 Back
BackThe Urinary System: Structure, Function, and Physiology
Study Guide - Smart Notes

The Urinary System
Overview of Urinary System Structures
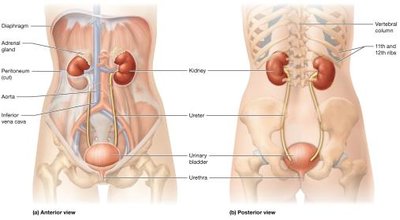
The urinary system is essential for filtering blood, removing waste, and maintaining homeostasis. It consists of the paired kidneys and the urinary tract (ureters, urinary bladder, and urethra).
Kidneys: Retroperitoneal organs located against the posterior abdominal wall. The left kidney extends from T12 to L3, while the right sits lower due to the liver. Both are partially protected by the 11th and 12th ribs and are capped by adrenal glands.
Urinary Tract: Includes paired ureters (transport urine from kidneys to bladder), the urinary bladder (stores urine), and the urethra (expels urine from the body).
Functions of the Kidneys
Removal of Metabolic Wastes: Kidneys filter waste products from the blood.
Fluid and Electrolyte Balance: Regulate osmolarity by conserving or eliminating water and electrolytes (Na+, K+, Ca2+).
Acid-Base Balance: Maintain blood pH by controlling H+ and HCO3- levels.
Blood Pressure Regulation: Influence systemic blood pressure via blood volume control and secretion of renin.
Regulation of Erythropoiesis: Release erythropoietin to stimulate red blood cell production.
Other Metabolic Functions: Detoxification, vitamin D activation, and gluconeogenesis.
Kidney Anatomy
External Anatomy of the Kidneys
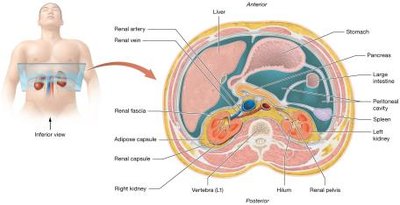
Each kidney is about 11 cm long, 6 cm wide, and 3 cm thick, weighing around 150 grams. They are protected by three connective tissue layers:
Renal Fascia: Anchors the kidney to surrounding structures.
Adipose Capsule: Cushions and protects the kidney; loss can cause nephroptosis (kidney droop).
Renal Capsule: Thin, protective outer layer.
Hilum: Medial opening for vessels, nerves, and ureter.
Renal Sinus: Central cavity containing urine-draining structures and adipose tissue.
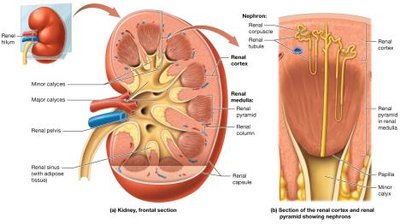
Internal Anatomy of the Kidneys
Renal Cortex: Outer region, rich in blood vessels.
Renal Medulla: Contains renal pyramids separated by renal columns.
Renal Pelvis: Central collecting region for urine.
Nephrons: Over one million per kidney; functional units that filter blood and produce urine.
Urine Flow: Papilla → Minor Calyx → Major Calyx → Renal Pelvis
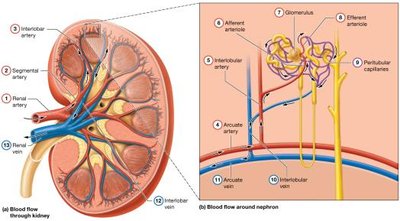
Blood Supply of the Kidneys
The kidneys receive about 25% of cardiac output (~1,200 ml/min). Blood flows through a series of arteries and capillaries:
Renal artery → Segmental artery → Interlobar artery → Arcuate artery → Interlobular (cortical radiate) artery → Afferent arteriole → Glomerulus → Efferent arteriole → Peritubular capillaries → Interlobular vein → Arcuate vein → Interlobar vein → Renal vein
Microanatomy: The Nephron and Collecting System
Nephron Structure
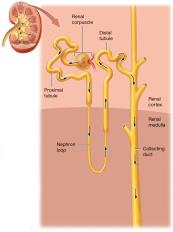
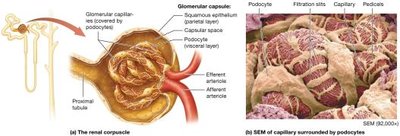
Renal Corpuscle: Includes the glomerulus (capillary tuft with fenestrations) and Bowman's capsule (parietal and visceral layers with podocytes forming filtration slits).
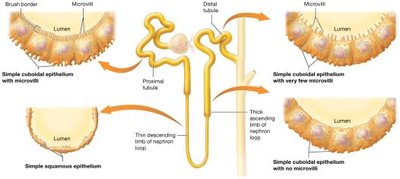
Renal Tubule: Proximal tubule (with brush border), nephron loop (descending and ascending limbs), and distal tubule.
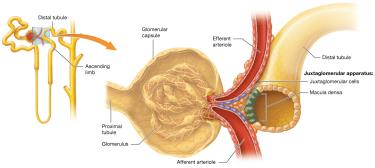
Juxtaglomerular Apparatus (JGA)
The JGA includes macula densa cells of the distal tubule and juxtaglomerular (JG) cells of the afferent/efferent arterioles. It regulates blood pressure and glomerular filtration rate (GFR).
The Collecting System
Distal tubule empties into the cortical collecting duct, which becomes the medullary collecting duct, then the papillary duct. At the end, filtrate is now urine.
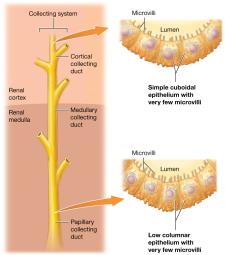
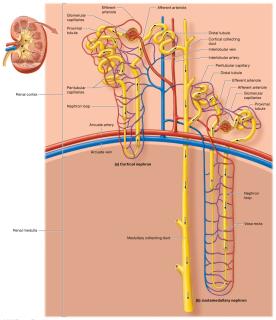
Types of Nephrons
Cortical Nephrons: 80% of nephrons, mostly in cortex, short loops.
Juxtamedullary Nephrons: Long loops extend into medulla, surrounded by vasa recta; crucial for urine concentration.
Renal Physiology
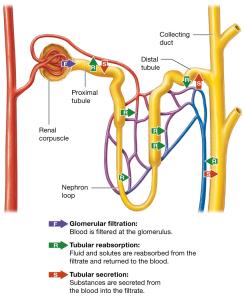
Three Basic Processes
Glomerular Filtration: Blood pressure forces plasma (minus cells/proteins) into the capsular space, forming filtrate.
Tubular Reabsorption: Water, glucose, amino acids, and ions are reclaimed from filtrate back into the blood, mainly in the proximal tubule and nephron loop.
Tubular Secretion: Additional substances (e.g., H+, drugs) are secreted from blood into filtrate for excretion.
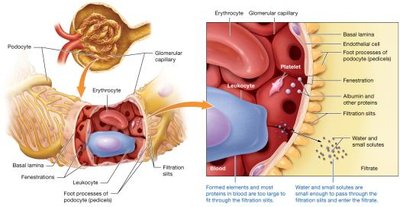
The Filtration Membrane
Composed of fenestrated glomerular capillary endothelial cells, a basal lamina, and podocytes (visceral layer of Bowman's capsule).
Allows passage of water, small solutes, and wastes; blocks cells and most proteins.
Glomerular Filtration Rate (GFR) and Net Filtration Pressure (NFP)
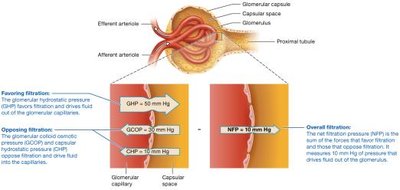
GFR ≈ 125 ml/min (180 L/day); NFP is determined by:
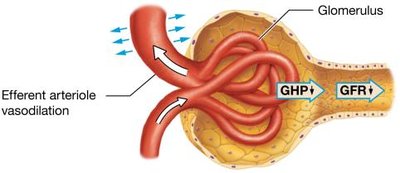
Glomerular Hydrostatic Pressure (GHP): ~50 mm Hg, favors filtration.
Glomerular Colloid Osmotic Pressure (GCOP): ~30 mm Hg, opposes filtration.
Capsular Hydrostatic Pressure (CHP): ~10 mm Hg, opposes filtration.
Net Filtration Pressure: mm Hg
Regulation of GFR
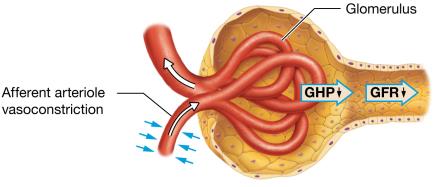
Autoregulation: Myogenic mechanism and tubuloglomerular feedback keep GFR constant over a range of blood pressures.
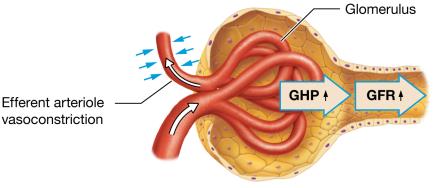
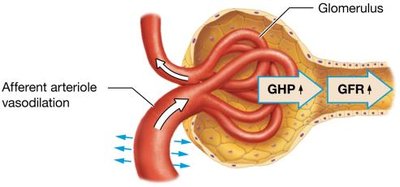
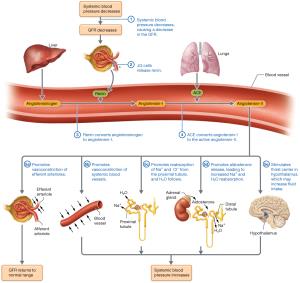
Hormonal Regulation: Renin-angiotensin-aldosterone system (RAAS) increases GFR via vasoconstriction and sodium/water reabsorption; atrial natriuretic peptide (ANP) increases GFR by dilating afferent and constricting efferent arterioles.
Neural Regulation: Sympathetic stimulation can decrease GFR during stress or blood loss.
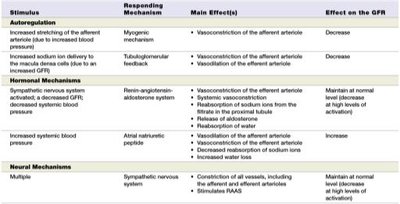
Stimulus | Responding Mechanism | Main Effect(s) | Effect on GFR |
|---|---|---|---|
Increased afferent arteriole stretch | Myogenic | Vasoconstriction of afferent arteriole | Decrease |
Increased NaCl to macula densa | Tubuloglomerular feedback | Vasoconstriction of afferent arteriole | Decrease |
Low blood pressure | RAAS | Vasoconstriction of efferent arteriole, Na+ reabsorption | Maintain/increase |
Increased blood volume | ANP | Dilation of afferent, constriction of efferent arteriole | Increase |
Sympathetic stimulation | Neural | Constriction of vessels | Decrease |
Tubular Reabsorption and Secretion
Principles of Tubular Reabsorption and Secretion
Paracellular Route: Substances pass between tubule cells (e.g., small ions, water).
Transcellular Route: Substances move through tubule cells (e.g., glucose, amino acids).
Carrier-Mediated Transport: Includes facilitated diffusion, primary and secondary active transport, antiporters, and symporters. Carrier proteins have a transport maximum (Tm).
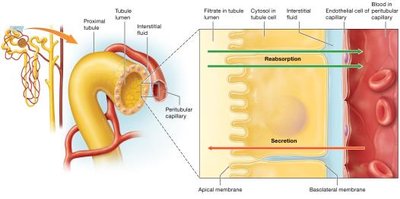
Reabsorption and Secretion in the Proximal Tubule
Reabsorbs most electrolytes, nutrients, bicarbonate, and water; secretes H+, nitrogenous wastes, and drugs.
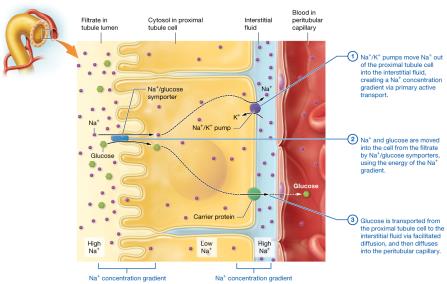
Sodium reabsorption occurs via leak channels, symporters, and antiporters.
Glucose and other solutes are reabsorbed via Na+-symporters and facilitated diffusion.
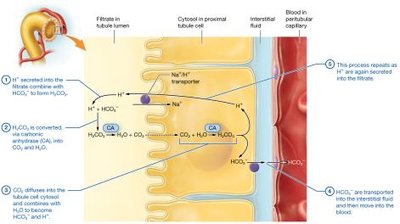
Bicarbonate reabsorption involves the carbonic acid-bicarbonate buffer system.
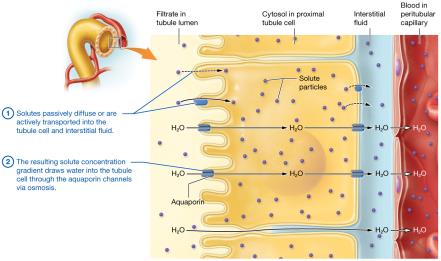
Obligatory water reabsorption follows solute reabsorption via aquaporins.
Reabsorption in the Nephron Loop
Thin Descending Limb: Permeable to water, not solutes; filtrate becomes more concentrated.
Thick Ascending Limb: Impermeable to water, actively reabsorbs NaCl; filtrate becomes less concentrated.
Reabsorption and Secretion in the Distal Tubule and Collecting System
Most water and sodium have already been reabsorbed; fine-tuning occurs here.
Hormonal Regulation:
Aldosterone: Increases Na+ reabsorption, K+ and H+ secretion.
Antidiuretic Hormone (ADH): Increases water reabsorption via aquaporins.
Atrial Natriuretic Peptide (ANP): Inhibits Na+ and water reabsorption.
Medullary Collecting System: Impermeable to water without ADH; permeable to urea and ions; secretes H+.
Urine Concentration and Dilution
Osmolarity of the Filtrate
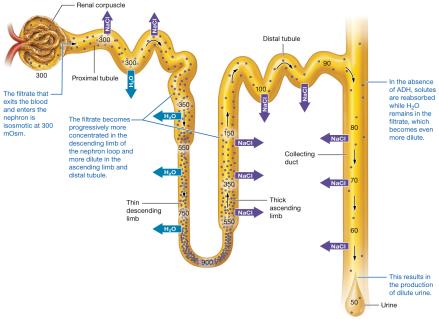
Filtrate is isosmotic with plasma at first (300 mOsm).
Descending limb: filtrate becomes concentrated (up to 1,200 mOsm).
Ascending limb: filtrate becomes dilute (<300 mOsm).
Late distal tubule and collecting system: final concentration depends on ADH and body needs.
Production of Dilute and Concentrated Urine
Dilute Urine: Low ADH, principle cells impermeable to water, urine can be as dilute as 50 mOsm.
Concentrated Urine: High ADH, water reabsorbed, urine can reach 1,200 mOsm.
The Countercurrent Mechanism
Establishes and maintains the medullary osmotic gradient, allowing the kidneys to concentrate urine.
Countercurrent Multiplier: In juxtamedullary nephrons, NaCl is pumped out of the ascending limb, water leaves the descending limb, creating a gradient.
Urea Recycling: Urea diffuses into the interstitial fluid, contributing to the gradient.
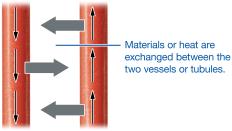
Countercurrent Exchanger: Vasa recta preserves the gradient by exchanging water and solutes as blood flows in opposite directions.
Urine Composition, Transport, and Elimination
Urine Composition and Urinalysis
Normal urine contains water, electrolytes, and metabolic wastes (urea, creatinine, uric acid).
Urinalysis examines color, translucency, odor, pH, specific gravity, and presence of abnormal solutes (e.g., blood, protein, glucose).
Renal Clearance
Measures the rate at which the kidneys remove a substance from the blood (ml/min).
Creatinine and inulin are used to estimate GFR.
Urine Transport, Storage, and Elimination
Urine drains from papillary ducts → minor calyces → major calyces → renal pelvis → ureters → urinary bladder → urethra.
Ureters: Transport urine via peristalsis; lined with transitional epithelium.
Urinary Bladder: Stores urine; detrusor muscle contracts during micturition.
Urethra: Shorter in females, longer in males (with prostatic, membranous, and spongy regions).
Micturition (Urination)
Reflex mediated by the parasympathetic nervous system; involves stretch receptors, spinal cord, and detrusor muscle contraction.
Voluntary control develops with age; involves relaxation of the external urethral sphincter.
Clinical Connections
Nephrolithiasis (Kidney Stones): Crystalline stones (often calcium oxalate) can cause pain, hematuria, and obstruction.
Glomerulonephritis: Inflammation of glomeruli, leading to proteinuria, hematuria, and possible renal failure.
Renal Failure: Acute or chronic; may require dialysis or transplantation.
Diuretics: Drugs that increase urine output by inhibiting solute reabsorption at various nephron sites.
SIADH: Excess ADH secretion causes water retention and concentrated urine.
