 Back
BackCardiovascular Health: Structure, Function, Disease, and Prevention
Study Guide - Smart Notes

Cardiovascular System: Structure and Function
Major Components of the Cardiovascular System
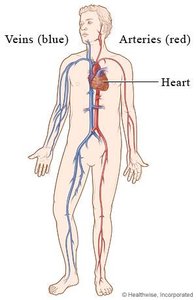
The cardiovascular system is responsible for circulating blood throughout the body, delivering oxygen and nutrients, and removing waste products. It consists of the heart and a network of blood vessels.
Heart: A muscular organ with four chambers (two atria and two ventricles) that pumps blood.
Blood Vessels: Include arteries (carry blood away from the heart), veins (carry blood to the heart), and capillaries (exchange of gases and nutrients).
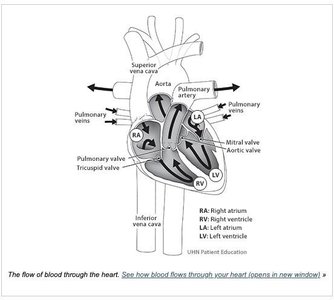
Heart Chambers and Valves
The heart is divided into four chambers and contains valves that ensure unidirectional blood flow.
Atria: The two upper chambers that receive blood returning to the heart.
Ventricles: The two lower chambers that pump blood out of the heart.
Valves: Structures that open and close to prevent backflow of blood (e.g., tricuspid, mitral, pulmonary, and aortic valves).
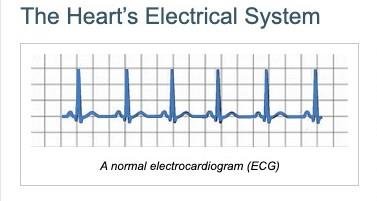
The Heart’s Electrical System
The heart’s electrical system controls the timing of heartbeats, ensuring coordinated contractions. The sinoatrial (SA) node acts as the natural pacemaker, initiating electrical impulses that travel through the atria and ventricles.
Electrocardiogram (ECG): A recording of the heart’s electrical activity, used to assess heart rhythm and detect abnormalities.
Blood Supply to the Heart
The heart muscle receives oxygen-rich blood through the coronary arteries. Blockage of these arteries can lead to heart disease.
Right Coronary Artery (RCA): Supplies the right side of the heart.
Left Coronary Artery (LCA): Splits into the left anterior descending (LAD) and circumflex arteries, supplying the left side and back of the heart.
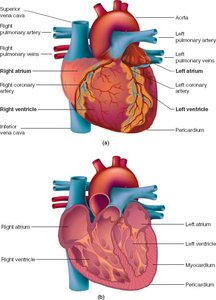
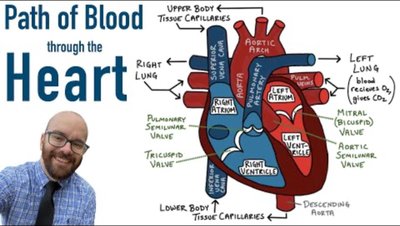
Path of Blood Flow Through the Heart
Blood flows through the heart in a specific sequence, passing through each chamber and valve to ensure efficient circulation.
Deoxygenated blood enters the right atrium via the venae cava, moves to the right ventricle, and is pumped to the lungs via the pulmonary artery.
Oxygenated blood returns from the lungs to the left atrium, moves to the left ventricle, and is pumped to the body via the aorta.
Major Forms of Cardiovascular Disease (CVD)
Heart Disease (Ischemic Heart Disease/Coronary Heart Disease)
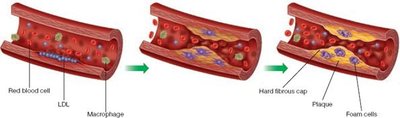
Heart disease refers to a group of conditions affecting the structure and function of the heart, often due to the buildup of plaque in the arteries (atherosclerosis).
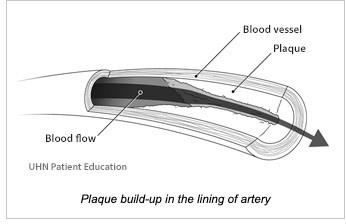
Atherosclerosis: Thickening and hardening of arteries due to deposits of fat, cholesterol, and other substances.
Plaque: Fatty deposits that narrow arteries and restrict blood flow.
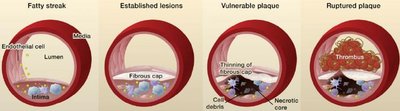
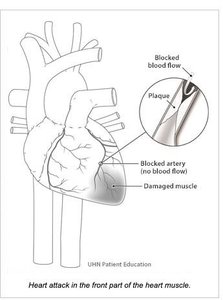
Heart Attack (Myocardial Infarction)
A heart attack occurs when blood flow to a part of the heart muscle is blocked, usually by a blood clot forming on a ruptured plaque. This leads to damage or death of heart muscle tissue.
Symptoms: Chest discomfort, pain in neck/jaw/back/arms, shortness of breath, sweating, nausea, light-headedness.
Immediate action: Seek emergency medical help to minimize heart damage.
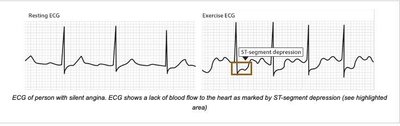
Angina
Angina is chest pain or discomfort caused by reduced blood flow to the heart muscle. It is a symptom of underlying heart disease.
Stable Angina: Occurs with physical activity or stress, predictable pattern, relieved by rest or medication.
Unstable Angina: Occurs at rest or with minimal exertion, unpredictable, may last longer, requires emergency care.
Silent Ischemia: Reduced blood flow without noticeable symptoms, common in people with diabetes.
Heart Failure
Heart failure is a condition where the heart cannot pump enough blood to meet the body’s needs. It can result from coronary artery disease, heart attack, high blood pressure, or valve disorders.
Symptoms: Shortness of breath, swollen legs, sudden weight gain, fatigue, nighttime cough.
Causes: Poor blood flow, heart muscle damage, untreated high blood pressure, faulty valves, infections.
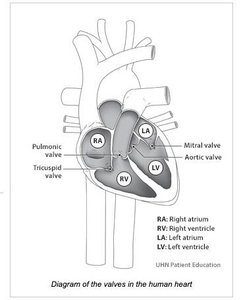
Valve Disorders
Heart valve disorders affect the function of the valves, leading to improper blood flow.
Stenosis: Narrowing of the valve, restricting blood flow.
Prolapse: Valve flaps do not close smoothly.
Regurgitation: Blood leaks backward due to improper valve closure.
Arrhythmias
Arrhythmias are abnormal heart rhythms caused by problems with the heart’s electrical system.
Bradycardia: Slow heart rate (<60 bpm).
Tachycardia: Fast heart rate (>100 bpm).
Symptoms: Chest pain, shortness of breath, weakness, dizziness, palpitations.

Risk Factors for Cardiovascular Disease
Modifiable Risk Factors
Tobacco use
High blood pressure
High cholesterol
Physical inactivity
Obesity
Type 2 diabetes
Stress
Non-Modifiable Risk Factors
Age
Sex
Heredity (genetics)
Ethnicity
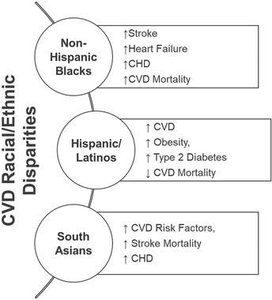
Early Life Risk Factors
Risk factors such as elevated blood pressure, high cholesterol, and smoking during childhood, adolescence, and young adulthood are associated with poorer cognitive and cardiovascular outcomes in mid-life.
Heart Age
Heart age is a concept used to illustrate cardiovascular risk. Many individuals have a heart age older than their actual age due to risk factors such as smoking, high blood pressure, diabetes, and obesity.

Prevention and Health Promotion
Reducing Risk of Cardiovascular Disease
Being smoke-free
Staying physically active
Eating a healthy diet
Maintaining a healthy weight
Limiting alcohol use
Life’s Essential 8
The American Heart Association identifies eight key measures for improving and maintaining cardiovascular health:
Healthy diet
Physical activity
Nicotine avoidance
Healthy sleep
Healthy weight
Blood lipid management
Blood glucose management
Blood pressure control


Heart-Healthy Grocery Shopping
Choose fresh, unprocessed foods such as fruits, vegetables, lean proteins, and whole grains. Pay attention to sodium, sugar, and saturated fat content to support heart health.
Health Equity and Disparities
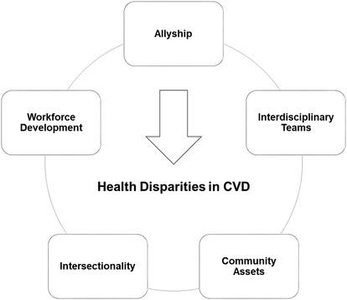
Cardiovascular disease risk and outcomes are influenced by social determinants of health, including socioeconomic status, access to care, and community resources. Addressing disparities requires culturally adapted interventions, health literacy programs, digital technology, and community partnerships.
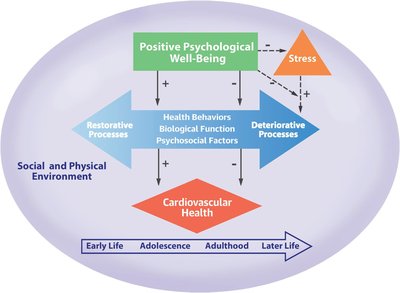
Psychological Well-Being and Cardiovascular Health
Pathways Linking Psychological Well-Being and Heart Health
Positive psychological well-being is associated with better cardiovascular health through behavioral, biological, and psychosocial pathways. It can reduce stress and promote healthy behaviors.
Biological: Blood pressure, cholesterol, glucose regulation, atherosclerosis
Behavioral: Smoking, physical activity, diet, body mass index (BMI)
Psychosocial: Social support, optimism, self-regulation
Interventions to Promote Psychological Well-Being
Mindfulness-based programs
Optimism and gratitude exercises
Community and culturally tailored interventions
Mobile and digital health tools
Health Asset Approach
This approach focuses on identifying and mobilizing resources (mental, social, material) that help individuals and communities maintain health and well-being. It emphasizes strengths and assets rather than deficits.
Summary Table: Activities to Promote Positive Psychological Well-Being
Characteristic or Asset | Introductory Activity | Structured Activities | Skill Developed |
|---|---|---|---|
Optimism | Discussing a better possible health-related future | Writing about a best possible health-related future and steps to achieve it | Developing optimistic health expectations |
Gratitude | Discussing reasons to be grateful for health | Journaling positive events, writing gratitude letters | Cultivating a grateful worldview |
Self-efficacy | Reflecting on past successes | Writing about successes and applying strengths to health goals | Building confidence and using strengths for health |
Positive affect | Discussing pleasurable activities | Scheduling and savoring positive events | Enhancing enjoyment of positive experiences |
Meaning or purpose | Discussing sources of purpose | Writing about legacy and meaningful goals | Linking self-care to life goals |
Key Equations
Blood Pressure:
Cardiac Output:
Additional info: These notes integrate foundational knowledge of cardiovascular structure and function, major diseases, risk factors, prevention strategies, and the role of psychological well-being, as relevant to a personal-health college course.
