system (RAAS):
Renin converts angiotensinogen to angiotensin I.
Angiotensin-converting enzyme (ACE) converts angiotensin I to angiotensin II.
Angiotensin II raises blood pressure by:
Vasoconstriction of arterioles
Stimulating aldosterone release (increases Na+ and water reabsorption)
Stimulating ADH release (increases water reabsorption)
Stimulating thirst
Blood volume is a major determinant of cardiac output and thus blood pressure.
Summary Table: Main Processes in the Nephron
Process | Main Site | Main Function |
|---|---|---|
Glomerular Filtration | Renal corpuscle | Filters blood plasma |
Tubular Reabsorption | PCT, nephron loop, DCT, collecting duct | Reclaims water, ions, nutrients |
Tubular Secretion | PCT, DCT, collecting duct | Removes wastes, regulates pH |
