 Back
BackUnit 8: Reproduction – Sex Determination, Gametogenesis, and Reproductive Physiology
Study Guide - Smart Notes

Sex Determination During Fetal Development
Chromosomal Sex and Genetic Basis
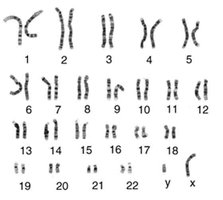
Sex determination in humans is governed by the presence of sex chromosomes, which are distinct from autosomes. Chromosomal sex is established at fertilization, when the sperm and egg combine their genetic material.
Sex Chromosomes: Humans have two types of sex chromosomes: X and Y. Females are typically XX, while males are XY.
Autosomes: The other 22 pairs of chromosomes are autosomes, which do not determine sex.
Genetic Sex: The presence of a Y chromosome (specifically the SRY gene) initiates male development.
Sexual Differentiation and Development of Internal Genitalia
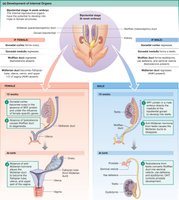
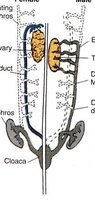
Sexual differentiation begins from a bipotential (sexually indifferent) gonad. The fate of internal ductwork depends on the presence or absence of specific signals.
Wolffian Ducts: Develop into male internal genitalia (epididymis, vas deferens, accessory sex glands) if testosterone is present.
Müllerian Ducts: Develop into female internal genitalia (fallopian tubes, uterus, cervix, upper vagina) if no anti-Müllerian hormone (AMH) or testosterone is present.
AMH: Produced by Sertoli cells in the testes, causes regression of Müllerian ducts in males.
Testosterone: Promotes development of Wolffian ducts and male external genitalia.
Gametogenesis
Comparison of Mitosis and Meiosis
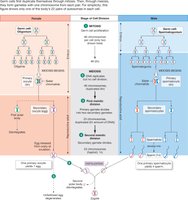
Germ cells undergo specialized cell division processes to produce gametes. Mitosis produces identical cells, while meiosis produces haploid gametes.
Mitosis: Cell division resulting in two identical daughter cells (somatic cell proliferation).
Meiosis: Cell division resulting in four non-identical haploid gametes (sperm or eggs).
Gametogenesis Timelines
The timing and process of gametogenesis differ between males and females.
Female Gametogenesis: Mitosis in oogonia occurs during fetal life. Eggs enter meiosis and arrest in meiosis I until ovulation. Meiosis II is completed only upon fertilization.
Male Gametogenesis: Mitosis in spermatogonia begins at puberty and continues throughout life. Meiosis and differentiation into sperm proceed without arrest.
Hypothalamic-Pituitary-Gonadal (HPG) Axis
Hormonal Regulation of Reproduction
The HPG axis is a central regulatory system for reproductive function in both sexes.
GnRH (Gonadotropin-Releasing Hormone): Released from the hypothalamus, stimulates the anterior pituitary to release LH and FSH.
LH (Luteinizing Hormone): Stimulates steroid production and gamete maturation.
FSH (Follicle-Stimulating Hormone): Supports gametogenesis and follicle development.
Feedback Regulation: Gonadal steroids (testosterone, estradiol, progesterone) exert negative feedback on the hypothalamus and pituitary, except for estradiol under certain conditions, which can trigger positive feedback (LH surge).
Reproductive Function in the Adult Human Male
Anatomy and Spermatogenesis
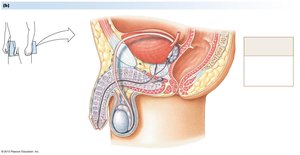
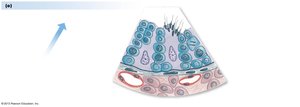
The male reproductive system includes the testes, epididymis, vas deferens, accessory glands, and penis. Spermatogenesis occurs in the seminiferous tubules of the testes.
Spermatogonium: Mitotic stem cell.
Primary Spermatocyte: Enters meiosis I.
Secondary Spermatocyte: Enters meiosis II.
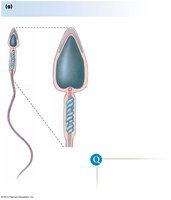
Spermatid: Completed meiosis, undergoes remodeling to become spermatozoa.
Sertoli Cells: Support spermatogenesis and produce AMH.
Leydig Cells: Produce testosterone.
Endocrine Control and Androgen Effects
Testicular androgens regulate spermatogenesis and development of male characteristics.
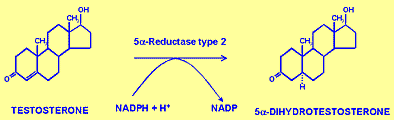
Testosterone: Main androgen, converted to DHT in target cells.
DHT (Dihydrotestosterone): Required for differentiation of external genitalia, development of accessory sex glands, and secondary sexual characteristics.
Negative Feedback: Testosterone and DHT suppress LH, FSH, and GnRH release.
Reproductive Function in the Adult Human Female
Anatomy and Oogenesis
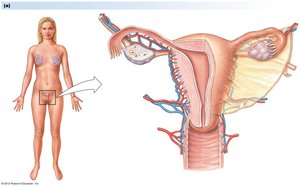
The female reproductive system includes the ovaries, fallopian tubes, uterus, cervix, and vagina. Oogenesis occurs in the ovaries.
Oogonia: Undergo mitosis during fetal life.
Primary Oocytes: Enter meiosis and arrest in meiosis I until ovulation.
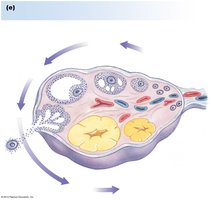
Follicular Development: Follicles mature through primary, secondary, and tertiary stages, culminating in ovulation.
Corpus Luteum: Formed from ovulated follicle, secretes progesterone.
Menstrual Cycle
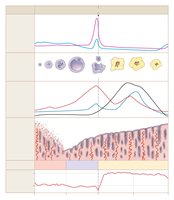
The menstrual cycle consists of the follicular phase, ovulation, and luteal phase, regulated by ovarian hormones and gonadotropins.
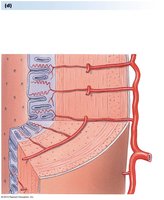
Follicular Phase: Growth of selected follicle, estrogen secretion, endometrial proliferation.
Ovulation: Triggered by LH surge, oocyte released.
Luteal Phase: Corpus luteum secretes progesterone, prepares uterus for pregnancy. If no pregnancy, luteal regression leads to menses.
Fertilization, Pregnancy, and Parturition
Ovulation, Fertilization, and Early Embryonic Development
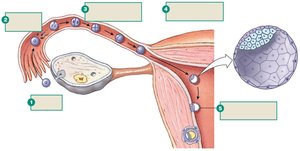
Fertilization occurs in the fallopian tube, followed by early cleavage and formation of the blastocyst, which implants in the uterus.
Zygote: Formed by fusion of sperm and egg.
Blastocyst: Differentiates into inner cell mass (embryo) and trophectoderm (placenta).
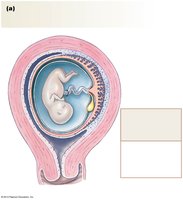
Pregnancy and Placental Development
The placenta and amniotic fluid support fetal development during pregnancy. The umbilical cord connects the fetus to the placenta.
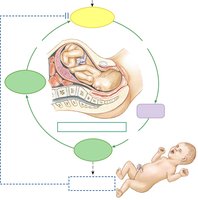
Parturition (Birth)
Parturition involves cervical ripening, uterine contractions, delivery of the baby, and expulsion of the placenta. It is regulated by a cascade of hormones, with oxytocin playing a key role in a positive feedback loop.
Oxytocin: Released from the posterior pituitary, stimulates uterine contractions.
Prostaglandins: Produced by the uterine wall, enhance contractions.
Positive Feedback: Cervical stretch increases oxytocin release, intensifying contractions until delivery.
Key Concepts to Review
Sex chromosomes vs. autosomes
Germ cells vs. somatic cells
Mitosis vs. meiosis
Disorders of Sexual Differentiation
Genetic Mutations Affecting Sexual Development
Mutations in genes such as 5α-reductase or androgen receptor can lead to disorders of sexual differentiation, especially in XY individuals.
5α-Reductase Deficiency: Impairs conversion of testosterone to DHT, affecting external genitalia development.
Androgen Insensitivity: Defective androgen receptor leads to incomplete masculinization.
Summary Table: Wolffian vs. Müllerian Derivatives
Structure | Male (Wolffian) | Female (Müllerian) |
|---|---|---|
Ducts | Efferent ductules, epididymis, vas deferens, accessory sex glands | Fallopian tubes, uterus, cervix, upper vagina |
Hormonal Signal | Testosterone, AMH | Absence of AMH, testosterone |
Additional info:
Some details about the steroidogenic pathway and feedback regulation were inferred from standard physiology textbooks.
Images were selected strictly for direct relevance to the adjacent text.
