 Back
BackPhlebotomy Practice and Quality Assessment: Foundations for Personal Health Professionals
Study Guide - Smart Notes

Phlebotomy Practice and Quality Assessment
Introduction to Phlebotomy
Phlebotomy is a critical component of modern health care, involving the collection of blood specimens for laboratory analysis, diagnosis, and treatment. This field requires technical skill, professionalism, and adherence to quality standards to ensure patient safety and accurate results.
Definition: Phlebotomy is the incision of a vein for collecting a blood sample for laboratory testing or therapeutic purposes.
Historical Context: Early forms of phlebotomy date back to the Stone Age, with bloodletting once used to treat various ailments. Modern phlebotomy focuses on safe, minimal blood collection for diagnostic and therapeutic reasons.
Common Techniques: Venipuncture (drawing blood from a vein) and capillary puncture (finger or heel stick for small samples).
Applications: Used for diagnostic testing, therapeutic assessments, and monitoring treatment effectiveness.

Role of Phlebotomy in Health Care
Phlebotomy supports clinical decision-making by providing accurate laboratory data. Health professionals such as certified phlebotomists, nurses, medical assistants, and patient care technicians may perform phlebotomy procedures.
Settings: Hospitals, clinics, urgent care centers, home health care, ambulances, dialysis centers, and laboratories.
Clinical Laboratory Test Results: Used to diagnose, monitor, and treat diseases. Examples include CBC, chemistry panels, coagulation studies, and more.
Health Care Teams and Laboratory Structure
Phlebotomists are integral members of the health care team, interacting with physicians, nurses, laboratory personnel, and other professionals. Understanding the structure and function of the clinical laboratory is essential for effective teamwork and patient care.
Laboratory Departments: Clinical chemistry, hematology, microbiology, immunology, blood bank, urinalysis, genetics, molecular diagnostics, and toxicology.
Personnel: Includes administrative staff, laboratory managers, pathologists, medical technologists, and phlebotomists.

Professionalism and Competencies for Phlebotomists
Professionalism in phlebotomy encompasses technical competence, ethical behavior, and effective communication. Certification and continuing education are required to maintain high standards.
Core Competencies: Knowledge of blood collection procedures, anatomy, infection control, patient safety, and regulatory requirements.
Professional Traits: Respect, service, support, growth, sincerity, compassion, emotional stability, accountability, and dedication to quality.
Certification: National certification exams and continuing education are often required.

Physical Fitness, Appearance, and Stress Management
Phlebotomists must maintain good physical health, personal hygiene, and manage workplace stress to ensure optimal performance and patient care.
Physical Fitness: Good nutrition, regular exercise, adequate sleep (7-9 hours/day), and proper posture are essential.
Appearance: Clean uniforms, proper grooming, and use of personal protective equipment (PPE) are required.
Stress Management: Techniques include exercise, humor, hobbies, adequate sleep, and seeking professional help if needed.

Quality Assurance and Improvement in Phlebotomy
Quality Concepts in Health Care
Quality in health care is defined by excellence, high standards, and the integrity of processes and outcomes. Both technical and interpersonal aspects are important for patient satisfaction and safety.
Major Concepts: Efficacy (positive patient outcomes), appropriateness (correct procedures), and caring functions (timely, effective, and respectful service).
Stakeholders: Internal (staff, management) and external (patients, regulatory agencies) groups are invested in quality outcomes.

Quality Initiatives and Standards
Quality assurance involves adherence to codes of ethics, standards of practice, and continuous quality improvement (CQI) models such as Six Sigma and Lean Six Sigma. Regulatory agencies and professional organizations set guidelines for laboratory operations and personnel certification.
Key Agencies: FDA, CMS, CLIA, OSHA, CAP, ASCP, and others.
Quality Management: Includes customer focus, leadership, engagement, process approach, improvement, evidence-based decisions, and relationship management.
CLIA Quality Control Plan: Involves risk assessment, quality control procedures, and quality assessment to ensure accurate and reliable results.
Tools for Quality Performance Assessment
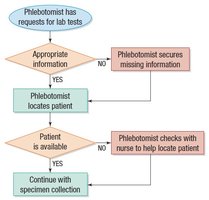
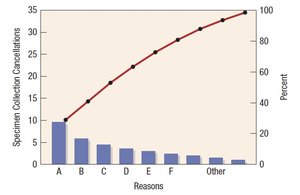
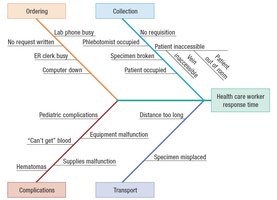
Various tools are used to monitor and improve laboratory quality, including brainstorming, cause-and-effect diagrams, flowcharts, Pareto charts, and the Plan-Do-Check-Act (PDCA) cycle.
Key Metrics: Sensitivity, specificity, accuracy, and precision of laboratory tests.
Data Visualization: Flowcharts, Pareto charts, and fishbone diagrams help identify and address quality issues.
Phases of Laboratory Testing and Quality in Specimen Collection
The laboratory testing process is divided into preexamination, examination, and postexamination phases. Each phase has specific requirements to ensure specimen quality and accurate results.
Phase | Description | Examples |
|---|---|---|
Preexamination | Before testing | Patient identification, specimen collection, labeling, transport |
Examination | During testing | Analyzing specimen, instrument calibration, quality control |
Postexamination | After testing | Reporting results, specimen storage, follow-up |

Basic Requirements for a Quality Specimen
Use standard precautions and correct patient identification.
Collect specimens using appropriate anticoagulants and preservatives.
Label, handle, and transport specimens promptly and accurately.
Ensure fasting and timed specimens are collected as required.
Future Trends in Phlebotomy
Phlebotomy is evolving with advances in technology and globalization. Trends include electronic medical records, point-of-care testing, direct access testing, robotics, and increased emphasis on education and certification.
Standardization: International standards (ISO) for quality and safety.
Technology: Nanotechnology, robotics, and direct-to-customer testing are shaping the future of specimen collection and analysis.
Summary Table: Key Laboratory Departments and Functions
Department | Examples of Tests/Functions |
|---|---|
Clinical Chemistry | Glucose, electrolytes, lipids |
Hematology/Coagulation | CBC, PT/INR, PTT |
Microbiology | Cultures, sensitivity testing |
Immunology/Serology | Antibody-antigen testing |
Blood Bank | Blood typing, crossmatching |
Urinalysis | Urine chemistry, microscopy |
Genetics/Molecular Diagnostics | DNA analysis, PCR |
Additional info: These notes provide a comprehensive overview of phlebotomy practice, professionalism, and quality assurance, suitable for personal-health college students preparing for exams or clinical practice.
