 Back
BackThe Urinary System: Structure, Function, and Physiology
Study Guide - Smart Notes

The Urinary System
Overview and Functions
The urinary system is essential for maintaining the body's internal environment by regulating water, electrolyte, and acid-base balance, as well as removing metabolic wastes. It also performs several endocrine functions and is involved in gluconeogenesis during prolonged fasting.
Regulation of water and solute concentration: Maintains total water volume and solute concentration in the body.
Ion balance: Regulates extracellular fluid (ECF) ion concentrations.
Acid-base balance: Ensures long-term acid-base equilibrium.
Excretion: Removes metabolic wastes, toxins, and drugs.
Endocrine functions: Secretes renin (regulates blood pressure) and erythropoietin (stimulates red blood cell production).
Vitamin D activation: Converts vitamin D to its active form.
Gluconeogenesis: Generates glucose from non-carbohydrate sources during fasting.
Organs of the Urinary System
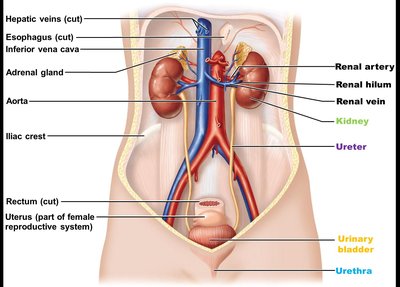
Kidneys: Major excretory organs that filter blood and form urine.
Ureters: Transport urine from kidneys to urinary bladder.
Urinary bladder: Temporary storage reservoir for urine.
Urethra: Transports urine out of the body.
Anatomy of the Kidneys
Location and External Structure
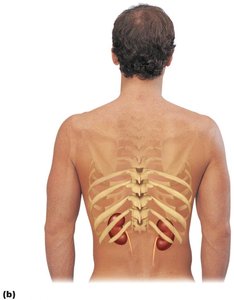
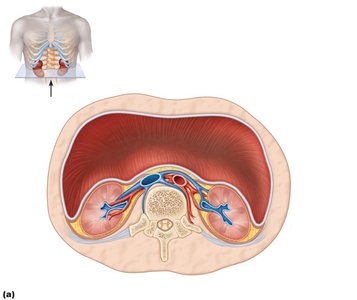
The kidneys are retroperitoneal organs located in the superior lumbar region, between T12 and L5 vertebrae. The right kidney is slightly lower than the left due to the position of the liver. Each kidney is capped by an adrenal gland.
Renal hilum: The medial indentation where ureters, blood vessels, lymphatics, and nerves enter and exit.
Supportive tissue layers:
Paranephric fat: Outermost layer between renal fascia and peritoneum.
Renal fascia: Dense fibrous connective tissue anchoring the kidney.
Perirenal fat capsule: Fatty cushion protecting the kidney.
Fibrous capsule: Prevents spread of infection to the kidney.
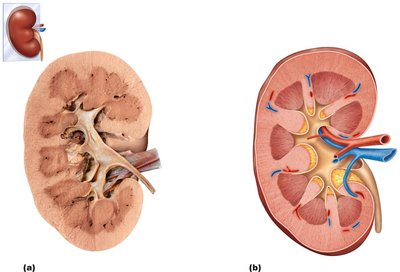
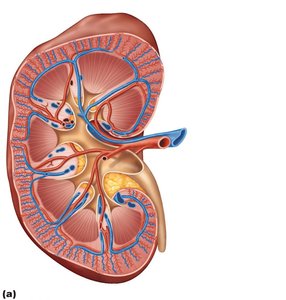
Internal Anatomy
Renal cortex: The outer, granular-appearing region.
Renal medulla: Composed of cone-shaped renal pyramids separated by renal columns (cortical tissue extensions).
Papilla: Tip of each pyramid, releasing urine into minor calyces.
Lobe: A pyramid and its surrounding cortex (~8 per kidney).
Renal pelvis: Funnel-shaped tube continuous with the ureter.
Minor calyces: Collect urine from papillae.
Major calyces: Collect urine from minor calyces and empty into the renal pelvis.
Urine flow: Renal pyramid → minor calyx → major calyx → renal pelvis → ureter
Blood and Nerve Supply
Renal arteries: Deliver about 25% of cardiac output to the kidneys each minute (~1200 ml/min).
Venous drainage: Follows a similar path as arteries.
Nerve supply: Sympathetic fibers from the renal plexus regulate blood flow and influence urine formation.
Nephrons: Structure and Function
Overview
Nephrons are the structural and functional units of the kidney, responsible for urine formation. Each kidney contains over one million nephrons.
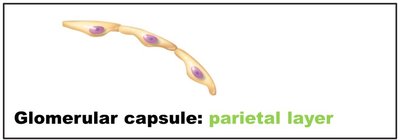
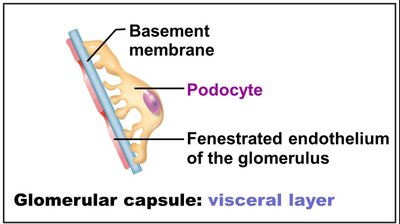
Renal corpuscle: Consists of the glomerulus (a tuft of capillaries) and the glomerular (Bowman's) capsule (surrounds the glomerulus).
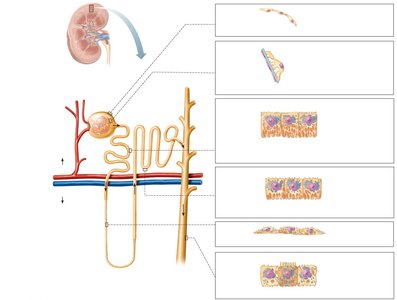
Renal tubule: Extends from the glomerular capsule and consists of three main parts:
Proximal convoluted tubule (PCT): Reabsorption and secretion; lined with cuboidal cells with microvilli.
Nephron loop (Loop of Henle): Descending and ascending limbs; different permeability to water and solutes.
Distal convoluted tubule (DCT): More involved in secretion than reabsorption; few microvilli.
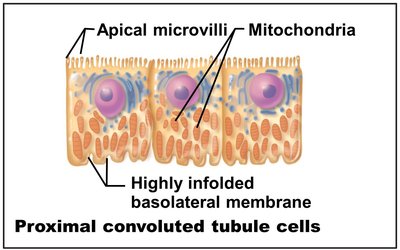
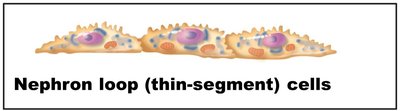
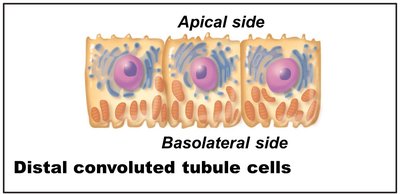
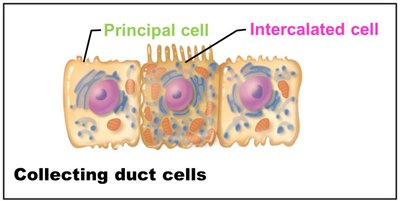
Collecting Ducts
Principal cells: Maintain water and sodium balance.
Intercalated cells (A and B): Regulate acid-base balance.
Collecting ducts receive filtrate from multiple nephrons and deliver urine to the minor calyces.
Classes of Nephrons
Cortical nephrons: 85% of nephrons; almost entirely in the cortex.
Juxtamedullary nephrons: Long nephron loops deeply invade the medulla; essential for producing concentrated urine.
Nephron Capillary Beds
Glomerulus: Specialized for filtration; fed and drained by arterioles (afferent and efferent).
Peritubular capillaries: Adapted for absorption; surround renal tubules in the cortex.
Vasa recta: Long, thin-walled vessels parallel to nephron loops of juxtamedullary nephrons; important for urine concentration.
Juxtaglomerular Complex (JGC)
The JGC is crucial for regulating filtrate formation and blood pressure. It consists of:
Macula densa: Chemoreceptors that sense NaCl content in filtrate.
Granular (JG) cells: Mechanoreceptors that sense blood pressure and secrete renin.
Extraglomerular mesangial cells: May relay signals between macula densa and granular cells.
Mechanisms of Urine Formation
Three Major Renal Processes
Glomerular filtration: Passive process producing cell- and protein-free filtrate.
Tubular reabsorption: Selective return of 99% of substances from filtrate to blood.
Tubular secretion: Selective movement of substances from blood to filtrate.
Glomerular Filtration
Filtration membrane: Three layers—fenestrated endothelium, basement membrane, and podocyte foot processes with filtration slits.
Permits passage: Water, glucose, amino acids, nitrogenous wastes; blocks cells and most proteins.
Net filtration pressure (NFP): Main force is hydrostatic pressure in glomerular capillaries (55 mm Hg out, 45 mm Hg in; NFP = 10 mm Hg).
Glomerular Filtration Rate (GFR)
Definition: Volume of filtrate formed per minute by both kidneys (normal: 120–125 ml/min).
Determinants: NFP, surface area, and membrane permeability.
Regulation of Glomerular Filtration
Intrinsic controls (renal autoregulation): Myogenic mechanism and tubuloglomerular feedback maintain GFR within 80–180 mm Hg MAP.
Extrinsic controls: Nervous and endocrine mechanisms (e.g., sympathetic nervous system, renin-angiotensin-aldosterone system) maintain systemic blood pressure.
Tubular Reabsorption and Secretion
Tubular Reabsorption
Selective process: All organic nutrients reabsorbed; water and ion reabsorption regulated by hormones.
Routes:
Transcellular: Through tubule cells.
Paracellular: Between tubule cells (leaky in PCT).
Reabsorption of Sodium and Other Substances
Sodium (Na+): Most abundant cation in filtrate; reabsorbed by active transport (Na+-K+ ATPase) and secondary active transport.
Water: Follows solutes by osmosis via aquaporins (obligatory in PCT, facultative in collecting ducts with ADH).
Other nutrients: Glucose, amino acids, and vitamins cotransported with Na+.
Transport Maximum (Tm)
Each substance has a Tm, reflecting the number of carriers available. Excess is excreted in urine (e.g., glucose in diabetes).
Reabsorptive Capabilities by Segment
PCT: Site of most reabsorption (all nutrients, 65% Na+ and water, many ions).
Nephron loop: Descending limb—water reabsorption; ascending limb—solute reabsorption.
DCT and collecting duct: Hormonally regulated reabsorption (ADH for water, aldosterone for Na+, ANP for Na+, PTH for Ca2+).
Tubular Secretion
Reverse of reabsorption; disposes of drugs, excess K+, H+, NH4+, and controls blood pH.
Regulation of Urine Concentration and Volume
Osmolality and Countercurrent Mechanism
Osmolality: Number of solute particles per kg of water; kidneys maintain plasma osmolality (~300 mOsm).
Countercurrent multiplier: Nephron loop establishes medullary osmotic gradient (300–1200 mOsm).
Countercurrent exchanger: Vasa recta preserves the gradient.
Collecting ducts: Use the gradient to adjust urine osmolality under ADH control.
Formation of Dilute or Concentrated Urine
Overhydration: Low ADH, large volume of dilute urine (~100 mOsm).
Dehydration: High ADH, small volume of concentrated urine (~1200 mOsm).
Urea recycling: Contributes to medullary osmotic gradient.
Diuretics
Increase urinary output by inhibiting ADH, Na+ reabsorption, or medullary gradient formation.
Renal Clearance
Definition: Volume of plasma cleared of a substance per minute.
Equation: Where:
C = renal clearance rate (ml/min)
U = concentration in urine (mg/ml)
V = urine flow rate (ml/min)
P = concentration in plasma (mg/ml)
Inulin: Standard for measuring GFR (125 ml/min).
Physical and Chemical Characteristics of Urine
Color: Clear, pale to deep yellow (urochrome pigment); abnormal colors may indicate pathology.
Odor: Slightly aromatic; ammonia odor develops upon standing.
pH: Slightly acidic (~6), but ranges from 4.5 to 8.0 depending on diet and health.
Specific gravity: 1.001–1.035, depending on solute concentration.
Chemical composition: 95% water, 5% solutes (urea, uric acid, creatinine, ions). Abnormal components (proteins, WBCs, bile pigments) may indicate disease.
Developmental Aspects and Homeostatic Imbalances
Embryonic development: Three sets of kidneys form in succession (pronephros, mesonephros, metanephros).
Congenital abnormalities: Horseshoe kidney, hypospadias, polycystic kidney disease.
Age-related changes: Kidneys shrink, nephrons decrease, GFR declines, bladder tone decreases.
Common disorders: Pyelonephritis, renal calculi, incontinence, urinary retention, chronic renal disease, renal failure.
