 Back
BackUrinary System: Structure, Function, and Histology
Study Guide - Smart Notes

The Urinary System: Overview
Functions of the Urinary System
The urinary system is essential for maintaining homeostasis by regulating the composition and volume of blood and eliminating metabolic waste.
Regulates plasma ion concentrations: Maintains balance of ions such as sodium, potassium, and chloride.
Regulates blood volume and blood pressure: Adjusts water excretion and releases hormones affecting vascular tone.
Stabilizes blood pH: Controls excretion of hydrogen and bicarbonate ions.
Prevents loss of valuable nutrients: Reabsorbs glucose, amino acids, and other essential molecules.
Eliminates metabolic wastes: Removes urea, creatinine, and other byproducts.
Synthesizes calcitriol and erythropoietin: Calcitriol aids calcium absorption; erythropoietin stimulates red blood cell production.
Aids liver metabolic functions: Assists in detoxification and gluconeogenesis.
Components of the Urinary System
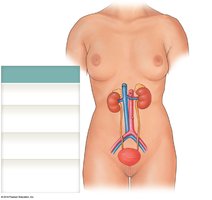
The urinary system consists of several organs that work together to produce, transport, store, and eliminate urine.
Kidneys: Produce urine and contain functional units called nephrons.
Ureters: Transport urine from kidneys to urinary bladder.
Urinary bladder: Temporarily stores urine prior to elimination.
Urethra: Conducts urine to the exterior; in males, also transports semen.
The Kidneys: Anatomy and Protection
Position and Structure
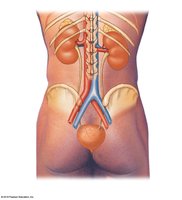
The kidneys are retroperitoneal organs located on either side of the vertebral column.
Right kidney: Covered anteriorly by the liver, right colic flexure, and duodenum.
Left kidney: Covered anteriorly by the spleen, stomach, pancreas, left colic flexure, and jejunum; positioned slightly higher than the right kidney.
Adrenal glands: Located on the superior surface of each kidney.
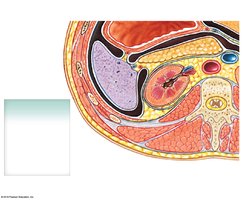
Connective Tissue Layers
Three layers of connective tissue protect the kidneys:
Fibrous capsule: Directly surrounds the kidney.
Perinephric fat (perirenal fat capsule): Cushions and insulates.
Renal fascia: Anchors the kidney to surrounding structures.
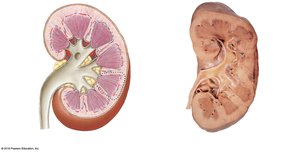
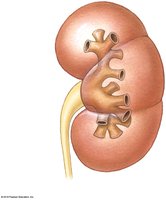
Superficial and Sectional Anatomy
A typical kidney is about 10 cm long, 5.5 cm wide, and 3 cm thick. The hilum is the medial indentation where renal arteries enter and renal veins and ureters exit.
Renal cortex: Outer region.
Renal medulla: Deep to cortex; contains renal pyramids, papillae, and columns.
Renal pelvis: Central collecting region; includes minor and major calyces.
Blood Supply and Innervation of the Kidneys
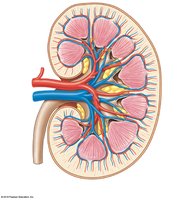
Arterial and Venous Flow
Blood enters the kidneys via the renal arteries and follows a branching pattern:
Renal artery → Segmental arteries → Interlobar arteries → Arcuate arteries → Cortical radiate arteries → Afferent arterioles → Glomerular capillaries
After filtration, blood leaves via:
Glomerular capillaries → Efferent arteriole → Peritubular capillaries → Cortical radiate veins → Arcuate veins → Interlobar veins → Renal vein
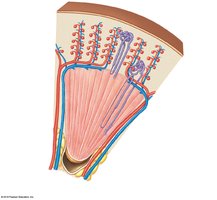
Innervation
Urine production is regulated mostly by autoregulation, involving reflexive changes in nephron arteriole diameter. Sympathetic nerve fibers regulate renal blood flow, pressure, renin release, and water/sodium reabsorption.
Histology of the Kidney: The Nephron and Collecting System
Nephron Structure
Each nephron consists of a renal corpuscle and a renal tubule.
Renal corpuscle: Glomerular capillaries (glomerulus) and glomerular capsule.
Renal tubule: Proximal convoluted tubule (PCT), nephron loop, distal convoluted tubule (DCT).
Collecting system: Connecting tubules, collecting duct, papillary duct.
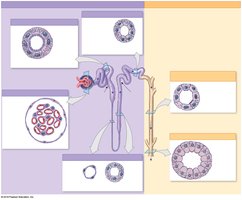
Types of Nephrons
There are two main types:
Cortical nephrons: 85% of nephrons; mostly in cortex; short nephron loop.
Juxtamedullary nephrons: 15% of nephrons; near cortex-medulla border; long nephron loop.
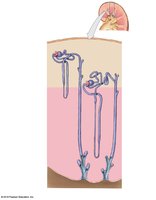
Main Functions of the Nephron
Reabsorbs useful organic material and ions from filtrate.
Reabsorbs more than 99% of water from filtrate.
Enhances elimination of wastes by actively secreting them into filtrate.
The Renal Corpuscle
The renal corpuscle consists of the glomerular capsule (Bowman's capsule) and glomerular capillaries. The capsule has a parietal (outer) layer and a visceral layer (podocytes).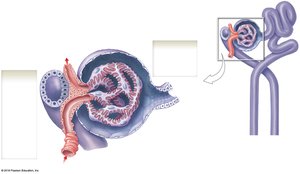
Filtration Barriers
Filtration involves five barriers:
Endothelial surface layer
Glomerular capillary endothelium (fenestrated)
Basement membrane
Glomerular epithelium (podocytes with filtration slits)
Subpodocyte space
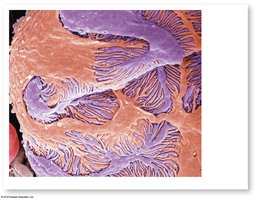
Filtrate Composition
Filtrate consists of water, ions, and small organic molecules (glucose, fatty acids, amino acids, vitamins), with very few plasma proteins. Many substances are reabsorbed in the nephron tubule.
Proximal Convoluted Tubule (PCT)
The PCT is lined with simple cuboidal epithelium containing microvilli. It reabsorbs organic nutrients, plasma protein, 60% of sodium and chloride ions, water, and other ions (calcium, potassium, phosphate, bicarbonate).
Nephron Loop
Descending limb: Water leaves and enters bloodstream, preventing dehydration.
Ascending limb: Pumps sodium and chloride ions out; impermeable to water.
Both limbs are lined with simple squamous epithelium.
Vasa recta are capillaries surrounding the nephron loop.
Distal Convoluted Tubule (DCT)
Active, regulated secretion of ions and acids.
Selective reabsorption of sodium and calcium ions.
Reabsorption of water.
Juxtaglomerular Complex
Located at the vascular pole, it consists of macula densa cells, juxtaglomerular cells, and extraglomerular mesangial cells. It produces renin (regulates blood pressure) and erythropoietin (stimulates erythrocyte production).
Collecting System
Consists of connecting tubules, collecting ducts, and papillary ducts.
Final adjustments to urine concentration are made in the collecting ducts.
Epithelium transitions from simple cuboidal to simple columnar.
Urine Transport, Storage, and Elimination
The Ureters
Ureters exit the kidney at the hilum, extend to the urinary bladder, and enter the bladder in the trigone area. Peristaltic contractions and gravity move urine.
Histology of the Ureters
Each ureter has three layers:
Inner mucosa (transitional epithelium)
Middle muscular layer (longitudinal and circular smooth muscle)
Adventitia (continuous with fibrous capsule and parietal peritoneum)
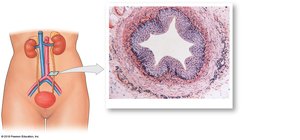
The Urinary Bladder
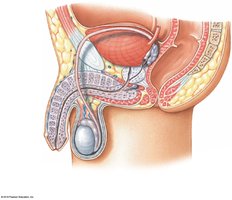
Males: Base is between rectum and symphysis pubis.
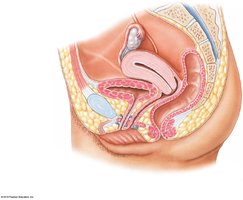
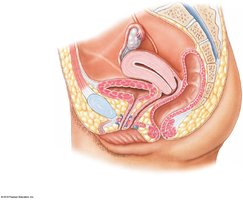
Females: Base is inferior to uterus and anterior to vagina.
Peritoneal folds (median and lateral umbilical ligaments) maintain position.
Histology of the Urinary Bladder
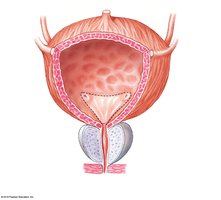
Mucosa has rugae to increase volume; lined by transitional epithelium.
Trigone region funnels urine to urethra.
Detrusor muscle forms the smooth muscle layer.
Neck of bladder surrounds entrance to urethra; internal urethral sphincter (involuntary control).
The Urethra
Female: 3–5 cm; external orifice near anterior vaginal wall; transitional epithelium at neck, stratified squamous elsewhere.
Male: 18–20 cm; subdivided into prostatic, membranous, and spongy urethra; complex histology (transitional, pseudostratified columnar, stratified columnar, stratified squamous).
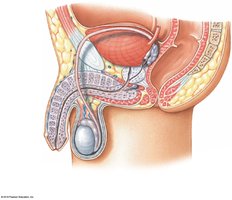
Urethral Sphincters
Internal urethral sphincter: Smooth muscle, involuntary control.
External urethral sphincter: Skeletal muscle, voluntary control; learned in infancy, lost with age or spinal injury.
Urinary Reflexes
Urine Storage Reflex
Increases sympathetic activity, inhibits detrusor muscle, and stimulates contraction of internal and external urethral sphincters.
Urine Voiding Reflex
First urge at ~200 ml bladder volume; stretch-activated spinal reflexes stimulate parasympathetic activity, detrusor contracts, internal sphincter relaxes. Voluntary effort is needed to relax external sphincter.
Upon complete void, ~10 ml urine remains.
When bladder nears capacity, both sphincters open based on pressure.
Aging and the Urinary System
Age-Related Changes
Number of functional nephrons decreases (30–40% decline from age 25 to 85).
Glomerular filtration rate declines.
Reduced sensitivity to antidiuretic hormone (ADH) causes frequent urination.
Urethral sphincters lose muscle tone, leading to incontinence.
Urinary retention increases risk of infection.
Enlarged prostate reduces urine flow in males.
