 Back
BackVascular System: Structure, Flow, and Blood Pressure
Study Guide - Smart Notes

Vascular System Overview
Lecture Outline
This lecture covers the anatomy of blood vessels, the principles of blood flow through the vascular system, and the regulation and measurement of blood pressure. Understanding these topics is essential for grasping cardiovascular physiology and the mechanisms that ensure efficient circulation throughout the body.

Cardiovascular System Structure
Major Vessel Types and Circuits
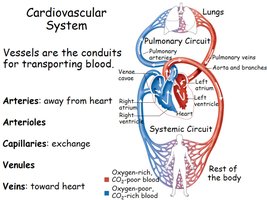
The cardiovascular system consists of a closed network of vessels that transport blood throughout the body. The heart acts as the pump, and vessels serve as conduits for blood flow. The system is divided into the pulmonary circuit (to and from the lungs) and the systemic circuit (to and from the rest of the body).
Arteries: Carry blood away from the heart.
Arterioles: Small branches of arteries leading to capillaries; regulate flow and pressure.
Capillaries: Sites of exchange between blood and tissues.
Venules: Collect blood from capillaries.
Veins: Return blood to the heart.
Vessel Anatomy
Generalized Structure of Arteries and Veins
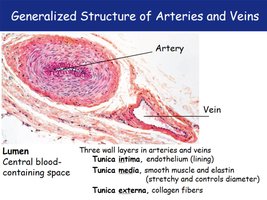
Both arteries and veins share a similar three-layered wall structure, but differ in thickness and composition to suit their functions.
Lumen: Central blood-containing space.
Tunica intima: Endothelial lining.
Tunica media: Smooth muscle and elastin; controls vessel diameter.
Tunica externa: Collagen fibers; provides structural support.
Vessel Composition
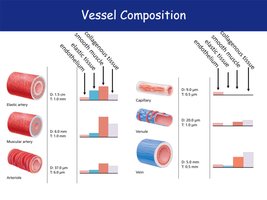
The composition of vessel walls varies by vessel type, reflecting their functional roles in the circulatory system.
Elastic arteries: Thick walls, abundant elastin for pressure buffering.
Muscular arteries: More smooth muscle for vasoconstriction.
Arterioles: Smallest arteries, primarily smooth muscle.
Capillaries: Only endothelium and basement membrane for exchange.
Venules and veins: Thinner walls, larger lumens, less smooth muscle, more collagen in large veins.
Arteries
Arteries are classified as elastic or muscular based on their structure and function.
Elastic arteries: Large, thick-walled, contain elastin in all layers, act as pressure reservoirs, and are inactive in vasoconstriction (e.g., aorta).
Muscular arteries: Distribute blood to organs, have more smooth muscle, and are active in vasoconstriction.

Arterioles
Arterioles are the smallest arteries and play a key role in regulating blood flow and pressure.
Contain smooth muscle to control flow into capillary beds and determine mean arterial pressure (MAP).
Vasodilation increases blood flow to regions; vasoconstriction decreases it.
No gas or nutrient exchange occurs in arterioles.

Capillaries
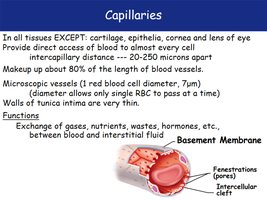
Capillaries are the primary sites for exchange between blood and tissues. They are present in almost all tissues except cartilage, epithelia, cornea, and lens of the eye.
Microscopic vessels (about 7 μm in diameter, just wide enough for a single red blood cell).
Walls consist of a thin endothelium and a basement membrane.
Allow exchange of gases, nutrients, wastes, and hormones.
Venules
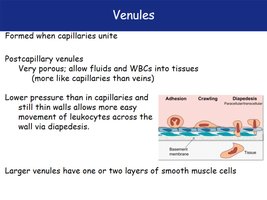
Venules are formed when capillaries unite. They are very porous, allowing fluids and white blood cells to move into tissues.
Lower pressure than capillaries; thin walls facilitate leukocyte movement (diapedesis).
Larger venules may have one or two layers of smooth muscle cells.
Veins
Veins are formed when venules converge. They have thinner walls and larger lumens compared to arteries, and serve as blood reservoirs.
Thin tunica media with smooth muscle (can constrict).
Thick tunica externa of collagen fibers.
Contain up to 60% of blood supply (capacitance vessels).
Blood pressure is lower than in arteries.

Venous Adaptations
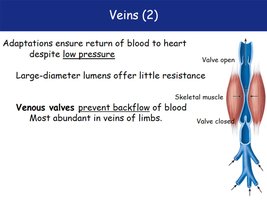
Veins have adaptations to ensure blood returns to the heart despite low pressure.
Large-diameter lumens offer little resistance.
Venous valves prevent backflow, especially in limbs.
Relative Blood Volume Distribution
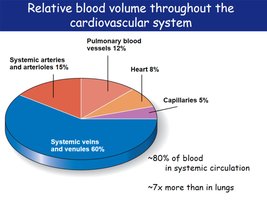
Blood volume is unevenly distributed throughout the cardiovascular system, with the majority in systemic veins and venules.
Systemic veins and venules: ~60%
Systemic arteries and arterioles: 15%
Pulmonary blood vessels: 12%
Heart: 8%
Capillaries: 5%
Flow Through Vessels
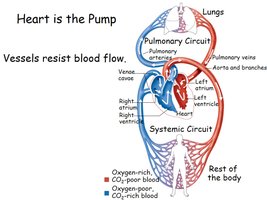
Heart as the Pump and Vascular Resistance
The heart generates the pressure that drives blood flow, but vessels resist this flow. The degree of resistance is determined by vessel properties and is crucial for regulating blood distribution.
Resistance in Blood Vessels
Resistance is the opposition to blood flow and is influenced by vessel length, blood viscosity, and vessel radius. The most significant factor is vessel radius.
Formula: where is resistance, is vessel length, is blood viscosity, and is vessel radius.
Resistance is inversely proportional to the fourth power of the radius.
Blood viscosity and vessel length are relatively constant; radius changes have the greatest effect.

Vessel Diameter and Resistance
Small changes in vessel diameter cause large changes in resistance. Arterioles are the primary regulators of peripheral resistance.
If radius doubles, resistance decreases to 1/16 of the original value.
If radius is halved, resistance increases 16-fold.
Fatty plaques (atherosclerosis) increase resistance.

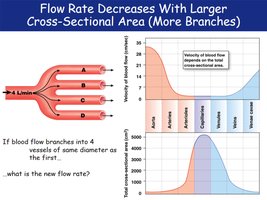
Flow Rate and Cross-Sectional Area
As blood flows through more branches (increased total cross-sectional area), the velocity of flow decreases. This is most pronounced in capillaries, allowing time for exchange.
Flow rate is inversely related to total cross-sectional area.
Blood Pressure
Blood Flow, Blood Pressure, and Resistance
Blood pressure is determined by the product of cardiac output and peripheral resistance. Blood flow is directly proportional to blood pressure and inversely proportional to resistance.
Blood Pressure (BP):
Blood Flow (BF):
Peripheral resistance is the most important factor for local blood flow regulation.

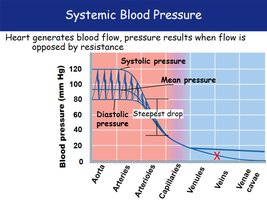
Systemic Blood Pressure
Blood pressure is highest in the aorta and decreases throughout the systemic circulation, with the steepest drop in arterioles. Pressure is nearly zero in the venae cavae.
Arterial Blood Pressure
Arterial blood pressure reflects the elasticity of arteries and the volume of blood forced into them. It is pulsatile near the heart.
Systolic pressure: Pressure during ventricular contraction (~120 mm Hg).
Diastolic pressure: Lowest aortic pressure during relaxation (~80 mm Hg).
Pulse pressure: Difference between systolic and diastolic pressure.
Arterial Blood Pressure Calculation
Mean arterial pressure (MAP) is the pressure that propels blood to tissues. It is calculated as:
Example: For BP 120/80, pulse pressure = 40 mm Hg, MAP = 80 + 1/3(40) = 93 mm Hg.
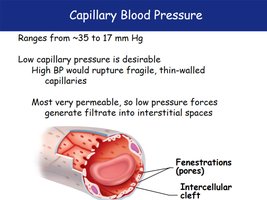
Capillary Blood Pressure
Capillary blood pressure is low (35–17 mm Hg) to prevent rupture of fragile capillaries and to allow exchange. High permeability allows fluid movement into interstitial spaces.
Venous Blood Pressure
Venous blood pressure is low (about 15 mm Hg) and changes little during the cardiac cycle. The low pressure is due to the cumulative effects of peripheral resistance.

