 Back
BackThoracic Cavity and Respiratory System: Gross Anatomy and Functional Organization
Study Guide - Smart Notes

Thoracic Cavity: Gross Anatomy
Orientation and Structure
The thoracic cavity houses vital organs such as the heart and lungs, and is bounded by the rib cage, vertebral column, and diaphragm. Understanding its cross-sectional anatomy is essential for clinical and anatomical studies.
Spinous process projects posteriorly, serving as a landmark in transverse sections.
The heart is slightly left of the midline, making the left lung slightly smaller than the right.
The position of vertebrae, bronchi, and arteries varies with the level of the thoracic cavity.
Bronchi contain cartilaginous plates for structural support.
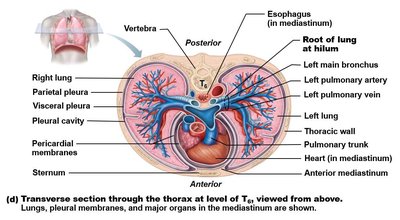
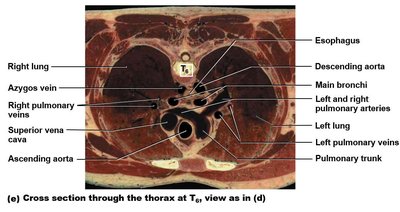
Arteries have elastic tissue and smooth muscle; veins have larger diameters and thinner walls.
Systemic and pulmonary vessels intermingle within the thoracic cavity.
Paired and unpaired vessels are distinguished by their anatomical positions.
Bronchopulmonary Segments
Segmental Organization of the Lungs
Each lung is divided into bronchopulmonary segments, which are functionally and anatomically discrete units. This segmentation is crucial for surgical resection and understanding pulmonary pathology.
There are approximately 10 segments per lung.
Each segment is supplied by a single tertiary (segmental) bronchus.
Segments are separated by dense connective tissue and contain multiple lung lobules.
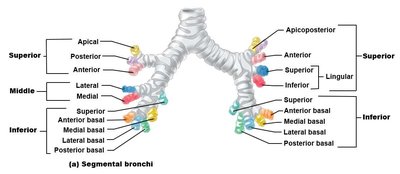
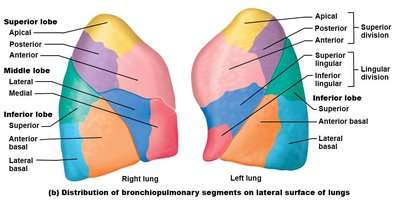
Segments are relatively independent, separated by connective tissue, with few small veins between them.
Pleural Membranes and Pleural Cavity
Structure and Clinical Importance
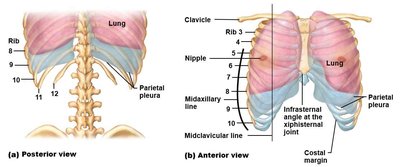
The lungs are enveloped by a double-layered serous membrane called the pleura. The pleural cavity, filled with pleural fluid, reduces friction during respiration and maintains negative pressure for lung expansion.
Visceral pleura adheres to the lung surface.
Parietal pleura lines the inner thoracic wall, diaphragm, and mediastinum.
The pleural cavity is the space between these layers, containing pleural fluid.
The inferior location of the parietal pleura is important for maintaining intrapleural pressure, especially during clinical procedures such as thoracentesis.
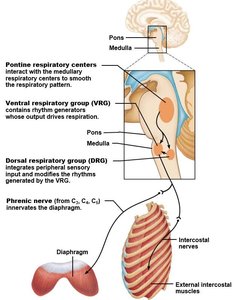
Respiratory Centers of the Brainstem
Neural Control of Breathing
Respiratory rhythm and pattern are regulated by centers in the brainstem, which integrate sensory input and coordinate muscle activity for ventilation.
Ventral Respiratory Group (VRG): Located in the medulla; generates the basic rhythm of breathing.
Pontine Respiratory Group: Located in the pons; smooths and modulates the respiratory pattern.
Dorsal Respiratory Group (DRG): Located in the medulla; integrates peripheral sensory input and modifies VRG output.
Peripheral and Central Chemoreceptors
Regulation of Ventilation by Blood Chemistry
Ventilation rate is adjusted based on blood chemistry, primarily the levels of carbon dioxide, oxygen, and pH. Chemoreceptors relay this information to the brainstem respiratory centers.
Central chemoreceptors: Located in the medulla; sensitive to changes in CO2 and pH in cerebrospinal fluid.
Peripheral chemoreceptors: Located in the carotid bodies (at the bifurcation of the common carotid artery, innervated by the glossopharyngeal nerve) and aortic bodies (in the aortic arch, innervated by the vagus nerve).
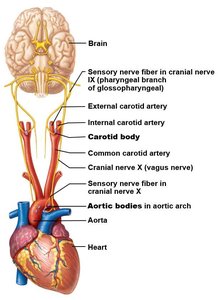
These receptors provide rapid feedback to adjust ventilation in response to hypoxemia, hypercapnia, or acidosis.
Summary Table: Key Features of the Thoracic Cavity and Respiratory System
Structure | Function | Clinical Relevance |
|---|---|---|
Thoracic cavity | Houses heart, lungs, major vessels | Landmarks for imaging, surgery |
Bronchopulmonary segments | Functional lung units | Segmental resection, pathology |
Pleural membranes | Reduce friction, maintain pressure | Pleural effusion, pneumothorax |
Respiratory centers | Control breathing rhythm | Central respiratory disorders |
Chemoreceptors | Monitor blood gases | Ventilatory response to hypoxia |
