 Back
BackThe Urinary System: Structure, Function, and Physiology
Study Guide - Smart Notes

The Urinary System
Overview and Functions
The urinary system is essential for maintaining homeostasis by regulating the volume and composition of blood. It plays a critical role in pH balance, waste removal, and fluid regulation. The system consists of two kidneys, two ureters, one bladder, and one urethra.
Homeostasis: Maintains blood pH through buffer systems and breathing.
Blood Buffer: Rapidly binds hydrogen ions to maintain pH.
Major Organs: Kidneys, ureters, bladder, urethra.
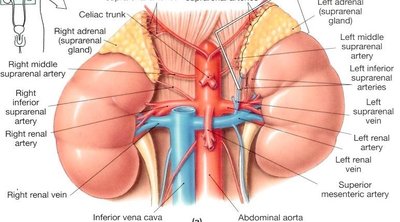
Kidneys
Gross Anatomy and Location
The kidneys are bean-shaped organs, approximately 4 inches long and 2-3 inches wide, located retroperitoneally in the posterior/superior abdominal cavity. They are partially protected by the 11th and 12th ribs, with the right kidney slightly lower than the left due to the liver's position.
Retroperitoneal: Positioned against the abdominal wall, minimizing movement and preventing ureter kinking.
Homeostasis: Regulate blood composition within minutes to hours by excreting bicarbonate (HCO3-) and hydrogen ions (H+).
Protective Layers of the Kidney
Renal Fascia: Outermost thin fibrous connective tissue anchoring the kidney.
Adipose Capsule: Middle fatty layer providing protection and insulation.
Renal Capsule: Innermost transparent, thick fibrous membrane.
The layers from superficial to deep: Peritoneal layer → Adipose (fat) layer → Renal capsule.
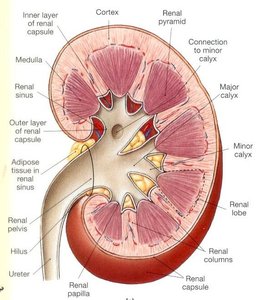
Internal Gross Anatomy
The kidney's internal structure includes the cortex, medulla, renal pyramids, minor and major calyces, and the renal pelvis, which narrows into the ureter.
Medulla: Inner region containing renal pyramids.
Renal Pelvis: Funnel-shaped structure leading to the ureter.
Calyces: Minor calyces join to form major calyces, collecting urine from pyramids.
Microscopic Anatomy of the Kidney
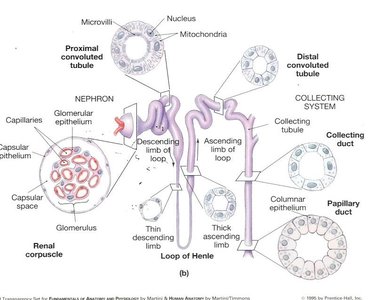
The Nephron: Structure and Function
The nephron is the functional filtration unit of the kidney, with approximately one million per kidney. Each nephron consists of a renal tubule and its associated blood vessels.
Filtration: Blood is filtered through the glomerulus into the Bowman’s capsule, forming filtrate.
Filtrate Volume: About 50 gallons of filtrate are produced daily, but most is reabsorbed; only ~1500 mL is excreted as urine.
Reabsorption: Most fluid and solutes are returned to the body.
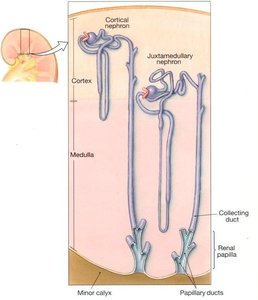
Types of Nephrons
Cortical Nephrons: Located in the cortex, have shorter loops of Henle, and are responsible for most urine production but less concentration.
Juxtamedullary Nephrons: Located at the cortex-medulla junction, have longer loops of Henle, and are specialized for producing highly concentrated urine. Their blood supply is the vasa recta.
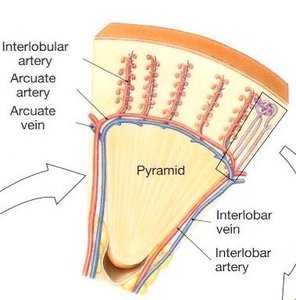
Blood Supply to the Kidneys
Approximately 1200 mL of blood flows through the kidneys each minute. The renal artery branches into segmental, interlobar, arcuate, and interlobular arteries, eventually leading to the afferent arteriole and glomerulus. Blood exits via the efferent arteriole, venules, and corresponding veins.
Vasa Recta: Specialized capillaries associated with juxtamedullary nephrons, crucial for urine concentration.
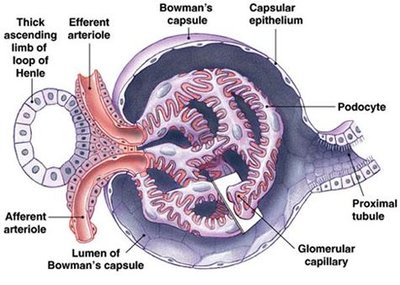
Bowman’s Capsule and Glomerulus
The Bowman’s capsule surrounds the glomerulus and is the initial site of filtration. Podocytes with pedicles (foot-like projections) form filtration slits, allowing selective passage of water and solutes.
Glomerulus: Capillary bed, one cell layer thick, surrounded by podocytes.
Podocytes: Specialized cells with interdigitating pedicles forming filtration slits.
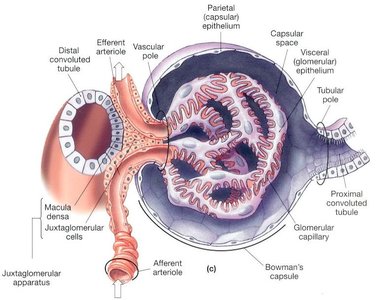
Juxtaglomerular Apparatus
This apparatus is formed where the distal convoluted tubule (DCT) contacts the afferent arteriole. It consists of juxtaglomerular cells and the macula densa, which regulate blood pressure and filtration rate.
Juxtaglomerular Cells: Located between afferent and efferent arterioles; secrete renin.
Macula Densa: DCT cells that sense sodium concentration and signal JG cells.
Hormonal Regulation
Renin: Increases blood pressure by activating the renin-angiotensin-aldosterone system (RAAS).
Erythropoietin (EPO): Stimulates red blood cell production in response to low oxygen.
Urine Formation
Step 1: Glomerular Filtration
Filtration occurs as blood pressure forces plasma components through the glomerular membrane into the Bowman’s capsule, forming filtrate. The afferent arteriole is wider than the efferent, creating a pressure gradient.
Opposing Forces: Capsular hydrostatic pressure and blood osmotic pressure resist filtration.
GFR (Glomerular Filtration Rate): Amount of filtrate formed per unit time (~50 gallons/day, only ~1500 mL excreted).
Step 2: Tubular Reabsorption
Most filtrate is reabsorbed from the tubules back into the blood, primarily in the proximal convoluted tubule (PCT).
PCT: Reabsorbs 60-70% of filtrate volume, nearly all glucose and amino acids, and significant amounts of ions (Na+, K+, Mg2+, HCO3-).
Microvilli: Increase surface area for absorption.

Step 3: Tubular Secretion
Active transport of harmful substances from blood into the tubule, bypassing the Bowman’s capsule, for excretion in urine.
Loop of Henle and Countercurrent Mechanism
The loop of Henle establishes a concentration gradient in the medulla, allowing the kidney to concentrate urine.
Descending Limb: Permeable to water, impermeable to solutes; water exits into the medulla.
Ascending Limb: Impermeable to water, actively transports NaCl out; decreases filtrate osmolarity.
Countercurrent Multiplier: The close proximity of ascending and descending limbs amplifies the osmotic gradient, facilitating water reabsorption.
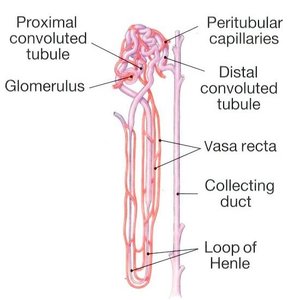
Vasa Recta
The vasa recta are capillaries that run parallel to the loop of Henle, maintaining the medullary osmotic gradient and returning reabsorbed water and solutes to the bloodstream.
Hormonal Control of Urine Concentration
ADH (Antidiuretic Hormone): Increases collecting duct permeability to water, concentrating urine. Low ADH (as in diabetes insipidus) leads to dilute urine.
Aldosterone: Increases Na+ reabsorption and K+ secretion in the DCT and collecting duct; water follows Na+, reducing urine volume.
Urinary Bladder and Urethra
Urinary Bladder Structure
The bladder is a hollow, muscular organ located posterior to the symphysis pubis. It stores urine until micturition (urination).
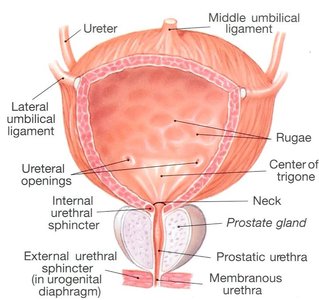
Ureter Openings: Smooth area where ureters enter.
Rugae: Folds in the mucosa allowing expansion.
Trigone: Triangular area with no rugae, acts as a funnel for urine outflow.
Internal Sphincter: Involuntary, controlled by the autonomic nervous system.
External Sphincter: Voluntary, controlled by skeletal muscle.
Bladder Wall Layers
Layer | Description |
|---|---|
Mucosa | Innermost, transitional epithelium, stretches as bladder fills |
Submucosa | Dense connective tissue, binds mucosa to muscle |
Detrusor Muscle | Three layers (longitudinal, circular, longitudinal); contracts during urination |
Serosa | Outermost, peritoneal covering |
Micturition Reflex
As the bladder fills (200-400 mL), stretch receptors send signals to the sacral spinal cord (S2-S4), triggering detrusor muscle contraction and internal sphincter relaxation. Voluntary control of urination is maintained by the external sphincter.
Urethra
Females: ~1.5 inches long, three layers (mucosa, spongy layer, smooth muscle); shorter length increases risk of infection.
Males: ~8 inches long, two layers (mucosa, submucosa); lacks smooth muscle, making voluntary interruption of urination more difficult.
