 Back
BackUrinary System: Structure, Function, and Regulation
Study Guide - Smart Notes

The Urinary System
Introduction and Functions
The urinary system is essential for maintaining the body's internal environment by regulating water, solute concentrations, and removing metabolic wastes. It consists of the kidneys, ureters, urinary bladder, and urethra.
Regulation of water and solute balance: Kidneys control total body water volume and solute concentration.
Ion regulation: Maintains ion concentrations in extracellular fluid (ECF).
Acid-base balance: Ensures long-term acid-base equilibrium.
Excretion: Removes metabolic wastes, toxins, and drugs.
Hormone production: Produces erythropoietin (regulates RBC production) and renin (involved in blood pressure regulation).
Vitamin D activation: Converts vitamin D to its active form (calcitriol).
Gluconeogenesis: Assists the liver during prolonged fasting.
Components of the Urinary System
Kidneys: Filter blood and form urine.
Ureters: Transport urine from kidneys to bladder.
Urinary bladder: Temporary storage for urine.
Urethra: Conducts urine out of the body.
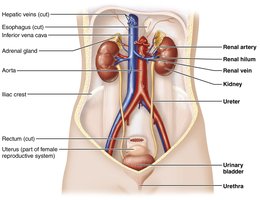
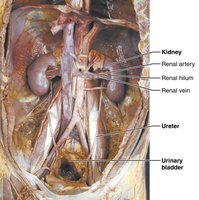
Kidney Structure and Blood Supply
Location and External Anatomy
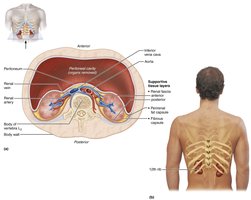
The kidneys are retroperitoneal, bean-shaped organs located in the superior lumbar region. The right kidney is slightly lower due to the liver. Each kidney is protected by the rib cage and surrounded by three supportive tissue layers:
Renal fascia: Anchoring outer layer of dense connective tissue.
Perirenal fat capsule: Fatty cushion for protection.
Fibrous capsule: Transparent capsule preventing infection spread.
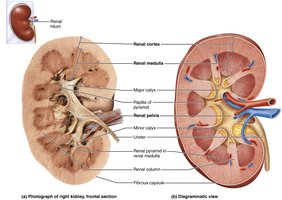
Internal Gross Anatomy
Each kidney has three distinct internal regions:
Renal cortex: Superficial, light-colored region.
Renal medulla: Deep, darker region with cone-shaped pyramids.
Renal pelvis: Funnel-shaped tube continuous with the ureter, collects urine from calyces.
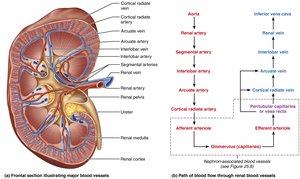
Blood and Nerve Supply
The kidneys receive about one-fourth of the cardiac output each minute. Blood flows through a series of arteries and veins, and the cortex receives most of the blood. Sympathetic fibers regulate blood flow and urine formation.
Nephrons: Functional Units of the Kidney
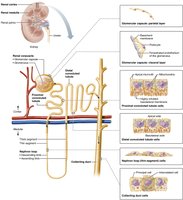
Structure of Nephrons
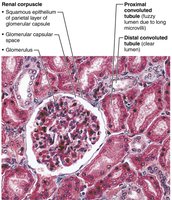
Nephrons are the structural and functional units that filter blood and form urine. Each nephron consists of a renal corpuscle and a renal tubule, and empties into collecting ducts.
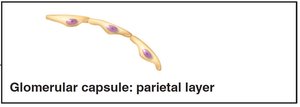
Renal corpuscle: Includes the glomerulus (fenestrated capillaries) and glomerular capsule (Bowman's capsule).
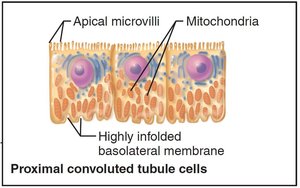
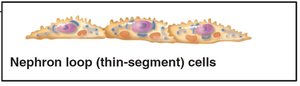
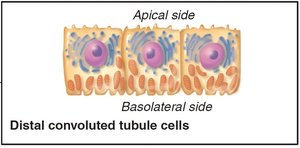
Renal tubule: Composed of proximal convoluted tubule (PCT), nephron loop, and distal convoluted tubule (DCT).
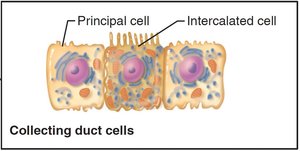
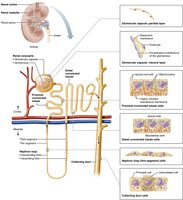
Classes of Nephrons
Cortical nephrons: 85% of nephrons, mostly in cortex, short loops.
Juxtamedullary nephrons: Located near cortex-medulla junction, long loops essential for concentrated urine.
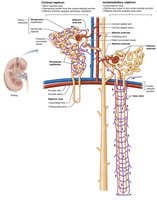
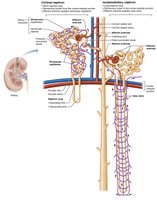
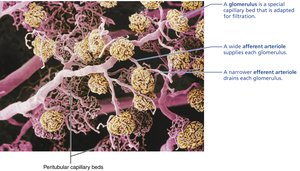
Nephron Capillary Beds
Glomerulus: Specialized for filtration, fed and drained by arterioles.
Peritubular capillaries: Surround tubules, pick up reabsorbed substances.
Vasa recta: Long vessels parallel to nephron loops, involved in urine concentration.
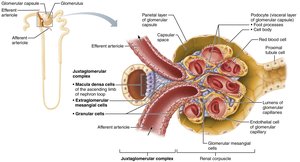
Juxtaglomerular Complex (JGC)
The JGC regulates filtrate formation and blood pressure. It consists of macula densa (chemoreceptors), granular cells (mechanoreceptors, secrete renin), and extraglomerular mesangial cells (signal transmission).
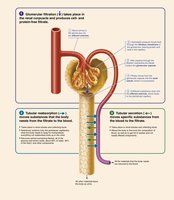
Urine Formation: Filtration, Reabsorption, and Secretion
Overview of Renal Processes
Three major processes are involved in urine formation:
Glomerular filtration: Passive process, hydrostatic pressure forces fluids and solutes through the filtration membrane.
Tubular reabsorption: Selective process reclaiming substances from filtrate into blood.
Tubular secretion: Moves substances from blood into filtrate.

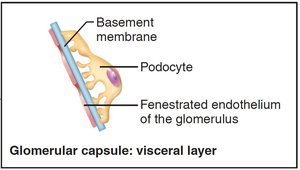
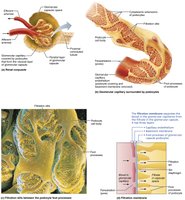
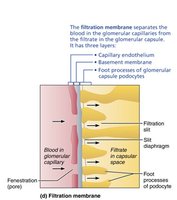
Filtration Membrane
The filtration membrane consists of three layers: fenestrated endothelium, basement membrane, and podocyte foot processes. It allows passage of water and small solutes, but excludes blood cells and most proteins.
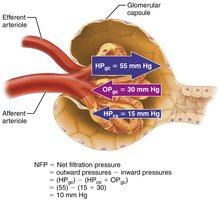
Pressures Affecting Filtration
Outward pressure: Hydrostatic pressure in glomerular capillaries (HPgc) promotes filtration.
Inward pressure: Hydrostatic pressure in capsular space (HPcs) and colloid osmotic pressure (OPgc) inhibit filtration.
Net Filtration Pressure (NFP):
Glomerular Filtration Rate (GFR)
GFR: Volume of filtrate formed per minute by both kidneys.
Factors affecting GFR: NFP, surface area, membrane permeability.
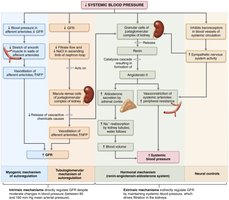
Regulation of Glomerular Filtration
GFR is regulated by intrinsic (renal autoregulation) and extrinsic (neural and hormonal) mechanisms. Intrinsic controls include myogenic and tubuloglomerular feedback. Extrinsic controls involve sympathetic nervous system and renin-angiotensin-aldosterone mechanism.
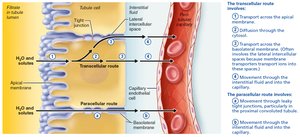
Tubular Reabsorption and Secretion
Tubular Reabsorption
Reabsorption occurs via transcellular and paracellular routes, using active and passive transport. Most nutrients, water, and ions are reabsorbed, with water reabsorption regulated by ADH.
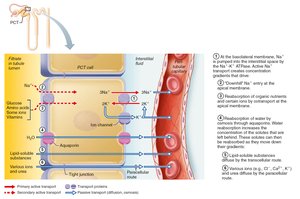
Transport Maximum
Transport maximum (Tm): Maximum rate at which a substance can be reabsorbed, determined by number of transport proteins.
Clinical relevance: Hyperglycemia can exceed Tm, causing glucose in urine.
Reabsorptive Capabilities of Renal Tubules and Collecting Ducts
Different segments of the nephron have distinct reabsorptive functions, regulated by hormones such as ADH, aldosterone, atrial natriuretic peptide, and parathyroid hormone.
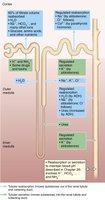
Tubule Segment | Substance Reabsorbed | Mechanism |
|---|---|---|
Proximal Convoluted Tubule (PCT) | Sodium ions (Na+), glucose, amino acids, water, ions | Primary active transport, secondary active transport, osmosis |
Nephron Loop | Water (descending), Na+, Cl-, K+ (ascending) | Passive diffusion (descending), active transport (ascending) |
Distal Convoluted Tubule (DCT) & Collecting Duct | Na+, Cl-, water, urea | Hormone-regulated active and passive transport |

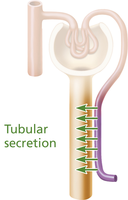
Tubular Secretion
Tubular secretion moves substances from blood into filtrate, important for disposing drugs, eliminating reabsorbed wastes, controlling potassium and pH.
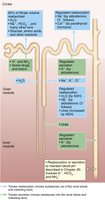
Regulation of Urine Concentration and Volume
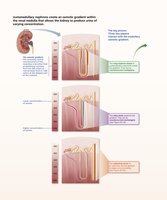
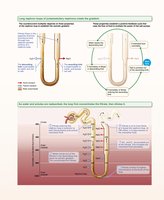
Osmotic Gradient and Countercurrent Mechanisms
The kidneys use countercurrent mechanisms to regulate urine concentration and volume, maintaining a medullary osmotic gradient from cortex to medulla. The countercurrent multiplier (nephron loop) creates the gradient, and the countercurrent exchanger (vasa recta) preserves it.


Renal Clearance
Definition and Clinical Application
Renal clearance is the volume of plasma cleared of a substance per unit time. It is used to assess kidney function and GFR. The formula is:
Where U = concentration in urine, V = urine flow rate, P = concentration in plasma.
Urine: Composition and Characteristics
Chemical Composition
95% water, 5% solutes (urea, uric acid, creatinine, ions).
Abnormal constituents (proteins, WBCs, bile pigments) may indicate pathology.
Physical Characteristics
Color: Pale to deep yellow (urobilin/urochrome).
Odor: Slightly aromatic, ammonia upon standing.
pH: Slightly acidic (4.5–8.0).
Specific gravity: 1.001–1.035.
Ureters, Urinary Bladder, and Urethra
Ureters
Transport urine from kidneys to bladder via peristaltic contractions.
Three layers: mucosa (transitional epithelium), muscularis (smooth muscle), adventitia (connective tissue).
Urinary Bladder
Muscular sac for temporary urine storage.
Three layers: mucosa, detrusor muscle, adventitia.
Trigone: triangular area prone to infection.
Urethra
Transports urine out of the body.
Epithelium varies along its length.
Internal (involuntary) and external (voluntary) sphincters control flow.
Micturition (Urination)
Requires contraction of detrusor, opening of internal and external sphincters.
Controlled by autonomic and somatic nervous systems.
Pontine centers in the brain mature in early childhood, allowing voluntary control.
Clinical Correlations
Homeostatic Imbalances
Pyelonephritis: Kidney infection, often from fecal bacteria.
Renal calculi: Kidney stones, can cause pain and obstruction.
Chronic renal disease: GFR < 60 mL/min for 3+ months, seen in diabetes and hypertension.
Renal failure: GFR < 15 mL/min, leads to uremia and requires dialysis or transplant.
Anuria: Abnormally low urine output, may indicate renal failure.
Summary Table: Reabsorption Capabilities
Segment | Substances Reabsorbed | Mechanism |
|---|---|---|
PCT | Na+, glucose, amino acids, water, ions | Active and passive transport |
Nephron Loop | Water (descending), Na+, Cl-, K+ (ascending) | Passive (descending), active (ascending) |
DCT & Collecting Duct | Na+, Cl-, water, urea | Hormone-regulated |
Key Equations
Net Filtration Pressure:
Renal Clearance:
Additional info: These notes expand on the original slides with definitions, examples, and clinical context for clarity and completeness.
