 Back
BackThe Urinary System: Structure, Function, and Disorders
Study Guide - Smart Notes

The Urinary System
Overview and Major Organs
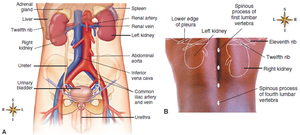
The urinary system is essential for maintaining homeostasis by filtering blood, removing waste, and regulating fluid and electrolyte balance. Its main organs include the kidneys, ureters, urinary bladder, and urethra.
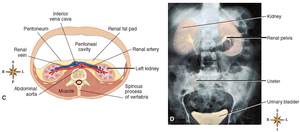
Kidneys: Bean-shaped organs located retroperitoneally, protected by the lower rib cage and back muscles. The right kidney is slightly lower than the left due to the liver's position.
Ureters: Muscular tubes that transport urine from the kidneys to the bladder.
Urinary Bladder: Elastic, muscular sac for urine storage.
Urethra: Tube that conveys urine from the bladder to the exterior.
Kidney Structure and Function
Gross Anatomy of the Kidney
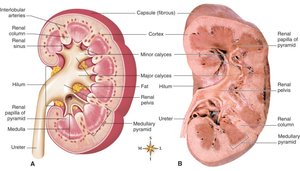
The kidney is divided into two main regions: the outer renal cortex and the inner renal medulla. The medulla contains renal pyramids, which are separated by renal columns. The tip of each pyramid, the renal papilla, drains into minor and major calyces, which converge into the renal pelvis—the funnel-shaped upper end of the ureter.
Renal cortex: Contains the renal corpuscles and convoluted tubules of nephrons.
Renal medulla: Contains the loops of Henle and collecting ducts.
Renal pelvis: Collects urine before it enters the ureter.
Microscopic Structure: The Nephron
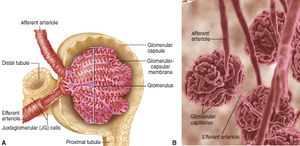
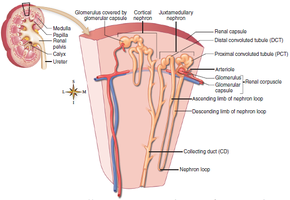
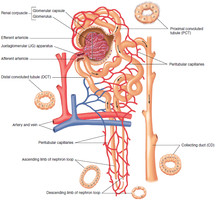
Each kidney contains over one million nephrons, the functional units responsible for urine formation. Each nephron consists of a renal corpuscle and a renal tubule.
Renal corpuscle: Composed of the Bowman capsule and the glomerulus (a tuft of capillaries).
Renal tubule: Includes the proximal convoluted tubule (PCT), nephron loop (loop of Henle), distal convoluted tubule (DCT), and collecting duct (CD).
Cortical nephrons: Located mostly in the cortex; comprise about 85% of nephrons.
Juxtamedullary nephrons: Located near the cortex-medulla junction; crucial for concentrating urine.
Kidney Physiology
Functions of the Kidney
The kidneys perform several vital functions:
Excretion of toxins and nitrogenous wastes (e.g., urea, creatinine).
Regulation of blood electrolyte levels (Na+, K+, Cl-, HCO3-).
Maintenance of water balance and blood pressure (via renin and erythropoietin secretion).
Regulation of red blood cell production (by secreting erythropoietin).
Urine Formation
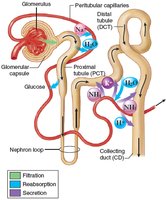
Urine formation involves three main processes: filtration, reabsorption, and secretion.
Filtration: Occurs in the renal corpuscle; blood pressure forces water and solutes from the glomerulus into the Bowman capsule. Normal glomerular filtration rate (GFR) is about 125 mL/min.
Reabsorption: Movement of substances from the renal tubules back into the blood, primarily in the PCT. About 99% of filtered water is reabsorbed. Sodium is actively reabsorbed, creating an osmotic gradient for water reabsorption.
Secretion: Additional substances (e.g., H+, K+, drugs) are actively transported from blood into the distal tubule and collecting duct.
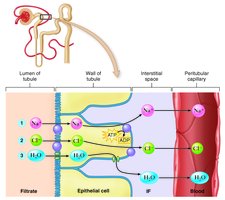
Mechanisms of Reabsorption
Reabsorption of sodium, chloride, and water is tightly regulated. Sodium is actively transported, followed by passive movement of chloride and water due to electrical and osmotic gradients.
Countercurrent mechanism: The nephron loop creates a hypertonic medulla, allowing for concentrated urine formation.
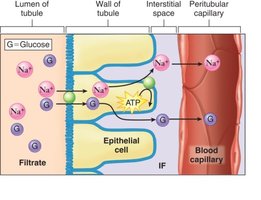
Glucose reabsorption: Occurs in the PCT via sodium-glucose co-transport. If blood glucose exceeds the renal threshold, glucose appears in urine (glycosuria), as seen in diabetes mellitus.
Hormonal Regulation of Urine Volume
Urine volume is regulated by several hormones:
Antidiuretic hormone (ADH): Increases water reabsorption in collecting ducts, reducing urine volume.
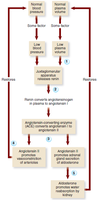
Aldosterone: Promotes sodium and water reabsorption; triggered by the renin-angiotensin-aldosterone system (RAAS).
Atrial natriuretic hormone (ANH): Increases sodium and water excretion, increasing urine volume.
Ureters, Bladder, and Urethra
Ureters
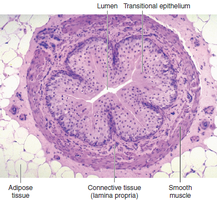
Ureters are narrow, muscular tubes lined with mucous membrane. They transport urine from the renal pelvis to the urinary bladder by peristalsis.
Urinary Bladder
The bladder is an elastic, muscular organ lined with mucosa arranged in rugae. It stores urine until micturition (voiding) and can expand significantly due to its structure.
Urethra
The urethra is a narrow tube lined with mucous membrane, conducting urine from the bladder to the exterior. In males, it also serves as a passage for semen.
Micturition and Disorders
Micturition (Urination)
Micturition is the process of expelling urine from the bladder. It is regulated by involuntary (internal urethral sphincter) and voluntary (external urethral sphincter) muscles. The emptying reflex is triggered by bladder wall stretch, leading to contraction and sphincter relaxation.
Common Disorders
Urinary retention: Urine is produced but not voided.
Urinary suppression: No urine is produced.
Urinary incontinence: Involuntary loss of urine; types include urge, stress, overflow, and reflex incontinence.
Nocturnal enuresis: Bedwetting during sleep.
Neurogenic bladder: Unpredictable voiding due to nerve dysfunction.
Urinalysis and Renal Disorders
Urinalysis
Urinalysis is the physical, chemical, and microscopic examination of urine. It provides diagnostic clues for various diseases by assessing color, turbidity, odor, specific gravity, pH, and the presence of abnormal substances (e.g., proteins, glucose, casts).
Major Renal and Urinary Disorders
Obstructive conditions: Blockage of urine flow can cause hydronephrosis (enlargement of renal pelvis and calyces) or renal calculi (kidney stones).
Tumors: Renal cell carcinoma and bladder cancer, often presenting with hematuria.
Urinary tract infections (UTIs): Infections of the urethra (urethritis), bladder (cystitis), or kidney (pyelonephritis).
Glomerular disorders: Damage to the glomerular membrane can cause nephrotic syndrome, proteinuria, hypoalbuminemia, and edema. Acute glomerulonephritis is often post-streptococcal; chronic forms may lead to renal failure.
Kidney failure: Acute (reversible) or chronic (progressive loss of nephrons). Polycystic kidney disease (PKD) is a hereditary cause of chronic renal failure.
Progression of Chronic Renal Failure
Stage 1: Compensation by remaining nephrons; normal BUN levels.
Stage 2: Renal insufficiency; BUN rises as function declines.
Stage 3: Uremia; complete failure requiring dialysis or transplantation.
Key Terms: Glomerulus, Bowman capsule, nephron, GFR, ADH, aldosterone, ANH, urinalysis, hydronephrosis, renal calculi, nephrotic syndrome, BUN (blood urea nitrogen)
Example: In diabetes mellitus, excess glucose in the blood exceeds the renal threshold, resulting in glucose in the urine (glycosuria).
Additional info: The RAAS system is a critical regulator of blood pressure and fluid balance, and its dysfunction can contribute to hypertension and edema.
