 Back
BackThe Urinary System: Structure, Function, and Physiology
Study Guide - Smart Notes

The Urinary System
Overview of Kidney Function
The kidneys are essential organs responsible for filtering blood, removing metabolic wastes, and maintaining homeostasis of fluids, electrolytes, and acid–base balance. They also regulate blood pressure, erythropoiesis, and perform several metabolic functions.
Filtration of Blood: Removes metabolic wastes such as urea, creatinine, and uric acid.
Fluid and Electrolyte Balance: Regulates osmolarity by conserving or eliminating water and electrolytes.
Acid–Base Balance: Maintains blood pH by managing hydrogen and bicarbonate ions.
Blood Pressure Regulation: Controls blood volume and secretes renin, influencing vascular resistance.
Erythropoiesis: Releases erythropoietin to stimulate red blood cell production.
Other Functions: Detoxifies blood, activates vitamin D, and performs gluconeogenesis.
Overview of the Urinary System Structures
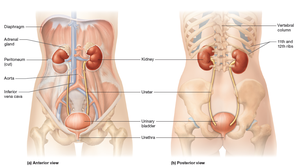
The urinary system consists of the kidneys, ureters, urinary bladder, and urethra. The kidneys are retroperitoneal and bean-shaped, with the right kidney slightly lower due to the liver. The adrenal glands sit atop each kidney but are part of the endocrine system.
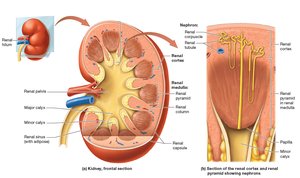
Internal Anatomy of the Kidneys
The kidney's internal structure includes the renal cortex, renal medulla, renal pyramids, renal columns, minor and major calyces, and the renal pelvis. Nephrons, the functional units, are located in both the cortex and medulla.
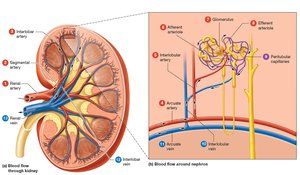
Blood Supply of the Kidneys
Blood enters the kidneys via the renal arteries, branches into segmental, interlobar, arcuate, and interlobular arteries, and is filtered in the glomerulus. Filtered blood exits through the renal veins.
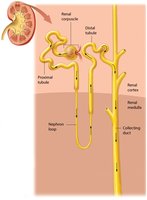
The Nephron
Structure and Function
The nephron is the functional unit of the kidney, responsible for filtration, reabsorption, and secretion. It consists of the renal corpuscle (glomerulus and glomerular capsule) and the renal tubule (proximal tubule, nephron loop, distal tubule, and collecting duct).
Renal Corpuscle
The renal corpuscle filters blood plasma. The glomerulus is a network of fenestrated capillaries, surrounded by the glomerular (Bowman's) capsule, which has parietal and visceral layers. Podocytes in the visceral layer form filtration slits.
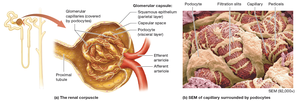
Histology of the Nephron
The nephron tubule is lined with various epithelial cells, including simple squamous and cuboidal cells, with or without microvilli, depending on the segment and its function.
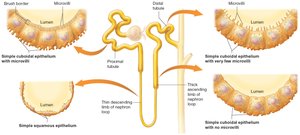
Juxtaglomerular Apparatus (JGA)
The JGA is located at the transition between the ascending limb of the nephron loop and the distal tubule. It consists of macula densa cells and juxtaglomerular (JG) cells, which regulate blood pressure and glomerular filtration rate (GFR).
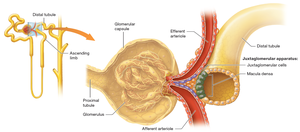
Types of Nephrons
There are two main types of nephrons: cortical nephrons (located mostly in the cortex) and juxtamedullary nephrons (extend deep into the medulla and are crucial for concentrating urine).
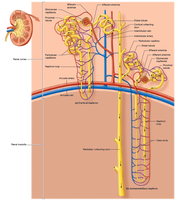
Filtration, Reabsorption, and Secretion
Tubular Secretion
Tubular secretion is the process by which substances are transported from the blood into the tubular fluid, aiding in waste removal and acid–base balance.
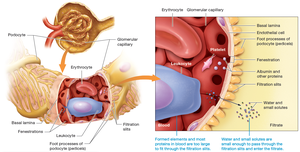
The Filtration Membrane and the Filtrate
The filtration membrane consists of fenestrated capillary endothelium, a basal lamina, and podocyte filtration slits. It allows water and small solutes to pass but restricts large proteins and cells. Nitrogenous wastes such as urea, creatinine, and uric acid are readily filtered.
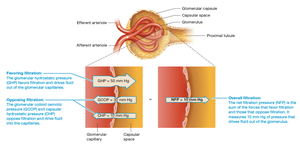
Glomerular Filtration Rate (GFR)
GFR is the amount of filtrate formed by both kidneys per minute (about 125 ml/min). It is determined by the balance of hydrostatic and colloid osmotic pressures across the glomerular capillaries.
Hydrostatic Pressure: Pushes water out of capillaries.
Colloid Osmotic Pressure (COP): Pulls water into capillaries due to plasma proteins.
Net Filtration Pressure (NFP): The difference between these forces determines filtration direction.
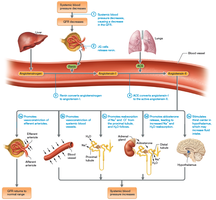
Regulation of GFR
GFR is regulated by autoregulation (myogenic mechanism and tubuloglomerular feedback), hormonal control (renin-angiotensin-aldosterone system, atrial natriuretic peptide), and neural regulation (sympathetic nervous system).
Myogenic Mechanism: Afferent arteriole constricts or dilates in response to blood pressure changes.
Tubuloglomerular Feedback: Macula densa senses NaCl concentration and adjusts arteriole diameter and hormone release.
Renin-Angiotensin-Aldosterone System (RAAS): Increases blood pressure and GFR via angiotensin-II and aldosterone.
Atrial Natriuretic Peptide (ANP): Increases GFR by dilating afferent and constricting efferent arterioles.
Sympathetic Regulation: Varies with stimulation level; can increase or decrease GFR.
Renal Failure
Decreased GFR can lead to acute or chronic renal failure. Uremia results from waste buildup and can cause severe complications. Dialysis (hemodialysis or peritoneal dialysis) is used to manage renal failure.
Reabsorption and Secretion in the Nephron
Proximal Tubule
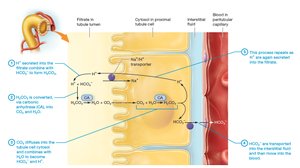
The proximal tubule reabsorbs most filtered ions, nutrients, bicarbonate, and water. It also secretes hydrogen ions, drugs, and nitrogenous wastes.
Sodium and Glucose Reabsorption: Sodium is actively transported, and glucose is reabsorbed via symporters.
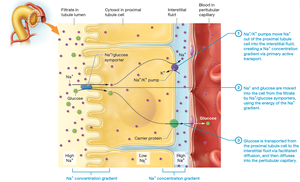
Bicarbonate Reabsorption: Bicarbonate is reabsorbed to maintain acid–base balance.
Nephron Loop (Loop of Henle)
The nephron loop reabsorbs additional water and ions. The descending limb is permeable to water, while the ascending limb is impermeable to water but actively transports NaCl.
Distal Tubule and Collecting System
By the distal tubule, most water and sodium have been reabsorbed. The distal tubule and collecting duct fine-tune water, electrolyte, and acid–base balance, regulated by hormones such as aldosterone, antidiuretic hormone (ADH), and ANP.
Aldosterone: Increases sodium reabsorption and potassium secretion.
ADH: Increases water reabsorption by inserting aquaporins.
ANP: Promotes sodium and water excretion.
Acid–Base Balance
The nephron maintains acid–base balance by secreting hydrogen ions and reabsorbing or excreting bicarbonate, depending on blood pH.
Osmolarity and Concentration of Urine
Osmolarity of Filtrate
Filtrate osmolarity changes throughout the nephron. Obligatory water reabsorption occurs in the proximal tubule and nephron loop, while facultative reabsorption in the distal tubule and collecting duct adjusts urine concentration based on body needs.
Countercurrent Mechanism
The countercurrent mechanism in juxtamedullary nephrons and vasa recta creates and maintains the medullary osmotic gradient, allowing the production of concentrated urine. Urea recycling also contributes to this gradient.
Urine Composition and Urinalysis
Normal Composition
Urine contains water, electrolytes (Na+, K+, Cl−, H+, phosphates, sulfates), metabolic wastes (urea, creatinine, ammonia, uric acid), and small amounts of bicarbonate, calcium, and magnesium. About 1.8 L of urine is produced daily.
Urinalysis
Urinalysis assesses urine color, clarity, odor, pH (normal: 6.0), and specific gravity (1.001–1.035). Abnormal findings may indicate disease or infection.
Renal Clearance
Renal clearance measures the rate at which kidneys remove a substance from blood, used to estimate GFR. Creatinine and inulin are commonly used markers.
Anatomy of the Urinary Tract
Ureters, Bladder, and Urethra
The urinary tract includes two ureters, the urinary bladder, and the urethra. The bladder stores urine and is lined with the detrusor muscle. The urethra differs in length and function between males and females.
Micturition
Micturition is the process of urination, controlled by the micturition center in the pons and regulated by reflexes involving stretch receptors in the bladder wall.
Summary Table: Key Functions of the Urinary System
Function | Description |
|---|---|
Filtration | Removal of wastes and excess substances from blood |
Reabsorption | Return of essential substances to blood |
Secretion | Active transport of additional wastes into filtrate |
Excretion | Elimination of urine from the body |
Homeostasis | Regulation of fluid, electrolyte, and acid–base balance |
Additional info: This guide integrates textbook content with academic context to provide a comprehensive overview of the urinary system, suitable for exam preparation in an anatomy and physiology course.
