 Back
BackUrinary System: Structure, Function, and Renal Physiology
Study Guide - Smart Notes

Overview of the Urinary System
Organs of the Urinary System
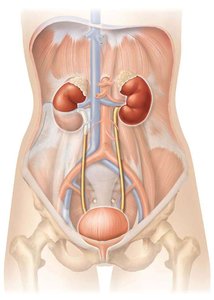
The urinary system is responsible for filtering blood, removing waste, and regulating fluid and electrolyte balance. It consists of the kidneys, ureters, urinary bladder, and urethra.
Kidneys: Filter blood, produce urine, and regulate various aspects of blood chemistry.
Ureters: Transport urine from the kidneys to the bladder.
Urinary Bladder: Stores urine until excretion.
Urethra: Conducts urine from the bladder to the exterior of the body.
Major Functions of the Kidneys
Filter 180–200 L of blood daily
Produce hormones (e.g., erythropoietin, renin)
Regulate blood ionic composition, pH, volume, pressure, and osmolarity
Assist in blood glucose regulation
Excrete metabolic wastes (e.g., urea, creatinine)
Anatomy of the Kidneys
External Structure of the Kidney
The kidneys are retroperitoneal organs located in the abdominopelvic cavity, partially protected by the 11th and 12th ribs. The medial border is concave, forming the renal hilum, which serves as the entry and exit point for the ureter, blood vessels, lymphatics, and nerves.
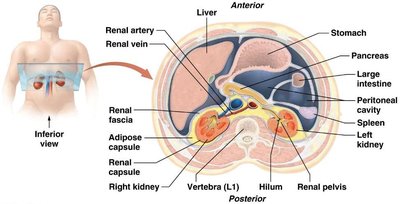
Support Structures: Renal fascia, adipose capsule, and renal capsule provide protection and anchorage.
Coverings: The renal capsule is a tough fibrous layer surrounding the kidney.
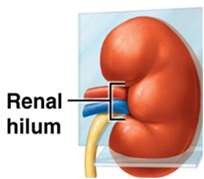
Internal Structure of the Kidney
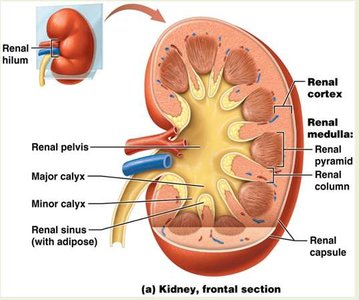
The functional portion of the kidney consists of the renal cortex and renal pyramids (medulla), which house the nephrons. Urine drains from the nephrons through a series of ducts and calyces to the renal pelvis and then to the ureter.
Renal Cortex: Outer region containing glomeruli and convoluted tubules.
Renal Medulla: Inner region with renal pyramids and columns.
Renal Pelvis: Funnel-shaped structure collecting urine from major calyces.
Major/Minor Calyces: Collect urine from papillary ducts.
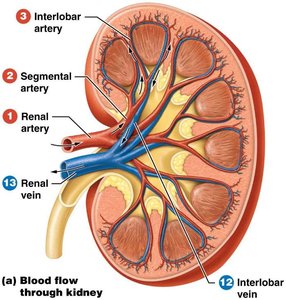
Blood Supply of the Kidneys
The kidneys receive 20–25% of resting cardiac output. Blood enters via the renal artery and exits via the renal vein. The renal portal system filters blood through two capillary beds: the glomerular capillaries and the peritubular capillaries.
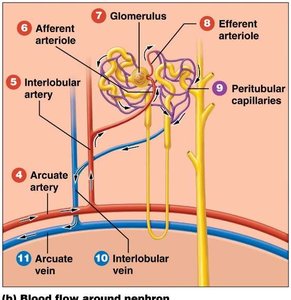
Nephron Structure and Types
The nephron is the functional unit of the kidney, responsible for filtering blood and forming urine. Each nephron consists of a renal corpuscle and a renal tubule.
Renal Corpuscle: Composed of the glomerular capsule and glomerulus (first capillary bed).
Renal Tubule: Includes the proximal tubule, nephron loop (descending and ascending limbs), and distal tubule.
Collecting Duct: Receives filtrate from multiple nephrons.
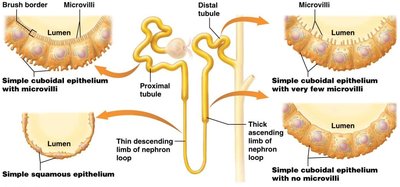
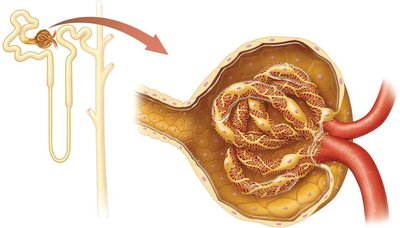
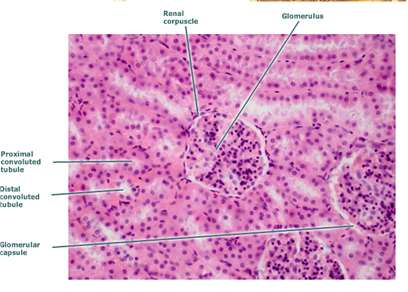
Cortical vs. Juxtamedullary Nephrons
Cortical Nephrons (80%): Glomerulus in outer cortex, short nephron loop.
Juxtamedullary Nephrons (20%): Glomerulus in inner cortex, long nephron loop extending deep into the medulla; essential for concentrating urine.
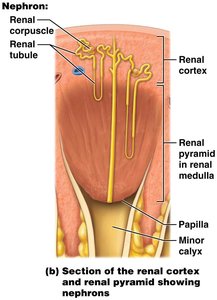
Renal Physiology: Urine Formation
Major Processes in Urine Formation
Urine formation involves three main processes, each occurring in specific regions of the nephron and collecting system:
Filtration: Occurs in the glomerulus; about 20% of plasma is filtered from the glomerular capillaries into the capsular space.
Reabsorption: 99% of water and useful solutes are returned to the blood from the filtrate, mainly in the proximal tubule and nephron loop.
Secretion: Additional waste products are actively transported from the blood into the filtrate, primarily in the distal tubule and collecting duct.
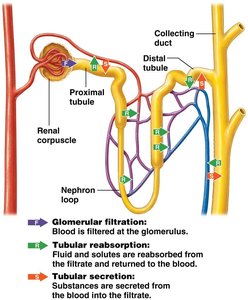
Glomerular Filtration
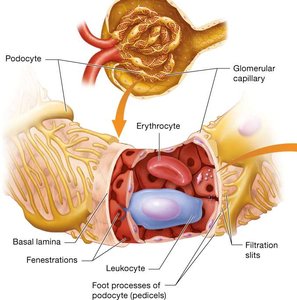
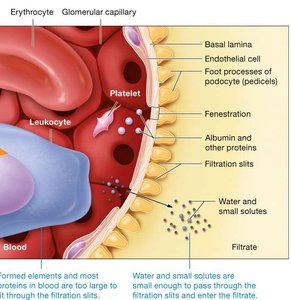
The filtration membrane consists of three barriers: glomerular endothelial cells, the basement membrane, and filtration slits between podocytes. This membrane allows water and small solutes to pass while preventing plasma proteins, blood cells, and platelets from entering the filtrate.
Glomerular Filtration Rate (GFR): The amount of filtrate formed per minute by both kidneys; average value is about 125 mL/min.
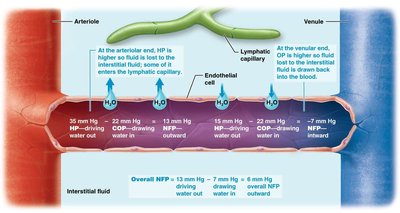
Net Filtration Pressure (NFP): Determined by the balance of hydrostatic and colloid osmotic pressures:
GHP: Glomerular hydrostatic pressure
CHP: Capsular hydrostatic pressure
GCOP: Glomerular colloid osmotic pressure
Regulation of Glomerular Filtration Rate (GFR)
GFR is regulated by three mechanisms:
Autoregulation: Myogenic mechanism and tubuloglomerular feedback (macula densa)
Neural Control: Sympathetic nervous system activity
Hormonal Regulation: Renin-angiotensin-aldosterone system (RAAS), atrial natriuretic peptide (ANP)
Tubular Reabsorption and Secretion
Mechanisms of Reabsorption and Secretion
Reabsorption returns most filtered water and solutes to the bloodstream via passive (diffusion, osmosis) and active (ATP-dependent) transport. Secretion moves substances from blood to tubular fluid, primarily by active transport.
Transcellular Route: Through the cells
Paracellular Route: Between cells
Active vs. Passive Transport
Active Transport: Requires ATP to move molecules against concentration gradients (e.g., Na+/K+ pump).
Passive Transport: Does not require energy; includes facilitated diffusion and osmosis.
Symporters and Antiporters
Symporter: Moves two substances in the same direction (e.g., Na+/glucose symporter).
Antiporter: Moves substances in opposite directions (e.g., Na+/H+ exchanger).
Reabsorption in Nephron Segments
Proximal Tubule (PT): Most active segment; reabsorbs 100% of glucose and amino acids, ~65% of water, Na+, K+, Ca++, Cl-, Mg++, and ~90% of HCO3-.
Nephron Loop (Loop of Henle): Descending limb reabsorbs water; ascending limb reabsorbs Na+ and Cl- but is impermeable to water.
Distal Tubule (DT) & Collecting Duct: Early DT reabsorbs Na+ and Cl-, secretes K+ and H+; late DT and collecting duct adjust reabsorption and secretion based on body needs (facultative reabsorption).
Hormonal Regulation of Water Reabsorption
Renin-Angiotensin-Aldosterone System (RAAS): Increases blood volume and pressure by increasing water reabsorption in the collecting duct.
Antidiuretic Hormone (ADH): Increases water reabsorption by increasing collecting duct permeability.
Atrial Natriuretic Peptide (ANP): Decreases water and electrolyte reabsorption.
Regulation of Urine Concentration and Volume
Dilute vs. Concentrated Urine
The kidneys adjust urine concentration based on hydration status and hormonal signals, primarily ADH. The nephron loop and vasa recta establish a medullary osmotic gradient, enabling the production of concentrated urine via the countercurrent mechanism.
Dilute Urine: ADH not secreted; more solutes reabsorbed than water, resulting in water excretion.
Concentrated Urine: ADH secreted; 99% of water reabsorbed, increasing urine solute concentration.
Urine and Renal Clearance
Physical and Chemical Properties of Urine
Normal Volume: 1–2 L/day
pH: 4.6–8
Color: Yellow to amber
Turbidity: Transparent
Odor: Mild, not sweet or ammonia-like
Specific Gravity: 1.001–1.035
Blood tests for kidney function include blood urea nitrogen (BUN) and plasma creatinine levels. Renal clearance measures the effectiveness of the kidneys at removing substances from plasma.
Urine Transport, Storage, and Elimination
Ureters, Urinary Bladder, and Urethra
Ureters: Connect renal pelvis to bladder; urine moves via peristalsis and gravity.
Urinary Bladder: Muscular organ posterior to pubic symphysis; stores urine until micturition.
Urethra: Drains urine from bladder to exterior; shorter in females, also serves as ejaculation duct in males.
Micturition Reflex
Stretch receptors in the bladder wall are stimulated as volume increases (200–400 mL), sending impulses to the spinal cord (S2–S3). The detrusor muscle contracts, and the internal urethral sphincter relaxes. Voluntary control requires relaxation of the external urethral sphincter.
Comparison of Male and Female Urinary Tracts
Female Urethra: Shorter (~4 cm), exclusive passage for urine.
Male Urethra: Longer, also serves as the duct for ejaculation (receives sperm and fluids from accessory glands).
