 Back
BackThe Urinary System: Structure, Function, and Regulation
Study Guide - Smart Notes

The Urinary System
Functions of the Urinary System
The urinary system is essential for maintaining the body's internal environment by regulating the composition and volume of blood. It performs several critical functions:
Adjusting blood volume and pressure: By controlling the amount of water excreted and the release of hormones that regulate blood pressure.
Regulating blood plasma ion concentrations: Maintains electrolyte balance (e.g., sodium, potassium, calcium).
Stabilizing blood pH: By excreting hydrogen ions and reabsorbing bicarbonate.
Producing urine: Removes metabolic wastes and excess substances from the blood.
Removing toxins: Filters out drugs and metabolic byproducts.
Producing hormones: Calcitriol (active vitamin D) and erythropoietin (EPO) for red blood cell production.
Urinary Tract Anatomy
Main Components
Ureters: Muscular tubes that conduct urine from the kidneys to the urinary bladder using gravity and peristalsis.
Urinary bladder: Hollow organ that stores urine until excretion.
Urethra: Tube that conducts urine from the bladder to the outside of the body.
Kidney Location and Structure
Located against the posterior body wall, protected by the 11th and 12th ribs.
Left kidney is slightly superior to the right due to the liver's position.
Supporting tissues:
Fibrous capsule (collagen fibers)
Perinephric fat (adipose tissue)
Renal fascia (anchors kidney)
Gross and Microscopic Anatomy of the Kidney
Major landmarks: Fibrous capsule, renal cortex, renal medulla (contains renal pyramids, papillae, and columns), kidney lobe.
Other features: Minor calyx, major calyx, renal pelvis (continuous with ureter).
Nephrons: Functional units of the kidney; two types:
Cortical nephrons
Juxtamedullary nephrons
Nephron Structure and Function
Segments of a Nephron
Renal corpuscle: Site of filtration; includes the glomerular (Bowman's) capsule and glomerulus.
Proximal convoluted tubule (PCT): Reabsorbs nutrients, water, and ions from filtrate back into the blood.
Nephron loop (Loop of Henle): Establishes osmotic gradient for water reabsorption.
Distal convoluted tubule (DCT): Adjusts tubular fluid composition by reabsorption and secretion.
Collecting system: Series of tubes carrying tubular fluid away from the nephron.
Circulation Patterns of the Kidneys
Arterial system: Renal artery → Segmental arteries → Interlobar arteries → Arcuate arteries → Cortical radiate arteries → Afferent arterioles → Glomerulus
Venous system: Reverse of arterial system.
Blood flow around a cortical nephron: Afferent arteriole → Glomerulus → Efferent arteriole → Peritubular capillaries
Kidney Homeostasis and Urine Formation
Renal Physiology
Maintains homeostasis by regulating blood volume and composition.
Concentrates urine and excretes metabolic wastes (e.g., urea, creatinine, uric acid).
Urine Formation
Filtration: Blood pressure forces water and solutes across glomerular capillaries into the capsular space.
Reabsorption: Movement of water and solutes from the filtrate back into the blood.
Secretion: Additional solutes are secreted from blood into the tubular fluid.
These three functions maintain blood volume, composition, and homeostasis.
Filtration Membrane
Consists of fenestrated glomerular capillaries (large pores), podocytes (cells with filtration slits), and a basement membrane.
Prevents most plasma proteins from entering the capsular space.
Factors Controlling Glomerular Filtration
Glomerular hydrostatic pressure (GHP): Blood pressure in glomerular capillaries (pushes filtrate out).
Capsular colloid osmotic pressure: Tends to draw water out of filtrate (usually negligible).
Capsular hydrostatic pressure (CsHP): Opposes GHP by pushing water and solutes back into blood.
Net filtration pressure (NFP): Sum of all pressures; determines overall filtration rate.
Glomerular filtration rate (GFR): Amount of filtrate produced each minute.
Control of GFR
Autoregulation: Local adjustment of blood flow and pressure in the kidney.
Central regulation: Involves endocrine (hormonal) and neural responses if autoregulation fails.
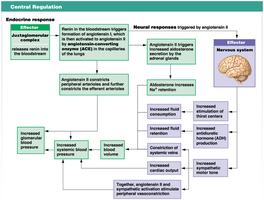
Additional info: The image above illustrates the Renin-Angiotensin-Aldosterone System (RAAS) and neural responses that regulate GFR, blood pressure, and blood volume. Renin release triggers a cascade resulting in angiotensin II formation, which increases blood pressure and stimulates aldosterone and ADH release, enhancing water and sodium retention.
Reabsorption and Secretion
Reabsorption in the Nephron
Most reabsorption occurs in the PCT (>99% of glucose, amino acids, and nutrients; ions; water).
Only 15–20% of filtrate reaches the DCT.
Nephron Loop and Countercurrent Multiplication
Countercurrent multiplication: Fluids move in opposite directions, increasing the effect of solute and water reabsorption.
Creates a concentration gradient in the renal medulla, enabling production of concentrated urine.
Water Reabsorption
Obligatory water reabsorption: Occurs in PCT and descending limb of nephron loop; not adjustable.
Facultative water reabsorption: Occurs in DCT and collecting tubule; regulated by ADH according to hydration status.
Without ADH: No facultative water reabsorption; urine is dilute.
With ADH: Aquaporins form, allowing water reabsorption; urine is concentrated.
Caffeine and alcohol inhibit ADH, increasing urine output.
Clinical Aspects of the Urinary System
Renal Failure
Chronic renal failure: Gradual loss of kidney function; irreversible; managed by diet and bicarbonate supplements.
Acute renal failure: Rapid loss of function; may recover with treatment; caused by toxins, ischemia, obstruction, or trauma.
Treatment: Dialysis (passive diffusion across a membrane); kidney transplant is the only cure.
Urinary Tract Structure and Function
Transports, stores, and eliminates urine.
Includes ureters, bladder, and urethra.
Visualized by pyelogram (X-ray with dye).
Ureters: Paired tubes with mucosa, muscular, and connective tissue layers; conduct urine to bladder.
Urinary bladder: Hollow, muscular organ with rugae (folds) for expansion.
Urethra: Extends from bladder to exterior; longer in males (also transports semen).
Conduction and Storage of Urine
Bladder wall: Three muscle layers (detrusor muscle).
Urethra wall: Lined with stratified epithelium.
Urinary Disorders
Primary Signs
Volume and appearance changes:
Polyuria: Excessive urine (diabetes, kidney disease).
Oliguria: Reduced urine; Anuria: No urine (serious kidney problems).
Frequency changes:
Increased urgency/frequency (UTI, irritation).
Incontinence: Inability to control urination (stress, urge, overflow types).
Urinary retention: Inability to urinate (often due to enlarged prostate in males).
Pain: Kidney infections (pyelonephritis), kidney stones (renal calculi), dysuria (painful urination).
Other clinical signs: Edema, fever (infection), cystitis (bladder infection), pyelonephritis (kidney infection).
Summary Table: Key Functions and Disorders of the Urinary System
Function/Disorder | Description |
|---|---|
Filtration | Movement of water and solutes from blood into nephron |
Reabsorption | Return of water and solutes from filtrate to blood |
Secretion | Active transport of solutes from blood into filtrate |
Polyuria | Excessive urine output |
Oliguria/Anuria | Reduced/no urine output |
Incontinence | Loss of voluntary control of urination |
Renal failure | Loss of kidney function; may be acute or chronic |
