 Back
BackIntegumentary System: Structure, Function, and Common Diseases
Study Guide - Smart Notes

Dermatology and the Integumentary System
Definition and Scope
Dermatology is the medical specialty focused on the anatomy, physiology, and diseases of the integumentary system. The term is derived from the word parts dermat/o- (meaning skin) and -logy (meaning study of).

Dermatologists diagnose and treat skin, hair, and nail disorders using laboratory tests, medical and surgical procedures, and pharmacological therapies.
Structure of the Integumentary System
Main Components
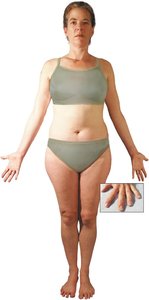
The integumentary system covers most of the body and consists of the skin, nails, and subcutaneous tissue. The skin is the largest organ in the body and is composed of two main layers: the epidermis (outermost layer) and the dermis (deeper layer). Beneath the dermis lies the subcutaneous tissue, which is primarily adipose tissue.
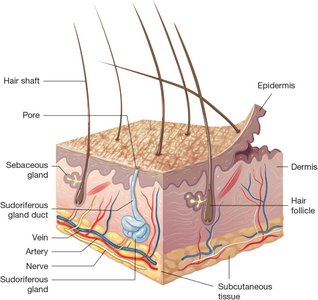
Word Parts Related to Skin
integument/o-: skin
cutane/o-: skin
-ary, -ous: pertaining to
Epidermis
The epidermis is the thin, outermost layer of the skin, made up of epithelial tissue. It consists of two main layers:
Squamous layer: Upper part, contains both living and dead cells. Surface cells are dead, filled with keratin, and form a protective, slightly acidic layer that discourages microorganism growth.
Basal layer: Deep part, made of living cells that constantly divide and move upward. The epidermis contains no blood vessels and relies on the dermis for nutrients.
The epidermis also contains melanocytes, which produce the pigment melanin to absorb UV light. All humans have the same number of melanocytes, but melanin production varies by skin tone and sun exposure.
Dermis
The dermis lies below the epidermis and is composed of connective tissue, including collagen (firm, white protein) and elastin (elastic, yellow protein). It contains blood vessels, nerves, hair follicles, sebaceous glands, and sweat glands.
Subcutaneous Tissue
The subcutaneous tissue (sub Q or subcu) is a layer of loose connective tissue beneath the dermis, composed mainly of adipose tissue. It cushions, insulates, and protects internal organs. The thickness varies with fat storage.
Functions of the Integumentary System
Protection
The skin acts as the first line of defense against injury and infection.
The acidic surface and keratinized cells prevent microorganism growth and water loss.
Sweat and sebum contain antibodies and enzymes that kill bacteria.
Repair
Basal epidermal cells migrate to cover wounds.
Deep wounds form blood clots and scabs; new cells fill in the wound.
Sensation
Sensory receptors in the dermis detect touch, pressure, vibration, pain, and temperature.
Signals are transmitted to the spinal cord and brain for interpretation.
Vitamin D Synthesis
UV rays convert epidermal cholesterol into vitamin D, which is essential for calcium absorption and bone health.
Sun exposure requirements vary by skin tone.
Thermoregulation
Subcutaneous fat conserves heat; piloerector muscles contract to generate heat (goosebumps).
Sweat glands cool the body; dermal blood vessels dilate to release heat.
Homeostasis
The integumentary system helps maintain internal balance and stability (homeostasis), especially through thermoregulation.
Common Integumentary Diseases and Conditions
General Terms
Dermatitis: Inflammation or infection of the skin.
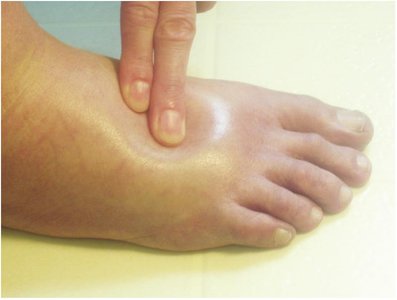
Edema: Swelling due to fluid accumulation in the dermis or subcutaneous tissue.
Hemorrhage: Bleeding into the skin from injured blood vessels.
Lesion: Any observable damage or abnormality of the skin.
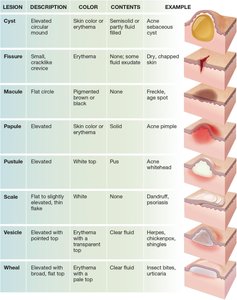
Types of Skin Lesions
Lesion | Description | Color | Contents | Example |
|---|---|---|---|---|
Cyst | Elevated, circular mound | Skin color or erythema | Semisolid or partly fluid-filled | Acne sebaceous cyst |
Fissure | Small, cracklike crevice | Erythema | Dry, chapped skin | Dry, chapped skin |
Macule | Flat circle | Pigmented brown or black | None | Freckle, age spot |
Papule | Elevated | Skin color or erythema | Solid | Acne pimple |
Pustule | Elevated | White top | Pus | Acne whitehead |
Scale | Flat to slightly elevated, thin flake | White | None | Dandruff, psoriasis |
Vesicle | Elevated with pointed top | Erythema with transparent top | Clear fluid | Herpes, chickenpox |
Wheal | Elevated with broad, flat top | Pale top, erythema around edge | Clear fluid | Insect bites, urticaria |
Skin Color Conditions
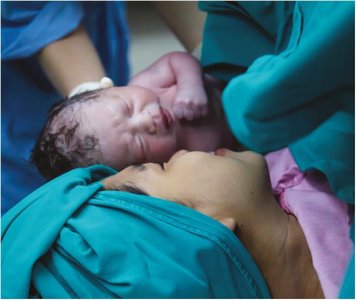
Albinism: Genetic lack of pigment in skin, hair, and eyes.
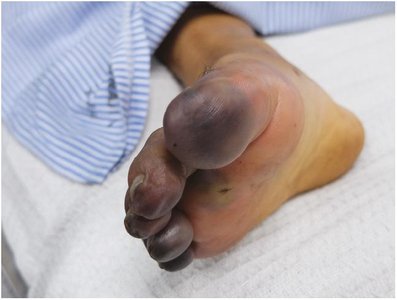
Cyanosis: Bluish-purple discoloration due to low oxygen.
Erythema: Red discoloration, local or widespread.
Jaundice: Yellowish discoloration from bilirubin buildup.
Necrosis: Gray-to-black discoloration from tissue death.
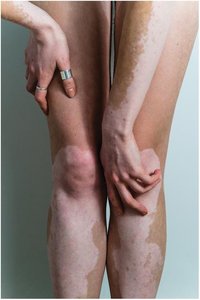
Vitiligo: Autoimmune destruction of melanocytes, causing white patches.


Skin Injuries
Abrasion: Scraping injury removing the epidermis.
Blister: Fluid-filled sac from repetitive rubbing.
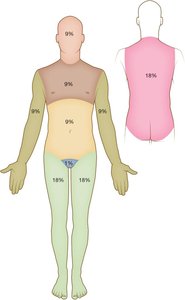
Burns: Damage from heat, chemicals, or radiation. Classified as superficial (first-degree), partial-thickness (second-degree), or full-thickness (third-degree).
Callus: Thickened pad from repetitive rubbing.
Cicatrix: Scar tissue formed during healing.
Excoriation: Linear scratch from a sharp object.
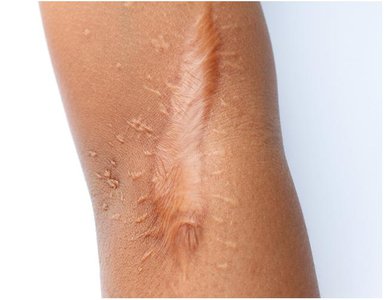
Keloid: Abnormally large, firm scar from excess collagen.
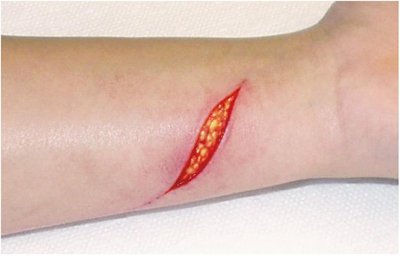
Laceration: Linear wound with clean or ragged edges.
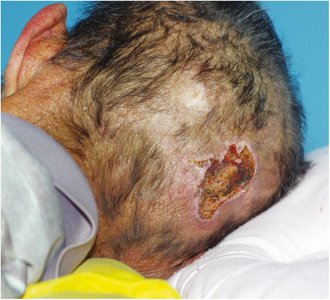
Pressure injury: Ulcer from prolonged pressure.
Skin Infections
Abscess: Localized pus pocket from bacterial infection.
Cellulitis: Spreading infection of skin and subcutaneous tissue.
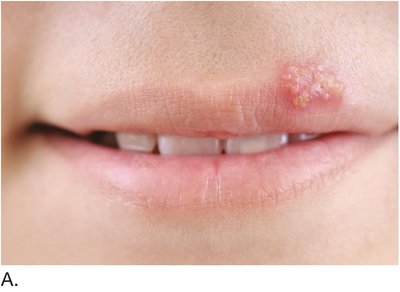
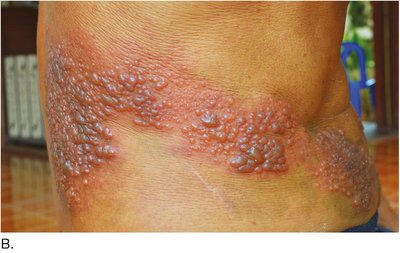
Herpes: Viral infection with vesicles and crusts (oral, genital, shingles).
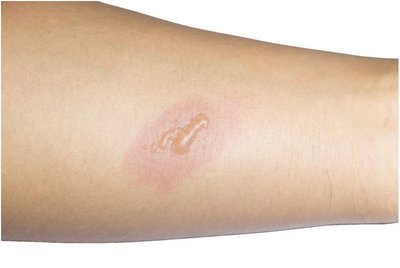
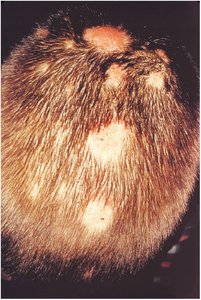
Tinea: Fungal infection (ringworm) affecting various body parts.
Verruca: Wart caused by human papillomavirus.
Skin Infestations
Pediculosis: Infestation with lice.
Scabies: Infestation with mites causing itchy vesicles.
Allergic Skin Conditions
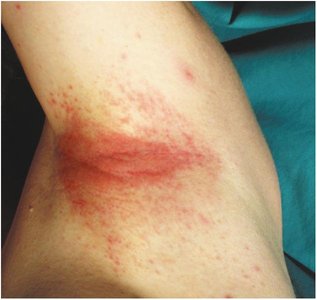
Contact dermatitis: Local reaction to allergens or irritants.
Urticaria: Hives, wheals, or welts from allergic reactions.
Benign Neoplasms of the Skin
Actinic keratosis: Rough, sun-exposed area that may become cancerous.
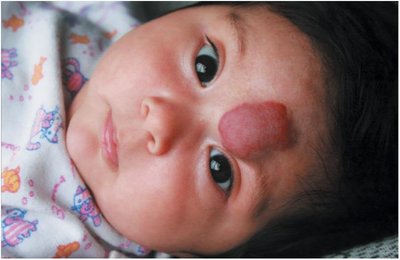
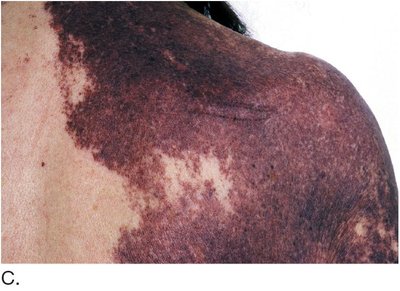
Hemangioma: Benign mass of dilated blood vessels.
Lipoma: Benign fatty tumor in subcutaneous tissue.
Nevus: Mole, present at birth, variable in color and shape.
Papilloma: Soft, flesh-colored growth on a stalk.
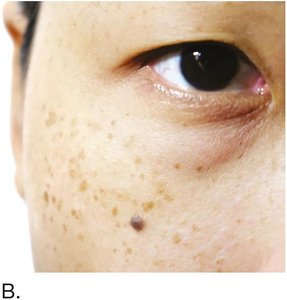
Senile lentigo: Age spots from sun exposure.
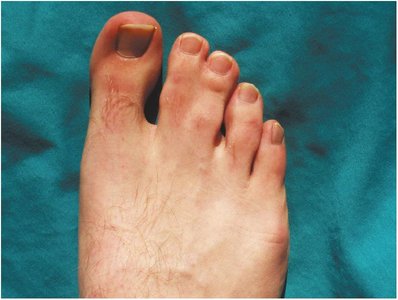
Syndactyly: Fused fingers or toes.
Malignant Neoplasms of the Skin
Basal cell carcinoma: Most common, slow-growing skin cancer in the basal epidermis.
Squamous cell carcinoma: Begins in the squamous epidermis, slow-growing red bump or ulcer.
Malignant melanoma: Aggressive cancer of melanocytes, can metastasize quickly.
Kaposi sarcoma: Cancer of connective tissue, often in immunocompromised patients.
Malignant melanoma is identified by the ABCDE criteria: Asymmetry, Border irregularity, Color variation, Diameter >6mm, and Evolving changes.
Autoimmune Disorders of the Skin
Psoriasis: Excessive abnormal epidermal cell production, causing red, scaly plaques.
Scleroderma: Hardening of skin and organs due to abnormal collagen deposits.
Systemic lupus erythematosus (SLE): Collagen deterioration with characteristic butterfly rash.
Anatomy and Diseases of Skin Appendages
Sebaceous (Oil) Glands
Exocrine glands producing sebum to moisturize hair and skin.
Diseases of Sebaceous Glands
Acne vulgaris: Blocked hair follicles with hardened sebum (blackheads, whiteheads).
Rosacea: Chronic facial redness and dilated blood vessels.
Seborrhea: Overproduction of sebum, causing oily and dry, scaly areas.
Sudoriferous (Sweat) Glands
Exocrine glands secreting sweat for cooling and waste removal.
Diseases of Sudoriferous Glands
Anhidrosis: Inability to sweat, leading to heat intolerance.
Diaphoresis: Excessive sweating, may indicate underlying disease.
Hair
Hair covers most of the body; color is determined by melanocytes.
Each hair forms in a follicle and is composed of keratinized cells.
Piloerection: Hair stands up when cold due to muscle contraction (goosebumps).
Diseases of Hair
Alopecia: Hair loss from various causes (disease, hormones, medication).
Hirsutism: Excessive, dark hair growth in females.
Nails
Nails consist of the nail plate, nail bed, lunula, cuticle, and nail root.
Diseases of Nails
Clubbing and cyanosis: Curved, bluish nails from chronic oxygen deficiency.
Onychomycosis: Fungal infection causing thickened, deformed nails.
Laboratory and Diagnostic Procedures
Allergy skin testing: Identifies allergens causing reactions.
Culture and sensitivity (C&S): Identifies bacteria and antibiotic sensitivity.
RAST: Blood test for IgE in allergic reactions.
Skin scraping: Examines cells for diagnosis.
Tzanck test: Examines vesicle fluid for infection.
Wood lamp: UV light highlights abnormal skin (e.g., vitiligo, tinea capitis).
Medical and Surgical Procedures
Botox injections: Reduce wrinkles by relaxing muscles.
Collagen injections: Plump wrinkles and scars.
Cryolipolysis: Freezes and destroys fat cells.
Cryosurgery: Freezes and destroys lesions with liquid nitrogen.
Curettage: Scrapes off superficial lesions.
Debridement: Removes necrotic tissue from wounds.
Electrosurgery: Removes lesions with electrical current.
Incision and drainage (I&D): Removes fluid or pus from cysts or abscesses.
Laser surgery: Removes birthmarks, tattoos, vessels, wrinkles, or hair.
Skin examination: Visual inspection, sometimes with magnification or biopsy.
Skin resurfacing: Removes epidermis to treat scars or irregularities.
Skin turgor assessment: Tests skin hydration by pinching and observing recoil.
Suturing: Closes wounds with stitches.
Ultherapy: Uses ultrasound to stimulate collagen production.
Biopsy: Removes tissue for microscopic examination (excisional, incisional, punch, shave).
Dermatoplasty: Plastic surgery to reshape or graft skin.
Liposuction: Removes excess fat deposits.
Mohs surgery: Removes skin cancer layer by layer with microscopic examination.
Rhytidectomy: Removes wrinkles (facelift).
Skin grafting: Covers wounds or burns with human or artificial skin.
Pharmacology: Drugs for Integumentary Diseases
Anesthetic drugs: Numb skin for procedures.
Antibiotic drugs: Treat bacterial infections.
Antifungal drugs: Treat fungal infections.
Antihistamine drugs: Reduce allergic reactions and itching.
Antiviral drugs: Treat herpes virus infections.
Corticosteroid drugs: Reduce inflammation in various skin diseases.
Alopecia drugs: Promote hair growth.
Drugs for infestations: Treat lice and mite infestations.
Coal tar drugs: Slow cell production in psoriasis.
Photodynamic therapy (PDT): Combines light and drugs to treat skin cancer.
Psoralen drugs: Sensitize skin to UV light for psoriasis treatment.
Vitamin A-type drugs: Treat acne by increasing cell turnover.
Routes of Administration
Topical: Applied directly to the skin for local effect.
Transdermal: Patch delivers drug systemically through the skin.
Intradermal: Injection just under the epidermis (e.g., allergy testing).
Hypodermic: Injection into subcutaneous tissue.
Common Abbreviations
Abbreviation | Definition |
|---|---|
B x | biopsy |
C & S | culture and sensitivity |
Derm | dermatology |
HSV | herpes simplex virus |
I & D | incision and drainage |
IgE | immunoglobulin E |
PDT | photodynamic therapy |
RAST | radioallergosorbent test |
SLE | systemic lupus erythematosus |
SQ, subcu, sub Q | subcutaneous |
