 Back
BackThe Urinary System: Structure, Function, and Mechanisms
Study Guide - Smart Notes

The Urinary System
Overview and Functions
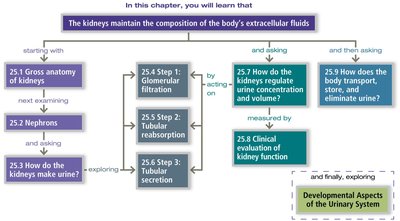
The urinary system is essential for maintaining the composition of the body's extracellular fluids by filtering blood, removing wastes, and regulating fluid and electrolyte balance. It consists of the kidneys, ureters, urinary bladder, and urethra.
Filtration: Kidneys filter 200–400 liters of fluid from the blood daily, removing toxins, metabolic wastes, and excess ions as urine.
Regulation: Maintains blood volume, chemical composition, water-salt balance, and acid-base balance.
Hormone Production: Produces renin (regulates blood pressure), erythropoietin (stimulates red blood cell production), and activates vitamin D.
Gross Anatomy of the Kidneys
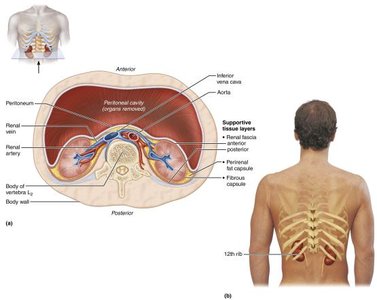
Location and External Anatomy
The kidneys are bean-shaped organs located in a retroperitoneal position in the superior lumbar region, extending from the 12th thoracic to the 3rd lumbar vertebrae. The right kidney is slightly lower due to the presence of the liver.
Lateral surface: Convex
Medial surface: Concave, with a vertical cleft called the renal hilus leading to the renal sinus
Structures entering/exiting at the hilus: Ureters, renal blood vessels, lymphatics, and nerves
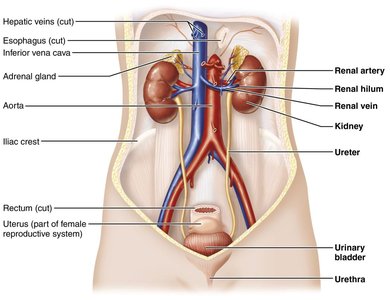
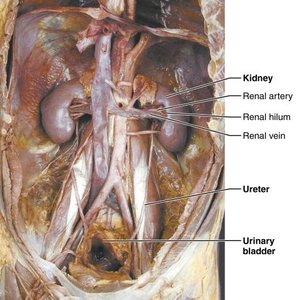
Other Urinary System Organs
Ureters: Paired tubes transporting urine from kidneys to bladder
Urinary bladder: Temporary storage reservoir for urine
Urethra: Transports urine from bladder out of the body
Internal Anatomy of the Kidneys
Regions and Structures
The kidney has three main regions: cortex, medulla, and renal pelvis.
Cortex: Light-colored, granular, superficial region
Medulla: Contains cone-shaped renal pyramids made of parallel bundles of urine-collecting tubules
Renal columns: Inward extensions of cortical tissue separating the pyramids
Renal pelvis: Flat, funnel-shaped tube within the renal sinus
Major and minor calyces: Collect urine from papillae and empty into the renal pelvis
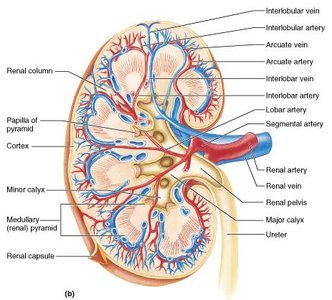
Blood and Nerve Supply
About one-fourth (1200 mL) of systemic cardiac output flows through the kidneys each minute.
Arterial and venous flow follow similar paths; nerve supply is via the renal plexus.
The Nephron: Functional Unit of the Kidney
Structure of the Nephron
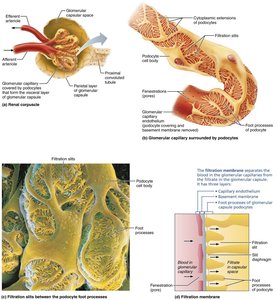
Nephrons are the blood-processing units that form urine. Each nephron consists of a renal corpuscle and a renal tubule.
Renal corpuscle: Includes the glomerulus (tuft of capillaries) and Bowman's (glomerular) capsule
Glomerular endothelium: Fenestrated epithelium allowing solute-rich, protein-free filtrate to pass
Bowman's capsule: Surrounds the glomerulus; has a parietal (structural) and visceral (podocyte) layer
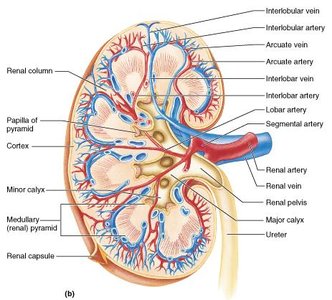
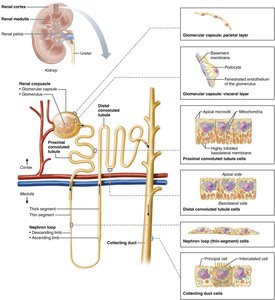
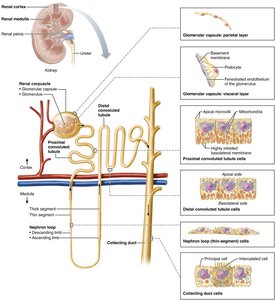
Renal Tubule Segments
Proximal convoluted tubule (PCT): Cuboidal cells with microvilli; reabsorbs water and solutes, secretes substances
Nephron loop (Loop of Henle): Descending limb (thin, simple squamous cells, permeable to water), ascending limb (thick, cuboidal/columnar cells, permeable to solutes)
Distal convoluted tubule (DCT): Cuboidal cells, mainly for secretion
Collecting duct: Contains principal cells (water/salt balance) and intercalated cells (acid-base balance)
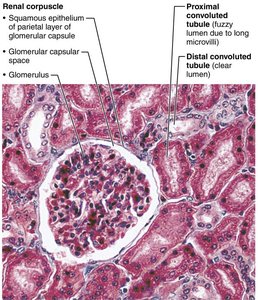
Types of Nephrons
Cortical nephrons: 85% of nephrons, located in cortex, short nephron loops
Juxtamedullary nephrons: Located at cortex-medulla junction, long loops deeply invade medulla, involved in concentrated urine production
Capillary Beds of the Nephron
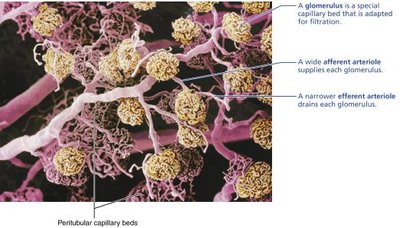
Glomerulus and Peritubular Capillaries
Each nephron has two capillary beds: glomerulus (filtration) and peritubular capillaries (reabsorption)
Glomerulus is fed by an afferent arteriole and drained by an efferent arteriole
Blood pressure in the glomerulus is high, promoting filtration
Peritubular capillaries are low-pressure, porous, and adapted for absorption
Vasa recta: Long, straight capillaries associated with juxtamedullary nephrons, maintain medullary osmotic gradient
Juxtaglomerular Apparatus (JGA)
Structure and Function
Located where the distal tubule contacts the afferent arteriole
Juxtaglomerular (JG) cells: Smooth muscle cells with renin-containing granules, act as mechanoreceptors
Macula densa: Tall, closely packed distal tubule cells, function as chemoreceptors/osmoreceptors
Mesangial cells: Control glomerular filtration rate
Mechanism of Urine Formation
Three Major Processes
Glomerular filtration: Passive process; hydrostatic pressure forces fluids and solutes through a membrane
Tubular reabsorption: Selective process; returns most filtrate to blood
Tubular secretion: Moves substances from blood into filtrate
Filtration Membrane
Three layers: fenestrated endothelium, visceral membrane (podocytes), and fused basement membrane
Allows passage of water and small solutes; blocks proteins and blood cells
Net Filtration Pressure (NFP)
Responsible for filtrate formation
Calculated as:
Where HP_g = glomerular hydrostatic pressure, OP_g = oncotic pressure, HP_c = capsular hydrostatic pressure
Glomerular Filtration Rate (GFR)
Total amount of filtrate formed per minute by the kidneys
Directly proportional to NFP, filtration membrane permeability, and surface area
Regulated by renal autoregulation, neural controls, and the renin-angiotensin system
Tubular Reabsorption and Secretion
Reabsorption
Most filtrate is reabsorbed into the blood via transcellular or paracellular routes
All organic nutrients are reabsorbed; water and ion reabsorption is hormonally controlled (ADH, aldosterone, ANP, PTH)
Sodium reabsorption is primarily active, via Na+-K+ ATPase pumps
Secretion
Reverse of reabsorption; substances move from peritubular capillaries into filtrate
Important for disposing of drugs, excess ions, and controlling blood pH
Regulation of Urine Concentration and Volume
Countercurrent Mechanism
Keeps the solute load of body fluids constant (~300 mOsm)
Countercurrent multiplier: Nephron loops create medullary osmotic gradient
Countercurrent exchanger: Vasa recta preserve the gradient
Formation of Dilute and Concentrated Urine
Dilute urine: Formed when ADH is not secreted; collecting ducts are impermeable to water
Concentrated urine: ADH increases water reabsorption; urine osmolality rises
Physical and Chemical Characteristics of Urine
Color: Clear, pale to deep yellow (urochrome pigment)
Odor: Slightly aromatic; ammonia odor develops on standing
pH: Slightly acidic (pH 6), range 4.5–8.0
Specific gravity: 1.001–1.035, depending on solute concentration
Chemical composition: 95% water, 5% solutes (urea, uric acid, creatinine, ions)
Ureters, Urinary Bladder, and Urethra
Ureters
Slender tubes conveying urine from kidneys to bladder
Enter bladder at an angle to prevent backflow
Wall has three layers: transitional epithelium, smooth muscle, fibrous connective tissue
Urinary Bladder
Muscular sac for temporary urine storage
Located retroperitoneally on pelvic floor
Wall has three layers: transitional epithelium, thick muscle, fibrous adventitia
Trigone: Triangular area prone to infection
Urethra
Muscular tube draining urine from bladder to outside
Internal urethral sphincter (involuntary) and external urethral sphincter (voluntary)
Female urethra: short, anterior to vaginal opening
Male urethra: prostatic, membranous, and spongy regions
