 Back
BackTuberculosis: Biological, Behavioral, and Societal Aspects
Study Guide - Smart Notes

Tuberculosis: Overview and Biological Basis
Introduction to Tuberculosis
Tuberculosis (TB) is a major infectious disease caused by the bacterium Mycobacterium tuberculosis. It primarily affects the lungs but can involve other organs. Understanding TB requires knowledge of its biology, transmission, risk factors, and the societal context in which it spreads and is managed. 
Biology of Mycobacterium tuberculosis
- Classification: Slow-growing, aerobic, non-motile, non-sporing, acid-fast bacillus. - Cell Wall: Contains complex lipids, including mycolic acids, making it resistant to decolorization by acid and alcohol (acid-fast property). - Growth: Grows slowly on Eaton agar, producing buff-colored, rough colonies in 3-5 weeks. - Staining: Ziehl-Neelsen stain is used to identify acid-fast bacilli. 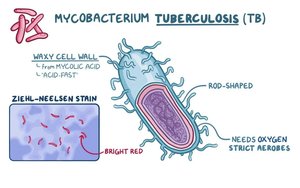
Transmission
- Primary Route: Airborne spread via droplets that remain suspended for hours. - Other Routes: Ingestion of contaminated milk (rare). 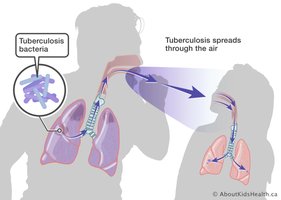
Pathophysiology and Clinical Manifestations
Pathophysiology
When inhaled, M. tuberculosis infects alveolar macrophages. The immune system usually contains the infection, resulting in latent TB. In some cases, the bacteria evade immunity, leading to active disease. - Latent TB: Bacteria remain dormant; no symptoms; not contagious. - Active TB: Bacteria multiply, causing symptoms and potential spread. - Progression: 90% develop latent infection; 5% develop active TB within 2 years; another 5% later in life. 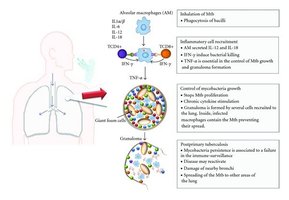
Symptoms and Complications
- Symptoms: Cough, fever, weight loss, night sweats. - Complications: Lung damage, pleural effusion, meningitis, pneumonia. 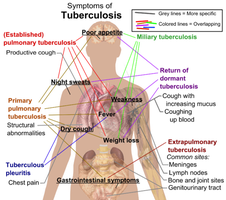
Latent vs. Active TB
Latent TB | Active TB |
|---|---|
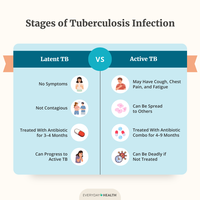
No symptoms | Cough, chest pain, fatigue |
Not contagious | Contagious |
Treated with antibiotics for 3-4 months | Treated with antibiotics for 4-9 months |
Can progress to active TB | Can be deadly if untreated |
Diagnosis of Tuberculosis
Diagnostic Tests
- Chest X-ray: May show Gohn focus, upper lobe lesions, pleural effusion, miliary pattern, or raised lymph nodes. 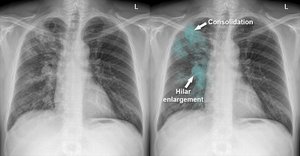 - Mantoux Test (Tuberculin Skin Test): Intradermal injection of PPD; positive result suggests TB infection.
- Mantoux Test (Tuberculin Skin Test): Intradermal injection of PPD; positive result suggests TB infection. 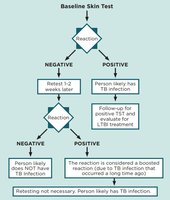 - Acid-Fast Bacilli (AFB) Test: Microscopy for acid-fast bacilli; limited sensitivity and specificity. - Blood Tests (IGRAs): Interferon-gamma release assays (e.g., QuantiFERON-TB Gold Plus, T-SPOT.TB) measure immune response to TB proteins; high sensitivity and specificity.
- Acid-Fast Bacilli (AFB) Test: Microscopy for acid-fast bacilli; limited sensitivity and specificity. - Blood Tests (IGRAs): Interferon-gamma release assays (e.g., QuantiFERON-TB Gold Plus, T-SPOT.TB) measure immune response to TB proteins; high sensitivity and specificity. 
Risk Factors and Epidemiology
Risk Factors for Active TB
- Immunocompromised state (e.g., HIV, older age, genetic immunodeficiency, transplantation, corticosteroid use, chemotherapy, TNF antagonists) - Malnutrition - Diabetes - Tobacco and excessive alcohol use
Global Burden and History
- TB has co-evolved with humans, with evidence from ancient Egypt and references in ancient texts. - Became endemic in the 19th century, causing significant mortality, especially among young people. - In 2023, 1.25 million deaths and 10.8 million new cases worldwide; TB is present in all countries and age groups. - TB is curable and preventable, but multidrug-resistant TB (MDR-TB) remains a major challenge.
Prevention and Treatment
Vaccination
- BCG Vaccine: First used in 1921; reduces TB risk by about 50%. Effectiveness varies by region and population genetics. 
Drug Resistance
- MDR-TB: Develops when treatment is incomplete, incorrect, or drugs are of poor quality. Also associated with reinfection and exposure to drug-resistant cases. 
Societal and Behavioral Factors
Social Determinants of TB
- Poverty, low income, poor housing, limited healthcare access, low education, and health literacy increase TB risk and hinder control efforts. - Social and cultural factors influence health-seeking behavior and treatment adherence.
Effective Healthcare Systems
- Key Elements: Education, evidence-based care, robust infrastructure, diagnostic and pathology services, high-quality medication, social support, and reliable health information. - Evidence-Based Medicine (EBM): Integrates best research evidence, clinical expertise, and patient values for optimal care. 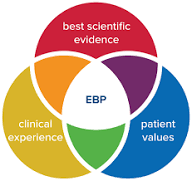
Healthcare Financing Models
- General Taxation: Beveridge and Semashko models (government-funded). - Insurance-Based: National, social, or private health insurance. - Out-of-Pocket Payments: Direct household spending; associated with financial hardship and lack of risk pooling.
Universal Health Coverage (UHC)
- UHC ensures access to high-quality health services for all, including preventive, diagnostic, treatment, and rehabilitation services, without financial hardship. - WHO evaluates health systems based on population health, health inequalities, responsiveness, and financial burden distribution.
Primary Healthcare
- First point of contact; essential for prevention, early detection, and management of TB and other diseases. - Rooted in social justice, aiming for equitable health outcomes.
Health Misinformation and TB
Fake News and Health Misinformation
- Misinformation: False or inaccurate information shared without intent to mislead. - Disinformation: Deliberately false information intended to mislead. - Types: Mischaracterization of disease, false treatments, scapegoating, conspiracy theories.
Psychological Factors
- Motivated Reasoning: People believe information that aligns with their worldview. - Confirmation Bias: Tendency to favor information that confirms existing beliefs. - Backfire Effect: Rejecting misinformation can sometimes strengthen false beliefs, especially on core issues.
Addressing Misinformation
- Societal Level: Intervene against false content, promote factual information, increase public resilience, and coordinate national strategies. - Individual Level: Understand information sources, consider cultural context, engage respectfully, encourage verification, and provide alternative sources.
Digital Health Literacy
- The ability to seek, find, understand, and appraise health information online is crucial for recognizing and countering misinformation. - Higher health literacy is associated with better health outcomes and reduced susceptibility to misinformation.
Patient Autonomy
- Adults with mental capacity have the right to make informed decisions about their health, even if those decisions carry risks. The role of healthcare professionals is to provide balanced information and respect patient choices.
