 Back
BackThe Urinary System: Structure, Function, and Physiology
Study Guide - Smart Notes

The Urinary System: Structure and Function
Overview of the Urinary System
The urinary system is essential for maintaining the body's internal environment by regulating water, electrolyte, and acid-base balance, as well as removing metabolic wastes. It consists of the kidneys, ureters, urinary bladder, and urethra.
Kidneys: Major excretory organs responsible for filtering blood and forming urine.
Ureters: Transport urine from the kidneys to the urinary bladder.
Urinary bladder: Temporarily stores urine until excretion.
Urethra: Conducts urine from the bladder to the outside of the body.
Kidney Structure and Function
Internal Anatomy of the Kidney
The kidney is divided into the renal cortex and renal medulla. The medulla contains cone-shaped renal pyramids separated by renal columns. The tip of each pyramid, called the papilla, releases urine into minor calyces, which then drain into major calyces and finally the renal pelvis, leading to the ureter.
Renal cortex: Outer region containing most nephrons.
Renal medulla: Inner region with renal pyramids.
Renal pelvis: Funnel-shaped tube continuous with the ureter.
Blood and Nerve Supply
The kidneys receive about 25% of cardiac output each minute via the renal arteries. Blood is filtered and returned through a network of veins. Sympathetic nerve fibers regulate blood flow and kidney function.
Nephrons: The Functional Units
Structure of the Nephron
Nephrons are the structural and functional units of the kidney, responsible for urine formation. Each kidney contains over one million nephrons, each consisting of a renal corpuscle and a renal tubule.
Renal corpuscle: Includes the glomerulus (a tuft of capillaries) and the glomerular (Bowman's) capsule.
Renal tubule: Composed of the proximal convoluted tubule (PCT), nephron loop (loop of Henle), and distal convoluted tubule (DCT).
Renal Tubule Cell Types
The renal tubule is lined with specialized epithelial cells that facilitate reabsorption and secretion. The PCT contains cuboidal cells with dense microvilli and abundant mitochondria, supporting active transport processes.
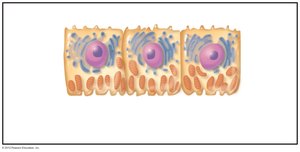
Collecting Ducts
Collecting ducts receive filtrate from multiple nephrons and play a key role in water and electrolyte balance. They contain two main cell types:
Principal cells: Regulate water and sodium balance.
Intercalated cells (Type A and B): Regulate acid-base balance.
Classes of Nephrons
Cortical nephrons: 85% of nephrons, located mostly in the cortex.
Juxtamedullary nephrons: Long loops extend deep into the medulla, crucial for concentrating urine.
Nephron Capillary Beds
Each nephron is associated with two capillary beds:
Glomerulus: Specialized for filtration, with high blood pressure maintained by afferent and efferent arterioles.
Peritubular capillaries: Adapted for absorption, surrounding the renal tubule.
Vasa recta: Long, thin-walled vessels in juxtamedullary nephrons, important for urine concentration.
Juxtaglomerular Complex (JGC)
The JGC regulates filtrate formation and blood pressure. It consists of macula densa cells (chemoreceptors for NaCl), granular (JG) cells (mechanoreceptors that secrete renin), and extraglomerular mesangial cells (signal mediators).
Mechanisms of Urine Formation
Three Main Processes
Urine formation involves three key processes:
Glomerular filtration: Passive process where hydrostatic pressure forces plasma (minus proteins) into the glomerular capsule.
Tubular reabsorption: Selective return of 99% of filtrate components to the blood.
Tubular secretion: Selective movement of substances from blood into the filtrate for excretion.
Filtration Membrane
The filtration membrane consists of three layers: fenestrated endothelium, basement membrane, and podocyte foot processes. It allows passage of water and small solutes but blocks proteins and cells.
Pressures Affecting Filtration
Hydrostatic pressure in glomerular capillaries (HPgc): Main force driving filtration (~55 mm Hg).
Hydrostatic pressure in capsular space (HPcs): Opposes filtration (15 mm Hg).
Colloid osmotic pressure in capillaries (OPgc): Opposes filtration (30 mm Hg).
Net filtration pressure (NFP):
Typical values:
Glomerular Filtration Rate (GFR)
GFR is the volume of filtrate formed per minute by both kidneys (normal: 120–125 ml/min). It is directly proportional to NFP, filtration surface area, and membrane permeability.
Regulation of Glomerular Filtration
Intrinsic controls (renal autoregulation): Myogenic mechanism and tubuloglomerular feedback maintain GFR within MAP 80–180 mm Hg.
Extrinsic controls: Sympathetic nervous system and renin-angiotensin-aldosterone system regulate GFR during extreme conditions (e.g., low blood pressure).
Tubular Reabsorption and Secretion
Mechanisms of Reabsorption
Reabsorption occurs via transcellular (through cells) and paracellular (between cells) routes. Most nutrients, water, and ions are reabsorbed in the PCT. Transport maximum (Tm) limits reabsorption based on carrier availability.
Hormonal Regulation
Antidiuretic hormone (ADH): Increases water reabsorption in collecting ducts.
Aldosterone: Increases Na+ reabsorption and K+ secretion in DCT and collecting ducts.
Atrial natriuretic peptide (ANP): Reduces Na+ reabsorption, lowering blood volume and pressure.
Parathyroid hormone (PTH): Increases Ca2+ reabsorption in DCT.
Summary of Tubular Reabsorption and Secretion
The following diagram summarizes the main sites and substances involved in reabsorption and secretion along the nephron and collecting duct.
Tubular Secretion
Tubular secretion removes substances such as K+, H+, NH4+, creatinine, and drugs from the blood into the filtrate. It is essential for eliminating wastes, controlling blood pH, and removing excess ions.
Regulation of Urine Concentration and Volume
Osmolality and Countercurrent Mechanisms
Osmolality is the number of solute particles per liter of water. The kidneys maintain plasma osmolality at ~300 mOsm using countercurrent mechanisms:
Countercurrent multiplier: Nephron loop creates an osmotic gradient in the medulla.
Countercurrent exchanger: Vasa recta preserve the gradient and remove reabsorbed water.
Renal Clearance
Renal clearance is the volume of plasma cleared of a substance per minute. It is calculated as:
C: Renal clearance rate (ml/min)
U: Concentration of substance in urine (mg/ml)
V: Urine flow rate (ml/min)
P: Concentration of substance in plasma (mg/ml)
Inulin is used as a standard for measuring GFR.
Physical and Chemical Characteristics of Urine
Physical Characteristics
Color: Clear, pale to deep yellow (urochrome pigment).
Odor: Slightly aromatic when fresh; ammonia odor develops upon standing.
pH: Slightly acidic (pH ~6), but ranges from 4.5 to 8.0 depending on diet and health.
Specific gravity: 1.001 to 1.035, depending on solute concentration.
Chemical Composition
95% water, 5% solutes
Nitrogenous wastes: Urea, uric acid, creatinine
Other solutes: Na+, K+, PO43–, SO42–, Ca2+, Mg2+, HCO3–
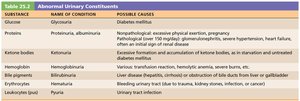
Abnormal Urinary Constituents
The presence of certain substances in urine can indicate pathology. The table below summarizes abnormal constituents, their associated conditions, and possible causes.
Substance | Name of Condition | Possible Causes |
|---|---|---|
Glucose | Glycosuria | Diabetes mellitus |
Proteins | Proteinuria, albuminuria | Nonpathological: excessive physical exertion, pregnancy Pathological: glomerulonephritis, severe hypertension, heart failure, renal disease |
Ketone bodies | Ketonuria | Starvation, untreated diabetes mellitus |
Hemoglobin | Hemoglobinuria | Transfusion reactions, hemolytic anemia, burns |
Bile pigments | Bilirubinuria | Liver disease, obstruction of bile ducts |
Erythrocytes (RBCs) | Hematuria | Trauma, kidney stones, infection, cancer |
Leukocytes (WBCs) | Pyuria | Urinary tract infection |
Urine Transport, Storage, and Elimination
Ureters
Ureters are muscular tubes that convey urine from the kidneys to the bladder. They are retroperitoneal and enter the bladder at an angle to prevent backflow. The wall consists of mucosa (transitional epithelium), muscularis (smooth muscle), and adventitia (fibrous connective tissue).
Urinary Bladder
The bladder is a muscular sac for temporary urine storage. It has a mucosal lining, a thick detrusor muscle, and an outer adventitia. The trigone region is prone to infection. The bladder can expand significantly without a large increase in internal pressure.
Urethra
The urethra is a muscular tube draining urine from the bladder. It has internal (involuntary) and external (voluntary) sphincters. The female urethra is short (3–4 cm), while the male urethra is longer (about 20 cm) and divided into prostatic, membranous, and spongy regions.
Micturition (Urination)
Control of Micturition
Micturition involves three simultaneous events:
Contraction of the detrusor muscle (ANS)
Opening of the internal urethral sphincter (ANS)
Opening of the external urethral sphincter (somatic nervous system)
Reflexive urination is present in infants, while voluntary control develops with maturation of pontine centers in the brain.
