 Back
BackN1016 Physical Changes of Aging - Class 4
Study Guide - Smart Notes

Introduction to Aging and Health
Overview of Aging
Aging is a complex, lifelong process influenced by biological, psychological, social, functional, and spiritual factors. It is characterized by a continuum of events from conception to death. Theories of aging are categorized as biological, sociological, psychological, and moral/spiritual, but the exact cause of aging remains unknown. Aging is highly individualized, with significant diversity among older adults.

Biological Theories of Aging
Stochastic (Error) Theories
Stochastic theories propose that aging results from the accumulation of random errors in the synthesis of DNA and RNA over time. With each cell replication, more errors occur until the cell can no longer function. The Wear and Tear Theory is a classic example, suggesting that cumulative damage leads to aging.
Nonstochastic (Programmed) Theories
Nonstochastic theories suggest that each cell has a natural life expectancy, programmed to replicate a set number of times before dying. The Neuroendocrine-Immunological Theory posits that immune function declines with age, increasing susceptibility to autoimmune diseases such as rheumatoid arthritis.
System-by-System Physiological Changes
Integumentary System (Skin, Hair, Nails)
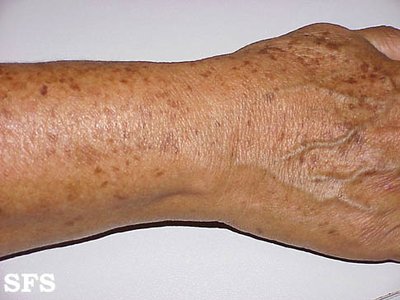
The integumentary system undergoes several age-related changes, including thinning of the skin, loss of elasticity, and decreased turgor. Melanocyte numbers decrease, leading to lighter skin color. Nails become harder, brittle, and discolored, while hair thins and grays. Environmental exposure accelerates these changes.
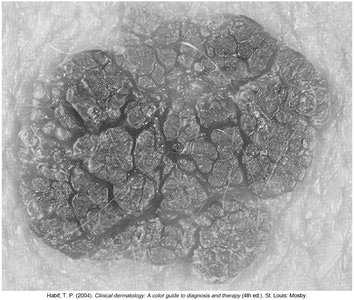
Common conditions: Senile purpura (purple spots), lentigines (age spots), seborrheic keratoses (brown, raised lesions), and xerosis (dry skin).
Implications: Increased risk of skin infections, injury, and skin cancer; altered absorption of topical medications.
Promoting healthy skin: Use sunscreen, avoid excessive sun, stay hydrated, and apply moisturizer after bathing.

Musculoskeletal System
Aging leads to changes in stature and posture due to reduced bone mineral density, muscle atrophy, and water loss in vertebral disks. Kyphosis (stooped posture) and loss of height are common. Muscle strength decreases, bone mass declines (especially after menopause in women), and joints become stiffer and less flexible, increasing the risk of osteoarthritis and fractures.
Promoting bone and muscle health: Adequate calcium and vitamin D intake, regular weight-bearing and flexibility exercises, and a diet rich in calcium.


Cardiovascular System
Normal aging of the cardiovascular system includes increased left ventricular wall thickness, slight enlargement of the left atrium, decreased cardiac output, and reduced contractile strength. Blood vessels lose elasticity, thicken, and narrow, increasing peripheral resistance and blood pressure. Perfusion to organs such as the liver and kidneys decreases.
Clinical significance: The heart rate responds more slowly to stressors (e.g., pain, fever, anxiety), and symptoms of heart disease (e.g., coronary artery disease) may develop.
Promoting heart health: Regular exercise, low-fat diet, diabetes control, avoiding smoking, minimizing sodium, and maintaining ideal body weight.

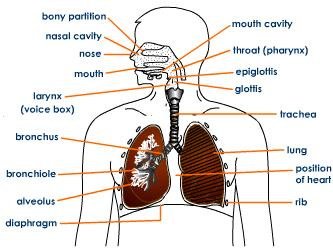
Respiratory System
With age, the trachea and rib cage stiffen, gas exchange efficiency decreases, and cilia become less effective. The lungs become smaller and less elastic, and the cough reflex weakens, increasing the risk of respiratory infections. Most respiratory problems in older adults are due to environmental exposures and lifestyle factors.

Renal/Urinary System
The kidneys lose nephrons and decrease in size, reducing the glomerular filtration rate (GFR) and affecting waste and drug excretion. Bladder capacity decreases, muscle tone is lost, and incomplete emptying becomes common, leading to frequency, nocturia, urgency, and increased risk of urinary tract infections. Urinary incontinence is more prevalent but not a normal part of aging.
Endocrine System
Most endocrine glands atrophy and secrete hormones at a reduced rate. The thyroid gland's activity decreases, lowering basal metabolic rate, while the pancreas becomes less sensitive to insulin, increasing the risk for type 2 diabetes.


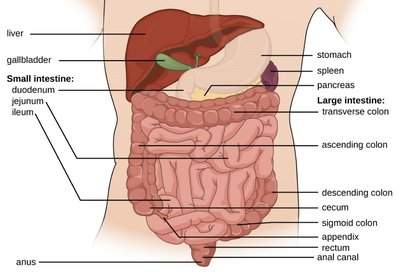
Gastrointestinal System
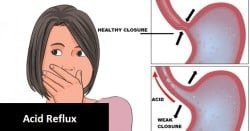
The digestive system experiences reduced taste sensation, saliva production, and increased risk for periodontal disease and tooth loss. Esophageal motility decreases, increasing the risk of reflux and hiatal hernia. Gastric atrophy leads to decreased hydrochloric acid and mucus secretion, slowing gastric emptying. Small bowel changes affect nutrient absorption, while large bowel motility slows, increasing the risk of constipation (primarily due to diet and inactivity). The liver decreases in size and blood flow, and the gallbladder may form more gallstones.


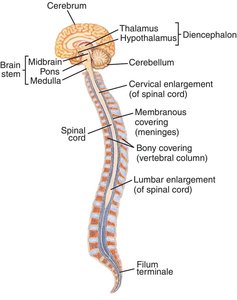
Neurological System
The central nervous system loses neurons, dendrites wear out, and the brain decreases in weight and size. Neurotransmitter levels decline, and the peripheral nervous system loses nerve endings, especially in the extremities. Intellectual performance is generally intact, but task completion is slower, and mild memory impairments may occur. Proprioception and balance are affected, increasing the risk of falls.
Immune System
The immune response to foreign antigens and organisms decreases with age, reducing the ability to fight infections. Thinner skin and reduced cilia in the lungs increase vulnerability to pathogens. T cell function declines, and signs of infection may be atypical (e.g., confusion instead of fever).


Summary Table: Key Age-Related Changes by System
System | Main Age-Related Changes |
|---|---|
Integumentary | Thinner skin, less elasticity, age spots, dry skin, slower healing |
Musculoskeletal | Bone loss, muscle atrophy, joint stiffness, increased fracture risk |
Cardiovascular | Thicker heart walls, higher blood pressure, slower heart rate response |
Respiratory | Stiffer chest wall, less efficient gas exchange, weaker cough |
Renal/Urinary | Reduced kidney function, smaller bladder, increased incontinence risk |
Endocrine | Lower hormone secretion, decreased insulin sensitivity |
Gastrointestinal | Reduced taste, slower motility, decreased absorption, constipation risk |
Neurological | Neuron loss, slower processing, balance issues, mild memory loss |
Immune | Weaker immune response, atypical infection symptoms |
