 Back
BackThe Vascular and Lymphatic Systems: Structure, Function, and Pathology
Study Guide - Smart Notes

Vascular System Overview
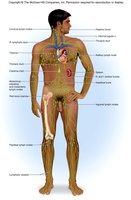
Introduction to the Vascular System
The vascular system is composed of two main components: the blood vascular system and the lymphatic vascular system. These systems are responsible for the transport of blood and lymph, facilitating the exchange of gases, nutrients, and metabolic wastes across vessel walls.
Blood vascular system: Provides continuous flow of blood to and from the heart.
Lymphatic vascular system: Returns excess tissue fluid to the bloodstream and plays a role in immune defense.
Blood Vessel Types and Structure
Types of Blood Vessels
Blood vessels are classified based on their structure and function:
Arteries: Carry blood away from the heart.
Veins: Return blood to the heart.
Capillaries: Sites of exchange between blood and tissues.
Structure of Blood Vessel Walls
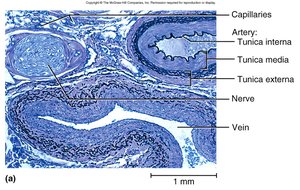
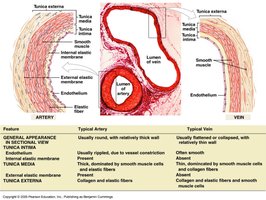
Most blood vessels have three layers, or tunics:
Tunica intima (interna): Innermost layer, lined by endothelium (simple squamous cells).
Tunica media: Middle layer, composed of smooth muscle, collagen, and elastic fibers; responsible for vasomotion (vasoconstriction and vasodilation).
Tunica externa (adventitia): Outermost layer, made of loose connective tissue.
Control of Vessel Diameter
The smooth muscle in the tunica media is regulated by the autonomic nervous system (ANS):
Sympathetic stimulation: Releases norepinephrine, causing vasoconstriction in skin, GI, reproductive, and urinary tracts; vasodilation in coronary, brain, and skeletal muscle vessels.
Parasympathetic stimulation: Releases acetylcholine, causing vasodilation in skin, GI, reproductive, and urinary tracts.
Arterial System
Types of Arteries
Arteries are classified by size and function:
Conducting (elastic) arteries: Largest arteries (e.g., aorta, pulmonary, common carotid); tunica media contains elastic tissue for expansion and recoil, reducing blood pressure fluctuations.
Distributing (muscular) arteries: Distribute blood to specific organs (e.g., femoral, splenic); thick smooth muscle layer.
Resistance arteries (arterioles): Control blood flow into organs.
Metarterioles: Short vessels connecting arterioles to capillaries, with precapillary sphincters.
Capillaries and Capillary Beds
Types of Capillaries
Capillaries are specialized for exchange and are classified by their permeability:
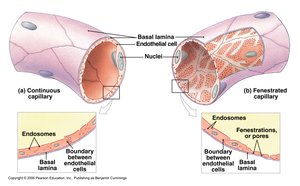
Continuous capillaries: Most common; tight junctions with intercellular clefts allow passage of small solutes.
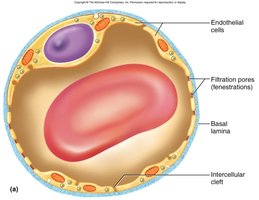
Fenestrated capillaries: Found in kidneys and small intestine; filtration pores allow rapid exchange of small molecules.
Sinusoids: Found in liver, bone marrow, spleen; large gaps allow passage of proteins and blood cells.
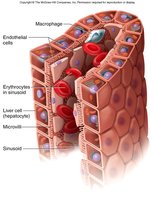
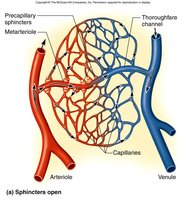
Capillary Beds and Regulation
Capillary beds consist of metarterioles, true capillaries, thoroughfare channels, and postcapillary venules. Precapillary sphincters regulate blood flow into true capillaries and are controlled by the ANS, local chemicals, and physical factors (O2, CO2, pH, heat).
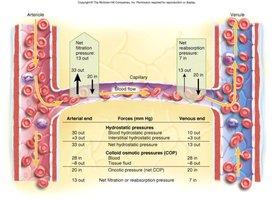
Capillary Exchange
Exchange of fluids and solutes across capillary walls is governed by hydrostatic and osmotic pressures:
Hydrostatic pressure: Outward force exerted by blood pressure.
Colloid osmotic pressure (COP): Inward force due to plasma proteins (mainly albumin).
On the arterial side, net filtration occurs; on the venous side, net reabsorption occurs. Excess fluid (about 3.6 L/day) enters lymphatic vessels.
Venous System
Types of Veins
Veins are classified by size and function:
Large veins
Medium veins
Small veins
Venules
Postcapillary venules
Venous sinuses: Thin walls, large lumens, no smooth muscle.
Venous Return Mechanisms
Venous return is aided by:
Pressure gradient (ΔP)
Skeletal muscle pump
Thoracic pump (during inhalation)
Cardiac suction (expanding atrial space)
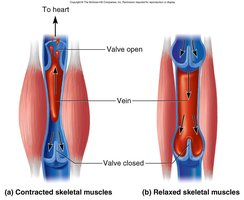
Circulatory Routes and Anastomoses
Circulatory Pathways
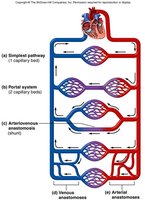
Blood can flow through different routes:
Classic route: Heart → arteries → arterioles → capillaries → venules → veins
Portal system: Blood flows through two consecutive capillary beds (e.g., hepatic portal system).
Anastomoses: Points where two blood vessels merge, providing alternate routes for blood flow.
Blood Pressure
Definition and Determinants
Blood pressure (BP) is the force exerted by blood against vessel walls. It is determined by the amount of blood flow and the resistance of vessels. The main equation is:
Where ΔP is the pressure difference and R is resistance.
Arterial Blood Pressure
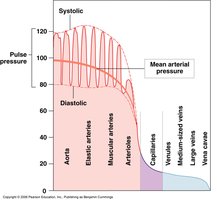
Systolic pressure: During ventricular contraction (systole).
Diastolic pressure: During ventricular relaxation (diastole).
Pulse pressure: Systolic - diastolic pressure.
Mean arterial pressure (MAP):
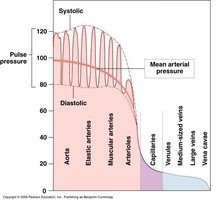
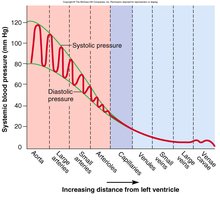
Blood Pressure Changes with Distance
Blood pressure decreases as blood moves from arteries to veins due to resistance and vessel elasticity. Arterial elasticity helps maintain steady flow and reduces stress on small arteries.
Lymphatic System
Components and Functions
The lymphatic system collects excess fluid and solutes lost from capillaries, returning about 3.6 L/day to the venous system. It also transports hormones, nutrients, and waste products, and plays a key role in immune defense.
Lymph: Fluid similar to plasma but low in proteins.
Lymphatic vessels: Network returning lymph to the bloodstream.
Lymphoid tissues and organs: Sites of immune cell production and function.
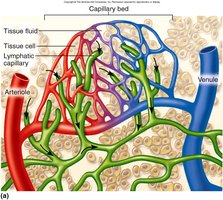
Lymphatic Capillaries
Lymphatic capillaries differ from blood capillaries:
Start as pockets, not tubes
Originate in capillary beds
Larger diameter, thinner walls
Endothelial cells overlap to form one-way minivalves
Lymphedema
Lymphedema results from blockage of lymph drainage, causing swelling and impaired immune function. Causes include tumors, obesity, inflammation, surgery, or parasitic infection (elephantiasis).

Vascular Pathology
Atherosclerosis
Atherosclerosis is the buildup of lipid, calcium, and fibrous deposits (atheromatous plaques) in the intima of large and medium arteries. It is the leading cause of death and morbidity in the US, causing myocardial infarction and stroke. Risk factors include smoking, hypertension, diabetes, and high cholesterol.
Pathogenesis: Endothelial injury allows lipid accumulation, macrophage infiltration, foam cell formation, and plaque development.
Complications: Ischemia, thrombosis, embolism, aneurysm formation.
Treatment: Lifestyle changes, statins, antihypertensives, surgical interventions (angioplasty, stenting, bypass).
Hypertension
Hypertension (high blood pressure) is a major risk factor for cardiovascular disease. It can be essential (primary, idiopathic) or secondary (due to renal, endocrine, or other causes).
Essential hypertension: Multifactorial, involving genetics and environment (diet, obesity, inactivity, stress).
Secondary hypertension: Often due to renal disease, endocrine disorders, or medications.
Complications: Heart failure, kidney disease, stroke, aneurysm, vision loss, metabolic syndrome.
Treatment: Lifestyle changes, antihypertensive medications (beta-blockers, diuretics, ACE inhibitors, ARBs, calcium channel blockers).
Other Vascular Diseases
Vasculitis: Inflammation of blood vessels, often autoimmune or secondary to infection or drugs.
Thrombophlebitis: Vein inflammation due to clot formation; risk factors include immobility, pregnancy, and estrogen therapy.
Raynaud's disease: Hyperactivation of sympathetic nervous system causing vasoconstriction, especially in fingers and toes.
Shock and Organ Failure
Shock is a life-threatening condition of inadequate tissue perfusion. Types include cardiogenic, hypovolemic, anaphylactic, septic, and neurogenic shock. Prolonged shock leads to multiple organ failure and death.
Symptoms: Low BP, rapid pulse, poor perfusion, confusion, pallor.
Complications: Acute respiratory distress syndrome, disseminated intravascular coagulation (DIC).
