 Back
BackUrinary System: Structure and Function Study Guide
Study Guide - Smart Notes

Urinary System Overview
Introduction
The urinary system is essential for maintaining homeostasis by regulating the composition and volume of blood, removing waste products, and controlling electrolyte and acid-base balance. It consists of the kidneys, ureters, urinary bladder, and urethra.
Key Functions: Filtration of blood, formation of urine, regulation of blood pressure, and maintenance of electrolyte balance.
Main Organs: Kidneys, ureters, bladder, urethra.
Kidney Anatomy
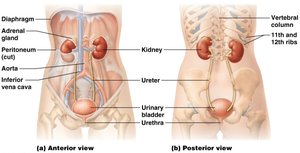
External Kidney Anatomy
The kidneys are retroperitoneal organs located on either side of the vertebral column. They are protected by several layers of connective tissue.
Renal Hilum: Entry/exit site for blood vessels, nerves, and ureter.
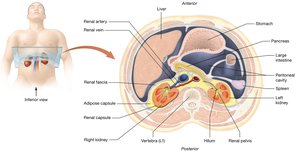
Renal Fascia: Anchors kidney to surrounding structures.
Adipose Capsule: Cushions and protects the kidney.
Renal Capsule: Tough, fibrous covering directly surrounding the kidney.
Internal Kidney Anatomy
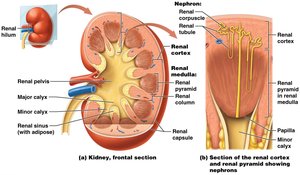
Internally, the kidney is divided into three distinct regions: cortex, medulla, and pelvis.
Renal Cortex: The outermost region, site of filtration.
Renal Medulla: Contains renal pyramids and columns.
Renal Pyramids: Cone-shaped structures containing nephron loops and collecting ducts.
Renal Columns: Extensions of cortex between pyramids.
Minor and Major Calyces: Collect urine from pyramids and funnel it to the renal pelvis.
Renal Pelvis: Central collecting region for urine before it enters the ureter.
Nephron Structure and Types
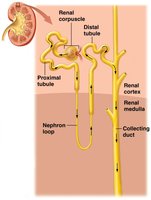
Nephron Anatomy
Nephrons are the functional units of the kidney, responsible for filtering blood and forming urine. Each nephron consists of a renal corpuscle and a renal tubule.
Renal Corpuscle: Includes the glomerulus (capillary network) and Bowman's capsule (surrounds glomerulus).
Renal Tubule: Composed of the proximal convoluted tubule (PCT), nephron loop (Loop of Henle), and distal convoluted tubule (DCT).
Collecting Duct: Receives filtrate from multiple nephrons and is not part of the nephron itself.
Nephron Types
There are two main types of nephrons, each with distinct locations and functions.
Cortical Nephrons: Located almost entirely in the cortex; comprise about 80% of nephrons.
Juxtamedullary Nephrons: Located near the cortex-medulla border; nephron loop extends deep into the medulla, important for concentrating urine.
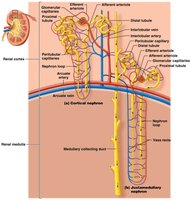
Blood Supply of the Kidneys
Renal Circulation
The kidneys receive a rich blood supply, filtering the entire plasma volume multiple times daily.
Renal Arteries: Branch into smaller arteries and arterioles, eventually reaching the nephrons.
Afferent Arterioles: Bring blood to the glomerulus.
Efferent Arterioles: Carry blood away from the glomerulus to peritubular capillaries.
Venous Return: Parallels arterial supply, with nearly identical vessel names.
Ureters and Bladder
Ureters
Ureters are muscular tubes that propel urine from the kidneys to the urinary bladder.
Function: Transport urine via peristalsis.
Entry: Drain urine into the posterior, inferior aspect of the bladder.
Urinary Bladder
The bladder is a muscular sac that stores urine until excretion.
Capacity: Usually stores about 500 mL, but can hold up to 800-1000 mL.
Trigone Area: Triangular region defined by ureter and urethra openings.
Detrusor Muscle: Smooth muscle responsible for bladder contraction.
Physiology of the Urinary System
Overview of Processes
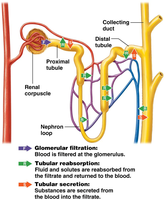
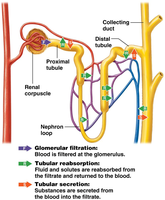
The urinary system performs three main physiological processes: filtration, reabsorption, and secretion.
Filtration: Movement of water and solutes from blood into the nephron.
Reabsorption: Return of useful substances from filtrate back to blood.
Secretion: Addition of waste products from blood into filtrate.
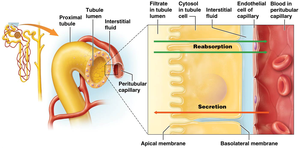
Glomerular Filtration
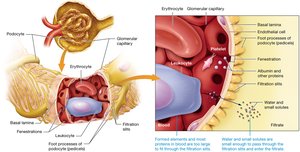
Filtration Membrane
Glomerular filtration occurs at the renal corpuscle, where blood is filtered based on size.
Filtration Membrane: Allows passage of water, electrolytes, and small molecules; blocks proteins and cells.
Example: Water, Na+, Cl-, H+, glucose pass through; albumin and erythrocytes do not.
Filtration Pressure and Rate
Net Filtration Pressure (NFP): Determines direction of water movement and is responsible for filtrate formation.
Glomerular Filtration Rate (GFR): Amount of filtrate formed per minute; normal value is about 125 mL/min.
Equation:
Regulation: GFR is regulated by intrinsic (renal autoregulation) and extrinsic (neural and hormonal) mechanisms.
Intrinsic Regulation of GFR
Myogenic Mechanism
The myogenic mechanism responds to changes in blood pressure by constricting or dilating the afferent arteriole.
Increase in BP: Stretches afferent arteriole, increases GFR; arteriole constricts to restore GFR.
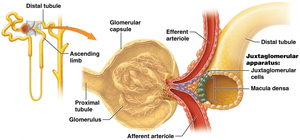
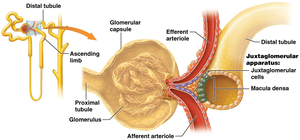
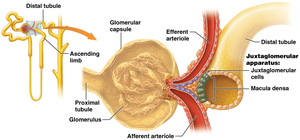
Tubuloglomerular Feedback
Tubuloglomerular feedback involves the juxtaglomerular apparatus and macula densa cells.
High GFR: Increased Na+ and Cl- delivery to macula densa; causes constriction of afferent arteriole, reducing GFR.
Persistent High Na+ and Cl-: Macula densa signals juxtaglomerular cells to reduce renin release.
Extrinsic Regulation of GFR
Neural and Hormonal Control
Neural: Sympathetic nervous system releases norepinephrine, triggering renin release from JG cells.
Renin-Angiotensin-Aldosterone System (RAAS): Activated by SNS, low BP, or low GFR; increases BP and GFR.
Atrial Natriuretic Peptide (ANP): Triggered by increased BP; dilates afferent and constricts efferent arterioles, raising GFR and promoting fluid loss.
Tubular Reabsorption and Secretion
Overview
Tubular reabsorption and secretion are processes that modify the filtrate as it passes through the nephron.
Reabsorption: Movement of substances from filtrate back to blood (peritubular capillaries).
Secretion: Movement of substances from blood into filtrate.
Segmental Functions
Proximal Convoluted Tubule (PCT): Most active in reabsorption and secretion; reabsorbs water, ions, organic substances; secretes H+, nitrogenous wastes, drugs.
Nephron Loop (Loop of Henle): Descending limb reabsorbs water; ascending limb reabsorbs ions (Na+, Cl-).
Distal Convoluted Tubule (DCT): Reabsorbs water and ions (Na+, Cl-, Ca2+); secretes K+ and H+; regulated by hormones.
Additional Notes
Na+ Reabsorption: Primarily via active transport.
Water, ions, organic substances: Secondary active and passive transport.
Collecting Duct: Not part of nephron; reabsorbs/secretes water and ions; regulated by ADH and aldosterone.
Urine Formation: Final product after filtration, reabsorption, and secretion.
Summary Table: Nephron Segment Functions
Segment | Reabsorption | Secretion |
|---|---|---|
PCT | Water, ions, organic substances | H+, nitrogenous wastes, drugs |
Loop of Henle | Descending: water; Ascending: Na+, Cl- | None |
DCT | Water, Na+, Cl-, Ca2+ | K+, H+ |
Collecting Duct | Water, ions (regulated by ADH, aldosterone) | Some ions |
Additional info: The notes above expand on brief points with academic context, definitions, and examples to ensure completeness and clarity for exam preparation.
