 Back
BackUrinary System: Structure, Function, and Physiology
Study Guide - Smart Notes

Urinary System Overview
Major Organs and Functions
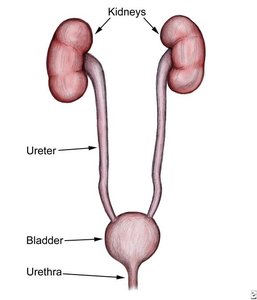
The urinary system is essential for maintaining the body's internal environment by regulating water, solute concentrations, and removing metabolic wastes. The main organs include the kidneys, ureters, urinary bladder, and urethra.
Kidneys: Major excretory organs; regulate water volume, solute concentration, ion balance, acid-base balance, and excrete wastes.
Ureters: Transport urine from kidneys to bladder.
Urinary bladder: Temporary storage for urine.
Urethra: Transports urine out of the body.
Kidney Structure and Internal Anatomy
Regions of the Kidney
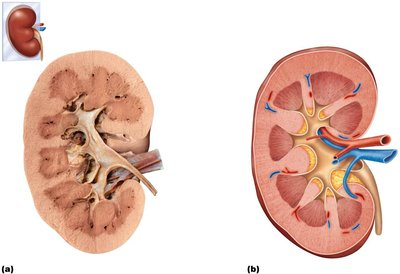
The kidney is divided into several distinct regions, each with specialized functions:
Renal cortex: Outer region containing most nephrons.
Renal medulla: Inner region with renal pyramids and columns.
Renal pelvis: Funnel-shaped tube that collects urine and channels it to the ureter.
Major and minor calyces: Collect urine from pyramids and pass it to the renal pelvis.
Nephrons: The Functional Units
Types of Nephrons
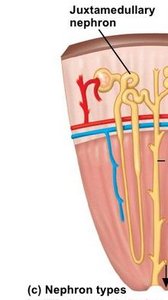
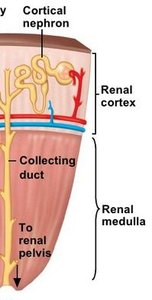
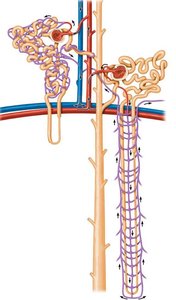
Nephrons are the structural and functional units of the kidney, responsible for urine formation. There are two main types:
Cortical nephrons: Located mostly in the cortex; make up ~85% of nephrons; involved in standard urine formation.
Juxtamedullary nephrons: Extend deep into the medulla; essential for producing concentrated urine.
Nephron Structure
Renal corpuscle: Composed of the glomerulus (a tuft of capillaries) and Bowman's (glomerular) capsule (surrounds the glomerulus).
Renal tubule: Includes the proximal convoluted tubule (PCT), nephron loop (loop of Henle), and distal convoluted tubule (DCT).
Collecting duct: Receives filtrate from multiple nephrons and channels it toward the renal pelvis.
Urine Formation: Three Key Processes
1. Glomerular Filtration
Filtration occurs in the renal corpuscle, where blood pressure forces water and solutes from the glomerulus into the glomerular capsule, forming a protein-free filtrate.
Filtration membrane: Consists of three layers—fenestrated endothelium, basement membrane, and podocyte foot processes with filtration slits.
Filtrate: Contains water, glucose, amino acids, and nitrogenous wastes; excludes large proteins and cells.
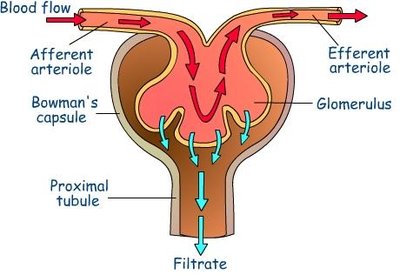

Filtration Pressures
Filtration is driven by hydrostatic pressure in the glomerular capillaries (HPgc), opposed by hydrostatic pressure in the capsule (HPcs) and colloid osmotic pressure (OPgc):
Net Filtration Pressure (NFP):
Typical values: mm Hg, mm Hg, mm Hg, so mm Hg

2. Tubular Reabsorption
Most filtrate is reabsorbed from the renal tubules back into the blood. This process is highly selective and involves both active and passive mechanisms.
Proximal convoluted tubule (PCT): Site of most reabsorption (all nutrients, 65% of Na+ and water).
Nephron loop: Descending limb reabsorbs water; ascending limb reabsorbs Na+ and Cl–.
DCT and collecting duct: Reabsorption is hormonally regulated (ADH, aldosterone, atrial natriuretic peptide, parathyroid hormone).
3. Tubular Secretion
Selected substances are moved from the blood into the filtrate, primarily in the PCT. This process helps eliminate drugs, excess ions, and maintain acid-base balance.
Secreted substances: K+, H+, NH4+, creatinine, and certain drugs.
Functions: Disposes of bound substances, eliminates undesirable substances, rids excess K+, and controls blood pH.
Regulation of Urine Concentration and Volume
Countercurrent Mechanisms
The kidneys use countercurrent mechanisms to maintain a medullary osmotic gradient, allowing for the production of concentrated or dilute urine.
Countercurrent multiplier: Nephron loop creates the gradient by differing permeabilities to water and solutes in descending and ascending limbs.
Countercurrent exchanger: Vasa recta preserve the gradient by exchanging water and solutes with the interstitial fluid.
Hormonal Regulation
Antidiuretic hormone (ADH): Increases water reabsorption in collecting ducts by inserting aquaporins.
Aldosterone: Promotes Na+ (and water) reabsorption in DCT and collecting ducts.
Atrial natriuretic peptide (ANP): Reduces Na+ reabsorption, lowering blood volume and pressure.
Parathyroid hormone (PTH): Increases Ca2+ reabsorption in DCT.
Urine Composition and Characteristics
Chemical Composition
95% water, 5% solutes
Nitrogenous wastes: Urea (from amino acid breakdown), uric acid (from nucleic acids), creatinine (from muscle metabolism)
Other solutes: Na+, K+, PO43–, SO42–, Ca2+, Mg2+, HCO3–

Physical Characteristics
Color: Pale to deep yellow (urochrome pigment); abnormal colors may indicate disease or diet effects.
Odor: Slightly aromatic; may change with disease or diet.
pH: Slightly acidic (pH ~6); varies with diet and health.
Specific gravity: 1.001–1.035 (compared to water at 1.000).
Transport, Storage, and Elimination of Urine
Ureters
Slender tubes that convey urine from the kidneys to the bladder. They enter the bladder at an angle to prevent backflow.
Urinary Bladder
A muscular sac for temporary urine storage. It can hold about 500 mL when moderately full but can expand to hold more if necessary.
Urethra
A muscular tube that drains urine from the bladder to the outside of the body. In males, it is longer and divided into prostatic, intermediate, and spongy regions.
Micturition (Urination)
The process of urination involves three simultaneous events:
Contraction of the detrusor muscle (autonomic nervous system)
Opening of the internal urethral sphincter (autonomic nervous system)
Opening of the external urethral sphincter (somatic nervous system)
Clinical Considerations
Renal Calculi (Kidney Stones)
Crystallized calcium, magnesium, or uric acid salts that may block the ureter, causing pain and urinary obstruction.
Treatment includes increased water intake, pain management, shock wave lithotripsy, or surgery.
Urinary Tract Infections (UTIs)
Urethritis: Inflammation of the urethra
Cystitis: Inflammation of the bladder
Pyelitis/Pyelonephritis: Inflammation of the kidneys
Symptoms: Painful urination, urgency, fever, cloudy or blood-tinged urine
Treatment: Antibiotics
Renal Failure
Defined as GFR < 15 ml/min
Leads to uremia, metabolic imbalances, and requires dialysis or transplant
Age-Related Changes
Kidneys shrink, nephrons decrease in number and size, GFR declines
Increased risk of nocturia and incontinence due to bladder changes
Summary Table: Reabsorption Capabilities of Renal Tubule Segments
Segment | Main Substances Reabsorbed | Regulation |
|---|---|---|
Proximal Convoluted Tubule (PCT) | All nutrients (glucose, amino acids), 65% Na+ and water, many ions, uric acid, half urea | Unregulated (bulk reabsorption) |
Nephron Loop (Descending Limb) | Water | Passive, not regulated |
Nephron Loop (Ascending Limb) | Na+, Cl– | Active and passive, not regulated |
Distal Convoluted Tubule (DCT) & Collecting Duct | Na+ (aldosterone), water (ADH), Ca2+ (PTH), K+ (secretion), H+ | Hormonally regulated |
