 Back
BackPopulation Health: Concepts, Evolution, and Nursing Roles
Study Guide - Smart Notes

Population Health: Concepts and Foundations
Definition and Scope of Population Health
Population health is a broad conceptual framework that focuses on the health outcomes of groups of individuals, including the distribution of such outcomes within the group. It considers the physical, social, and economic environments that influence health, as well as individual health practices, genetics, early childhood development, and access to health services.
Population Health: The health status of a population, measured by health indicators and influenced by various determinants.
Determinants of Health: Factors such as environment, genetics, health practices, and access to care that shape health outcomes.
Health Status Indicators: Metrics used to assess the health of a population (e.g., life expectancy, disease prevalence).

Population Health Approach vs. Traditional Approaches
The population health approach differs from traditional medical models by addressing the full range of health determinants and aiming to improve health for entire populations, not just individuals. It seeks to reduce health inequities and promote social and material balance.
Population Health Approach: Focuses on broad determinants, targets whole populations, and aims to reduce inequities.
Biomedical Approach: Focuses on individual risk factors, disease diagnosis, and cure.
Public Health: Uses health information to promote health and prevent disease, often implementing recommendations from population health studies.
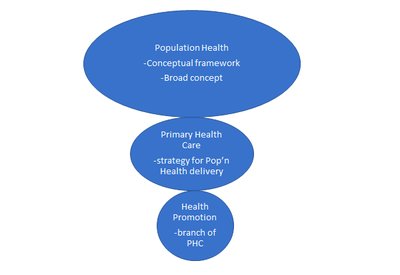
Determinants of Health and Causal Chains
Understanding Causal Chains in Health
Health outcomes are often the result of complex causal chains involving social, economic, and environmental factors. The story of "Jason" illustrates how upstream determinants, such as parental employment and education, can lead to downstream health issues.
Causal Chain: A sequence of events or factors that lead to a health outcome.
Upstream Determinants: Root causes such as socioeconomic status, education, and environment.
Downstream Effects: Immediate health outcomes, such as injury or infection.



Key Elements and Frameworks in Population Health
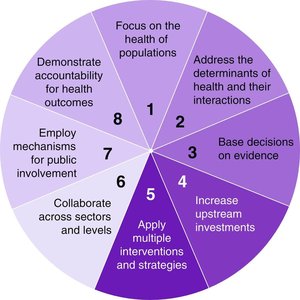
Core Elements of the Population Health Approach
The population health approach is structured around several key elements that guide policy and practice. These elements emphasize evidence-based decision-making, upstream investments, public engagement, and intersectoral collaboration.
Measure population health status
Analyze determinants of health
Use evidence-based decision making
Employ upstream investments
Apply multiple strategies
Engage the public
Think intersectoral collaboration
Demonstrate accountability for health outcomes
Population Health vs. Public Health vs. Biomedical Approach
It is important to distinguish between these approaches to understand their unique contributions and limitations.
Population Health | Public Health | Biomedical Approach |
|---|---|---|
Addresses broad determinants, targets populations, reduces inequities | Uses data to promote health and prevent disease in communities | Focuses on individual risk, diagnosis, and cure |
Health promotion, disease prevention, policy | Implements recommendations, community focus | Clinical care, individual treatment |
Evolution of Population Health in Canada
Major Milestones and Reports
Population health in Canada has evolved through key reports and international conferences, shaping current health promotion and policy frameworks.
1974: Lalonde Report
1978: Alma Ata Conference
1986: Ottawa Charter for Health Promotion
1986: Epp Report
1987-2003: Canadian Institute for Advanced Research
1996: Toward a Healthy Future report


Social Determinants of Health (SDOH)
Expanding the Determinants
The list of social determinants of health has expanded over time to reflect a broader understanding of the factors influencing health. As of 2020, 17 key determinants are recognized in Canada, including income, education, employment, housing, social exclusion, and more.
Income and income distribution
Education
Unemployment and job security
Employment and working conditions
Early childhood development
Food insecurity
Housing
Social exclusion
Social safety net
Health services
Geography
Disability
Indigenous ancestry
Gender
Immigration
Race
Globalization
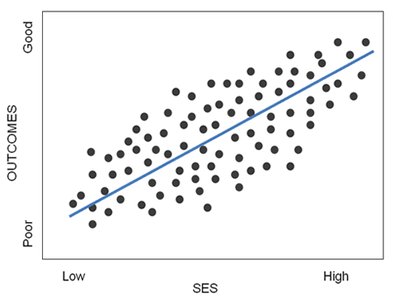
The Social Gradient and Health Inequities
The "social gradient" in health refers to the consistent finding that health outcomes improve with increasing socioeconomic status (SES). This gradient is observed even among higher SES groups, indicating that relative inequality, not just absolute poverty, affects health.
Wilkinson Hypothesis: Inequality, rather than absolute wealth, is a key driver of health outcomes.
SES Gradient: Higher SES is associated with better health outcomes; lower SES with poorer outcomes.
Nursing Roles in Health Promotion
Key Roles of Nurses in Population Health
Nurses play a central role in health promotion and population health, working in diverse settings and fulfilling multiple roles to improve health outcomes and reduce inequities.
Advocate: Helps clients access services and supports social justice.
Care Manager: Ensures appropriate and efficient use of health services.
Consultant: Provides expertise in health, illness, and community dynamics.
Direct Caregiver: Delivers care in various settings, often collaboratively.
Educator: Facilitates health education and promotes healthy changes.
Researcher: Engages in research to advance health promotion.

Critiques and Future Directions
Critique of the Population Health Approach
While the population health approach is evidence-based and comprehensive, it has been critiqued for being too focused on epidemiology, lacking a values base, and not sufficiently addressing social justice or political factors. The approach is sometimes seen as top-down and more suited for research than for driving change.
Rooted in epidemiology (disease-focused)
Lacks explicit values or social justice orientation
May overlook political determinants of health
Top-down, research-oriented model
Future Directions
There is a growing emphasis on expanding the determinants of health to better reflect lived experiences and social realities, as well as on intersectoral collaboration and community engagement to address health inequities.
Summary Table: Key Differences in Health Approaches
Approach | Focus | Target | Strategies |
|---|---|---|---|
Population Health | Determinants of health, equity | Populations/groups | Policy, prevention, promotion |
Public Health | Community health, disease prevention | Communities | Programs, surveillance, education |
Biomedical | Individual disease, risk factors | Individuals | Diagnosis, treatment, cure |
