 Back
BackPhlebotomy Practice and Quality Assessment: Foundations for Personal Health Professionals
Study Guide - Smart Notes

Phlebotomy Practice and Definition
Introduction to Phlebotomy
Phlebotomy is a critical procedure in health care, involving the collection of blood specimens for laboratory analysis, diagnosis, and treatment. The practice is guided by established standards and is performed by various health professionals.
Definition: Phlebotomy derives from Greek roots: phlebo (vein) and tomy (cutting). It refers to the incision of a vein for blood collection.
Purpose: Blood collection supports diagnostic testing, therapeutic interventions (e.g., blood transfusions), and monitoring of patient health.
Professionals Involved: Certified phlebotomists, nurses, medical assistants, patient care technicians, and other trained personnel.
Common Techniques:
Venipuncture: Drawing blood from a vein using a needle and collection device.
Skin (Dermal) or Capillary Puncture: Superficial puncture (finger or heel) for small blood samples, often used in infants.
Historical Context: Early phlebotomy practices date back to the Stone Age and were used for ritualistic or therapeutic purposes. Excessive bloodletting was once common and could be fatal, as in the case of President George Washington.
Role of Laboratory Testing in Health Care
Clinical Decision-Making
Laboratory test results are essential for diagnosing, treating, and monitoring diseases. They are used in:
Diagnostic and Screening Tests: Identify abnormalities or diseases (e.g., CBC, chemistry panels, coagulation tests).
Therapeutic Assessments: Guide treatment decisions (e.g., antibiotic selection, drug dosing).
Monitoring: Evaluate the effectiveness of treatments (e.g., glucose monitoring, PT/INR for anticoagulation).
Health Care Settings and Teams
Settings for Phlebotomy Services
Phlebotomy is performed in various health care environments:
Inpatient: Hospitals
Ambulatory Care: Outpatient clinics, urgent care centers, home health, dialysis centers, private labs
Phlebotomists interact with a multidisciplinary health care team, including physicians, nurses, laboratory personnel, and administrative staff.

The Clinical Laboratory and Specimen Collection Services
Laboratory Departments and Personnel
Clinical laboratories are organized into specialized departments, each responsible for specific types of testing:
Clinical Chemistry: Glucose, electrolytes, lipids
Hematology/Coagulation: CBC, PT/INR, PTT
Microbiology/Parasitology/Virology
Immunohematology (Blood Bank)
Immunology/Serology
Urinalysis
Genetics/Cytogenetics
Molecular Diagnostics
Toxicology
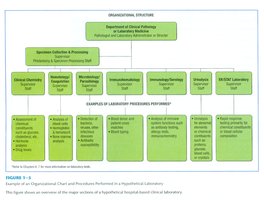
Personnel include administrative staff, laboratory managers, physicians/scientists, and technical staff (MT, MLT, MLA).
Competencies, Certification, and Professionalism for Phlebotomists
Education and Certification
Requirements: High school diploma or equivalent, formal training, and passing a national certification exam.
Continuing Education (CE): Required to maintain certification and stay current with advances in the field.
Professional Organizations: ASCLS, ASCP, NPA, NHA, among others.
Professionalism and Ethics
Professionalism: Involves respect, service, support, and growth. Phlebotomists must demonstrate reliability, effective communication, and commitment to team goals.
Ethical Standards: Do no harm, maintain confidentiality, respect patient rights, and act with integrity.
Character Traits: Sincerity, compassion, emotional stability, accountability, dedication to high standards, and respect for diversity.

Appearance, Grooming, and Stress Management
Physical Fitness: Good posture, hygiene, and use of personal protective equipment (PPE) are essential.
Stress Management: Techniques include exercise, proper nutrition, adequate sleep, humor, and seeking professional help when needed.

Quality Assurance: Control, Improvement, and Assessment
Quality Concepts in Health Care
Quality: Defined by excellence in both technical (accuracy, reliability) and interpersonal (communication, patient satisfaction) aspects.
Major Concepts: Efficacy, appropriateness, and caring functions (timeliness, safety, respect).
Stakeholders: Internal (staff, management) and external (patients, regulatory agencies).

Quality Initiatives and Standards
Continuous Quality Improvement (CQI): Ongoing efforts to improve processes and outcomes.
Six Sigma: A systematic, data-driven approach to reduce variation and improve quality. Phases: Define, Measure, Analyze, Improve, Control (DMAIC).
ISO Standards: International standards for quality management and laboratory operations.
CLIA: U.S. regulations for laboratory quality, including individualized quality control plans.
Tools for Quality Performance Assessment
Brainstorming: Generating ideas to address quality issues.
Cause-and-Effect (Fishbone) Diagrams: Identifying factors contributing to problems.
Flowcharts: Visualizing process steps and decision points.
Pareto Charts: Identifying the most frequent causes of problems (80/20 rule).
Plan-Do-Check-Act (PDCA) Cycle: Structured approach for implementing and reassessing changes.
Quality Control Charts: Monitoring data trends over time.
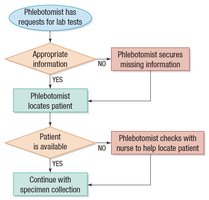
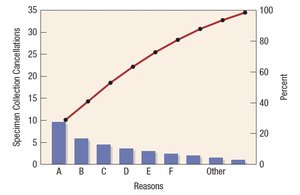
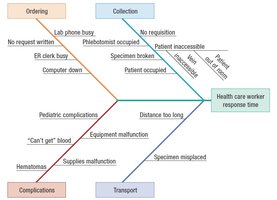
Phases of Laboratory Testing and Quality in Specimen Collection
Phases of Laboratory Testing
Preexamination: Patient preparation, specimen collection, labeling, and transport.
Examination: Laboratory analysis of the specimen.
Postexamination: Reporting and interpreting results, follow-up actions.
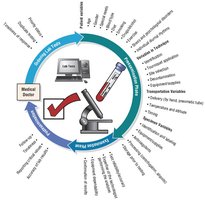
Requirements for Quality Specimens
Correct patient identification and labeling
Use of appropriate anticoagulants and preservatives
Timely collection and transport
Proper handling and documentation
Future Trends in Phlebotomy Practice
Emerging Developments
Standardization and globalization of laboratory practices
Electronic medical records and point-of-care testing
Direct access testing (DAT) and direct-to-customer (DTC) services
Use of robotics, drones, and nanotechnology in specimen collection and transport
Additional info: These notes provide foundational knowledge for personal-health students, emphasizing the importance of quality, professionalism, and teamwork in phlebotomy and laboratory services.
